Monday Morning Update 5/4/15
Henry Chao, the CMS CIO and deputy director who led the rollout of Healthcare.gov, has retired. He was little noticed until a September 2014 House report on the site’s failure, which quoted emails from former HHS CTO Bryan Sivak that characterized Chao as being in way over his head to the point that HHS plotted to hijack the project to try to salvage it. Chao reported to CMS CIO Tony Trenkle, who hightailed it for an IBM federal IT executive job just a handful of weeks after the site went down in flames (of taxpayer money).
Reader Comments
From Not So Lucky: “Re: McKesson EIS division. Big layoffs Friday.” Unverified.
HIStalk Announcements and Requests
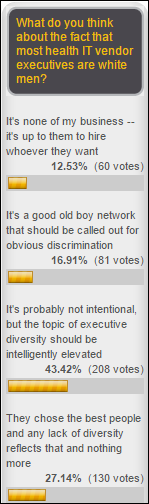
Around 17 percent of poll respondents think that HIT vendors intentionally stack the executive deck against women and unstated minorities, but most of them feel that companies have simply chosen the best people for the job and possibly only need ongoing reminders of the desirability of diversity. Some readers commented that perhaps companies can’t even see the benefit of executive diversity because they’ve never practiced it, while others commented that the “mommy track” may present a more attractive option for women who aren’t very interested in the never-ending hours, travel, and relocation required to move up the executive ladder. Cerner Europe GM Emil Peters referenced the poll on Twitter, saying, “Personally I think it’s a travesty. And I’m going to do what I can to fix it. However, I don’t think it’s by design.” New poll to your right or here: within the past two years, have you had to pay a medically related bill that created at least a modest degree of personal financial hardship?
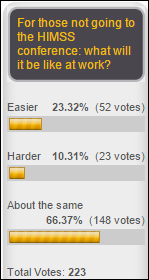
Here another poll that interests me since I see a lot of people playing around with media in ways I don’t quite get: which would be the most attractive way to catch up on a weekly health IT news summary? I personally have never listened to a podcast and don’t anticipate a time that I ever will, so the results will help me figure out if I’m in the Bell curve hinterlands.
Check HIStalk Practice for the Population Health Management Weekly Roundup.
I bought Regina Holliday’s brand new book “The Writing on the Wall” from Amazon and became so engrossed that I read it nearly straight through this weekend. My expectations are modest for healthcare IT-related books given some fairly lame ones, but this one is among the most moving things I’ve ever read, more of a story about love and family, overcoming adversity, and standing up for what’s right than the usual preachy, recycled facts about technology coming from someone who thinks of patients as people and/or customers different from themselves (the big secret: we’re all frightened, marginalized patients at one time or another). If your blood runs above room temperature, I predict you’ll laugh, cry, and get fighting mad at the very system you work within as you read about her life and the untimely death of her husband, but you’ll also find it uplifting and empowering. It would be a great read even without the IT connection. I’ll most likely write a full review shortly since to do less would be a disservice to people who either want or need to peruse it, but here are some excerpts that got me as I learned that Regina’s art is not limited to the visual variety:
We come into this world screaming and owning nothing. We grow and change. The years pass by and we fill with life experience as our homes fill with possessions. Time rolls on and on, but for all of us there is an end. Some will meet their end on highways and some in hospitals, but for most of us the end is the same. We are patients in the end. We pluck at cloth hospital gowns, left with only a few possessions: our watches, rings, and wallets … Hospitals can deconstruct a person as assuredly as I could lay bare a jewelry box. Take any professional adult and remove their clothes and their accessories. Dress them in a threadbare gown that is faded by thousands of wash cycles. Give them a number rather than a name. Confuse them with jargon while applying copious amounts of medication. Then watch them try to navigate the maze of care … I felt like a bright blue inconsequential bird in my Easter dress as I fluttered among the forests of polo shirts, hoodies, and business suits. Conference attendees in the world of medicine have a uniform look. You were welcomed if you wore a suit, tolerated if you wore a hoodie, and ostracized in a church dress. I was not wearing the correct uniform, but I took a deep breath and introduced myself. I would say, “Hello, my name is Regina Holliday. I want to paint about healthcare to improve health policy for patients.” I’d then say that I was inspired to paint by my late husband who very recently died of kidney cancer. I would give them my slip of paper masquerading as a business card. Then tell them to reach out to me via social media or email. Then I’d share the horrific things we had experienced during my husband’s 11-week hospitalization at five different facilities. I would see them step back from me with a brief condolence. A nervous half-laugh would often escape their lips. I was a widow fresh from the graveside asking questions that affect the lives of us all. I was not supposed to be there. They were having a ball and I was death walking among them.

I’ll have more DonorsChoose project updates later, but here’s a photo from Ms. Classen’s intervention algebra class using the calculators we provided. She says, “What we’re able to do now with these calculators is amazing. Many more students are going to get the practice they need to graduate high school and learn to solve difficult problems thanks to you all.”

Here’s a photo of Mrs. Rowe’s third graders using the six iPad Minis we bought them for math study.
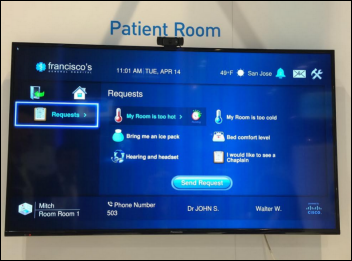
I was thinking about how hospital patient rooms often resemble hotel rooms in being littered with previously popular but now-useless technology components, which in the hotel’s case often includes iPod docking stations and dial-up ports that get used rarely and never, respectively.
Last Week’s Most Interesting News
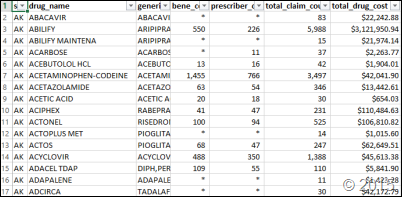
- CMS releases a gigantic Medicare Part D prescribing database for 2013 that includes details on $103 billion of drug spending.
- Teladoc announces IPO plans and files an antitrust lawsuit against the medical board of its home state of Texas for requiring prescribers to see a patient at least once in person before issuing a prescription.
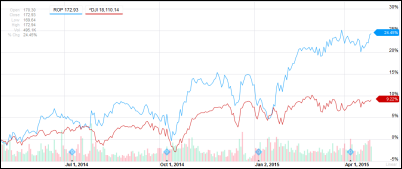
- Anthem books $865 million in Q1 profit, up 25 percent despite its massive data breach during the quarter.
- Imprivata acquires palm vein scanning biometric vendor HT Systems.
- The chair and ranking member of the Senate’s HELP committee follow through on HHS Secretary Sylvia Burwell’s request for help identifying pressing but easily solved EHR-related issues.
- A Brookings Institution report questions why patients are charged significant and inconsistent prices to receive copies of their own electronic medical records from providers.
- CareCloud announces $15 million in additional funding and a new CEO.
- Validic receives another $12.5 million in funding.
- Vanderbilt University Medical Center announces that it will replace McKesson Horizon, some of which was developed internally by Vanderbilt, with either Cerner or Epic.
Webinars
None scheduled soon. Contact Lorre for information about webinar services.
Acquisitions, Funding, Business, and Stock
Startup MORE Health receives $3 million in Series A funding for its multi-language EHR that connects doctors and patients in China with US specialists.

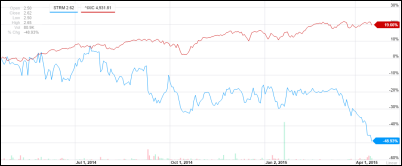
From the Athenahealth earnings call, which followed Friday’s expectations-beating earnings report that for some reason triggered a 7.4 percent share price drop:
- The company added 2,300 providers in the quarter, raising its total to 64,000.
- The RazorInsights team has been moved into the Atlanta office and the company has made RazorInsights sales, cross-sold AthenaOne to a RazorInsights client, and sold both products to a new client.
- Jonathan Bush says the urgent and convenient care market is the most important to him because it’s growing fast and is managing “worried well” lives.
- Bush says of big, non-academic health systems buying Athenahealth, “These guys have done their homework, gotten out their protractors and done the math on the arc of their flight, and they see it not clearing the tree tops. Not clearing the tree tops due to lack of profit is a great way to make you for-profit … They know that they can’t put the kind of obscene amounts of capital against or manage internal IT systems in the way that the fancy pants universities can afford to do and they’re slowly coming around to us and it’s exciting.”
- The company says it won’t talk about individual hospitals or sales of RazorInsights, but “When we look at our growth, first of all, we’re starting with a very new company with a small base, so it’s relatively easier to grow a lot on the small base. We don’t intend to talk specifically about the number of individual Razor deals or that sort of thing. We really bought RazorInsights as a strategic asset along with WebOMR to build out our full inpatient solution over time.” Bush added that RazorInsights got its clients to Meaningful Use but “the billing needs a lot of work, like a lot” and says by year-end Athenahealth will offer a full-service revenue cycle program to RazorInsights users.
- In justifying the $40 million paid for RazorInsights, Bush says Athenahealth got the best deal it could since the VCs who owned the company were either going to re-fund it or step out, so he sees it as an “acqui-hire” play in buying a product, a founding team, and brave early customers, adding that he’d like to do more of that.
- Bush responded to an analyst who asked how bookings revenue drove operating income improvement, “If you’ve been following us for a while, you’re following a caterpillar, right? There’s sometimes where the nose of the caterpillar doesn’t appear to be moving at all, but back in the ass, it’s building up potential energy which will turn into a great nose stretch. ”
- Bush said of ICD-10, “Never has a Bush felt so longing for more federal mandates as I have felt since the dying down of Meaningful Use and ICD-10 and PQR and ABC and do-re-mi. It is so easy when some fearful group of federal apparatchik are going to come for your prospect if they don’t buy. We are currently in a period where there are no apparatchiks coming … if ICD-10 tightens up and actually looks real later in the year it will help our close rate. I will feel sheepish about it because it seems a silly reason to make a free market move. But it’s true that right now our close rates are lower and that the specific reason we can attributed to it is no urgent federal mandate to buy.”
- Bush said that Athenahealth’s connection to CommonWell is in beta and that he’s OK with making EHRs interoperable via other methods because “otherwise we’re all going to be on some federally mandated ridiculous EHR.” He adds, “CommonWell could have been perceived as sort of a PR smite against Epic, which I assure you I would never want … I want to be anything that Epic’s in as well, even if we have to double pay. This is not the solution for interoperability by any stretch. This is just a service so that a patient can get their freaking chart and have the same patient match to all the different systems that their chart is in. So I don’t think you guys should think of CommonWell as some sort of silver bullet that fixes everything … I don’t think it’s a solution to the real challenge, which is the B2B interoperability … that’s kind of the new frontier that we’re doing most of our work on.”
Sales
Erlanger Health System (TN) chooses Epic in what the local paper says is a $100 million deal.
CoverMyMeds will use state-specific electronic prior authorization requirements information from Point-of-Care Partners.
People

Valence Health hires Michael McMillan (Cleveland Clinic) as SVP of strategic solutions.
Announcements and Implementations
CVS says in its earnings call that its Epic rollout is on schedule and will be completed by mid-year.
Government and Politics
A Washington Post review finds that nearly half of the 17 health insurance exchanges created as alternatives to Healthcare.gov are struggling with high technology and call center costs along with less-than-expected enrollment numbers. They’re considering raising fees charged to insurance companies, sharing costs with other states, asking for state money, or shutting down and using Healthcare.gov instead.
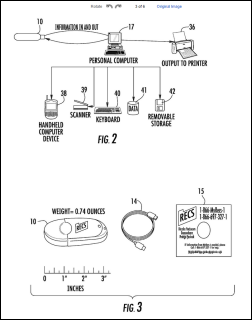
Consumer personal health record vendor LMG 3 Marketing and Development Corp. sues Apple, claiming that its Health and HealthKit apps violate its patents for technologies that it claims to have licensed to retailers such as Target. I found the original 2012 patent, which is a vague and seemingly unrelated description of a personal health record on a thumb drive. The primary inventor is Mike Lubell of Raleigh, NC, who developed MyPMR in 2000 while creating an EMR/PM business unit for Canon Business Solutions. LMG 3 apparently still offers MyPMR for $34.95.
Other
Former National Coordinator David Brailer, MD, PhD says in a Wall Street Journal opinion piece titled “They’re Your Vital Signs, Not Your Medical Records” that Congress should ensure that individuals have unqualified ownership of their health information and be given legal control over who sees it. He adds that patients should be allowed to designate an “infomediary” who can manage their information on their behalf. He warns that EHR vendors and providers block interoperability to gain a competitive edge and because “whoever controls health information will dominate the healthcare marketplace and its vast profit pool.”

Intermountain Healthcare CHIO Sameer Badlani, MD lists his favorite apps for reference guides (DynaMed, UpToDate, ACP Smart Medicine); drug reference (Epocrates, Lexicomp, and one listed as Medimex that I assume is supposed to be Micromedex); clinical calculators (MediMath, MDCalc, and one I haven’t heard of, OxCalc); and antibiotic guides (Johns Hopkins Antibiotics Guide, Sanford Guide).
UnitedHealthcare will offer 24×7 video-based virtual physician visits to members enrolled in self-funded employer health plans, expanding availability to employer-sponsored and individual plan participants in 2016. It’s working with Doctor On Demand, Optum’s NowClinic, and American Well, with access through its Health4Me app.
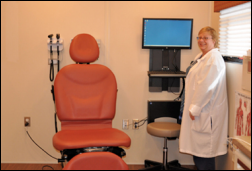
A Phoenix TV station profiles the local neurosurgeon who in 2008 developed The Medical Memory, which provides doctors with video recording equipment for recording patient encounters and posting them securely online for reference and sharing. I checked out the video link from the site showing his overview, but was kind of turned off that he got rather curt with whoever was running his slides (he’s a neurosurgeon, after all). It’s fascinating to me that on at least half a dozen occasions recently, I’ve had email or telephone conversations with healthcare IT people who came across as rude and clueless, leading me to question: could they possibly be that unlikeable in real life, or do they just come across poorly online without realizing it?
I’ll go out on a limb with this story: a Florida man sues a hospital for discarding his amputated leg in the trash, which he discovered when homicide detectives knocked on his door to inquire about what it was doing there.
Sponsor Updates
- The SSI Group will exhibit at the Louisiana HFMA meeting May 3-5 in Lafayette.
- Streamline Health will host the 2015 NEXT Summit Client Conference May 3-5 in Atlantic Beach, FL.
- VitalWare shares “Five More Facts about ICD-10.”
- Versus Technology recaps its HIMSS15 presentation on “Transforming Process Improvement through RTLS Data.”
- Huron Consulting Group will sponsor the 2015 Cristo Rey Viva Event on May 7 to support the students of Cristo Rey Jesuit High School in Chicago.
- Verisk Health offers“How Dollars Flow to Fight Medicaid Fraud.”
- Sunquest Information Systems will exhibit at the Pathology Informatics Summit May 5-8 in Pittsburgh.
- T-System President and CEO Roger Davis weighs in on EHR interoperability.
- Team Hackasaurus Rex wins TransUnion’s first Hackathon, held at California Polytechnic State University.
- Truven Health Analytics will host its Advantage Conference May 4-7 in Boca Raton, FL.
- Valence Health will exhibit at Becker’s Review and Annual Meeting May 7-9 in Chicago.
- ZirMed CEO Tom Butts shares his thoughts on IT trends and challenges, hospital CFOs on preventing claim denials before they happen, and ICD-10.
- MedData exhibits at the MGMA Anesthesia Administration Assembly through May 1 in Chicago.
- MediQuant President Tony Paparella is interviewed as part of the #TalkHITwithCTG podcast series.
- Navicure exhibits at Centricity Live through May 2 in Orlando.
- New York eHealth Collaborative will exhibit at the Crain’s Health Care Summit May 5 in New York City.
- Nordic Consulting releases the fifth episode of its “Making the Cut” video series on Epic conversion planning.
- NTT Data offers “It’s Beginning to Look a Lot Like Christmas … Thoughts on the Apple Watch.”
- Oneview Healthcare will exhibit at Digital Health Live 2015 May 5-7 in Dubai, UAE.
- Orion Health, Patientco, and PDS reflect on their HIMSS15 experiences.
- PMD offers “There’s More to Health Than Being Happy: What a Patient Satisfaction Score Really Means.”
- Qpid Health will exhibit at the Medical Informatics World Conference May 5 in Boston.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.













































































































































































Re: Deliberately Faked Academic Papers in Nature See, this doesn't surprise me at all. Of course AI quotes these bogus…