Monday Morning Update 12/15/25
Top News

A GAO report says that the VA must address several previously raised issues to support its accelerated Oracle Health rollout. Among them:
- Produce an updated cost estimate and schedule.
- Implement change management activities and conduct an independent assessment of the EHR’s user suitability and effectiveness.
- Document a change management strategy to drive user adoption.
- Develop change readiness scores before future deployments.
- Assess whether enhanced VA and Oracle Health training has been effective.
- Establish user satisfaction goals.
- Monitor trouble ticket resolution within established goals.
- Postpone deployment in new locations if critical test issues have not been resolved.
Reader Comments
From Jacinto: “Re: Dr. Craig Joseph’s comments about packaging AI as cuddly robots to improve behavior change. This is blazingly insightful. I can think of quite a few examples where words on a screen or delivered by a faceless voice would be more effective.” His company blog post made me think about the patient care value of anthropomorphized AI speech that is delivered by a comforting, universally understood form factor (which also happens to be inexpensive). As he says, “People don’t struggle with anxiety or diabetes or rehab exercises because they are missing the right paragraph of text.” Potential uses that I can see:
- Deploy virtual avatar-powered staff extenders that engage with patients instead of being used in the factory robot model of making deliveries and lifting. This would be especially powerful if connected to humans who could seamlessly take over the conversation or look at real-time video as needed. Such use would be beneficial in any care setting, but especially in staff-stretched skilled nursing facilities.
- Use a human-like robot to coach exercise or rehabilitation routines, with real-time personality tuning to adapt to whatever style works best for each patient (drill sergeant versus cheerleader).
- Monitor and coach hospital-at-home patients, providing nudges and a sense that caregivers remain involved and invested in their outcomes.
- Reassure children during pre-op coaching, MRI prep, and medication / injection administration and teaching.
- Support patients who are experiencing agitation, dementia, or withdrawal symptoms and provide ongoing reorientation about place and situation.
- Perform real-time language translation for informed consent, discharge instructions, and staff communications.
- Conduct pre-rounding conversations that AI then turns into a clinician-ready daily narrative.
- Allow distant family members to deliver verbal patient support via the comforting form factor.
- This is way out there, but empathetic, carefully guardrailed robots could be used to reduce clinician burnout by debriefing them about the emotional weight of caring for distressed or critically ill patients or delivering bad news to families. Clinicians may lack social support or may avoid sharing concerns with peers. Studies show that people are often more candid with technology.
HIStalk Announcements and Requests
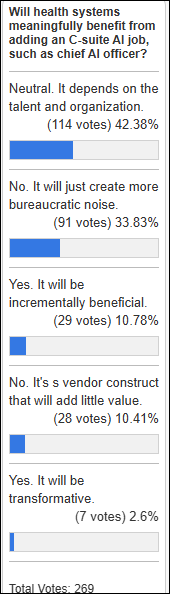
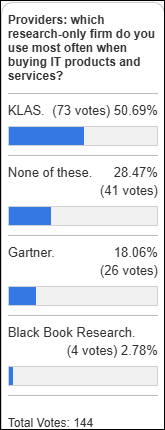
Poll respondents are still trying to figure out if having a C-level AI advocate provides clear benefit.
New poll to your right or here, from the discussion above: Will socially assistive AI robots outperform chatbots when the goal is patient behavior change? I expect a lot of respondents to punt with the “need more evidence” option, but let’s see votes and comments from those who have firmer opinions.

A generation donation from Bill, amplified by matching funds from outside sources and my Anonymous Vendor Executive, fully funded these Donors Choose teacher grant requests:
- Cricut tools for STEM projects for Ms. N’s middle school class in Paterson, NJ.
- Compassion corner furnishings for Ms. H’s elementary school science academy class in Youngstown, OH.
- Science supply cabinets for Mr. T’s middle school class in Paterson, NJ.
- STEM design supplies for Ms. P’s elementary school class in North Miami Beach, FL.
- A microscope and STEM activities kits for Ms. Y’s elementary school class in Van Nuys, CA.
- A document camera for Ms. R’s elementary school science academy class in Austintown, OH.
- Headphones for Ms. S’s middle school class in High Point, NC.
- Magnetic stick building blocks for Ms. O’s elementary school class in Hayward, CA.
- Flexible seating and STEM kits for Dr. H’s elementary school class in Forest Park, GA.
- Science club supplies for Ms. S’s middle school in Utica, NY.
- Science and engineering expo supplies for Ms. S’s elementary school class in Lorton, VA.
Sponsored Events and Resources
None scheduled soon. Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock

A report by The Information says that new fundraising by OpenEvidence values the company at $12 billion.
Mass General Brigham spins out AIwithCare, an AI-powered tool that matches patients to clinical trials.

A new reach for private equity tentacles shows up in software for volunteer fire departments. PE-backed ESO Solutions bought the $795-per-year system that is used by Norfolk VFD, shut it down, and offered a $5,000 replacement. Norfolk found a cheaper option, but ESO then acquired that vendor, too. ESO now serves 20,000 of the nation’s 30,000 fire departments, and its two largest rivals are also PE-backed. ESO’s majority owner is Vista Equity Partners, which also holds positions in Greenway Health, SimplePractice, and TigerConnect. Its president and CEO is Erick Beck, DO, MPH, who left his president / COO role at University Hospitals to join ESO in June 2022.
Announcements and Implementations
Investment banker and former FDA Commissioner Scott Gottlieb, MD says in a JAMA Health Forum article that AI has not boosted healthcare productivity because the industry depends on labor-intensive work that is better measured by outcomes than output. He predicts that AI will raise productivity by taking over some cognitive and physical tasks, which will free physicians to focus on work that requires human judgment. He argues that FDA should replace its static device framework with one that permits safe, iterative AI updates without full reapproval unless performance standards are violated. He adds that adoption lags because Medicare does not pay for technology directly and must remain budget-neutral, which forces any new payments to be offset by cuts to physician reimbursement.
Private equity firm Geneva PE launches the development and funding of NXXIM, an AI-powered enterprise medical imaging platform. The announcement provides few details, such as naming the “world-class leadership team of industry veterans” who are involved.
Other
A San Francisco woman gives birth in the back seat of a Waymo driverless car that she had hailed for a ride to the hospital. The car noticed “unusual activity” and called emergency services en route.
Interesting: HIMSS members who participate in any of its volunteer committees, task forces, and workgroups are prohibited from recording the content (that’s reserved for HIMSS to package as its own content) and can’t use any AI devices or software to record or transcribe the meeting.
Not health tech related (yet), but fascinating. Google upgrades Translate so that users can hear real-time translations in their earbuds. It also translates the user’s speech into the other person’s language. The Gemini AI enhancement auto-detects the languages being spoken, filters ambient noise, and preserves the original speaker’s intonation and pacing. I can’t imagine traveling internationally without Translate and Maps on my IPhone’s homepage.
Sponsor Updates
- Nordic releases a new “Designing for Health” podcast episode featuring Matthew Trowbridge, MD.
- Optimum Healthcare IT publishes a new white paper titled “Strategic Transformation in the AI Era: Turning Innovation into Impact.”
- The “Lead the Team” podcast features RLDatix North America CEO Dan Michelson in an episode titled “The CEO Who Saw What Success Hid.”
- Switchboard Health offers a new case study titled “Large Health System Cuts Provider Message Touches by 42% with Switchboard, MD.”
Blog Posts
- Redefining pharmacy: As the role of hospital pharmacists evolves, drug decision-making requires a new approach (Wolters Kluwer Health)
- Empowering Pharmacists to Prevent Opioid-Related Harm: A Patient-First Prescription (First Databank)
- The Reality of Incident Response Readiness in Healthcare (Fortified Health Security)
- Build or Buy? Choosing the Right Path for Effective Member Outreach (ReferWell)
- How Riverside County is Driving Connected Care (Netsmart)
- Cutting Through AI Hype: The 3 Tiers of Medical Coding Automation (Nym)
- 5 Trends Shaping Healthcare in 2026 (and 3 to Leave Behind) (PerfectServe)
- A Rural Hospital’s Guide to Revenue Recovery (Sliced Health)
- Tegria’s Biggest Event Takeaways From 2025 (Tegria)
- Harnessing AI for post-acute RCM: How leaders can build a smarter revenue cycle (Waystar)
- The Biggest Shift in Health Tech Regulation Since HITECH (And What It Means for Your Organization in 2026) (Zen Healthcare IT)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Follow on X, Bluesky, and LinkedIn.
Sponsorship information.
Contact us.



























 e
e



![image[10] image[10]](https://histalk2.com/wp-content/uploads/2025/11/image10.png)
![image[6] image[6]](https://histalk2.com/wp-content/uploads/2025/11/image6.png)














































![image[8][3] image[8][3]](https://histalk2.com/wp-content/uploads/2025/11/image83.png)

![image[5][3] image[5][3]](https://histalk2.com/wp-content/uploads/2025/11/image53.png)












Today's post contains the phoenixes rising from the ashes of the post COVID telehealth era. There's two things that destroy…