News 7/2/14
Top News

Bloomberg profiles InterSystems founder and owner Terry Ragon, net worth $3.1 billion, and the connections he has with other early healthcare IT companies such as eScription and IDX.
Reader Comments

From Illinois Blago: “Re: Riverside in IL. Moving from McKesson to Epic.” Unverified.
From GhostofEclipsys: “Re: Allscripts. In an effort to reduce costs as sales continue to wane, the company is considering outsourcing its client education and training group this fall. This has not worked well for other HIT companies and is an often quoted reason for not selecting a vendor during RFP. Clients want training by experts from inside the four walls who have critical relationships with engineering, not the B-team outsourcer. The Allscripts education team has won several awards for client education nationally.” Unverified.

From Block and Tackle: “Re: Self Regional Healthcare. Has had three days of Allscripts Enterprise downtime due to a known issue involving a patch. I’m curious if readers have had similar experiences with Allscripts Enterprise.” Unverified.
From Nasty Parts: “Phytel laid off a large number of people today. Rumor has it that the primary VC wants their $40M investment back and that Premier backed out of a deal to buy Phytel. I hear Phytel wants $225M and Premier wants to only pay $165M. So, today’s layoffs are to help the company get to a more profitable number that can justify the larger purchase price.” Unverified.
From Furydelabongo: “Re: athenahealth. The Belfast, ME office is bringing in a local primary care practice, Searsport Family Medicine, to serve as the clinic practice for their employees as well as be a test site for new functionality.” Unverified.
DoD EHR Update from Dim-Sum

DHMSM status and latest rumors in the halls of bedlam, located “just to the right” of K Street. Sorry about he delay, I have been rather busy.
- June marked the date where the DHMSM vendors will finally peruse a more comprehensive assessment of what each and every vendor will have to endeavor.
- Great job Captain W and your respective team – The REAL RFP will be dropped September 2014.
- One can only hope that your DHMSM team’s work will allay the fears and will fuel the excitement of those that are crazy brave and yet confident to move forward with this unique EHR experience
- Rumors are ringing about the Womack ousting. In all sincerity, I believe that all three impact solution teams could improve safety across the DoD HIT environment, be it Cerner, Siemens/athena, or Epic (have yet to decide if Allscripts can compete with their sub-mundane acute solution). Good news, DoD, all of these solutions will improve workflows, enable true integration and interoperability, and will be focused on clinician adoption. In the immortal words of the DoD, “There is no such thing as too much training?” COTS love to train the trainer (for a nominal fee) and perhaps that mentality will be a bright spot in a bleak environment.
- Six site visits by DoD to Epic sites, one gratis for McKesson, Meditech, and Cerner. I guess Siemens/athena and Allscripts missed the boat?
- Can anyone explain how with two media submissions (one article, one announcement) the DHMSM solution price went from $5.5B to $11B? Perhaps it is the Watson effect?
- In that same way of thinking, I believe that the first decade in a half of amateur DoD HIT design cost tax payers a trillion dollars give or take a half a billion!
- Claims rumors abound. Wondering how much of the claims processing debacle including collections will be handled by one of the big three. This is an essential component, and since ABACUS is having FISMA issues, I figured that maybe Mr. Miller will see value in pushing claims in the DHMSM deal – more than revenue cycle, so sorry, Epic, you will have to actually find a third-party system (feel the fear!)
- Industry Day – interesting, not as interesting as the RFP team read. Telehealth, asset tracking, real enterprise scheduling, military styled healthcare logistics (COTS, this is more of a challenge than most realize – hope there are some real discussions to understand what it means to be a functional ERP+ system).
- Cerner, you are not ranked in the top five to install your own system. Good thing you have Accenture to pick up the slack – Leidos “as is” is your key to victory – Theme “transition, transition, transition”
- Siemens, be happy athena is a very competitive ambulatory care solution. Teamed with your SOA your co-hosting maturity in acute and ambulatory settings make a lot of sense. I believe it might be appropriate for Tibco to lend a hand in the technology story that is truly a differentiation for the Lockheed team.
- BTW, Lockheed, I could have sworn you had more than a part-time employee working your public relations program – is it difficult to state your intentions? CSC passed you as though you were riding a moped on the autobahn.
- Allscripts, CSC, and HP — what a combination. You only need a population health solution and have to press the fact that Eclipsys is not archaic – good luck with that. Great announcement, short, succinct, and made people scratch their head.
- McKesson is rumored to be in deep negotiations with themselves – so far no progress.
- Cerner is the closest COTS to try to emulate what Epic has done, stating proudly that they are a monolithic solution, built on a myriad of frameworks they are competitive and can hold their own (however, I do not like the ambulatory solution, but the RFP will not have a weighted value assessment on features and functions, merely a check box that allows a team to state “YES we CAN"). Cerner should also utilize the Oracle story as they did in Utah for a win.
- Accenture “good on you” for the Henry Schein relationship. If my teeth were falling out of my mouth, the first and most exciting dental EHR solution I would want managing my episode of care would be Dentrix!
- GE Healthcare is missing in action. Perhaps an upcoming announcement will be made about their acquisition by SAIC? OK, maybe that is pure rumor 🙂
- VistA – we all know your solution is awesome, everyone loves it, adoption in a monopoly environment is 110 percent. However, do you really think after the debacle that is VA, informatics should try to be proliferated across the DoD? Methinks NO.
- NOTE: After several “as is” and “to be” meetings, the EHR vendors real fears have more to do with two things: (a) Legacy solutions that were so poorly designed and the manner in which they were integrated requires duct tape and glue – can any vendor that programmed the old solutions actually stand behind their solution? Did anyone within 50 miles of the beltway ever read anything about HIT standards? (b)How does a real EHR maintain parallel operations with a variety of poorly designed systems? These two thoughts are constantly on the minds of the EHR vendors – it haunts their dreams!
- There is a sobering thought I had with a colleague over a cigar — that Leidos (SAIC in general) and Grumman should not be allowed to bid as a member of any team, but instead be enlisted as enablers to access the “stuff” they created. Perhaps they should be relegated to provide 100 percent support for all transitions, migrations, parallel synchronization, and conversions for the new EHR solution team. This time using real standards, ones that people can understand, would be refreshing. In essence they should act as Switzerland so they can actually do something that emits value over the next 5-7 years associated with rollout. Think of it as penance.
Webinars
July 2 (Wednesday) noon ET. The CIO’s Role in Consumer Health. Sponsored by HIStalk. Presenter: David Chou, CIO, University Of Mississippi Medical Center. We are moving towards an era where the consumer is searching for value. Healthcare is finally catching up with other industries and this is forcing health care providers and health plans to rethink their "business model" as consumers test new decision-making skills and demand higher quality and better value. Technology can provide value in this space as we move towards a digital healthcare.
Sales
Arkansas Methodist Medical Center (AR) chooses T-System’s ED documentation and coding solutions.

Children’s of Alabama extends its contract for Allscripts Sunrise and adds dbMotion, Sunrise Ambulatory Care, and Sunrise Emergency Care.
People

Voalte promotes Trey Lauderdale to CEO and appoints a new board of directors: Tom Johnson (Global Imaging Systems), Nico Arcino (Kaiser Permanente), William Gish (Cerner Corporation), Isobel Harris (PeopleFluent), Jeffrey Lozon (Revera), Michael Marvin (MapInfo).

SRS names Scott Ciccarelli (GE Healthcare) as CEO. He replaces Evan Steele, who will become senior advisor.


AirStrip promotes Matt Patterson, MD to president and hires Nancy Pratt, RN, MSN (St. Joseph Health) as COO.

Robin Raiford, RN-BC (The Advisory Board Company) died on June 26 at 62. The visitation and service will be held Wednesday, July 2 in Springfield, VA. Details and guest book are here.
Announcements and Implementations
PatientKeeper adds a rules engine to its charge capture solution that allows billers and coders to manage code edits.
QSI subsidiaries NextGen and Mirth announce NextGen Share, a Health Information Service Provider (HISP) that will connect NextGen and non-NextGen EHR users via Direct.
Albany Area Primary Health Care (GA) goes live on Forward Health Group’s PopulationManager and The Guideline Advantage.
Innovation and Research
Researchers develop the capability to create blood vessels using a 3D printer and then growing cells around them, leading to the possibility of “printing” a full organ.
Other
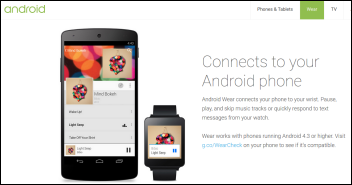
An Ars Technica article written by an early Google Glass Explorer says Android Wear smart watches make Google Glass obsolete. Reasons: (a) Google is developing more technology for Android Wear than for Glass; (b) Glass will always look weird and raise suspicions that the wearer is secretly recording them; (c) Google disabled live video streaming on Glass because it didn’t work well; (d) Glass doesn’t fold, so it takes up a lot of room wherever you place it other than on your face; (e) it’s easier to look at a watch than upward to Glass; (f) Android Wear watches cost $200 vs. Glass at $1,500 and do more; (g) Android Wear is being run by Google’s powerful Android team while Glass is a skunkworks project that hasn’t even exited beta; (h) Android Wear is faster and less buggy; and (i) Google has no plans to add augmented reality or facial recognition to Glass to make it something more than just a computer built into a pair of glasses.
Weird News Andy wonders “retail or wholesale” when an ED patient is charged with walking out with $300 worth of medical supplies that included bed sheets, 47 latex gloves, a bloody syringe, oxygen tubing, washcloths, alcohol wipes, lubricant, and pulse oximeters. WNA concludes, “The list price on a pulse oximeter on Amazon is $199. A single aspirin might be a hospital charge of $25. Seems like the perp might have gotten off cheap.”
Sponsor Updates
- Aventura releases the latest in its “This is Aventura” video series, seasonally appropriate in being set to the “1812 Overture.”
- EDCO Health Information Solutions publishes an article, “Solve Patient Indexing Errors Once and for All.”
- Liaison Healthcare will offer its EMR-Link laboratory and radiology integration solution to members of GNYHA Services.
- Beacon Partners offers an article, “Four Key Components for Building a Sustainable mHealth Strategy” and publishes a blog post “Are You Ready for Change? Four Questions to Ask Before Launching a Healthcare IT Project.”
- Truven Health Analytics reports that 300 hospitals have integrated Micromedex patient education and clinical decision support with their EMRs so far in 2014.
- QPID CEO Mike Doyle will participate in the “Big Data and Decision Making” panel at the Connected Health Symposium 2014 October 23-24 in Boston.
- ADP AdvancedMD introduces integrated fax with a short video clip.
- ICSA Labs certified products from First Databank, Iatric Systems, Juniper Networks, Orion Health, Quest Diagnostics and The Advisory Board Company in June.
- Health Catalyst explains the anatomy of healthcare delivery model in a recently published white paper.
- Maury Regional Medical Center (TN) selects Nuance services for its medical transcription needs.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.

















































































Re: Deliberately Faked Academic Papers in Nature See, this doesn't surprise me at all. Of course AI quotes these bogus…