Neither of those sound like good news for Oracle Health. After the lofty proclamations of the last couple years. still…
Monday Morning Update 11/3/14
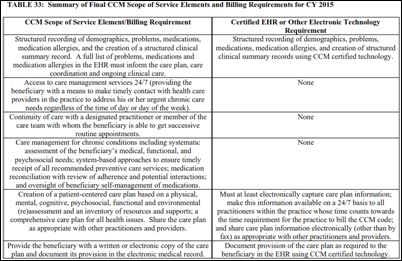
CMS adds a scope of service element to the final version of the Medicare Physician Fee Schedule for Calendar Year 2015 that would require providers who bill for Chronic Care Management services (a new reimbursement item) to use certified EHRs and patient-centered electronic care plans for demographics, problem list, meds, allergies, and a structured clinical summary record, using that technology to manage care transitions. The schedule also provides payment for several types of telehealth visits, including annual wellness and psychotherapy.
Reader Comments


From BigDeal: “Re: Epic lawsuit against Tata. Filed quietly Friday evening.” Epic sues India-based Tata Consultancy Services, seeking an injunction and damages for what it alleges is misuse of Epic’s confidential information. The lawsuit claims that Tata’s people downloaded information from Epic’s UserWeb in an “elaborate campaign” that could give that company an advantage in its project to develop a competing product. Epic’s lawsuit says that a Tata employee based in Portland, OR downloaded at least 6,477 documents from an India-based IP address after claiming to be a Kaiser employee and using a KP.org email address. Epic says that it questioned the employee and he first claimed that he didn’t download anything, but when presented with the audit log, admitted that he shared his UserWeb credentials with two other Tata employees. The lawsuit says Epic won’t identify the material it claims Tata stole unless the court grants a protective order to keep it out of the public record.
HIStalk Announcements and Requests
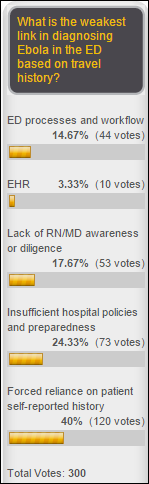
Ebola diagnosis is made harder by reliance on a patient’s self-reported history and a lack of hospital preparedness, poll respondents said, with only a small percentage blaming the EHR. New poll to your right or here: CommonWell Health Alliance is 20 months old – what will be its impact on interoperability? Add a thoughtful comment to impress others that you’re not just a reactionary poll-clicker.
Yes, it’s November already. The clocks have been turned back all over the US, excluding non-observers Arizona, Hawaii, and a few counties in Indiana. Stalwart hospital IT people gained an hour Sunday to make up for the sleep they lost in babysitting their systems just in case something went wrong. Thanksgiving (and thus RSNA shortly afterward) is three weeks from Thursday.
Thanks to the following sponsors, new and renewing, that recently supported HIStalk, HIStalk Practice, and HIStalk Connect. Click a logo for more information.
Listening: new goosebump-inducing blood harmonies from Indianapolis-based Lily & Madeleine, who sing together as only sisters can. They sound eerily similar to First Aid Kit, which is a good thing.
Last Week’s Most Interesting News
- McKesson announces that its RelayHealth unit has signed a multi-year agreement as the technology provider for CommonWell Health Alliance.
- Google X Life Sciences says it hopes to bring a swallowed sensor to market within five years that can detect molecular-level health problems.
- California’s attorney general issues her 2014 breach report that says healthcare lags only retail in exposing the information of individuals, largely because many provider organizations don’t encrypt mobile devices.
- HHS, responding to negative industry reaction to a nearly complete loss of ONC leadership over the past few months, announces that Karen DeSalvo will continue to oversee ONC’s work even while reassigned as Acting Assistant Secretary for Health.
- CCHIT announces that it has shut down effective immediately after losing its primary revenue source by exiting the certification business in January 2014.
- The first UK hospitals go live on Epic.
- Reuters suggests that Salesforce is about to make a major push into healthcare.
Webinars
November 5 (Wednesday) 1:00 ET. Keeping it Clean: How Data Profiling Leads to Trusted Data. Sponsored by Encore, A Quintiles Company. Presenters: Lori Yackanicz, administrator of clinical informatics, Lehigh Valley Health Network; Randy L. Thomas, associate partner of performance analytics, Encore, A Quintiles Company; Joy Ales, MHA, BSN, RN, senior consultant, Encore, A Quintiles Company. Data dictionaries, organizational standards, and pick lists for data entry fields may describe the intent of a particular data field, but don’t guarantee that the data captured in the source system actually reflects that intent. Data profiling is the statistical analysis and assessment of the data values in source systems for consistency, uniqueness, and logic to ensure that the data landing in a data warehouse or analytic application is as expected. Attendees will learn which projects benefit from data profiling and the resources needed to accomplish it.
November 12 (Wednesday) 1:00 ET. Three Ways to Improve Care Transitions Using an HIE Encounter Notification Service. Sponsored by Audacious Inquiry. Presenters: Steven Kravet, MD, MBA, FACP, president, Johns Hopkins Community Physicians; Jennifer Bailey, senior director of quality and transformation, Johns Hopkins Community Physicians; Robert Horst, principal, Audacious Inquiry. Johns Hopkins Community Physicians reduced readmissions and improved quality by implementing a real-time, ADT-based encounter notification service (ENS) to keep the member’s healthcare team informed during transitions in care. Johns Hopkins presenters will describe the clinical, operational, and financial value of the ENS for care coordination along with its technology underpinnings.
November 18 (Tuesday) 1:00 ET. Cerner Takeover of Siemens, Are You Ready? Sponsored by HIStalk. Presenters: Frank L. Poggio, president and CEO, The Kelzon Group; Vince Ciotti, principal, HIS Professionals. The Cerner acquisition of Siemens impacts 1,000 hospitals that could be forced into a “take it or leave it” situation based on lessons learned from similar takeovers. This webinar will review the possible fate of each Siemens HIS product, the impact of the acquisition on ongoing R&D, available market alternatives, and steps Siemens clients should take to prepare.
November 19 (Wednesday) 1:00 ET. Improving Trial Accrual by Engaging the Digital Healthcare Consumer: How to Increase Enrollment with Online Consents and Social Marketing. Sponsored by DocuSign. Presenters: B. J. Rimel, MD, gynecologic oncologist, Cedars-Sinai Medial Center; Jennifer Royer, product marketing, DocuSign. The Women’s Cancer Program increased trial accrual five-fold by implementing an online registry that links participants to research studies, digitizing and simplifying a cumbersome, paper-based process. This webinar will describe the use of e-consents and social marketing to engage a broader population and advance research while saving time and reducing costs.
Recordings of recent webinars are available on YouTube:
Electronic Prescribing of Controlled Substances Is Here. What Should You Do?
Data Governance – Why You Can’t Put It Off
Using BI Maturity Models to Tap the Power of Analytics
Electronic Health Record Divorce Rates on the Rise- The Four Factors that Predict Long-term Success
Meaningful Use Stage 2 Veterans Speak Out: Implementing Direct Secure Messaging for Success
Acquisitions, Funding, Business, and Stock
A New Mountain Capital fund acquires release of information vendor HealthPort. CompuGroup bought the company’s IT solutions business for $24 million in late 2010 as HealthPort had been rumored to have been exploring both an outright sale of the company and an IPO.
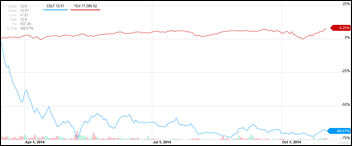
Castlight Health reports Q3 results: revenue up 238 percent, adjusted EPS –$0.18 vs –$1.58, beating analyst estimates of both. Shares dropped nearly 4 percent Friday after Thursday’s announcement. Above is the one-year CSLT share price (blue, down 69 percent) vs. the Dow (red, up 8 percent).
Oncology decision support vendor COTA names Eric Schultz (Quantia) as CEO.
Announcements and Implementations

Philips extends its Lifeline medical alert service to Lifeline GoSafe, a mobile service that uses multiple GPS location technologies to locate users who need help while away from home. A press of the button initiates two-way communication with the monitoring station via AT&T’s network. The system also automatically detects falls and places a call for help. Monthly services starts at $55. I’m a lot more interested in technology like this than wearables that monitor questionably useful body data.
Cleveland Clinic’s annual “Top 10 Medical Innovations” list includes only one healthcare IT-related item, but it came in at #1: mobile stroke units in which ambulances connect with hospital-based stroke neurologists via broadband-connected video. The list’s track record from prior years is pretty good: it previously included private sector HIEs (2009), telehealth-based CHF monitoring (2011), mobile device apps (2012), and big data analysis (2012).
Government and Politics
A report from the HHS OIG finds that Medicare keeps paying for expensive prescription drugs after the patient has died, following a CMS policy that allows prescriptions to be filled at its expense for up to 32 days after death. The report urged an immediate policy change, saying that post-death prescriptions “clearly are not medically indicated.” Some of the drugs are expensive and are feared to have been diverted to the black market. CMS says it’s fixing the problem. Perhaps there’s an ICD-10 code for normal respiration — not holding your breath.
Google fine tunes its Flu Trends tool to include CDC data, acknowledging research from earlier this year that showed that the accuracy of Google’s own “big data” approach was improved when combined with even bigger data.
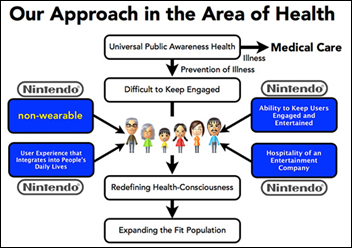
Nintendo creates a health division and is working with sleep disorders product vendor ResMed to develop a “quality of life” sleep and fatigue tracker that it will sell as a subscription service. The hand-sized device will use microwave-based sensors to collect information from the bedside. It won’t be available for several months. ResMed announced its S+ product a month ago that offers “the world’s first contactless sleep sensor.” Its bedside monitor measures breathing, body movements, and room conditions, sending the information to apps that track sleep scores and recommend changes. Nintendo says the health division, which appears to include the Wii Fit and Brain Age, will be profitable in the 2015/2016 financial year.
Other
Dean Sittig and Hardeep Singh observe in a Future Medicine editorial that too many factors exist to make comparison of one EHR vs. another possible in comparative effectiveness research, proposing instead that they be evaluated by how they’re used in the field. They provide some examples, although I found them to be insufficient to picture the possibilities the authors envision. I would also see more value in using that kind of framework to assess how a given user implements their EHR of choice since in hospitals at least, the new/replacement market has consolidated into just A and B – Cerner and Epic, with some Meditech in the mix for smaller, non-academic health systems, reducing the need to compare the short list of products. My bottom line: treat EHRs as the ubiquitous medical tool or device they have become by letting providers make their own choices, but then hold them accountable for the patient outcomes that result, no different than for a patient monitor or IV pump that can’t be evaluated in a vacuum other than for safety and usability. All the certifications, rankings, and independent evaluations don’t mean a thing if a hospital implements a highly regarded system without seeing improvements in outcomes measures – otherwise, why bother? (other than to rake in more revenue) I never cease to be amazed that hospitals rarely publish their pre- and post-EHR quality metrics after spending dozens or hundreds of millions of dollars to implement systems they assured would do exactly that. The article’s examples:
- Convert free-text entries using natural language processing instead of forcing users to choose from drop-downs.
- Perform drug-lab interaction checks at the point of care and not just during order entry.
- Assess the usefulness of on-screen clinical warnings by measuring how often the provider cancels the order that triggered the alert.
- Evaluate whether implementing Meaningful Use data entry requirements improves outcomes.
Epic will pay $5.4 million to settle a class action lawsuit brought by 45 quality assurance employees who claimed they should have been paid overtime wages. Each employee will be paid for their clocked hours plus 3.7 hours per week in assumed off-the-clock time. Money left over in the fund after the employees and attorneys have been paid, if any, will be donated to Access Community Health Centers.

Awards given at CHIME’s Fall CIO Forum:
- Neal Patterson, chairman and CEO, Cerner — Industry Leader Award
- Truman Medical Centers, Kansas City, MO — CHIME/AHA Transformational Leadership Award
- Frank Fear, VP/CIO, Memorial Healthcare, Owosso, MI and Iatric Systems – Collaboration Award
- Intermountain Healthcare and VMware – Collaboration Award
Researchers find that less than half of the dermatologists listed in the Medicare Advantage provider rosters of insurance companies are actually available. Forty-six percent of doctors were listed twice, 18 percent weren’t reachable, 9 percent were dead or retired, and 9 percent weren’t accepting new patients. The average wait for a new patient appointment was 46 days.
More on Epic’s newly built hosting data center: it was started a couple of years ago, but wasn’t announced until the recent UGM. It’s online now and being used to host client build copies. Live client hosting will start next fall. A hosted Epic option is not good news for Cerner since that’s a big differentiator for them.
A former patient registration specialist at Parkland Memorial Hospital (TX) will plead guilty to Medicare and Medicaid fraud, accused of using insurance information from the hospital’s computer system to bill the government for services he claimed to have performed for 3,000 patients in his home health business. He also bribed patients with cash, food, and gift cards to perpetuate his scam . His wife and business partner, a Baylor nurse, was accused of looking up patient information from the hospital and falsifying clinical documentation.
Interesting: the cash-strapped, currency-controlling socialist government of Venezuela implements food rationing, requiring grocery store customers to verify their ID via fingerprint biometrics to limit black market resale in neighboring countries. The government does the same at gas stations, scanning windshield bar code stickers to prevent people from filling up on $0.01 per gallon, government-subsidized gasoline and driving next door to Colombia to resell it for $4.50 per gallon. The country finished worse than the US in WHO’s ranking of healthcare systems, coming in at #54 vs. our #37 (even Cuba finished #39).
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.















IANAL, but I don’t see how Epic could claim any damages in that lawsuit, at most the guy violated their UserWeb TOS. They do mention trade secrets, though, and I would love to hear Epic’s description of how information available to tens of thousands of customers are considered trade secrets.
RE: The country (Venezuela) finished worse than the US in WHO’s ranking of healthcare systems, coming in at #54 vs. our #37 (even Cuba finished #39).
Do not forget to congratulation Slovenia #38 for ranking between the US. and Cuba. Slovenia??? They are members of IHTSDO.
These ranking of WHO health systems have been around since 2000 and there was no
WHO update in 2010. Perhaps the U.S. would slip even further down the rankings if the decade update of the WHO ranking were to take place. Remember there are eight attributes that compile the final ranking but at least the U.S. had been number #1 in Total Expenditure on Health as % of GDP 2000-2005
in the approx.190 countries of the WHO. Good old Marshall Islands beat out the U.S. as of recent ranking for Total Expenditures.
Just saying…
I doubt Epic is trying to win damages.I’m sure this is a warning to say, we’re watching you and be prepared for more lawsuits in the future if your product starts to look anything like ours.
Remember, they didn’t find it themselves. Someone warned them about what Tata was up to, so clearly there is some kind of intent here.
“Shared his credentials with two other Tata employees” I’m only surprised that businesses are considered plausible after that.
Wow, the US is 38th in the WHO ranking of healthcare systems! I wonder what country a WHO staff member would want to go for healthcare if they had a sick child?
why not limit any user’s ability to download extremely large volumes of documents? seems like a failure to secure confidential info or analyze use patterns, which is so easy these days. either lack of focus on security or incompetence…
Hey b, I support of DOING simple things to act minimally competent. So nobody asking: “If breaches are only discovered after someone squeals, how can an organization possibly qualify issues that nobody’s squealing about?” strikes me as less than minimally viable. Still, I’m a noob pedestrian as I can count decades of experience on one hand, while epic and tata “Folks” seem to firmly grasp how to do things royally.