Top News
Struggling consumer genetic testing company 23andMe considers selling its Lemonaid telehealth business.
23andMe acquired the business in 2021 for $400 million.
23andMe’s entire board resigned last September over differences in the company’s direction. It announced a restructuring plan several months later that included laying off 40% of its staff and cutting several therapy programs.
Reader Comments
From ACIO: “Re: Children’s National. If I may, this isn’t a net-new deal against Epic. Children’s National (AKA The Bear Institute) was one of the first Cerner ITWorks clients, where Cerner basically took over all of IT (essentially full IT outsourcing). About the last ITWorks deal out there is University of Missouri (The Tiger Institute) as I believe at this point they pay almost nothing to Cerner and we all know that a university in today’s climate would really have a PR nightmare if they tried to replace an IT system to the tune of several 100s of millions of dollars.”
From What Happens In Vegas: “Re: Epic. It was recently reported that Carl Dvorak is no longer president of Epic. For as long as I can remember, the names ‘Carl and Judy’ were always mentioned together. Judy is getting older, so it seems like news that the person who was assumed to be taking over might not be poised to do so.” Carl recently said that he took a job in Epic’s international business sometime around May 2024. Sumit Rana’s LinkedIn says that he became president in August 2024. Sumit has been at Epic for 26 years and started as a developer, which I think I remember is a board requirement to run the company per Judy’s wishes. Carl has been with the company for 38 years, wrote a lot of Epic’s code at the beginning, and led the company’s architecture decisions. Google stalking suggests that Judy is 81, Carl is 59, and Sumit is 48.

From Matthew: “Re: Color Screens. Pretty sure Glen Tullman was an investor in the company that made the weird computer doors for Walgreens. EWTD (Everything Walgreens Touches Dies), including itself?” The company’s website had a now-archived web page that listed Glen Tullman as co-founder and vice chair. Co-founder and board chair of Chicago-based Cooler Screens (now CoolerX) is Greg Wasson, former president and CEO of Walgreens.
HIStalk Announcements and Requests

A reader’s donation funded the purchase of a document camera for Ms. H in Yonkers, NY, who provided the view above from her middle school classroom as she projects material onto the screen that all can now see. Students are also using it for collaboration projects. I will say, having directing other people’s money to hundreds of DonorsChoose projects, that the biggest bang for the buck comes from document cameras, headphones for students, Chromebooks, and small PA systems to allow the teacher to be heard without wrecking their voice. In fact, I see that Ms. H is asking for headsets to allow students to interact with AI-tailored reading lessons, the use of which is being piloted by her classroom (OK, I admit that I just fully funded that one since another teacher’s funded project was cancelled, which freed up some money).

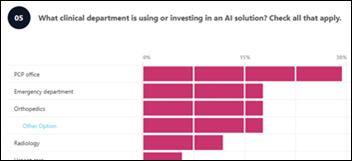
Here’s a fantastic opportunity to support frontline teachers through DonorsChoose, courtesy of Volpara Health, a wholly owned subsidiary of Lunit Inc. that provides clinically validated AI-powered software for personalized breast cancer screening and early detection. Teri Thomas, MSN, RN — Volpara’s CEO and an industry long-timer – will make a generous Donors Choose donation for each health system executive, technologist, or radiologist who completes a short, anonymous survey describing their organization’s AI purchasing plans. It’s like a slot machine where you pull the lever once, the money jingles into my teacher bucket, and I choose STEM projects to support. Not only will your participation fund classroom needs, Volpara’s donation will be doubled by matching money that is provided by my Anonymous Vendor Executive. If you work for a provider in administration, technology, or radiology, please answer 11 easy questions and Volpara and I will do the rest.
Webinars
January 23 (Thursday) 11 ET. “Maximizing Revenue With Minimal Resources: Work Smarter, Not Harder in Claims Management.” Sponsor: Inovalon. Presenter: Travis Fawver, senior sales engineer, Inovalon. Navigating the challenge of hitting revenue goals is daunting, but billing doesn’t have to be. The presenter will explore how strategic adoption of new technology can transform claims management processes from reactive to proactive. Learn how to reduce denials while empowering staff to focus on high-value activities, and gain proven strategies to simplify workflows, automate routine tasks, and build a more efficient RCM operation to maximize reimbursement.
Stream on demand. “Healthcare Data Security: Aligning Processes with Evolving Threats & Regulations.” Sponsor: Inovalon. Presenters: Anthony Houston, MBA, senior director of security, risk, and compliance, Inovalon; Paul Wilder, MBA, executive director, CommonWell Health Alliance; Luke McNamara, MPA, deputy chief analyst, Google Cloud; Michael Quinn, VP of strategic partner development, Inovalon. Hear leaders in healthcare data security discuss some of the top recent threat evolutions and how organizations can proactively respond by making ongoing improvements to security protocols.
Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
Acquisitions, Funding, Business, and Stock
Percipio Health officially launches with $20 million in Series A funding from investors that include UPMC Enterprises and Labcorp. The company offers app-based population health monitoring and management. Medhost founder and former CTO Eric Rock started the company with David Lucas, a former colleague at Medhost, Vivify Health, and Optum, in 2022.
Inovaccer acquires actuarial software vendor Humbi AI.
Behavioral telehealth vendor Iris Telehealth acquires InnovaTel, which offer telepsychiatry services.
Sales
- University of Kentucky HealthCare will implement Visage Imaging’s Visage 7 Enterprise Imaging Platform.
- University Hospitals Plymouth NHS Trust and Torbay and South Devon NHS Foundation Trust in England will go live on Epic in 2026.
People

CompuGroup Medical US promotes Benedikt Brueckle to CEO, a position he also held between 2017 and 2021.

Qure.ai names Jim Mercadante (RapidAI) chief commercial officer.

Rob Cornelssen (Huron) joins Health Systems Informatics as VP of business development.

Ken Kaufman (Mpaired) joins Sirona Medical as CEO.

Waystar promotes Todd Woods, MBA to chief growth officer, ambulatory.

RevSpring hires Nicole Rogas, MBA (Symplr) as president.
Announcements and Implementations

Arrive Health develops Arrive Accelerate to offer providers AI-generated guidance on medication coverage requirements for improved prior authorization workflows.
In New York, Somos Community Care, Forward Leading IPA, and Western New York Integrated Care Collaborative implement Findhelp’s social care referral software.

OCH Regional Medical Center (MS) will go live on Oracle Health on January 27.
Government and Politics

ASTP/ONC publishes newly updated SAFER guides, which address EHR safety.
Northeast Surgical Group (MI) will pay $10,000 to settle federal allegations that it violated the HIPAA Security Rule by failing to conduct risk analyses on its information system. A ransomware gang attacked the group in 2023, exposing the PHI of 15,300 patients.
Privacy and Security

Allegheny Health Network files a breach report indicating that the information of 294,000 of its home medical equipment and home infusion patients was compromised by a cyberattack on IntraSystems, which manages AHN’s servers.
Sponsor Updates
- Consensus Cloud Solutions offers a free plan of its flagship digital cloud fax solution, eFax, to aid in disaster response.
- Ascom names Tobias Stanelle (Philips Healthcare) managing director for the Ascom Americas region.
- Capital Rx adds more than 80 new partnerships in 2024 and prepares for another year of record growth.
- Gartner recognizes Dimensional Insight in its Peer Insights Voice of the Customer for Analytics and Business Intelligence Platforms report with an overall rating of 4.6 out of 5.
Blog Posts
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Follow on X, Bluesky, and LinkedIn.
Contact us.





















































RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…