News 1/12/24
Top News
Artisight, which offers a smart hospital platform, raises $42 million in a Series B funding round.
Co-founder and CEO Andrew Gostine, MD, MBA formed the company while working in his anesthesiology residency.
Reader Comments
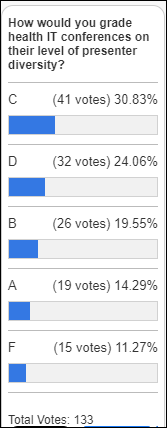
From Video Kills Brain Cells: “Re: vendor videos. I saw Dr. Jayne’s mention that she doesn’t watch them. You should conduct a poll.” I’m with Dr. Jayne in usually declining to spend time consuming vendor videos or podcasts. Skimming text visually is faster than watching even 3x speed video unless the graphics are uncharacteristically vital. My advice to those who create multimedia is to avoid making it an either-or situation – send your video or audio files to an AI-powered transcription service like I use, and for an incremental cost and time of just about zero, you can post the transcript along with the original and satisfy both audiences. Requiring people to sit through your precious AV meanderings is a vanity play that excludes some folks who might be interested. Perhaps my poll will ask whether respondents are decision-makers since I don’t picture many C-suite members using video as their preferred vehicle for gaining industry information.
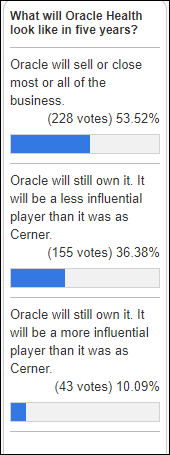
From Letme Throw: “Re: AI. I”m curious to hear your thoughts about the 2024 strategies that were announced by Oracle Health and Epic.” Oracle’s Larry Ellison talked up AI and voice-powered user interfaces in announcing the Cerner acquisition in December 2021, saying that Oracle would jump-start the business converting to a primarily voice-based UI for Millennium using Oracle’s Digital Assistant (along with creating a national EHR database, rewriting Millennium, getting the VA’s implementation done, etc.) I haven’t seen examples of Oracle Health’s real-life use of AI, not to mention that it won’t really matter if they keep losing customers to Epic. Epic seems to be way ahead, with some of its clients testing or using ambient listening documentation, inbox management, scheduling automation, AI-enhanced Cosmos research inquiries, and enhanced patient communications. Epic’s user base of huge academic health systems also gives it access to on-the-ground innovators who have the resources to design, use, and even develop AI-related tools that have an actual use case that is free of Oracle’s vested interest as a tech company in selling technical products to Cerner users. I would have low expectations of the provider impact of a quick bolt-on of Digital Assistant. I would enjoy hearing directly from Cerner and Epic customers about how they are using, or hoping to use, AI with their respective products. Also note that Meditech has arguably done a lot more with AI in Expanse than Oracle Health in Millennium, and at a friendlier price point.
HIStalk Announcements and Requests

Something reminded me of one-time high flyer Nant Health, which hit $21 per share on its first day of trading in mid-2016 drug billionaire Patrick Soon-Shiong, MD launched several Nant-named companies. Those shares are now at $0.06, valuing the company at $12 million. The company’s headquarters address is a UPS store in the tiny town of Winterville, NC, a few steps away from the notable Sam Jones BBQ.
Webinars
January 19 (Friday) 1 ET. “Unlocking Reliable Clinical Data: Real-World Success Stories.” Sponsor: DrFirst. Presenters: Alistair Erskine, MD, MBA, CIO/CDO, Emory Healthcare; Jason Hill, MD, MMM, associate CMIO, Ochsner Health; Colin Banas, MD, MHA, chief medical officer, DrFirst. Health system leaders will describe how they are empowering clinicians with reliable patient data while minimizing workflow friction within Epic. They will offer real-world experience and tips on how to deliver the best possible medication history data to clinicians at the point of care, use clinical-grade AI to infer and normalize prescription instructions in Epic, and encourage patient adherence to medication therapies for optimal outcomes.
January 24 (Wednesday) noon ET. “Medication Management Redefined.” Sponsor: DrFirst. Presenters: Nick Barger, PharmD, VP of product, DrFirst; Caleb Dunn, PharmD, MS, senior product manager, DrFirst. Clinical workflow experts will paint a reimagined vision for e-prescribing that offers enhanced patient adherence, customizable clinical support, intelligent pharmacy logic, and data integrity and safety. Join this first chapter of an ongoing conversation about what medication management should be, how to deliver greater benefits today, and how to prepare for the future. Elevating your solution and customer benefits isn’t as hard, scary, or economically challenging as you may think.
Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
Acquisitions, Funding, Business, and Stock
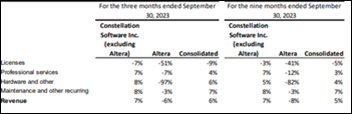
Veradigm lowers its FY2023 revenue and earnings guidance below consensus estimates. MDRX shares have lost 47% of their value in the past 12 months, much of that in a big price drop in early December. The company said in an SEC filing Wednesday that it doesn’t yet know when it will file overdue financial reports for the last three quarters and year-end of FY2023 or convene its annual meeting of shareholders.
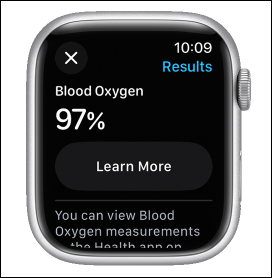
Rune Labs, whose FDA-cleared software tracks symptoms of Parkinson’s disease via the Apple Watch, raises a $12 million funding round. CEO Brian Pepin, MSEE founded the company after leaving his senior hardware engineer job at Verily Life Sciences in late 2018.

An Apple share price drop caused by demand doubts makes Microsoft the world’s most valuable company. Had you invested $10,000 in MSFT shares 10 years ago, you would have nearly $102,000 today, or if you are former CEO Steve Ballmer, you would be rolling in $128 billion worth of shares that throw off $1 billion per year in dividends.
Sales
- Spectrum Healthcare (AZ) chooses NextGen Healthcare for EHR/PM.
People

Industry long-timer Jeff Stern (Carium) joins Brado as VP of business development.
Announcements and Implementations
AI medical scribing technology vendor DeepScribe launches integration with Epic’s SmartData elements, allowing users to customize note preferences and standards that are mirrored in Epic.

Clearsense will present Billy Idol live in concert at ViVE 2024 in Los Angeles next month. I saw him a few years ago and he puts on a good show that goes beyond sneering through “Rebel Yell.” I’m predictably skeptical about the relevance of celebrity entertainment to healthcare, but if you are spending your employer’s money to attend ViVE, you might as well happily pump your fist overhead along with the punk rocker, who has been Medicare-aged for several years.

Amazon rolls out its Just Walk Out checkout-free technology to hospitals, allowing employees to pay for food by scanning their badges to create a payroll deduction.
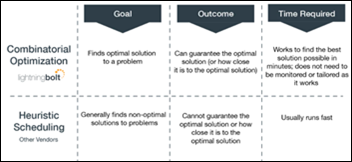
PerfectServe’s Lightning Bolt describes combinatorial optimization, a mathematical process that chooses the best possible solution given a finite set of possibilities. The interesting article describes, with some level of detail, how the company uses that process, rather than the more common heuristic method, to build the best physician schedules. The article wasn’t credited, but someone did a nice job of explaining a useful concept.
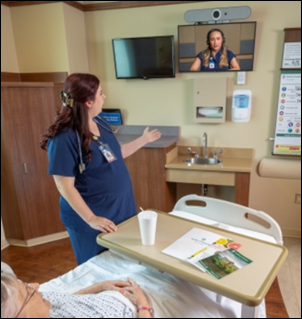
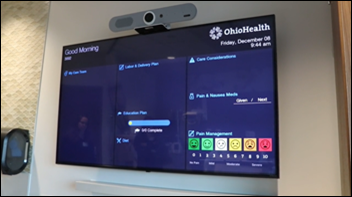
Caregility announces its new telehealth edge devices for hospital-based telehealth such as e-sitting, virtual rounding, patient-family communication, and tele-ICU, with OhioHealth and UMass Memorial Health being early adopters.
Palantir and University of Colorado Anschutz Medical Campus establish the Center for Linkage and Acquisition of Data as part of the NIH’s All of Us research program. The project will integrate claims and mortality data and address the challenges of linking EHR data from health information networks to improve data completeness. The principal investigator of the 18-month, renewable project – which is funded by a $30 million NIH grant — is Melissa Haendel, PhD, the chief research informatics officer of the medical campus.
Health insurer Elevance will offer people who are covered by its Medicaid health plans a free smartphone with unlimited data, talk, and texting to provide access to digital and virtual healthcare tools, supported by funding through the FCC’s Affordable Connectivity Program.
Privacy and Security
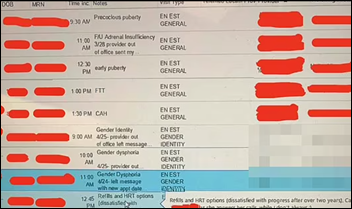
HHS investigates a 33-year-old Texas surgeon for providing case lists of minors who were undergoing gender-affirming care at Texas Children’s Hospital to a conservative activist, which HHS deems to be a HIPAA violation. Eithan Haim, MD, who completed his residency in 2023, says that he is innocent because he redacted specific information from his Epic screen shots. The hospital said in March 2022 that it was halting provision of the services in response to the state’s interpretation that they constitute child abuse, but his records indicate that treatments continued. I’m thinking that at least from the redacted screenshot provided, he’s correct in that while he disclosed some of the 18 HIPAA identifiers (such as age and diagnosis), redacting patient-identifiable fields such as name or medical record number makes it de-identified PHI, which isn’t protected by HIPAA, although the question remains about whether he accessed and disclosed the data inappropriately if not illegally. I suppose HHS knows best.
Novant Health will pay $6.6 million to settle a lawsuit that was brought by 10 of its patients for the health system’s use of the Meta Pixel website user tracking tool.
Other
Two hospital EDs in Australia will revert to their previous IT system for six months after implementation of InterSystems TrakCare in mid-November caused long patient wait times and user frustration.

Noetik co-founder and CEO Ron Alfa, MD, PhD shares his tab for a single bottle of water at the J.P. Morgan Health Care Conference in San Francisco, where the moneylenders fly private to sit at $100 per hour lobby tables while pondering the mystery of why US healthcare is so expensive.
Sponsor Updates
- EClinicalWorks announces that McKenzie Health System (MI) is improving operations using its EHR, clinical rules engine, and robotic process automation.
- Net Health launches the next phase of its digital musculoskeletal thought leadership program in partnership with the American Physical Therapy Association.
- First Databank names Kara Zebrowski (Glytec) product manager, Hamman Eltareb (Hearst Health) health data analyst, and Christian Wong software engineer.
- Findhelp launches season two of its American Compassion Podcast about the history of the social safety net in America.
- Meditech recognizes international customers of its Expanse EHR, which include providers in East Africa, Ireland, Australia, UK, and Singapore.
- FinThrive releases a new episode of its Healthy Rethink Podcast, “He’s Here, He’s There … Virtual Care Everywhere.”
- Medicomp Systems releases a new episode of the Tell Me Where It Hurts Podcast featuring Juan Carlos Gallegos, RN senior director of product, Homecare Homebase.
Blog Posts
- A Look Back at 2023: Critical Cyber Threats in Healthcare (Fortified Health Security)
- Keys to Releasing “Hidden Clinical Capacity” (Impact Advisors)
- How Can You Use ChatGPT for Software Testing? (Keysight Technologies)
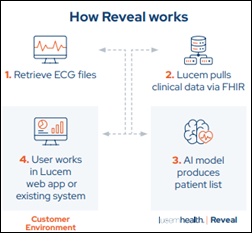
- Treatable Stage I and Stage II Colon Cancer: Importance of AI-enabled Early Detection (Lucem Health)
- 5 steps to take before embarking on your AI journey (Meditech)
- The Future of Wound Care: 5 Trends for 2024 (Net Health)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.
















































































































Hard agree, and not just because I'm a spreadsheet nerd. Why are we all here? Isn't it in the service…