News 7/28/23
Top News

Informa Markets will acquire the HIMSS Global Health Conference & Exhibition, the London-based company announced in its six-month financial report.
Informa is a London-based B2B events and publishing company. Its shares are traded on the London Stock Exchange, valuing the company at $11 billion. Some of Informa’s many health-related conferences include Bio-Europe, Pharma Forum, Arab Health, Asia Health, Medlab Asia, Healthcare Innovation Show, and BioMedevice Boston.
HIMSS has not acknowledged the announcement or covered it on its Healthcare IT News site.
HIMSS announced last month that it will move its global headquarters to Rotterdam, the Netherlands.
Reader Comments
From Jordan: “Re: HIMSS Accelerate. Seems to be offline.” I tried logging in, resetting my password, and creating a new account over a couple of days, all with no result. I’ve emailed the HIMSS press contact.
From Bean Me Up: “Re: HIMSS. Why haven’t they filed their IRS Form 990 for non-profits? They aren’t saying anything about selling the annual conference despite the news, so their financials would certainly be interesting.” The most recent annual IRS Form 990 for HIMSS covered from July 1, 2020 through December 31, 2020, when it moved its fiscal year end to December 31. I have not seen the filings that were due on May 15, 2022 (for FY2021) and May 15, 2023 (for FY2022), although I seem to recall asking HIMSS for those forms a few months ago.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
Kettering Health’s CMIO and its oncology product owner did an outstanding webinar in which they described how the health system uses Volpara Health’s technology, seamlessly integrated with Epic, to perform cancer risk assessments and create personalized treatment plans. It held my attention throughout, and I enjoyed seeing screenshots of how it works for clinicians and patients. Nice job, Albert Bonnema, MD, MPH (who is a former US Air Force CMIO and USAF genomics research lab chief) and Chris Yuppa.
Acquisitions, Funding, Business, and Stock
Remote monitoring and digital therapeutics technology vendor Biofourmis lays off 120 employees, 48 of them based in the US.
Sales
- Student health EHR vendor Medicat announces that an unnamed Major League Baseball team will implement its product to manage its mental health initiatives.
People

Divurgent hires Jeff Fuller, MS (CipherHealth) as VP of analytics delivery.
Recently retired Vanderbilt University Medical Center pediatric informaticist Stuart Weinberg, MD died July 18. He was 63.
Announcements and Implementations
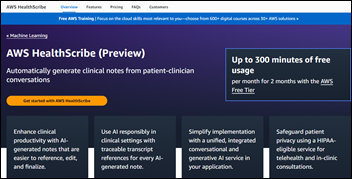
Amazon Web Services announces AWS HealthScribe, an API-powered cloud service that allows developers to create applications that convert audio recordings of doctor-patient discussions into clinical documentation that can be entered into the EHR. The product will focus initially on general medicine and orthopedics. Amazon says that 3M’s MModal, Babylon Health, and ScribeEMR are already using the product.
AWS also announces the rollout of AWS HealthImaging, a developer’s API service for creating medical imaging applications.
Blue Shield of California will use Microsoft Azure to consolidate member, provider, and payer data into a near-real time view that will allow personalizing services and closing care gaps. Its first use case is creating an integrated digital health record of conditions, labs, medications, ED visits, utilization, and plan coverage, which will support care coordination, transitions of care, and connecting members to social services.

Essentia Health’s new St. Mary’s Medical Center in Duluth, MN will feature Sonifi Health’s engagement platform.
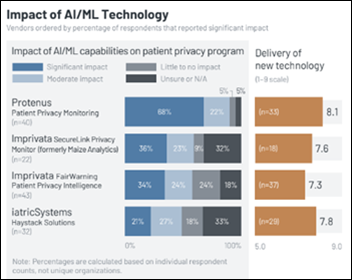
A new KLAS on patient privacy monitoring solutions finds that Protenus tops the four-product performance ranking among its user base of mostly large Epic sites that also report high impact from the company’s use of AI/ML capabilities. Imprivata’s scores initially dropped following acquisitions, but are improving.
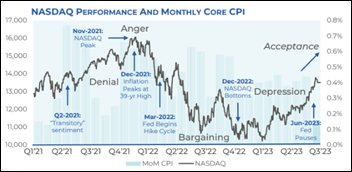
I always await the always superbly written and surprisingly engrossing health IT market reports from Healthcare Growth Partners, fidgeting with impatience like a Netflix series viewer who can’t wait for a fresh season to drop. Here are some high points from its new Midyear Market Review:
- HGP says the market is working through the five stages of grief related to inflation and interest rate hikes, noting the “loss” of a 10-year cycle of easy money that created ever-rising valuations and transaction volume that peaked with COVID euphoria.
- Investors have reached the acceptance of the new normal and are anxious to get back in the game, as hope re-emerges.
- Distressed companies are bringing assets to market via carve-outs and divestiture, in some cases involving underperforming acquisitions that were a mistake in the first place. Examples: Pear Therapeutics and Olive completing asset sales and Centene exiting Apixio.
- The lower risk appetite has resulted in more structured deals instead of cash purchases, adding equity consideration and earn-outs.
- Money-losing companies are out of favor, but not dead, even as the market shifts away from growth at all costs and demands a clear path to profitability.
- No health IT companies have gone public via IPO or SPAC merger in 2023, with HGP also noting that none of the 16 health IT companies that took the SPAC route have increased share price and several have resorted to reverse stock splits after tanking share price threatened de-listing.
- COVID euphoria ended in Q1 2022, and while the Nasdaq is a valid indicator of recovery, it is misleading because it is weighted by market cap, with just seven giant companies making up 50% of the index.
- The market is ideal for buyers who are brave enough to acquire on the market’s reset, as even with the possibility of ongoing high interest rates, as “sitting on the sidelines is not an effective strategy.”
Government and Politics

Sen. Elizabeth Warren (D-MA) is investigating Google’s “aggressive” attempts to gain access to data from the military’s Joint Pathology Center for use in building healthcare AI. ProPublica previously reported that Google offered to digitize the military’s 55 million pathology slides in return for exclusive access to the archive.
Privacy and Security
Federal health services technology contractor Maximus confirms via an SEC filing that Russian hackers accessed the protected health information of up to 11 million people by using a known exploit in the MOVEit Transfer secure file transfer program. The MOVEit vulnerability resulted in Harris Health sending letters last week to 325,000 patients whose records were exposed.
Two Vanderbilt University Medical Center patients whose medical records were turned over to Attorney General Jonathan Skrmetti in an investigation of billing for services to transgender patients file a class action lawsuit against VUMC. The lawsuit claims that VUMC violated its own privacy policies and HIPAA in failing to push back on the state’s civil investigative demands.
Sponsor Updates
- Wolters Kluwer Health’s Sentri7 clinical surveillance and Simplifi+ pharmacy compliance solutions receive a 2023 Black Book award for highest client satisfaction.
- Netsmart integrates Rethink Behavioral Health’s autism care resources and applied behavior analysis clinical solution with its CareFabric platform.
- Divurgent releases a new Vurge Podcast, “Bridging Healthcare Disparities Through Technology.”
- First Databank names Derrick Oliphant cloud operations manager, Varun Reddy associate product manager, and Matt O’Connor regional manager.
- Healthcare Triangle’s ransomware protection and prevention initiative draws initial support from multiple health system clients.
- InterSystems releases a new Healthy Data Podcast, “Delegation in an Epic Conversion.”
- Medicomp Systems releases a new “Tell Me Where It Hurts” podcast with Grace Cordovano of Unblock Health.
Blog Posts
- Checklist: How Strong is Your Hospital’s Data Strategy? (Dimensional Insight)
- Behind the scenes of a hospital ransomware attack (Fortified Health Security)
- Leveraging Content to Support Virtual Care (Healthwise)
- Generative AI in Healthcare: Looking to the (Near) Future (Impact Advisors)
- The Pan-Canadian Interoperability Roadmap: Does it get us where we need to go? (Nordic)
- Predictive Analytics in Healthcare: An Overview (Lucem Health)
- Building a Digital Support Ecosystem for Chronic Health Conditions (Medhost)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.


































I've figured it out. At first I was confused but now all is clear. You see, we ARE running the…