News 1/23/26
Top News

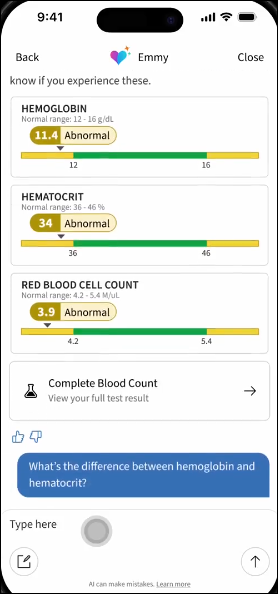
ECRI publishes its “Top 10 Health Technology Hazards for 2026,” with misuse of chatbots topping the list.
ECRI says that unregulated chatbots give users expert-sounding responses, but have offered incorrect diagnoses, recommended unnecessary tests, promoted questionable supplies, and based answers on body parts they made up.
HIStalk Announcements and Requests
Companies exhibiting at ViVE and/or HIMSS, you are about to spend a small fortune on a well-lit, carpeted rectangle that you will occupy for a few exhausting hours while handing out geegaws. For a tiny fraction of that spend, you can claim a different rectangle, this one virtual and this one lasting 365 days, on HIStalk. It is read obsessively by the people who buy, influence, complain about, and occasionally approve health IT purchases. Black Book Research, in a health tech media analysis that found this amateurish and cynical site to be #1 for industry trust and influence, puts it this way: “HIStalk stands out for its influence, independence, and continued relevance to the decision-makers shaping the future of health IT.” Contact Lorre, who has a soft spot for new sponsors that sometimes leads her to offer perks that she glosses over when telling me.
Listening: Porcupine Tree, a 40-year-old English progressive rock band whose “In Absentia” popped up at me.
Sponsored Events and Resources
Live Webinar: February 18 (Wednesday) 2 ET. “From Blind Spots to Insights: Gaining Real-Time Visibility into Healthcare Risk.” Sponsor: CloudWave. Presenters: Jacob Wheeler, MBA, director of sales engineering, CloudWave; Mike Donahue, chief operating officer, CloudWave. Resilience starts with the ability to see clearly, across every endpoint, cloud workload, user, and clinical system. Join CloudWave’s cybersecurity leaders for an in-depth session on how real-time visibility transforms your ability to detect threats early, respond decisively, and strengthen resilience across the care ecosystem. Attendees will learn the practical steps that hospitals can take to move from reactive defense to resilient action.
Publication: HIStalk’s Guide to ViVE 2026 lists the activities of sponsors at the conference.
Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock
Harmony Healthcare IT acquires Meditech solutions provider Blue Elm.
OpenEvidence confirms earlier reports that it recently raised $250 million in a Series D funding round that values the company at $12 billion. The company says that physicians used its system to treat 100 million patients last year and requested 18 million clinical consultations in December 2025 alone.
People


Health data management platform vendor Health Chain names Eric Rosow, MS (Conduce Health) as CEO and Reed Perry, MBA (Availity) as chief commercial officer.

Valerie Mondelli, RPh, MBA (Iodine Software) joins DrFirst as chief commercial officer.
Announcements and Implementations
VectorCare launches Smart on FHIR as a Service, which incudes a no-code workflow builder and developer tools for building and deploying EHR-embedded applications.

The Washington Post covers Epic’s lawsuit that alleges that Health Gorilla knowingly provided treatment access to patient records by law firms that were looking for malpractice plaintiffs.
In England, Slingshot AI takes its therapy chatbot down over uncertainty about its compliance with medical device regulations. The company launched the therapy bot Ash in mid-2025.
Government and Politics
The federal government’s Health Information Technology Advisory Committee (HITAC) will resume its meetings on February 19 following a year-long hiatus that was imposed by the White House. Both co-chairs of HITAC, which advises ASTP/ONC, resigned last week. The committee is scheduled to meet four times in 2026.

Epic files an answer to a Texas lawsuit that alleges that the company is a monopoly and violates Texas laws by blocking parents’ access to their child’s Epic medical records. In its response:
- Texas has not substantiated its claim that Epic is a monopoly.
- The state’s presumption that antitrust laws require Epic to provide free API access to any company, including competitors, is not supported by law.
- Antitrust laws do not prohibit Epic from sharing its software update plans with customers, as the lawsuit alleges.
- Despite a six-month investigation by State Attorney General Ken Paxton, the complaint relies on dated press releases, blog posts, and excerpts from Particle Health’s lawsuit against Epic.
- Epic created a guide that told its customers how to comply with the new Texas law about parental access, but ultimately those customers control access to patient records.
- The lawsuit does not identify any Epic customer that has not complied with the law.
- Epic’s response concludes, “What appears to be going on here is that the State has decided to target Epic over a politicized issue regarding proxy access that Epic does not belong in the middle of. The State confirms as much in its press release, calling Epic a ‘woke corporation’ that supposedly “undermines” parents’ rights. That simply is not true.”
Sponsor Updates
- Springhill Medical Center goes live on Altera Digital Health’s Sunrise 25.1.
- Black Book Research releases two new reports to help rural hospitals and critical access hospitals convert state awards into audit-ready implementation and accelerate vendor selection.
- Ellkay sponsors the 2026 AdvancedMD Sales Kickoff.
- Meditech announces Expanse Outpatient Therapy.
- Findhelp adds mental and behavioral health provider data company MiResource to its Behavioral Health Network.
- Fortified Health Security will host a roundtable dinner focused on current healthcare cybersecurity trends and patient protection strategies January 27 in Cincinnati.
- Health Data Movers will sponsor the CHIME Innovation Summit February 4-6 in Orlando.
- MRO releases a new report titled “2026 State of the Industry: Navigating Health Policy and Market Shifts with Smarter Data.”
Blog Posts
- Innovation starts with strong digital foundations (Altera Digital Health)
- Why Enterprise Healthcare Faces Different EHR Challenges in 2026 (Bizmatics)
- C-Suite Briefing: Top Health IT Trends and Takeaways from the 12th Annual HIT Industry Outlook Report (Med Tech Solutions)
- Epic Space Bridge – An HL7 Interface Message Transformation Solution (CereCore)
- What Healthcare Providers Need to Know About Qualified Overtime Reporting (Healthcare IT Leaders)
- Ensuring Success During Your Epic Refuel Project (Impact Advisors)
- Finding the Right Balance for Operating Room Utilization (LiveData)
- VBC under pressure: Five insights from the front lines (Navina)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Follow on X, Bluesky, and LinkedIn.
Sponsorship information.
Contact us.






































RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…