Top News
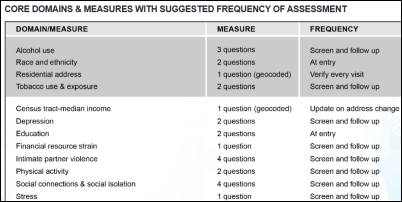
The Institute of Medicine urges ONC and CMS to add additional social and behavioral health measures to EHR certification and Meaningful use criteria to allow researchers and health systems to uncover determinants of health. The unshaded items on the list above, involving 17 patient questions, would be new for most providers.
Reader Comments


From Flatus Maximus: “Re: ONC’s data matching project. I can’t believe that ONC thinks that these two (or anyone, for that matter) can solve this problem in two years given the huge legal an policy issues. I don’t think ONC understands that this is a socio-technical problem that requires more than a technology fix.” ONC and HIMSS bring in two people to solve the patient identity matching problem via HHS’s “Innovators in Residence” program that temporarily hires technologists to fix specific problems. Hired were Catherine Costa, RN (marketing director at PatientPoint) and Adam Culbertson (NIH biomedical informatics fellow). Political reality takes the obvious answer off the table: a unique consumer ID with biometric verification.
HIStalk Announcements and Requests
This week on HIStalk Practice: The Massachusetts eHealth Institute offers grants to spur EHR adoption among behavioral health and long-term care providers. New York inches closer to becoming the largest HIE in the nation. SCHIEx and GaHIN launch one of the first state-to-state HIE connections. Billings Clinic implements vein scanners. Envision Medical Group selects new Aprima RCM services. Florida Heart & Vascular’s IT Administrator details the tough time they’ve had with EHRs.
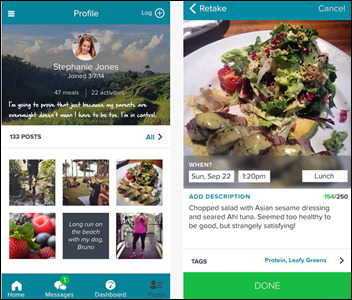
This week on HIStalk Connect: The Nokia Health Sensor XPRIZE competition concludes, with DMI Diagnostics taking the $525,000 grand prize. Samsung opens its SAMI health data SDK service to developers and showcases its new open design Simband prototype. Two Singularity University grads raise $12 million to launch a machine learning-backed population health platform. Ginger.io announces a handful of new research partnerships that will test its behavioral health app within a variety of remote patient monitoring initiatives.
Webinars
November 18 (Tuesday) 1:00 ET. Cerner Takeover of Siemens, Are You Ready? Sponsored by HIStalk. Presenters: Frank L. Poggio, president and CEO, The Kelzon Group; Vince Ciotti, principal, HIS Professionals. The Cerner acquisition of Siemens impacts 1,000 hospitals that could be forced into a “take it or leave it” situation based on lessons learned from similar takeovers. This webinar will review the possible fate of each Siemens HIS product, the impact of the acquisition on ongoing R&D, available market alternatives, and steps Siemens clients should take to prepare.
November 19 (Wednesday) 1:00 ET. Improving Trial Accrual by Engaging the Digital Healthcare Consumer. Sponsored by DocuSign. Presenters: B. J. Rimel, MD, gynecologic oncologist, Cedars-Sinai Medial Center; Jennifer Royer, product marketing, DocuSign. The Women’s Cancer Program increased trial accrual five-fold by implementing an online registry that links participants to research studies, digitizing and simplifying a cumbersome, paper-based process. This webinar will describe the use of e-consents and social marketing to engage a broader population and advance research while saving time and reducing costs.
Acquisitions, Funding, Business, and Stock

Australian telecommunications company Telstra’s health division acquires 2 percent of New Zealand-based Orion Health prior to Orion’s upcoming IPO that values the company at $725 million.

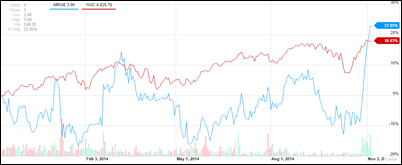
MMRGlobal, which makes a lot of its money licensing (via nuisance vendor infringement lawsuits) its PHR and other medically related technology, took in nearly $2 million in the most recent quarter, up 1,584 percent over last year. I interviewed CEO Bob Lorsch last year and asked him some pointed questions about the company’s business model – you can decide what you think about it.

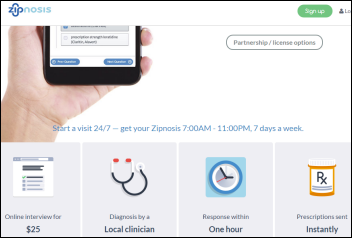
Xerox invests in telemedicine kiosk vendor HealthSpot and will provide it with cloud hosting, system integration, and claims processing services.
The Portland, OR business paper highlights the $150 million venture fund of Providence Health & Services, which is looking for healthcare startups in telehealth, wearables, clinical applications, and e-commerce that seek up to $5 million. The fund is finishing due diligence on four unnamed companies. The fund’s partner explains, “The point isn’t just financial. Our chief investment officer could buy bonds. Our goal to make products and services that help our community, our patients, our members and providers.”

IBM invests an unspecified amount from its Watson investment fund in genetic testing company Pathway Genomics, which will develop a Watson-powered mobile app that will answer a consumer’s health questions by analyzing information from their wearables, genetic markers, and electronic health records.
Sales
Baylor Scott & White Health selects McKesson’s Performance Analytics, Analytics Explorer, and Pay-for-Performance for financial analytics.
City of Health and Science University of Turin, Italy chooses InterSystems TrakCare.
Wellmark Blue Cross and Blue Shield (IA) will implement employer reporting from MedeAnalytics.
Presbyterian Medical Services (NM) selects the analytics platform of Lightbeam Health Solutions.
Christus Health signs a five-year extension with Strata Decision Technology.
NantHealth licenses Streamline Health’s Looking Glass analytics to track populations and compare clinical effectiveness.

MaineGeneral Health (the combined words represent their conceptual mistake, not my typographic one) renews its Allscripts Sunrise and TouchWorks agreements and adds FollowMyHealth.
People

Nordic Consulting CEO and co-founder Mark Bakken will leave the company to start a venture capital fund in which he and Nordic will invest.

Ed Kopetsky, CIO of Lucile Packard Children’s Hospital Stanford (CA), receives the Distinguished Achievement Award of his alma mater, University of Wisconsin-Madison and its College of Engineering.

Allina Health announces that CEO Ken Paulus will retire at the end of the year, with President and Chief Clinical Officer Penny Wheeler, MD replacing him. She’s done quite a bit of work with their Epic and data warehouse systems.
Announcements and Implementations
Named to Deloitte’s “2014 Technology Fast 500” are DrFirst, Etransmedia, Imprivata, InstaMed, Kareo, Liaison Technologies, Qlik, VMware, and ZeOmega.

Silver Hill Hospital (CT) implements QPID Health’s Cohort App to product HBIPS behavioral health quality metrics and will work with the company to deliver a behavioral health portal.
Billings Clinic (MT) goes live on patient identification via palm vein scanning using technology from PatientSecure that is integrated with its Cerner system.
The medical school of Mount Sinai (NY) enrolls its first patient in a televideo-powered prostate cancer clinical trial, working with real-time patient management solutions vendor AMC Health.
The state HIEs of Georgia and South Carolina connect to each other with the help of technology partners Truven Health Analytics and CareEvolution.
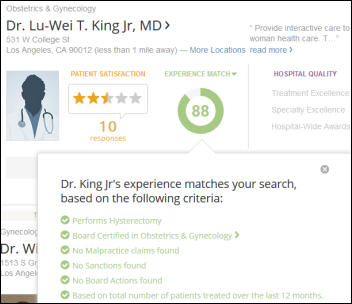
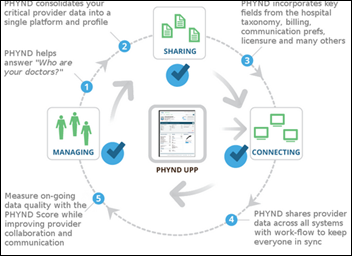
Healthgrades launches a new version of its doctor search site that uses claims data to show users the level of experience a doctor has with a given procedure or diagnosis.

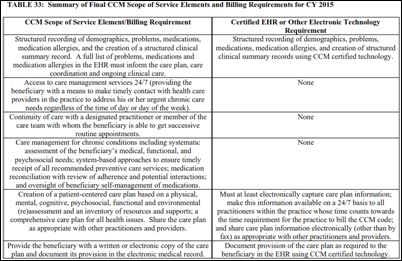
Intel-GE Care Innovations announces Health Harmony, a remote patient monitoring platform that aggregates information for clinician review and helps them collect the new $40 per month Medicare payment for chronic care management. The joint venture was started in January 2011. Only one executive remains of its original 10-member management team.
Novant Health (NC) joins the federal eHealth Exchange, adding that so far this year it has shared 148,000 patient records via Epic’s interoperability as well as a total shared record count of 38 million this year.
Government and Politics
UCSF School of Medicine Professor Bob Wachter, MD says the “accidental” Meaningful Use program has achieved its goals of putting stimulus dollars on the street and increasing EHR use, but says that Meaningful Use Stage 2 is an indication that ONC should be put out to pasture once it has handed out its remaining incentive money. He says it’s time to declare victory, move Meaningful Use toward encouraging API-driven interoperability, and let quality and clinical demands rather than government checklists drive the technology market.
CMS releases three free ICD-10 education resources that offer CME and nurse CE credits.

In the UK, the Department of Health’s National Information Board creates a wide-ranging, technology-focused policy draft covering digital health over the next several years. Highlights:
- EHRs are used by 96 percent of doctors, but only 4 percent of them allow patients to see their information. All will be required to offer patient access by April 2015.
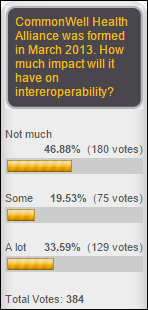
- Technology has had minimal impact on the patient experience.
- Interoperability is a big problem, as hospital systems are “impenetrable” and little electronic information exists for nursing home and hospice patients.
- Hospitals and practices don’t integrate their services with mental health and social care.
- Digital services should be the default delivery channel, with services such as appointment booking and prescription refill requests combined into a single information platform (an extension of NHS Choices) that requires citizens to verify their identity through the Government Digital Services IDA program.
- Health-related apps and devices should be nationally accredited and service marked to encourage their adoption
- Specifications will be published by April 1, 2015 for accessing NHS’s core systems, such as Spine and e-referrals.
- NHS England will pilot technology in which patients will hold their electronic records and a personal budget.
- A national pilot will give consumers a PHR that they control that is also available in real time to clinicians, which will also include their end-of-life preferences.
- NHS will seek universal adoption of its healthcare ID number, which was introduced in April 2014 as the primary identifier in clinical correspondence.
- NHS will propose that clinical systems adopt clinical structure standards developed by the Academy of Royal Medical Colleges.
- The entire health system will adopt SNOMED CT clinical terminology by April 2020, while additional work with semantic web technologies will be undertaken.
- NHS England will develop a standard for adopting the GS1 identification standard of patients, products, and places as well as RFID tagging.
- NHS will reduce the number of organizations that collect patient information for purposes other than clinical care, moving by 2020 to process that requires patients to consent to having their data shared.
- The Department of Health has created the role of National Data Guardian for health, which will lead efforts inform patients where their data has been used and the benefits they received as a result. Named to the role is Dame Fiona Caldicott, chair of the Oxford University Hospitals NHS Trust and a psychiatrist whose government-created committee reviewed the protection and use of patient information in 1997.
- Technology made available under the General Practice Systems of Choice will be more selectively targeted to encourage integrated services, SaaS-based systems for new providers of primary care services, and innovative systems for non-hospital services.
- IT investment will shift to investments that support older citizens, those with chronic conditions, and those being cared for informally.
- NHS England will decide with the GPSoC contract ends in April 2018 whether it should continue or whether PCP payments should be increased to let them buy whatever systems they want as long as they meet data standards.
Also in England, the $6 billion fund created to reduce ED visits and readmissions of elderly patients is declared a “shambles” by auditors who say it probably won’t save NHS even one-third of the original $1.5 billion estimate.

A Reuters report says that the Federal Trade Commission has been meeting with Apple for several months to make sure the health information contained in HealthKit and Apple’s upcoming smart watch will be managed appropriately and not shared with third parties as was found to be the case with health and fitness apps from other companies. Sources say Apple is considering hiring a health privacy czar.
Innovation and Research

A study of Pennsylvania’s mandatory hospital patient safety reporting database finds that “advanced EMRs lead to a 27 percent decline in patient safety events.” I was predisposed to not liking the article because its overly cute title asks a question rather than states a conclusion (“Saving Patient Ryan – Can Advanced Medical Records Make Patient Care Safer?”) and its regurgitative academic meandering goes on for 40 painful pages. However, I originally assumed the authors didn’t look at individual hospital performance pre- and post-EHR, but I asked an expert in statistics to wade through the endless graphs and methods to tell me and he says they did, which is admirable. That still leaves a few weak links – underreporting of errors, failing to distinguish between how individual EHRs were implemented, and non-EHR confounders that make proving causation difficult – but overall it seems to be pretty solid as long as you trust the HIMSS Analytics database, which was built for selling data to vendors for marketing rather than research.
Other
India-based hospital chain Narayana Health, best known for performing high-volume and low-cost heart surgeries, opens Health City Cayman Islands in a joint venture with Ascension Health. It expects the 108-bed hospital, its first outside of India, to expand to 2,000 beds as it capitalizes on a location near (but not in) the US for medical tourism. The hospital chain prices its services in flat rate bundles and sends the patient a single, all-inclusive bill. The Cayman Islands hospital has a sophisticated EHR, its clinicians use Google Glass and smart watches to review information and communicate with patients as they round, and (most interesting to me) every patient gets a mobile tablet that is updated with their most current information. The chain is also a big user of telemedicine, where India-based command center doctors monitor patients all over the world. Health Catalyst created the video above that includes a profile of Narayana Health’s founder, philanthropist and cardiac surgeon Devi Shetty, called “the Henry Ford of heart surgery” by the Wall Street Journal. He also designed a comprehensive health insurance plan for poor farmers in India that costs 20 cents per month.
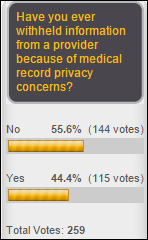
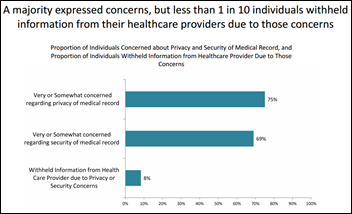
An interesting survey finds that Americans are increasingly worried about their electronic privacy, yet continue using the services they distrust (social media, text messaging, email, and cell phones) because they don’t see an alternative. They’re also willing to give up privacy in return for getting something free, such as providing personal information to use a website.

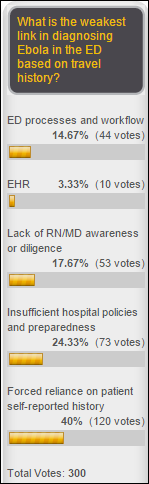
Texas Health Resources apologizes, creates a memorial fund, and pays an undisclosed settlement to the family of deceased patient Thomas Duncan for discharging him from its ED without making an Ebola diagnosis. Meanwhile, Duncan’s fiancée signs a book deal.

The former CFO of Shelby Regional Medical Center (TX) pleads guilty to falsifying the hospital’s Meaningful Use attestation in November 2012, earning it a $785,655 CMS payment. He faces up to five years in federal prison. The CFO, who rose from the position of maintenance worker, claimed the hospital used EHRs when in fact it remained mostly paper-based and entered minimal EHR information after discharge. He attested using the Social Security number of another employee who refused to put his own name on the form. The for-profit hospital, since closed, was one of six owned by Tariq Mahmood, MD, who was involved in the scheme and was found guilty in July 2014 of healthcare fraud, identity theft, and conspiracy. He threatened to fire coders who declined to falsify diagnosis codes and hand-wrote his own additions to patient records to maximize billing. The six hospitals were paid $18 million in HITECH money despite ongoing allegations of fraud from former administrators going back to 2008. CMS didn’t even know Mahmood owned multiple hospitals.

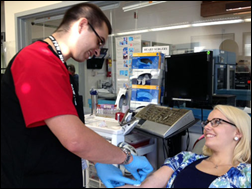
Spartanburg Regional Healthcare System (SC) celebrated Veterans Day by honoring 240 of its employees, volunteers, and contractors who are veterans. VP/CIO Harold Moore (second from left) was among the executives serving lunch. It looks like barbeque given the squirt bottles of what could be the mustard-based South Carolina style sauce that isn’t my favorite, but the picture wasn’t clear enough for definitive zooming.

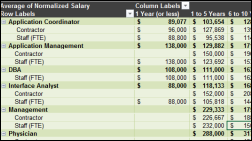
Niko Skievaski polls some of his fellow Epic alumni to determine why they left the company, with results that aren’t too surprising since they are similar in most places: lack of work-life balance, technicians with poor people skills who are promoted into management, and lack of company appreciation. Meanwhile, copies of Niko’s “MU2 Illustrated” art book have arrived from the publisher and are ready to ship. His projects are often fun, marginally commercial, and reflective of his youthful optimism, so Lorre contributed some art and I wrote the book’s foreword. We’ll probably have a virtual launch party or something just for fun and maybe invite him to sign books at our microscopic HIMSS booth.
Weird News Andy gestated this story that makes his heart go pitter-patter. Doctors at a Florida hospital perform CPR for three hours trying to resuscitate a woman who had an amniotic fluid embolism (which has a fatality rate of at least 25 percent, up to 90 percent in some studies) during an otherwise successful C-section. The team called the family into the room to say goodbye after 45 minutes of a flat-line ECG, but just as they were pronouncing her, she spontaneously revived. The baby is fine and the mom is not only alive, but miraculously free of brain damage.
Sponsor Updates

- MediQuant’s employees launch a fundraiser to help build a school in Sierra Leone, with a goal of $5,000. A fundraiser will be held tonight (Friday) in Broadview Heights, OH and donations are being accepted. Company President Tony Paparella spent two years as a Peace Corps volunteer in Sierra Leone and will personally match the funds raised. Tony also plays harmonica in the company band The DeCommissioners and their “Legacy System Blues.”
- First Databank informatics pharmacists Joan Kapusnik-Uner, PharmD and George Robinson, RPh will present sessions on pharmacy informatics and drug terminology standards at AMIA’s Annual Symposium November 15-19 in Washington, DC.
- TeraMedica will debut Evercore 6.0, the latest version of its vendor-neutral archive, at RSNA.
EPtalk by Dr. Jayne

I’ve subscribed to multiple CMS mailing lists in an attempt to stay current as an Eligible Provider. It’s to the point, however, that it’s a rare day when I don’t hear from CMS when I open my inbox. This morning’s offering gave me chuckle, however, as CMS is “pleased to announce that the 2012 Electronic Prescribing (eRX) Incentive Program Supplemental Incentive Payments are now available.”
Originally I thought it was a typo, but yes, now that it’s November 2014, you can get your money for 2012. I hope no one switched jobs because payments are going as a lump sum to the taxpayer ID associated with the claims. I’m not sure why it takes 20+ months to figure out the payments, so feel free to clue me in.
I spent a couple of days earlier in the week at Ebola response training. Our hospital asked for physician volunteers and I was assigned to be one of the clinical documentation liaisons. Essentially my job would be to scribe documentation as the care team treats patients. We’ve not been designated as a primary response site, but are training anyway, which is probably a good thing.
It’s a bit of a strange feeling though to have your EHR skills valued above your clinical skills. Experiencing what our scribes deal with on a daily basis was also an eye-opener. I’m putting some thoughts together on how to improve their documentation protocols and workflows.
There are still exhibitor openings available at the mHealth Summit’s Consumer Engagement and Wearables Pavilion. Even better, if you need a sassy spokesdoctor to show off your wearables, I might know where to find a couple. You could also pick our brains on what primary care physicians really think about wearables and how we do or do not want to handle the volumes of data that can be produced as patients quantify themselves.
I’m a big fan of my Garmin, but I’m pretty sure my doc just wants to know that I run at least five days a week as opposed to knowing what route I chose and what my lap split times were. My EHR vendor is starting to integrate personal tracker data and what we’re seeing come in is far more than we would ever want to see.

It’s possible that being at some vendor events last week has given me trade show fever. Although I wasn’t initially looking forward to the upcoming HIMSS conference — the keynote lineup certainly didn’t help — I found myself today dusting off last year’s Social Schedule Pocket Guide so I can keep my eye out for noteworthy happenings and interesting events.
For anyone making his or her first trip to the big show, HIMSS is offering a series of “HIMSS15 Unveiled” webinars for attendees to learn about the event’s education, exhibition, and networking opportunities. Learning objectives for the webinars promise to “identify the latest initiatives designed to enhance the attendee experience.” I’m hoping those initiatives involve mid-afternoon martinis and massage therapists at the end of every exhibitor aisle.

The holidays are approaching and I’m already dreading the dinner table conversations. In addition to the usual topics of Medicare and Social Security, we also have the recent elections as a potential discussion thread. To make things even better, the Supreme Court has agreed to hear King vs.Burwell, which addresses insurance premium subsidies under the Affordable Care Act. Thinking about those combinations almost makes me wistful for my favorite holiday table topic: health conditions of people that aren’t at the table.
Are you starting to plan for HIMSS? Have any suggestions for the holiday table? Email me.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.































































































































































Re: Deliberately Faked Academic Papers in Nature See, this doesn't surprise me at all. Of course AI quotes these bogus…