News 4/23/25
Top News
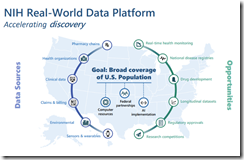
NIH is aggregating data from insurance claims, the VA, Indian Health Service, pharmacy chains, and even wearables to support the HHS-mandated autism research initiative that was launched by HHS Secretary Robert F. Kennedy Jr.
NIH will also create a disease registry to track Americans with autism.
Kennedy has stated that HHS will determine the cause of autism by September.
Reader Comments
From Oingo Boingo: “Re: engagement. You said your site was tops in health tech media, but didn’t explain what that means.” The Black Book Research survey included these questions: (a) whether respondents had read anything on a given site in the past month, and (b) whether they spent more than 20 minutes there. Becker’s Health IT & CIO Report beat HIStalk on raw visits, but trailed badly on time spent on site, which I take to mean that they write a strong headline but less-strong content. One site that I assumed was a capable competitor turned out to be a non-factor, with 0% of respondents saying they had read it in the past month. HIStalk was also #1 in overall credibility and industry respect and also topped the category of providing unbiased and accurate information with a score of 9.9 on a 10 scale. As a lazy, part-time amateur, I’ll take it.
HIStalk Announcements and Requests
I visited a family member who was a patient in a small, university-affiliated hospital several times last week. Given that I’ve only spent one night in a hospital myself, and that was years ago, these were my technology observations:
- The entire staff impressively used Stryker-owned Vocera’s communication for both clinical and administrative conversations, including in the patient rooms. I didn’t hear a single overhead page.
- They used Epic’s secure messaging function to ask questions and coordinate care in real time to get answers quickly rather than promising to find out later.
- Barcode verification was performed for just about everything.
- Clinical information flowed spectacularly across care that included ED, procedures, and clinical team rounds.
- The ability to order patient meals and guest trays via room service was very different than in my early hospital days.
- The nurse made appointments for follow-visits and had prescriptions filled and delivered at discharge, all via Epic, I presume.
Dear people of the Internet: if your graph’s y-axis doesn’t start at zero, I assume that you’re trying to support a shaky opinion rather than presenting facts and I move on.
Sponsored Events and Resources
None scheduled soon. Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock
Brellium announces $16.7 million in Series A funding. The company offers automated chart auditing software to help providers maintain clinical and payer compliance.
Value-based care workflow automation vendor Reveleer acquires Novillus, which offers provider engagement and care gap management software to payers. Headquartered in California, Reveleer opened an operations hub in India last month.
Automated case management software startup Ascertain raises $10 million in Series A funding.
Patient experience software vendor Promptly acquires medical practice software from Patient Spectrum.
People

MyMichigan Health promotes Pankaj Jandwani, MD, MMM to VP/CIO.

Clearwater appoints Jeff Englander, MBA (New York University) executive advisor, business development.

Adam Weinstein, MBA (Cityblock Health) joins Teladoc Health as chief product officer.
Announcements and Implementations
South Australia Health implements Altera Digital Health’s Sunrise EHR and patient administration system across all of its public hospitals. The contract for the $225 million project was signed in 2011.

Emory University Hospital Midtown (GA) integrates AI-powered fall-prevention capabilities from VirtuSense Technologies with its virtual nursing service. Emory Healthcare plans to deploy the VSTOne technology across eight inpatient units this year.
University of California Health describes how its nurses are using AI.

Adventist HealthCare rolls out Mednition’s Kate AI to several of its EDs to support and validate nurse decisions for high-risk and complex patients.
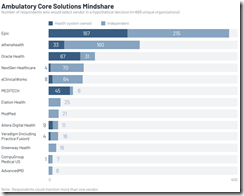
A new KLAS report on ambulatory core solution mindshare finds that while functionality is the highest consideration factor, interoperability trails just behind, while usability is #3.
Government and Politics
A VA memo to regional directors stresses the need for clinicians who provide virtual consults to do so in private workspaces as they return to working in VA facilities in the coming weeks, per a mandatory return-to-office order that has left some providers concerned about working in open, call-center-like spaces. The memo doesn’t specify what providers should do if such spaces aren’t available. Meanwhile, the VA reports a 12% increase in veteran satisfaction with its virtual care services, particularly the VA Video Connect app.
Other

The apparently popular “Acquired” podcast devotes a four-hour (!!) episode to the history of Epic. It doesn’t say much that you and I don’t already know about the company, but it’s aimed at generalists who won’t realize until the hosts finally say it that Epic has never acquired or been acquired and never will be, according to the policy of its board. I downloaded the audio into my AI tool to transcribe, saving me about 3:45 of that ridiculous runtime. I found only a few nuggets:
- The hosts call Judy Faulkner the most successful female entrepreneur in history.
- Judy’s mother was part of a group that won the Nobel Peace Prize. This is the only new fact that I learned.
- Harvard Medical School Professor Warner Slack, MD sent Judy to Boston to learn how to run a business from Meditech’s Neil Pappalardo, who mentored her for three days. The hosts gave Meditech and Pappalardo a lot of props, but surprisingly didn’t mention InterSystems.
- Hosts: “Epic basically never did hire any business people. It is essentially a big gigantic company of programmers, logicians, implementation people who could be programmers, who would think like programmers. That is the DNA of the company to this day.”
- Epic won the Kaiser deal because Carl Dvorak knew that system architecture and performance was a big deal and pulled a team all-nighter to model it out in Excel using Kaiser’s data, which Cerner didn’t do. Kaiser wanted equity, so Cerner offered 10% of the company while Judy said no, that wouldn’t be good for Epic, its customers, or Kaiser.
- [Hosts on the VA contract] “Talking to Epic customers and CIOs in the research, they are like down on their hands and knees, thankful that Epic did not win this deal. Because Cerner just got dragged so into the muck … your founder and your leader is passing away in the midst of this very complex process. After that, Cerner cycles through a whole bunch of different leaders over the next few years. Meanwhile, Epic, kind of unburdened by this DoD and VA shitshow for lack of a better word, just keeps winning deal after deal in the large system providers and in their own way.”
Sponsor Updates
- AGS Health will exhibit at the 2025 ACDIS Conference May 4-7 in Orlando.
- CereCore publishes a new case study titled “Better User Satisfaction, Valuable Focus and Confidence Restored with Knowledgeable IT Service Desk.”
- A new Black Book Research survey finds that healthcare organizations are accelerating plans to shift from traditional revenue cycle outsourcing to AI-powered RCM platforms.
- The “This Just In” podcast features Arcadia Chief Strategy Officer Aneesh Chopra.
- Optimum Healthcare IT launches the first episode of its “Visionary Voices” podcast featuring guests from Northeast Georgia Health System.
- Capital Rx will present at the Business Group on Health Annual Conference April 22-24 in Nashville.
- Divurgent names Patricia Allvin (MLH Healthcare Consulting) senior director of client service.
Blog Posts
- Embracing Coding AI: A Strategic Vision for the future (AGS Health)
- CIOs Reveal Insider Initiatives: Transforming Budget Woes into New Victories (CereCore)
- How AI is Improving Clinical Documentation Accuracy and Compliance (Nym)
- Teamwork & Team Leaders: Making the Difference in Retaining & Supporting Nurses (Symplr)
- Improving EHR Training To Reduce Clinician Burnout (Tegria)
- The journey ahead: Truly transforming healthcare organizations (Altera Digital Health)
- Celebrating 10 Years of Artera: A Decade of Innovation in Patient Engagement (Artera)
- Virtual Care Solutions to Nurse Staffing Shortages (AvaSure)
- Smart revenue cycles start with smart build (Cardamom Health)
- Navigating AI-Driven Cybersecurity Threats in Healthcare with Enhanced Security Operations (CloudWave)
- What My Recent ER Visit Taught Me About Healthcare and Data (Dimensional Insight)
- Pharmacy’s Missed Moment—and What Comes Next (DrFirst)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Follow on X, Bluesky, and LinkedIn.
Contact us.



































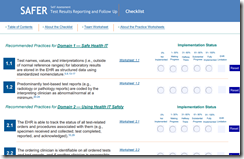
The news about AHRQ is very unfortunate. The AHRQ staff were always excellent to collaborate with. They had an impressive…