News 11/22/24
Top News

House lawmakers pass a VA legislative package with its original EHR oversight requirements removed. The bill will move to the Senate.
The originally submitted version would have increased Congressional oversight of the VA’s struggling Oracle Health implementation, which included requiring facilities to return to pre-deployment efficiency before moving on to the next go-live.
A House VA Committee spokesperson said that the EHR provisions were removed during negotiations “due to a lack of political viability in both the House and Senate.”
Rep. Mark Tarkano (D-CA) accused Oracle of using its “army of lobbyists” to kill the EHR requirements. Rep. Matt Rosendale (R-MT) said, “Oracle Cerner bought and bullied their way into getting this bill passed without their company being scrutinized.”
Reader Comments

From Sportsman: “Re: Oracle. This article says it will ‘trounce’ Epic.” This piece is an example of someone who (a) doesn’t know what they’re talking about in healthcare, or (b) is trying to spew hot takes for clicks and advertiser attaboys. Maybe both. My issues with it are these:
- The author who wrote the article – which is a facts-lite opinion piece — owns the cloud-focused media site that ran it. He is basing his conclusion on Oracle’s size and technology expertise.
- His site sells marketing services, with one of his clients being Oracle and one of his non-clients being Epic.
- Not only does the author have zero healthcare experience, he spent five years as an Oracle PR flack and is a fanboy of Larry Ellison, who he claims recruited him personally.
- Healthcare is an afterthought for Oracle, while it is Epic’s only business. That seems important.
- Oracle Health placed below Epic, Meditech, or both in every Best in KLAS 2024 EHR category. Oracle also finished #3 in a three-horse race in healthcare ERP and scored a dismal 60 versus Epic’s 92 in large hospital patient accounting, with customers raising serious concerns about Oracle Health’s lack of results, product roadmap, and ability to execute.
- He ignores Epic’s massive market share and fanatic customer loyalty and doesn’t mention that Oracle Health is headed south on those scales.
- He says that the entire resources of Oracle have been committed by Larry Ellison, while he’s alive anyway, to address “the entire $16 trillion healthcare industry.”
- He really hates that Epic accuses the former Cerner of interoperability foot-dragging, dramatically concluding that, “to the degree Ellison gives any thought to Epic as he undertakes that mission, Epic’s silly ankle-nipping will only serve to reinforce Ellison’s resolve.”
Notes from Wednesday’s “Oracle Health Inside Access: The Future of the EHR” webcast

The overly gushy host of the webcast ran the charitable foundations of Cerner and now Oracle Health (she has no healthcare or technical experience or education). Oracle Health Chairman David Feinberg, MD, MBA made a somewhat brief appearance from a room with a sweeping view that sent me Googling to see if it was the $18 million LA penthouse that he bought from The Weeknd (it apparently wasn’t, based on celebrity real estate listing photos).
Most of the webcast involved a nicely done demo with product director Jeffrey Wall, MD that had been recorded at the Oracle Health Summit. It was not clear on whether the work in progress that was shown is the new EHR, old Millennium with a facelift, or Oracle’s digital assistant.
- The functions shown were running in a browser and was apparently a mix of live code and mock-ups.
- Oracle’s Clinical AI Agent displays an input bar at the top. The physician clicks the microphone icon to initiate voice input, much like using ChatGPT in voice mode.
- The system covers ambulatory practice only. Non-physician use was not mentioned.
- It can answer questions about the day’s visits and create generative AI summaries of individual patient histories.
- A new concept is an AI timeline of encounters that helps the physician visualize the patient’s history.
- The information that is displayed by the AI references its source.
- The voice operation opens whatever function the user’s question references, and from there it’s clicking and scrolling to interact with the information that is displayed.
- The user interface is visually logical and offers a good presentation of information.
- The user can drill down into individual problems to see history, notes, and meds for that condition.
- It occurred to me in watching the demo that whatever the physician speaks to the AI will be heard by the patient who is in the room, which may be interesting in some cases. Also, the physician will need to stay close to keyboard and microphone.
- Incoming patient messages are displayed with full chart context.
- The physician can ask about medication doses and side effects from Oracle Health-owned Multum.
- Creating a new prescription brings up that user’s most common prescriptions as well as those of physicians like them.
- Patients can enter free text when confirming their appointment or checking in. AI will interpret and route based on what they enter.
- The new EHR will be open and connected as part of an ecosystem that will allow data to flow.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present or promote your o
Acquisitions, Funding, Business, and Stock
Release of information vendor Verisma acquires Olah Healthcare Technology, which offers an enterprise archiving solution.
Clinical collaboration technology company TigerConnect acquires Twiage, whose software supports pre-hospital communication involving emergency medical services.
Sales
- UCHealth chooses competency management software from Kahuna Workforce Solutions.
- Sarasota Memorial Health Care System will implement Epic in a $160 million project, replacing Altera Digital Health’s Sunrise.
People

Chris Penwarden (Minerva Surgical) joins Eagle Telemedicine as VP of sales. He is a West Point graduate who served in combat roles in Iraq and Afghanistan as a US Army rifle and anti-tank platoon leader and company commander before retiring from the military after 14 years due to injuries sustained in combat.

HarmonyCares hires Jonathan D’Souza, MS (MedArrive) as chief product and technology officer.

Community Medical Centers President and CEO Craig Castro will retire after 22 years with the organization. He joined the health system in 2002 as SVP/CIO and held that position for 10 years before adding the CEO role at Clovis Community Medical Center.
Announcements and Implementations
Veradigm launches an ambient scribe platform for its EHR using AvodahMed’s generative AI.
ED physicians at Canada’s Alberta Health Services are testing a doctor-created AI scribe in a two-year project that is being funded by a Canadian Medical Association grant.
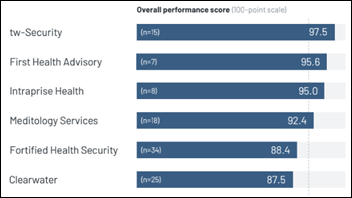
KLAS looks at security and privacy consulting and managed service providers.
Other

Fun fact: an article about businesswoman and sports teams owner Michele Kang’s $30 million women’s soccer donation mentions that she made her money in health IT. She was founder and CEO of federal IT healthcare contractor Cognosante, which she sold to Accenture Federal Services earlier this year (she had previously sold the company’s consulting practice to NTT Data). She emigrated from South Korea to the US as a student at the University of Chicago and then Yale.
Sponsor Updates

- Healthcare IT Leaders staff bring holiday cheer to Head Start families at the YMCA of Greater Kansas City with Christmas Tree Santas.
- Artera promotes Adrianna Hosford to chief communications officer and head of marketing, and Zach Wood to chief product officer.
- FinThrive announces new capital to support its accelerated growth.
- The Northern Virginia Technology Council recognizes DrFirst as a top technology leader for the fifth year in a row.
- ACOs participating in the Medicare Shared Savings Program that use a combination of Arcadia and CareJourney solutions achieve one-and-a-half times more savings compared to other ACOs nationally.
- Health Data Movers releases a new “Quick HITs” podcast titled “Dr. Aaron Neinstein on AI, Automation, and the Future of Healthcare.”
- Netsmart announces that several of its solutions, including its EHR for public health, have received Level 2 Certification from the Texas Risk and Authorization Management Program.
- Ellkay profiles Cook Children’s Health Care System SVP and CDIO Theresa Meadows as a part of its “Women in Health IT” series.
- Wolters Kluwer Health and the Australian College of Mental Health Nurses will partner to develop mental health resources available via the Lippincott Procedures Australia educational resource.
- Five9’s GenAI Studio wins Best New Product from the 2024 Big Awards for Business.
- Meditech lists its customers that have been recognized as CHIME Digital Health Most Wired.
- Fortified Health Security names Dow Perkins senior threat defense analyst, Kerry Shelton threat assessment analyst, and Guy Denton penetration tester.
- CHIME recognizes Impact Advisors co-founder and Managing Partner Andy Smith with its Foundation Industry Leader Award.
- Linus Health Director of Cognitive Science Ali Jannati, MD, PhD receives the 2024 Neuropsychopharmacology Editor’s Award for a Review from the American College of Neuropsychopharmacology.
- MRO publishes a new case study, “Healthcare Providers Explore Payer Direct Access to EHRs, but Most Are Still Awaiting the Benefits.”
Blog Posts
- Automate Your Fax Inbox with Image AI Assistant (EClinicalWorks)
- Medicare Bad Debt 101 (FinThrive)
- Understanding Communication Styles: A Guide for Customer Service Agents (Five9)
- Elevating data security with HITRUST certification, HIPAA compliance, and employee awareness (Healthmonix)
- Quality, Workflow, and Health Information Exchange (Konza National Network)
- Meditech customers share their innovations with the healthcare industry (Meditech)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.






































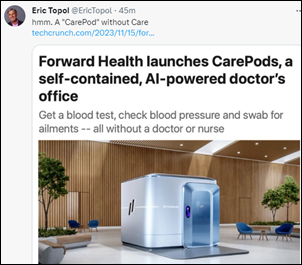
Thank you for the mention, Dr. Jayne — we appreciate the callout, the kind words and learning more about the…