Top News

Hackers breach the systems of NextGen Healthcare and access the information of one million patients, according to a filed breach report.
The company says that its cloud-based NextGen Office EHR/PM was accessed using stolen credentials between March 29 and April 14, 2023.
NextGen was also breached in a ransomware attack in January 2023.
Reader Comments
From Sundowner: “Re: Oracle Cerner’s Helix molecular diagnostics platform. I hear that they are sunsetting it. Can you confirm?” I’ve heard this from multiple readers. I’ve asked an Oracle media contact to clarify, but haven’t heard back.

From Tootie: “Re: Sentara. Another $1M down the drain. They must have used the same firm Intermountain did. Perhaps health systems should rethink adding to their already bloated C-suites. I mean how many marketing, digital, experience, etc., ‘leaders’ do they really need to come up with this stuff? I have interns who can crank out better options than this in an hour. Maybe hospitals really do need ChatGPT.” Sentara claims to possess a newfound focus on overall health in renaming itself to Sentara Health, also announcing plans to rename its health plans under Sentara Health Plans. The president and CEO claims that the slightly new name will make healthcare simple, seamless, personal, and more affordable, apparently anxious to break free of being held back all these years by the omission of “health” in its name. Oddly, the organization says people should just keep calling it “Sentara” when talking about it. Interestingly, Sentara’s first hospital under its old name was called Retreat for the Sick, which seems most accurate and least gimmicky. The ever-growing health system chose the Sentara name in 1987 following a consultant’s recommendation to pick a meaningless name that it could copyright. It has since (expensively) gone through the usual hospital evolution of trendy names – Sentara Health System, Sentara Healthcare, Sentara, and now Sentara Health. Despite their emphasis on “health,” they still make most of their money from “healthcare.” I consulted with ChatGPT, which opines that spending all that money when Sentara is already well known as a healthcare organization might be silly, not to mention that business name changes usually involve shortening a name rather than making it longer.
HIStalk Announcements and Requests
That big banner spot at the top of every HIStalk page is available after years of being fully booked, so get in touch if your company is interested.

Welcome to new HIStalk Platinum Sponsor Waystar. Healthcare payments are too complex for providers and patients. It’s time to simplify. Waystar’s technology is the way to make healthcare payments more human, helping your team prioritize care, improve margins, and give patients more clarity and trust. Waystar provides market-leading technology that simplifies and unifies healthcare payments. Its cloud-based platform streamlines workflows and improves financials for healthcare providers of all kinds, and brings more transparency to the patient financial experience. The Waystar platform is used by more than 450,000 providers, 750 health systems and hospitals, and 5,000 health plans and integrates with all major HIS and practice management systems. Thanks to Waystar for supporting HIStalk.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
Acquisitions, Funding, Business, and Stock

Premier Inc. is evaluating strategic alternatives that could involve selling some or all of the company. PINC shares – which rose 6% on the announcement — are down 28% in the past 12 months versus the Nasdaq’s 1% gain, valuing the company at $3 billion. The company said in its most recent earnings call in February 2023 that it would realign its Remitra invoice and payment platform business due to slower-than-expected adoption. It noted that its group purchasing business was being affected by lower provider utilization, reduced pricing and demand for pandemic-related categories, and provider use of previously stockpiled supplies. Premier has implemented a cost savings plan that included layoffs.
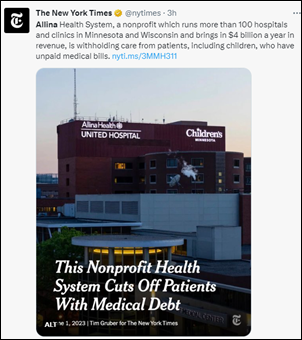
The New York Times looks at the rapid pace at which big corporations such as CVS Health and Amazon are acquiring primary care practices, especially those that serve Medicare Advantage patients. Seven in 10 doctors are employed by either a health system or a corporation, and while those owners tout cost savings and care coordination, experts warn that profit-seeking behavior will increase overall costs and frustrate patients and providers with gatekeeping functions such as prior authorization. The at-risk shared cost saving structure of Medicare Advantage allows primary care doctors to be paid up to $14,000 per year to manage a single patient instead of a few hundred dollars per visit.
Sales
- Australia’s Northern Health contracts for Agfa’s enterprise imaging solution for radiology.
- Weirton Medical Center (WV) will implement Oracle Cerner in a $65 million project. The hospital sued Cerner in 2017 over problems with its $30 million implementation in 2013 of Siemens Health Services Soarian. Cerner acquired that company in early 2015. The hospital said Cerner executives told them that they had inherited an unprofitable deal, after which Cerner failed to keep the promises Siemens had made.
- Nashville General Hospital (TN) will implement RLDatix solutions for governance, risk, compliance, and workforce management.
People

Jackson Healthcare promotes Brad Chason to SVP of IT.

Edifecs hires Chris Lance, MBA (Evolent Health) as chief product officer.

Medicus promotes Tony Niemotka to EVP of community health.
Announcements and Implementations
Medhost’s Medteam Solutions services business launches a managed IT services program that includes infrastructure management, network administration, and desktop support.
Harrison County Community Hospital (MO) goes live on Meditech Expanse’s patient portal, while Pinckneyville Community Hospital implements the full Meditech Expanse system.
Northwell Health provides $500,000 in funding each of to two employee-proposed innovation projects: (a) an AI-enabled solution to navigate cancer patients to care and clinical trials; and (b) a trigeminal nerve stimulator to help in recovery of acute ischemic stroke.
Australia will spend $290 million in a two-year project to modernize its My Health Record system, which will include a new national repository and increased connection to GPs and pharmacies. The health minister describes the system, which was implemented as a personally controlled EHR in 2012, as “a pretty outdated, clunky, PDF format system.”
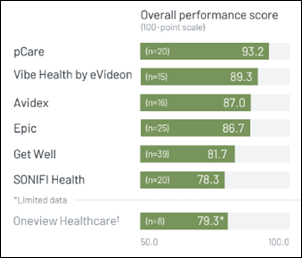
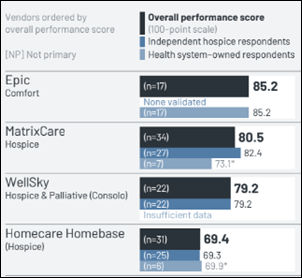
A new KLAS report on interactive patient systems – which include patient care coordination, BYOD integration, non-clinical service requests, room controls, feedback surveys digital door signs, digital whiteboards, and in-room telehealth – finds that PCare earns the top performance score of 93.2. Vibe Health by EVideon is broadly evaluated in all areas except BYOD integration, while Epic, Sonifi Health, and Oneview Healthcare are rarely seen as complete solutions.
Government and Politics

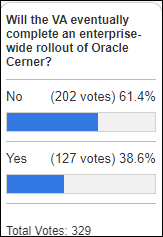
The VA tells the technology modernization committee of the House Committee on Veterans’ Affairs that while Oracle Cerner is improving its pharmacy software, the changes are “small and incremental”and need to be sped up. Oracle EVP Mike Sicilia says that Cerner had provided the VA with an “unacceptable” timeline of three years to fix problems involving integration of Medication Manager Retail to PowerChart to support the VA’s role as both prescriber and prescription filler. Sicilia did not mention his previous commitment for Oracle to rewrite the pharmacy system by April 2023. Committee chair Rep. Matt Rosendale (R-MT) closed the hearing by saying that, “The worst thing the VA could do is to continue down this dead-end road perpetuating the same failed strategy” and says that he expects to see the VA “disentangle itself from this monopoly” by next week’s contract renegotiation deadline, urging the VA to “cut their losses and move on” because Oracle is unlikely to be able to resolve existing problems quickly enough to meet the VA’s needs.
Privacy and Security
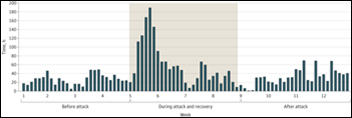
A study finds that one hospital’s ransomware attack disrupts other local EDs, leading the authors to recommend that cyberattacks be treated as disasters with coordinated planning and response efforts. The authors found that the EDs of hospitals that were not part of the cyberattack saw resulting jumps in patient census, ambulance arrivals, waiting room times, patients who left without being seen, and length of stay as the affected hospital recovered its systems.
Other
Northwell Health sues a former Long Island Jewish Medical Center morgue attendant who allegedly posted autopsy videos on her Instagram and TikTok accounts under the name “Autopsy Bae.” Hospital administrators confronted Quantaise Sharpton, who expressed no remorse for being an “influencer” with 20,000 followers who monetizes morgue “content.” She also claimed that her intention was to inspire her followers to pursue mortician and autopsy careers.
Sponsor Updates
- Clinical Architecture releases its “2023 Healthcare Data Quality Report,” highlighting the impact that data quality has on patient care and organization performance.
- Black Book Research announces that Netsmart has swept the post-acute health technology platform ratings for highest customer satisfaction in its annual client experience polling of 20 top vendors.
- Access publishes a new patient e-signature case study, “Northern Regional Hospital: Creating a Better Experience for Healthcare Workers and Patients.”
- AdvancedMD publishes a new e-book, “The Current State of Telehealth in Ambulatory Care.”
- Arrive Health publishes a new white paper, “The Terrifying Truth About America’s Healthcare Affordability Crisis.”
- Availity wins the platinum-level Healthiest Companies Award from the First Coast Worksite Wellness Council.
- Baker Tilly publishes a new case study, “Medical products provider undergoes PMO assessment to prioritize initiatives and improve technology landscape.”
- ChartSpan and Illinois Primary Health Care Association partner for better health outcomes in Illinois.
- CTG releases a new episode of its This Week Health Podcast featuring Managing Director of Health Solutions in North America Tanya Johnson.
Blog Posts
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.













































































































































Thank you for the mention, Dr. Jayne — we appreciate the callout, the kind words and learning more about the…