News 5/30/25
Top News
Kaiser Permanente announces that all of its technology systems are back online after dealing with a network outage most of Wednesday. The outage, which Kaiser has attributed to an issue at one of its data centers, impacted facilities – and patients – across the country.
Reader Comments
From Mr. Friendly: “Re: Murray-Calloway County Hospital’s EHR implementation. Hospital officials shared the growing pains their staff are dealing with 45 days into their Oracle Health implementation, with new CEO Reba Celsor noting that “pleased” might be a bit of a stretch: “Because sometimes companies overpromise and underdeliver, and there’s a little feeling of that, so we’re working to make sure we’re holding them accountable to the agreement.” I’m not so sure this is an atypical experience for any hospital EHR implementation. Go-live teams are welcome to weigh in.
Sponsored Events and Resources
Live Webinar: June 18 (Wednesday) noon ET. “Fireside Chat: Closing the Gaps in Medication Adherence.” Sponsor: DrFirst. Presenters: Ben G. Long, MD, director of hospital medicine, Magnolia Regional Health Center; Wes Blakeslee, PhD, vice president of clinical data strategies, DrFirst; Colin Banas, MD, MHA, chief medical officer, DrFirst. Magnolia Regional Health Center will describe how its Nurse Navigator program used real-time prescription fill data from DrFirst to identify therapy gaps and engage patients through timely, personalized outreach. The effort led to a 19% increase in prescription fills and a 6% drop in 30-day readmissions among participating patients. Attendees will learn why prescribing price transparency is key to adherence, how real-time data helps care teams support patients between visits, and how Magnolia aligned its approach with value-based care and population health goals.
Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock

Amwell co-founder and former co-CEO Roy Schoenberg, MD, MPH launches Aileen, an AI companion for seniors that will also offer access to virtual care. He remains an executive director at Amwell.
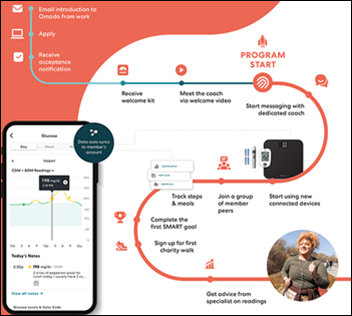
Virtual chronic care management company Omada Health expects to raise $158 million during its IPO next week, which would give it a valuation of $1.1 billion.
Sales
- Harbor Regional Health (WA) will transition to Meditech Expanse through the company’s MaaS subscription model.
People

Wolters Kluwer promotes Greg Samios to CEO of its Health division.

CVS Health names Ravi Patel, MD (Oak Street Health) VP and chief health informatics officer for healthcare delivery.

Jay Sultan (Tegria) joins Motive Medical Intelligence as EVP of product strategy and management.
Announcements and Implementations

Houston Healthcare (GA) will move from Meditech Magic to Epic as a part of its recently approved integration with Emory Healthcare (GA).

Boone County Hospital in Iowa goes live on Meditech Expanse.
Several providers and government agencies within Austin and Travis County in Texas connect to Watershed Health’s health information exchange and care coordination platform.

UF Health St. Johns (FL) implements Epic.
Government and Politics

DoD health officials share several IT updates at a recent State of the Federal EHR event, noting that virtual visit capabilities will soon be implemented across the department and US Coast Guard, and that it is working with the VA on a joint tele-critical care application. Plans to eventually add ambient dictation capabilities to MHS Genesis are also in the works.
Privacy and Security
BayCare Health System (FL) will pay $800,000 to settle potential HIPAA violations related to a 2018 data breach involving an unauthorized user who accessed a patient’s medical records, took photographs of them, and videoed themselves scrolling through the record on a computer screen. An unidentified individual then called the patient to let them know about the breach.
Sponsor Updates

- Cardamom Health staff work with the United Way of Dane County to assemble 500 snack packs benefiting Rise Wisconsin.
- Capital Rx will present at the AMCP Mid-Atlantic Day of Education May 30 in Falls Church, VA.
- The “MSSP 1337” podcast features Fortified Health Security CISO Russell Teague.
- Infinx releases a new episode of its “Revenue Cycle Optimized” podcast titled “From Paper to Patient-Ready – How Chesapeake Medical Imaging Cut Processing Time from Days to Hours.”
Blog Posts
- Top Physician Communication Frustrations (PerfectServe)
- How to Save Time and Increase Revenue: Automate ED Care Levels (CereCore)
- AI in the NHS: Hype, hope and how we make it work (Altera Digital Health)
- From First Call to Final Placement: What Candidates Can Expect Working with DRI (Direct Recruiters)
- The Unspoken Pillar: Why Social Care is Essential to CMS’s Evolving Health Strategy (Findhelp)
- 3 Ways Claim Denials Undermine Growth (and What to Do) (FinThrive)
- Thinking About Boomi for Healthcare? Here’s What You Should Know (Healthcare IT Leaders)
- How to Avoid the Latest Cyberthreat: MFA Notification Fatigue (Med Tech Solutions)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Follow on X, Bluesky, and LinkedIn.
Sponsorship information.
Contact us.
























































































The New Yorker cartoon of Readers Write articles.