News 7/21/21
Top News

WebMD acquires The Wellness Network, which offers advertising-supported patient education videos and broadcast channels for hospitals.
Reader Comments
From A Concerned Citizen: “Re: HIMSS21. Will it be cancelled, or just set records for poor attendance? Between the delta variant and the White House report that ranks Las Vegas the most dangerous of all metropolitan areas, registration must be falling quickly.” A couple of readers said their employers have instituted policies that will prohibit their planned attendance. I was about to say that it’s too close to the conference kickoff to contemplate shutting down the live component, but then I recalled that HIMSS20 was cancelled March 5, four days before it would have started. A virtual-only conference is the backup plan, but I don’t think that HIMSS could survive losing its main money-maker for two consecutive years. I predict the show will go on, even with an attenuated audience.
From Tom Paine: “Re: IBM Watson. Former CEO Ginny Rometty is to blame for overhyping it. It was presented as the great hope for IBM, while more important initiatives like the cloud fell further behind.” Rometty should have been skeptical about the Watson hype given that her degree was in computer science and electrical engineering and her IBM background was mostly spent in technical roles. IBM is usually late to parties at which competitors have already taken the best seats, so maybe the draw of being an early entrant into AI was appealing. The company’s biggest Watson mistake was probably choosing healthcare as its showcase, a hill that many swaggering tech companies have died whimpering on.
HIStalk Announcements and Requests

I found the Clear Health Pass app frustrating to use for HIMSS21 vaccination verification, especially since my submission is stuck in “pending verification” status. I strongly recommend using Safe Expo Vaccine’s online option instead, as recommended by reader Susan Newbold. The submission page is 1990s clunky, but it took seconds to submit photos of my driver license and vaccination card and then just another 1-2 minutes to have it confirmed by email.
More evidence of the decline of US journalism – it seems that every news website now features cursory “product reviews” that hope to entice readers to click to buy, generating an affiliate commission for the site. The link is almost always to Amazon because it pays those commissions reliably and people are more likely to buy from Amazon anyway, meaning that non-Amazon products are ignored along with other sites that offer the same item cheaper.
Webinars
July 28 (Wednesday) 1 ET. “Stop running from your problem (list): Strategies for streamlining the EHR’s front page.” Sponsor: Intelligent Medical Objects. Presenters: Amanda Heidemann, MD, CMIO, CMIO Services LLC; James Thompson, MD, physician informaticist, IMO. How can clinicians mitigate the longstanding EHR problem list challenges of outdated or duplicative entries, rigid displays, and limited native EHR capabilities? The presenters will describe how to analyze current problems, create a problem list governance strategy, and measure improvement progress.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
The Massachusetts EHealth Collaborative dissolves and distributes its assets to six public charities. The organization says it has completed its work and fulfilled its mission related to interoperability, standards development, and health IT policy.
Sales
- Georgia-based ACO TC2 will implement Jvion’s Avoidable Admissions technology.
- St. Bernard’s Hospital (AR) selects NICUtrition clinical decision support software from Astarte Medical.
- North Mississippi Health Services will implement Picis Total Perioperative Automation software with Envision Analytics from Picis Clinical Solutions.
People

Adam Laskey (Cerner) joins EverCommerce as GM of EverHealth.

VitalTech names Chad Haynes (Cerner) as chief commercial officer.

John McCullough (Cleveland Clinic) joins The Chartis Group as principal in its Informatics & Technology practice.

Patricia Daiker, RN (Dragonfly Lights) joins Orb Health as VP of clinical operations.


Signify Health names Sam Pettijohn (Cerner) chief growth officer and Erin Kelly (CVS Health) chief commercial officer.

Industry long-timer Scott Weingarten, MD, MPH (Cedars-Sinai) joins Medicare Advantage insurer SCAN Group as its first chief innovation officer, where he will launch its geriatric primary care medical group.

Shayna Schulz (Blue Shield of California) joins Grand Rounds Health and Doctor on Demand as COO.
Announcements and Implementations
Illinois Bone & Joint Institute begins implementing Epic at its facilities in Illinois and Indiana.
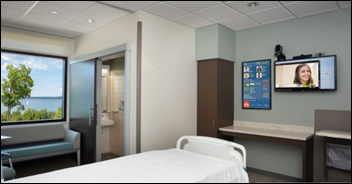
McLaren Health Care implements Medi+Sign’s automated patient communication technology across its network in Michigan and Ohio.
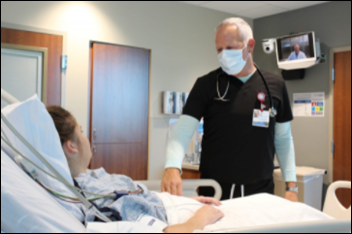
Covenant Health rolls out tele-ICU services at its facilities in Tennessee using technology from Hicuity Health.
InterSystems develops HealthShare Message Transformation Service, enabling users to convert existing data formats to FHIR standards to populate Amazon HealthLake.
Amazon’s AWS machine learning blog profiles Medhost’s migration of all its data to AWS to provide patient access and to support advanced analytics and compliance needs.
Wolters Kluwer announces EmmiEducate, which delivers patient educational material.
Other
JAMA-published research finds that medical debt is the largest source of debt in collections in the US, now totaling $140 billion from the 18% of Americans who hold medical debt that has gone to collection. Total medical debt is likely larger since hospitals are increasingly suing patients rather than selling their debt to collections agencies at a discount. The total also does not include balances owed on credit cards or payment plans. Medical debt is increasing faster in the 12 states that do not participate in the ACA’s Medicaid expansion program (AL, FL, GA, KS, MS, NC, SC, SD, TN, TX, WI, WY).

And EHR trigger analysis of the VA’s corporate data warehouse finds that nearly one-third of patients who were admitted for stroke had been discharged from the ED with seemingly benign headache or dizziness in the previous 30 days. The authors approached the study not to prove the existence or extent of diagnostic errors, but rather to (a) highlight the need to validate the data that appears to prove such problems for such issues as miscoding; and (b) use it as a springboard for reviewing ED workflow and clinician diagnostic methods to reduce future harm from missed diagnoses.
Sponsor Updates
- InterSystems and University Hospital Sharjah celebrate a decade of successful partnerships for digital transformation.
- Infor and Change Healthcare announce their support for the AWS for Health initiative.
- Kyruus describes the use of its ProviderMatch platform by AtlantiCare (NJ).
- Diameter Health has been selected by AWS as a Connector Partner for Amazon HealthLake.
- CereCore welcomes Michael Gagnon (NTT Data) as its first Enterprise Fellow.
- Diameter Health publishes a case study featuring HealtheConnections, “Improving Ambulatory Clinical Quality Measurement Using a Consolidated Patient View.”
- The Lifelong Customer Podcast features Dimensional Insight VP of Marketing Kathy Sucich.
- Elsevier Clinical Solutions releases a new Clinical Insights Podcast, “How Well are COVID-19 Vaccines Working in the Real World?”
- Experian Health announces that its Enterprise Health Patient Identifier Solution and Hospital Claims Management Systems have been deemed top-rated solutions in Black Book’s 2021 “Top Client-Rated Financial Solutions Achieving Accelerated Digital Transformation in the Nation’s Healthcare Systems.”
- EClinicalWorks releases a new podcast, “How Population Health Solutions Improve Patient Outcomes and Experiences.”
Blog Posts
- How a family medicine practice protected revenue and served more patients with telehealth (Ability Network)
- What are the economics of remote patient monitoring for your practice? (AdvancedMD)
- Acquire and Secure Medical Images with Mobile Devices (Agfa HealthCare)
- Disaster Preparedness: How Ready Are We for Hurricane Season? (Audacious Inquiry)
- Understanding First Call Resolution and what it means for your healthcare system’s bottom line (Bluetree)
- Pre- and Post-Pandemic: Comparing SNF Quality Ratings (CarePort)
- Advancing health equity: Understanding and meeting the challenges with data (Cerner)
- Reining in Costs by Closing Care Gaps: Next Steps for Payers (Collective Medical)
- Reimagining Healthcare Technology at NCPDP 2021 (CoverMyMeds)
- Insights from the Inside: CHIME Members Discuss the Future of Managed Services (Cumberland Consulting Group)
- Winning the Medical Information Game (EClinicalWorks)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.










































One solution would be federal (or state) requirements; but more ideally health systems would view their digital patient tools as…