ViVE and CHIME Wrap Up with Dr. Jayne 3/30/23
It was another busy couple of days at the conference. I had the opportunity to walk the show floor with a couple of friends yesterday and today as well as to hit a couple more sessions.
Overall, I liked the conference better than HLTH. It wasn’t as in your face trying to be cool as HLTH, but it was well organized. The exhibitor booths are all formatted the same way, depending on size and a couple of other factors, and I found it made for a less-distracting trip around the show floor. It’s less glitzy than you see at HIMSS, but it felt like it was easier to visually scan a booth. A vendor I spoke to said they like the setup because it helps level the playing field and also makes it easier to get the booth up and running compared to all the packing and unpacking at some other shows.
I’m still not a huge fan of having sessions on the show floor, but understand how it came to be. None of the panels I attended were jaw-dropping, but I had low expectations and wasn’t disappointed.
I thought the food service was better at HLTH, especially the grab and go options. At ViVE, the meal lines seemed long regardless of when I tried to eat during the scheduled blocks. On Monday, I ended up at the CHIME member luncheon that was held upstairs. It was a quieter venue to have a solid conversation with one of my colleagues about some healthcare IT problems I’m trying to solve.
CHIME provided several other networking opportunities, but my favorite was the CHIME League of Women luncheon on Tuesday. The program’s theme was “Mentorship in Action” and included a mentor-mentee pair among the speakers. The comments of panelist Kris Nessa from Innovative Insights really resonated with me. Kris was talking about the community of CIOs and other execs that has come together through CHIME and how the relationships and support have helped lift a lot of people up and encourage the development of the next generation of healthcare IT executives.
It made me think about the early days of my career, when our health system’s CIO was intent on crushing the IT project I was working on because it was being led by the operations group with IT support as opposed to being run by IT. He made it clear that he didn’t think clinical people should be working on IT projects and seemed particularly hostile to the women on the team, despite the fact that we were going live with some bleeding edge technology that ended up being the subject of numerous conference presentations. Thinking back, it’s likely he viewed innovation as a threat.
I’ve never had a non-clinical mentor. The conversation made me wonder what my career might have been like if someone from the technology side had taken me under their wing. I hope that in the current phase of my career I can be helpful to those working their way up the ladder or trying to break out of a mold that they might not have chosen.

Dr. Nick van Terheyden @drnic1 and I stopped by the Health 2047 booth to ask what it was all about, since “helping early-stage startups transform bold ideas into healthy returns” sounds interesting. It’s actually an initiative of the American Medical Association, and the year is tied to the anniversary of the founding of the AMA rather than the timing of any bold initiative.

Nomi Health’s booth reps were engaging. In addition to sharing the local favorite Goo Goo Cluster candies, we had a great conversation about the design of their booth and some of their ideas for enhancing it. I admire the knowledge or marketing folks. There’s so much more to color, graphics, and flow than most people appreciate.

CoverMyMeds was sponsoring haircuts, blowouts, and makeup applications. If you timed it right, you could get all fancied up then head over to the DrFirst booth for a complimentary headshot.
Speaking of DrFirst, their team did not disappoint, with matching shirts. Apparently they had matching shoes earlier in the week, but I missed those.

The Best Shirt award definitely goes to Perx Health’s VP of marketing. I think he said it was from Australia, and he was a great sport to pose.

The costumes at Teletalk reminded me of HIMSS of yore, when lots of exhibitors tried to be as catchy as possible. The boots were nice also.

The Best Shoe/Sock Combo was found at the Intelligent Medical Objects (IMO) booth. They’re always a strong contender in this category, and I can’t wait to see what they have in store for HIMSS. Since it’s local to their home base, folks might not even have to be choosy when they pack.

Hyro’s Whac-A-Task booth was a hit. I’ll have to use this pic to explain to some of my younger colleagues who never had the pleasure of playing the original Whac-A-Mole game.

Saving the best for last, Liberty Solutions hosted a bourbon tasting at their booth. They were giving solid advice on the characteristics of the different options, which makes sense given the fact that they’re a consulting firm.

The closing bash was a concert with the Black Crowes at the Wildhorse Saloon, although I preferred the opening group Chapel Hart. They were clearly having fun with their performance. The entire event was sponsored by Clearsense. From where I was standing on the second floor, I could see the decibel meter and it was interesting to see how it got louder as the night progressed.

I ducked out early but not before spotting the ultimate bedazzled ViVE jacket. Everyone seemed to have a good time, although threading my way through the crowds on Broadway as I headed back to the hotel seemed more like a contact sport than a walk.
On Wednesday, I had a little more downtime than planned at the Nashville airport and was glad to take advantage of some of the local food offerings that were better than the generic fare you find at most airports. Although the airport is undergoing construction, it didn’t feel chaotic. I decided to walk off some of the southern hospitality I’ve experienced this week with a lap through all the concourses. At the end of the A gates where some of the more commuter-type carriers arrive, I spotted some workers looking out the windows and acting generally giddy with excitement. It turns out that a Boeing 777 aircraft was diverted in from Atlanta last night and they were watching it being moved on the tarmac. Several of them couldn’t get over how large it was (towering over the other planes) or that a small tug was pulling it around the airport. Sometimes you just run across things that make you smile and I was glad to be part of that moment.
I wrangled the email beast and played catch up on the plane and was glad to see that the FDA has cleared the opioid overdose reversal drug Narcan for over-the-counter sales. Overdoses are a major problem across the US and we’re seeing lots of accidental ingestions by children as well. Hopefully removing the prescription hurdle will make a difference for people. I had to provide the date of my last COVID booster on a form I was completing, so I popped into my patient portal to confirm the dates. I was surprised to see a recommendation to schedule a flu shot. The flu season is long over in most of the US and I’m also current with a vaccine documented in the portal. It also recommended that I schedule my mammogram, and I’m current on that as well.
Alert fatigue is real and applies to patients as well as clinicians, and inappropriate reminders just encourage people to click through without reading. I’ll have to ask my IT friends at that institution what they’re trying to solve for with those reminders, which weren’t there a couple of weeks ago.
What aggravates you the most about your patient experience in patient portals? Leave a comment or email me.

Email Dr. Jayne.





![image[6] image[6]](https://histalk2.com/wp-content/uploads/2023/03/image6_thumb.png)




















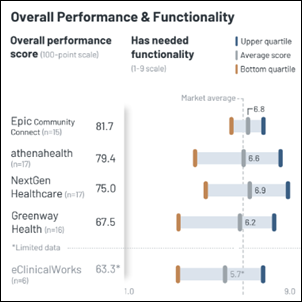


Yes, but why is Epic "the best in the industry for many healthcare systems"? And sure, it's a complex software…