Monday Morning Update 2/3/25
Top News

Veradigm’s strategic review fails to attract acquisition bids from the five organizations that had expressed interest, reportedly among them McKesson and Oracle. The company says it will refocus on making operational improvements and working to get its shares re-listed.
The company says it will provide an updated FY2023 and preliminary 2024 report in March. Tom Langan remains interim CEO after eight months.
Veradigm also announced that board member Beth Altman, who served as chair of its audit committee, has resigned due to health reasons.
MDRX shares dropped 32% on the news, valuing the company at $588 million. They are down 54% from their 52-week high.
Reader Comments
From Color Me Skeptical: “Re: Oracle Health. I’m skeptical of its claims about its next-generation EHR, since Cerner under Oracle has over-promised and under-delivered. I’m also befuddled by the promotion by company spokespeople about the EHR being voice driven. Is anyone really asking for that?” David Feinberg says that Oracle will rebuild the EHR with clinicians and patients in mind, integrating it with the company’s other systems, such as ERP and human capital management. Oracle emphasizes voice navigation, which might draw interest if it doesn’t slow clinicians down. He claims that the new EHR is now generally available, which I hadn’t heard before (anybody know the live sites?) He agrees that Cerner had a reputation for slow-motion fumbling but insists that Oracle ownership has fixed everything.
We have a customer base that has been patient with us as we haven’t really executed. In saying “we,” I’m really talking about Cerner, which did not execute fast enough. We became Oracle. I think we have literally leapfrogged the competition. We have executed and hit on every timeline. Now it’s 2025, it is time for us to deliver and delight our customer base.
From Aye I: “Re: AI training. As an AI dabbler, what training or certification do you recommend?” None. The technology and approach changes every five minutes, so whatever you learn today will be worthless tomorrow. Just get your hands dirty. The value of most certifications and online courses accrues to the seller, not the buyer.
HIStalk Announcements and Requests
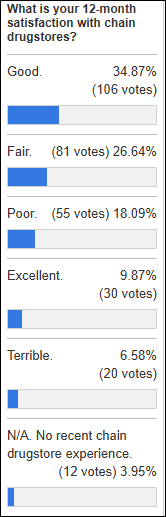
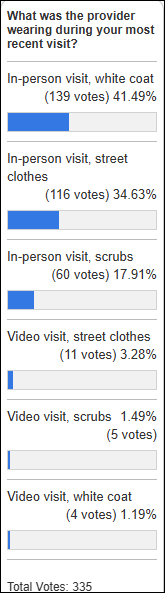
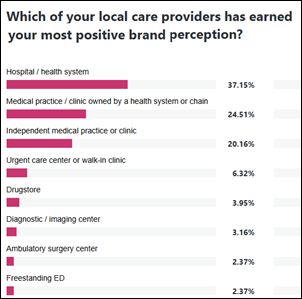
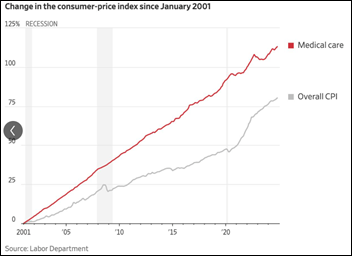
Nearly all respondents from last week’s poll have had recent experience with a chain drugstore, of whom two-thirds report an OK or better experience.
New poll to your right or here: What type of visit would you choose for a sore throat? Bonus points for adding a post-vote comment that explains your choice. I’m probably an outlier since I’ve never had a virtual visit, a trip to urgent care, or an ED visit except a long time ago when I had an out-of-the-blue episode of laryngospasm, a terrifying but harmless choking-like moment when your throat decides to rage quit breathing (pro tip: relax, breathe slowly, make a sound such as humming, and don’t bother going to the ED because they can’t do anything).
DeepSeek can generate fun trivia quizzes, so I gave it the link to Vince Ciotti’s HIS-tory series.
Health system executives, technologists, and radiologists — Volpara Health will make a significant donation to Donors Choose for your response to this quick survey.
Sponsored Events and Resources
Instant Access Webinar: “Successfully Navigating Post-Acute Rev Cycle Challenges.” Sponsors: Inovalon and KanTime. Presenters: David Swenson, senior manager of sales engineering, Inovalon; Lucy Lopez, VP of product management, KanTime. Learn how to speed up your revenue cycle processes and avoid the common RCM and eligibility errors that cause delays and denials. Discover strategies to boost your bottom line: streamline eligibility verification, simplify complex processes, and optimize denial management for improved cash flow.
Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock
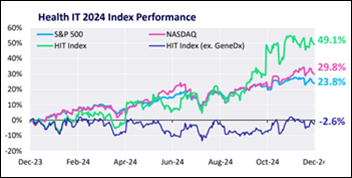
The latest Health IT Market Review from Healthcare Growth Partners reports a narrowing bid-ask spread in company acquisitions as buyers show greater risk tolerance. Investors are seeking portfolio liquidity, while sellers are offering higher-quality opportunities. Key takeaways:
- M&A valuations rebounded to pre-pandemic levels in 2024, with private equity buyouts hitting a record high.
- Distressed asset sales may not yield the apparent proceeds. Truepill, once valued at $1.6 billion with $250 million in annual revenue, sold for $525 million, but just $25 million was paid in cash. Upfront Healthcare’s $86 million acquisition by Health Catalyst fell short of its total raised funding.
- Take-private deals saw steep discounts from pandemic highs: R1 (-54%), CompuGroup (-74%), and Accolade (-89%).
- Early-stage fundraising is picking up, reflecting broader market confidence.
- AI investment accounted for 25% of total funding, with investor interest shifting almost entirely from clinical AI tools to workflow automation.
- Investors view AI as an operational enhancer for a company’s existing business rather than a primary investment focus.
People

Keith Dowling, MBA (Cleveland Clinic) joins Catholic Health as VP/CISO.

RxLogic hires Paige Zimmer, MHSA (First Databank) as EVP of business development.

Andrea Kowalski, MBA (1upHealth) joins Datavant as SVP of product, provider solutions.
Announcements and Implementations
HIMSS conference owner Informa launches WHX Tech, a healthcare events brand that will hold its first conference later this year in Dubai with the involvement of HIMSS.
Government and Politics
The White House fires VA Inspector General Mike Missal, whose VA OIG report that highlighted patient harm that was linked to its Oracle Health rollout led to the project being temporarily halted.
FDA Digital Health Center of Excellence Director Troy Tazbaz, who guided the agency’s policy related to AI and software as a medical device, resigns.
Sponsor Updates

- SmarterDx staff assemble 250 patient comfort kits for UC Irvine.
- Wolters Kluwer Health announces that six of its book publications have won Book of the Year awards from the American Journal of Nursing.
- Vyne Medical releases a new case study, “How a Tennessee Health System Leveraged Automation for Success.”
- CereCore releases a new podcast, “CIO Insights: How to Pursue Big Technology Opportunities and Satisfaction.”
- Black Book Research publishes a new digital book, “The 2025 Black Book of Global Healthcare IT.”
- Tegria will sponsor and exhibit at the AHA Rural Health Care Leadership Conference February 23-26 in San Antonio.
Blog Posts
- 5 Reasons Why AI is a Platform, Not Just a Solution (Netsmart)
- The case for bundled de-implementation: Could doing less deliver better patient care? (Nordic)
- 8 questions product leaders should ask when evaluating EMPI solutions (Rhapsody)
- The Role of Per Diem Nurses in Addressing Seasonal Patient Surges (SnapCare)
- Large Academic Medical Center Expands Adoption of Vyne Medical Solutions, Adding Cloud Fax Services (Vyne Medical)
- Unlocking Hidden Gems: Leveraging RCMTAM for Revenue Cycle Excellence (CereCore)
- Revolutionize Healthcare Payments with TrustCommerce: Meet Us at ViVE, HIMSS, and CORE 2025 (TrustCommerce)
- The cost-benefit of data quality and strategy in healthcare (Wolters Kluwer Health)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Follow on X, Bluesky, and LinkedIn.
Contact us.

















































































































































Thank you for the mention, Dr. Jayne — we appreciate the callout, the kind words and learning more about the…