To take the counterpoint to the "don't just schedule more visits" argument - it depends on if you're looking at…
News 7/17/20
Top News
Congressional Democrats criticize HHS for issuing a no-bid, $10.2 million contract in April for developing a hospital bed and supply tracking database to TeleTracking Technologies, the Pittsburgh-based hospital equipment and bed tracking vendor.
HHS has ordered hospitals to submit their COVID-related capacity, patient count, and supply information to the TeleTracking system, called HHS Protect, instead of the CDC’s National Healthcare Safety Network (NHSN), starting this past Wednesday. The administration says CDC’s database is outdated and requires manual entry that delays analysis.
CDC Director Robert Redfield, MD said Wednesday that CDC provided input into developing HHS Protect, which previously accepted both data that was submitted directly from hospitals as well as extracts from NHSN. Redfield says that requiring hospitals to send their data directly to HHS Protect will reduce duplicate reporting, help HHS make quick field changes, and allow CDC to focus its system on capturing reports from nursing homes.
Redfield says that CDC and state and local health agencies will have access to HHS Protect, adding that CDC will continue to provide daily updates and dashboards. Several outside sites use CDC’s dashboard for modeling, such as school reopening readiness.
Meanwhile, CDC’s hospital capacity dashboard went offline on Wednesday, the final day in which hospitals could submit data to NHSN.
UPDATE: HHS Assistant Secretary of Public Affairs Michael Caputo said Thursday afternoon that HHS has ordered CDC to restore the COVID-19 hospital dashboards that CDC “withdrew from the public Wednesday.” However, the dashboard indicates that information will not be updated after July 14.
Reader Comments
From Data Deliverance: “Re: HHS changing hospital-submitted operational data from CDC to HHS. The new database isn’t publicly visible. Can the public use other dashboards, such as the one from Johns Hopkins?” HHS collects daily hospital reports about beds, ventilators, cases, admissions, ED visits, remdesivir inventory, and details about staff and PPE shortages. Most of this information has minimal overlap with the infection dashboards published by Hopkins and other sites that I assume use data that hospitals have submitted to state health departments.
From Epic Historian: “Re: Kaiser Permanente. Early on they were considering both Cerner and Epic. Cerner offered a complex plan to rebate KP the software cost in the form of Cerner company shares, basically giving them the software for free (UPMC may have fallen for this). KP decided to pick Cerner for inpatient and Epic for outpatient (since it was already being used in some regions), and they asked Judy end Epic to run the integration. She told them to forget it, just use Cerner because one vendor is better than two. KP realized what she was saying and took Epic even though the inpatient system was pretty untested back then.” Unverified, but fascinating. This was in response to an email conversation I had with EH in which I described one instance (there were actually two, but I just now remembered the second) in which we as a big health system seriously pondered whether it would be cheaper to buy our fading vendor of choice as a company instead of their product, or if we did buy the product, whether our contractual demands that they were desperately willing to accept might drive them out of business anyway.
From Kay: “Re: HIStalk. I’ve enjoyed most of the 50-year career I’ve had in health IT and am lucky to have found something I loved. I’m finally retiring and will miss the industry and the wonderful people. You have made a huge difference to me and how I was able to do my job. You are the best. Ever. I want to thank your family for sharing you with us. By the way, I’m not retiring from reading your blog. Stay safe and well and clever and endlessly interesting.” I excerpted some of Kay’s comments, without including personal details, purely to thank her for those thoughts (hold on, got something in my eye here) and to wish her a happy retirement as an industry pioneer, a concept that I hope she celebrates both as the beginning of a fresh chapter as well as a reward for completing the previous one. I’m always uplifted to hear from someone who has enjoyed their career and their simultaneous personal life that raced by while they were pursuing it – it’s a lot easier to continue gratification than to catch up from deferring it.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
Digital access and care navigation company Gyant raises $13.6 million in a Series A investment round. The company launched a COVID-19 digital screening tool several months ago with development help from investor Intermountain Healthcare that has since been deployed by 16 healthcare organizations.

Boston-based care coordination software startup Cohere Health launches with a $10 million Series A funding round. The company offers care paths, care journey recommendations, and physician behavior change. CEO Siva Namasivayam, MS, MBA was previously CEO of SCIO Health Analytics and an executive with Perot Systems.
Cerner says it will keep employees working from home for at least several more months, pushing back its phased plan to bring up to 50% of employees back to office-based work.

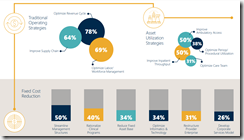
The six-month health IT review of Healthcare Growth Partners says that while COVID-19 has accelerated the shift to “hospitals without walls,” M&A transaction activity has slowed a bit and will likely stay that way through the end of this year, although not as much as in other industries. Underlying health IT investment sentiment remains strong among private equity firms. Private equity investors generally see COVID-19 as neutral with regard to valuations. The most common COVID-19 strategies that companies are using include applying for federal government relief (40%), accessing additional capital (30%), and delaying payables (30%). Many of them are furloughing or laying off employees or imposing pay cuts.
Sales
- Banner Health signs up for Cerner’s revenue cycle system, expanding its Millennium implementation.
- Boulder Community Health (CO) will implement data and analytics, RCM, and care coordination services from Optum.
- Virginia Mason Health System (WA) will use supply chain services and cost-management analytics from Premier.
- Parkview Medical Center (CO) will go live on Epic through a software-sharing arrangement with UCHealth.
People

Appriss Health promotes Krishan Sastry, MBA to president and CEO. He replaces Michael Davis, who will remain as executive chair.
Tom Underman (Accuray) joins Loyale Healthcare as VP of enterprise sales.
Announcements and Implementations
Banner Health implements acute-care telemedicine capabilities developed by VeeMed and Intel across its 28 hospitals.

Phynd Technologies announces GA of advanced provider search capabilities for patient-facing hospital websites and internal directories.

Vanderbilt University Medical Center profiles its Clickbusters campaign to reduce alert fatigue from Epic-generated best practice advisories. The program, operated by Vanderbilt Clinical Informatics Center, has reduced the nearly 500,000 weekly generated alerts by 10% and has set a goal of having users act on the recommendations 30% of the time instead of the current 8%. VUMC has also added a feature to allow clinicians to score their satisfaction with individual alerts and add suggestions for refining them that are sent to a review team.
Urgent care provider Remedy is working on virtual care solutions with Redox, one of 13 virtual care customers Redox has added to its network since March in a 46% increase.
A new KLAS report on legacy data archiving finds that Harmony Healthcare IT and MediQuant have a record of satisfying customers that have complex needs, while Triyam and Ellkay customers report getting their projects finished on time and with good communication. Sites that used MediQuant, Galen Healthcare, and Harmony Healthcare IT reported more delays, but some of those customers say it was their own lack of planning and expectation-setting that extended their timelines.
Athenahealth renames its Centricity product line to AthenaIDX, which includes Centricity Business (AthenaIDX), Centricity EDI Services (AthenaEDI), and Centricity Group Management (AthenaIDX). The product line has a long but tortuous history — the former IDX developed and sold the systems for years, GE Healthcare acquired IDX for $1.2 billion in 2005, GE Healthcare sold part of that business to private equity firm Veritas Capital in mid-2018 for $1.05 billion, Veritas named the acquisition Virence Health Technologies a few weeks later, and Veritas acquired Athenahealth for $5.7 billion a few months later and combined it with the Virence product line under the Athenahealth brand.
Government and Politics
An HHS OIG audit finds that CMS Administrator Seema Verma inappropriately spent millions of taxpayer dollars on contractors — some of them connected to Republican loyalists — who she engaged to polish her public image. CMS had paid more than $5 million to the contractors at above-market rates – up to $380 per hour — before halting the program following Politico’s investigation. CMS has 235 FTEs in its Office of Communications. Politico previously reported that Verma had directed contractors to craft her speeches, book her media appearances, obtain invitations for galas, and work to get her included on “Power Women” lists. HHS accepted the inspector general’s recommendations, but Verma disputed the findings and scolded OIG for investigating her when CMS is dealing with coronavirus. HHS Assistant Secretary for Public Affairs Michael Caputo, an advisor to President Trump, responded that the White House has confidence in Verma, but not his own department’s inspector general. Note: that acting inspector general is Principal Deputy Inspector Christi Grimm, who drew the White House’s ire and the nomination for her replacement in April after HHS OIG published results of a 300-hospital survey that indicated widespread shortages of PPE.
COVID-19

Oklahoma Governor Kevin Stitt, who was among the majority of attendees of President Trump’s June 20 rally in Tulsa who refused to wear masks, becomes the first state governor to test positive for COVID-19. He attended state meetings unmasked after being tested while awaiting results, forcing state and local officials who were exposed to him to begin their own testing and self-isolating.
New research using EHR data finds that, contrary to previous speculation, blood type has little impact on COVID-19 susceptibility or outcomes.
University of California Health uses de-identified patient data from its Epic system to create a database for COVID-19 treatment research.
The UK’s cybersecurity center warns that a Russian hacking group is targeting COVID-19 vaccine research and development organizations in the US, UK, and Canada to steal their intellectual property.
White House Press Secretary Kayleigh McEnany says in a press briefing on school reopenings that “the science should not stand in the way of this.”

In Bangladesh, a hospital owner is arrested for selling migrant workers certificates that they tested negative for COVID-19 without actually testing them. He sold 10,000 of the $59 certificates that allowed his untested customers to work in Europe as restaurant workers and grocery store clerks. The hospital owner, who sports a long criminal record, was arrested while trying to cross the border into India dressed as a woman. Two other doctors were previously arrested in Bangladesh for issuing thousands of phony certificates.
Other
A small survey of health systems by The Chartis Group finds that 40% expect it to take at least a year to return to pre-pandemic patient volumes, and that 45% will reduce expenses by at least 10% during that time.
Weird News Andy acknowledges that stories like this are hard to swallow. Japanese doctors resolve a woman’s throat irritation by removing a sashimi-transmitted parasitic worm from her tonsils. You’re welcome for me not showing you the photo.
Sponsor Updates
- Frost & Sullivan recognizes Wolters Kluwer Health as a Frost Radar global leader in AI for healthcare IT.
- Healthwise names Cydni Waldner (Hawley Troxell Ennis & Hawley) general counsel.
- Hyland Healthcare partners with Life Image to optimize data and imaging access between providers and patients.
- The Philadelphia Business Journal honors InstaMed CFO Frank McAnally with its CFO of the Year Award.
- Black Book ranks Imprivata as the top company for client satisfaction for identity governance solutions.
- Redox has increased its roster of virtual care customers by 46% over the last several months.
- Loyale Healthcare parent company RevSpring integrates Loyale’s payment facilitator program with its Merchant Services offering.
- PMD adds a Web-based telemedicine option for patients who lack access to or don’t feel comfortable using mobile devices.
Blog Posts
- How Grady Improved Patient Safety in the ICU with Computer-Guided IV Insulin Therapy (Glytec)
- CGH Medical Center Finds Root Cause and Resolves End-User Citrix Performance Issues in Minutes (Goliath Technologies)
- The Best Virtual Care Setup for Your Clinicians (Access)
- Caring for caregivers: UNC’s Heroes Health Initiative supports healthcare workers’ mental health (Google Cloud)
- Employee Engagement During COVID-19: Using Culture to Manage Stress, Maintain Productivity (Health Catalyst)
- Pitfalls of Long Prescription Renewal Turnaround Times (Healthfinch)
- The Key to Improving Coaching Efficiency and Member Outcomes (Healthwise)
- Hey Epic – Epic’s New Voice Assistant (Optimum Healthcare IT)
- AHIP: Payers are Addressing Socioeconomic Needs During COVID-19 and Beyond (Imat Solutions)
- In the COVID-19 battle, did we leave our best players on the bench? (Imprivata)
- How to avoid expanding IT costs (Infor)
- Information Blocking: To Block or Not to Block (Nordic)
- 5 Ways to Increase Revenue with Healthcare Business Analytics (Ingenious Med)
- At a glance: Medical coding system updates for 2020-2021 (Intelligent Medical Objects)
- Healthcare’s COVID-19 Secret Weapon – Innovation (Loyale Healthcare)
- The Pros and Cons of Hiring Individual Contract Physical Therapists (MWTherapy)
- 10 Essential Elements of Wound Care Documentation (Netsmart)
- Human Connections and Telehealth: Navigating the COVID-19 Era (PMD)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.





Re: Parkview Medical Center going to Epic – I’m very excited to hear this! I used to teach across the street from the other hospital in Pueblo and many of my students and their families bounced between Parkview and St. Mary Corwin (Centura, on Epic) for their care. I imagine Care Everywhere will make it a bit smoother to coordinate care between the two entities once Parkview is live.
Changing Saddles While Swimming the River
Imagine swimming a horse across a river, then having someone change out your saddle halfway through the crossing. You’re going to go swimming and not in a good way. This analogy is how I see changing reporting on CV-19 from the CDC to a private database run for the CV-19 Task Force. It isn’t going to go well, unless the purpose of the change is to make sure we can’t tell up from down during this pandemic.
What makes me say this?
This is first and foremost an interoperability project, receiving data from enumerable sources, through multiple formats. The variable set here is also quite complex, with different vendors, HL7 and CCDA feeds, fax, and who knows what else. On top of that, you have exchange relationships that have been established over decades. The requirements, design, coding and encoding, plus testing required to make this system work is and was quite intense.
If someone asked me to estimate a chaos project like this I would assume it would be a multi-year phased endeavor, culminating in dual reporting until a cross over date is established, published, promoted, and agreed upon.
None of that happened here
One would assume that there is collaboration between the existing agency and the agency receiving the data. That would imply that there was agreement that such a project was needed. It would imply that the existing agency recognized that it had strayed from its core mission. That would imply that the new organization would do a better job than the existing organization.
None of that is true here
Changing the method of reporting on two days notice while we are still in the first wave of this pandemic has no value. Unless someone sees value in a 50-70% reduction in reported cases. Unless someone sees value in a 50-70% reduction in reported deaths. Unless someone sees value in a significant reduction in the positivity, hospitalization, ICU, and ventilator numbers. Unless someone sees value in hiding the number of tests performed or the turn around rate for those test results. Unless someone sees value in not having the data on what levels for precursors, reagents, swabs, or PPE are. Unless you don’t want to know how many ICU beds remain.
Seems transparent and obvious
Is this even the problem space that this company is in, with only 15 or 20 positions open how are they able to take this project on? Awarding a 10 million dollar no bid project in April, 75 days ago, and turning it on with 2 days notice is plain and simply not going to work. I don’t even believe it is intended to work. I do believe there is a desire to further politicize data to obfuscate the current state of the epidemic.
Is this cronyism or malfeasance?
I was always told to never assign to malice that which can be attributed to incompetence. In this case I believe there may be equal parts of both
The KP story is correct. Neal never, ever forgave them.
I’ve been saying this since she got the job, Seem Verma cares more about what the president who appointed her thinks, than the needs of CMS beneficiaries. In my decades getting CMS bulletins, this is the first CMS administrator who spends considerable time praising her great president for whatever the topic of the bulletin is. This president wants to take away healthcare from tens of millions of Americans in the middle of this epic pandemic, and privatize her very organization. She should be protecting her beneficiaries, not the president! This audit proves what I thought, image is everything, policy and work content come last.
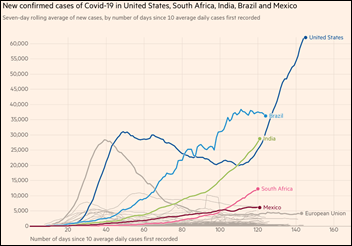
Raw numbers for COVID-19 cases are interesting, but a country with a large population and a low infection rate could still have high numbers. Per capita numbers provide more insight (IMO). Currently, the US, Brazil, and South Africa have the highest rates of infections (cases per one million people). In the US, the rate climbed quickly & streadily, leveled off, and has begun climbing again. This site (https://ourworldindata.org/coronavirus) offers a variety of data views.
Re: From Kay: “Re: HIStalk.”
Ditto.