EPtalk by Dr. Jayne 4/21/22
Telehealth company Amwell adds two new clinical programs to its platform. Payers can brand the offerings as part of their digital engagement strategies. The dermatology program offers sessions with board-certified dermatologists in an effort to alleviate delays in dermatologic consultations which can be several months in many parts of the country. The press release notes that it offers “most diagnoses returned in just 24 hours,” which makes me wonder if it’s an asynchronous offering versus a virtual visit with a dermatologist. The musculoskeletal program will help payers address challenges with physical therapy access, disrupted productivity, and downstream costs. It will provide patients with a personalized physical therapy plan, telehealth visits, digital sensors for guided exercise sessions, behavioral health support, and patient engagement services.
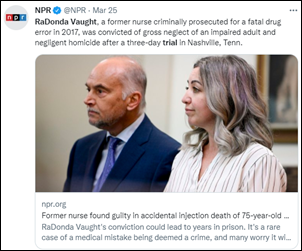
This article about non-fungible tokens (NFTs) caught my eye since it’s not often that you see them mentioned in the same sentence as “medical ethicists.” It raises important points about the fact that EHR data is being sold without patients being fully aware of it. How many of us actually read the documents given to us at medical appointments such as the Consent to Treat, Assignment of Benefits, and HIPAA Notice of Privacy Practices? The numbers are likely low because we just want to be treated and aren’t going to walk away regardless of what’s in there, for the most part. The last time I was at my local academic medical center, I was asked to sign a signature pad saying I had received the documents despite not having been actually offered the documents.
The premise is that a patient could own an NFT of their medical information, which could be stored in a secure database that would track access requests and approvals. The piece also points out that patients could maintain ownership of their biological specimens, from blood to tissue and even down to the cellular level. When you learn about the cell lines used in research and where they came from, there’s been tremendous injustice. (“The Immortal Life of Henrietta Lacks” is a great read if you’re curious.) Some ethics professionals disagree, saying that ownership of such data is shared between patients and the physicians and health systems who are involved in their care. The article notes that there needs to be a balance between privacy and public health along with greater understanding of why patients might not want to share their data.
There are also sustainability concerns around the creation of NFTs and maintaining the blockchains used to track them, as well as the risks of data making it outside of the public ledger or it moving to the black market. One researcher points out that “you can’t de-identify something with a genome,” reminding us of the uniqueness of each and every one of us. I would settle for greater attention to how patients are informed of the ways in which their information is used, and protections for those who want to opt-out of having their data become part of anonymized data sets that lead to profits for others. I’m not sure what the other potential answers are here, but will be interested to see how things evolve over the coming years.
With as much time as I’ve spent recently with marketing and branding exercises, I was surprised to learn that “debranding” is also a thing. Upon further review, it’s an extension of branding, but with a focus on simplicity and cleaner design. Examples include removing complicated color gradients or shadows in order to make logos cleaner. Increased use of mobile devices is a driving factor, as is a drive towards a more professional appearance. It’s fun to look at certain brands and see how their presentation has changed over time, especially in the consumer space.
A recent KLAS publication looked at the causes of clinician turnover. Although nurses are most likely to leave in the next year, other types of clinicians are close behind. EHR and IT tools are cited as a major cause, along with burnout, chaotic work environment, lack of personal control over workload, and more. I recently joined an online physician forum for EHR issues and have been shocked that the majority of questions are actually operational and management questions rather than technology issues, but physicians are turning to technology hacks to try to fix deeper issues.
I feel like I’m yelling into the void every time I say something along the lines of, “This is an operational issue requiring a policy and procedure to keep your practice staff from dumping on you, not something that needs another macro or preference or configuration in your EHR.” One physician confided in me that her two partners have left because the practice, owned by a large health system, is so chaotic and mismanaged. Rather than hiring a locum tenens physician until they can fix the problem and find permanent hires, the employer expects her to manage a panel of over 10,000 patients by herself with only a front desk staffer and two medical assistants. This is in a semi-rural area, and I’ve seen the complexity of her case mix. She’s to the point where she’s ready to resign if she doesn’t get some help, and the health system doesn’t seem to care. From a couple of decades in practice management and healthcare operations, I’d bet on the fact that better EHR templates and macros to respond to patient portal messages are not the answer. Shame on the health system for letting it get to this point and especially for thinking this is an acceptable solution.
When people are under stress, they turn to different diversions – often during the workday. If my Facebook feed is any reflection, there are many people are into playing the New York Times Wordle game. There have been plenty of imitators as well as specialty games. If you’re looking for some brain-stretching timewasters, I offer for your consideration:
Ever gotten the Wordle on the first try? How fast can you transcribe Morse code? Leave a comment or email me.

Email Dr. Jayne.










I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…