HIStalk Interviews Bryan Hinch, MD, CMIO, University of Toledo Medical Center
Bryan Hinch, MD is assistant professor of medicine and CMIO of University of Toledo Medical Center of Toledo, OH.

Tell me about yourself and your job.
I work clinically in internal medicine. I’m assistant professor of internal medicine and chief medical information officer at the University of Toledo Medical Center, as well as an associate program director for the internal medical residency. I wear a few hats.
On the CMIO tech side, I help coordinate, oversee, and am one of the decision-makers on the inpatient and outpatient EMR front. Most of my time is spent optimizing clinical activity or implementing new products.
I also help guide a skunk works that we’ve developed in house. We have a group of programmers that develop custom applications that fill niches that the bigger systems don’t fill. We’ve developed a number of applications that meet our unique needs. I help give them guidance and oversee what they’re doing and whatnot. That’s been my role lately.
I started here in 2008. I did my medical school training here. I did my residency here. I left for six years, four of which was in Dearborn, Michigan at Oakwood Hospital – a good place to work — my wife was doing her residency there in orthopedics.We went to Cleveland for a while and I worked at Metro Hospital. Then I came back because my wife’s family is from here and joined a group.
When I started, I was hired in in part to help them implement an outpatient EMR, which was Horizon Ambulatory Care, the McKesson system. From there, my responsibilities grew and I took over some of the inpatient stuff. They really didn’t have anybody like me on staff, so I started doing the CMIO position without the formal title. Eventually they formalized it with the title.
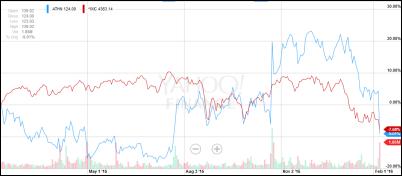
What is the medical center doing in the recently announced development project with Athenahealth?
We’re really excited about this. We were primarily — and still are — a McKesson shop, more or less. Horizon, McKesson’s systems, permeate everywhere. There was some dissatisfaction with the outpatient product. The practice plan decided a couple of years ago to begin looking at a replacement. Athena won that contract.
From the clinical side, at least, we’ve been really happy. In terms of the clinical workflows, the number of complaints that I used to get with the McKesson system was enormous. Every day I’d get complaints from the docs about workflows or whatever. It’s a bit of an exaggeration, but not much.
With Athena, I had conversations with people about that. Are people just not happy with me and they’re not complaining to me any more, or are they happy with the EMR? It seems like they’re happy with the EMR and they’re complaining about other stuff now. They’re not complaining about IT on the outpatient side.
It’s been a relatively smooth transition. We’ve been live on Athena outpatient for just over a year. We went live on January 21. We basically swapped out the entire system, big bang in one day. It was about a five-month project. After contract signing, it took us about five months, which is a bit truncated, and it was a holiday. There was a ton of work in a short period of time, but we got it done.
It was relatively smooth. It was rough at first, but like any of these projects go, it was relatively successful.
There were some rumors going around with McKesson Horizon, but they made it very formal. Right as we were making this transition to Athena on the outpatient side, they told us that Horizon is going to be going away. They gave us a deadline of March 2018.
When we were reviewing our options, looking at budgets, timelines, Meaningful Use, and all of that stuff, we felt that we were somewhat going to be stuck with Paragon. McKesson was going to give us a deal that we were going to swap out what we currently own. There’s going to be a lot of cost reductions there because of swapping one-for-one for some of the stuff that we own. But Athena came along, and when we were doing our go-live on the outpatient side, they approached us with this idea of this partnership to help them work on the inpatient space.
We were relatively impressed with their vision, the corporate culture that they have, and what they’re trying to do with healthcare in general in terms of technology. We took this pretty seriously. We spent quite a bit of time reviewing our options and what it really meant to do an alpha. We understand it’s a ton of work.
We ultimately decided that they have proven themselves in the outpatient arena of building a really good product. The KLAS rankings is one metric that shows that. Our internal satisfaction with the clinical workflows was another.
We had a kickoff meeting just about a week ago. I’m as impressed now as I was then with their approach. What they’re looking to do is not just build an EMR, because they’ve done that. They’ve got a product that’s in place in a couple of critical access hospitals that they’re using as a test bed. But the approach that they’re taking with us is more than that.
Yes, we’re going to have an EMR at the end, but they’re looking to use us to learn how hospitals — especially hospitals with an academic mission – work and identify what they call the hidden industry of scut work that could be automated or offloaded away from the staff, whether it’s nurses or doctors or whoever, to make them more productive.
It’s exciting. We’re really looking forward to taking this journey with them. We have some expectations of some concrete deliverables later this year, something we can show our board, “Yes, we’re making progress.” We expect to have something in place, like physician documentation or whatever. But so far, we’re pretty excited about this.
How do you draw the box around what you’re building with Athena?
A couple of things. The initial discussions with them were all about the clinical workflows. Lab would stay in place, so we’d keep McKesson. We have Horizon Lab, which I don’t think is getting sunsetted. But basically everything that’s getting sunsetted by McKesson, Athena’s made a promise to us that they’re going to swap out in some way, shape, or form.
That would be our ED system, so HEC, the nursing documentation system, HED, McKesson’s clinical portal, which is not the patient portal, but the physician workflows of looking at results and transcribed documents and that kind of stuff. That would be replaced. Physician workflows, order entry, and documentation, so HEO.
We had never implemented HEN, Horizon Expert Notes, which is the physician progress notes. We were never really satisfied with that product, so we were still paper until our skunk works built an online notes for the docs to use for progress notes if they want. That went live a couple weeks ago, but that was an internal thing. We built that thinking that’ we’ll be on Paragon, because Paragon is basically flip-the-switch two years from now. I wanted something in place for our medical students and residents to use, something electronic to give them that experience.
The pharmacy system is getting swapped out. That’s probably going to be later in 2017. Horizon Surgical Manager … we were under the impression that that would be sunsetted or at least swapped out, but McKesson is indicating that may not be the case, but we likely will swap that out, too.
Revenue cycle … we approached them and said, if you do a good job with this, what do you guys think about revenue cycle? Star, which is the McKesson product, is our current revenue ADT feed. They said, why not?
If this all goes well, we may consider using them for our registration system, which would be nice because one of the troubles we have on the outpatient side is having the two registration systems. A lot of our clinics are facility-based and registering for both the facility side and the clinic side has been a bear. Getting that down to a single registration system would be ideal. That is contingent upon things going well with the clinical side.
That’s a long list of tasks to accomplish. How many people are Athenahealth and the Medical Center putting on the project?
From our side, because most of our resources on the inpatient side right now are in optimization mode and not implementation mode because we’ve got everything in place except for upgrades, those same resources, we expect, will be used for Athena. We have a core group that we think can handle the amount of work.
From the Athena side, we don’t have specifics yet, but we expect they’re going to be all over this place with folks, learning our culture, learning how the workflows operate in an academic setting, and helping us with all this work.
A big piece, of course, is our interface team. We are in the process of evaluating how much work the interface guys are going to need to do and bulking that group up on our side, but also on their side, making sure that we’ve got a good collaborative relationship with their interface team.
People who have worked with one system often end up building a new one that looks just like the old one because that’s their world view. On the other hand, the vendor needs to have enough knowledge to build a product that can be commercialized instead of just taking what one hospital says and going to market with it. How will you balance those interests?
I’ve given that some thought, as has our CIO. Our CIO, Bill McCreary, is taking on the stewardship of ensuring that what we create is going to be marketable to more than just us. He’s helping Athena negotiate that, thread that needle, so that we get what we need, but it’s also something you could sell tomorrow to another hospital.
We’re very aware that we’re not building just a custom job for us and that the relationship really is one of collaboration. We want this to be successful, and if we’re the only customer, we know that’s not going to be a success. We want it to be successful.
The second issue that you raised is, how do you prevent yourself from rebuilding what you have? The interesting thing is a lot of what we have in the clinical portal is what we built ourselves to meet our needs. It’s not just McKesson’s stuff in front of us. It really is a lot of custom work that we’ve built. We think we’ve got knowledge of how to interface with technology and provide physicians what they need at the time they need it. We want to take that knowledge and use it with Athena.
Athena, on their side, they’re planning on bringing some folks that are experts in human interface with technology. They’ve got some in-house expertise there. They’re going to bring those folks here and talk to us and do time-motion studies. Dive into the workflows and identify what needs to be blown up and what works and should be replicated.
Have you had discussions about the underlying technology?
It’s cloud-based. They’re going to host it. I don’t know their database architecture for this. That’s going to be one of our conversations, especially once we get with the interface team and start talking about this.
In terms of mobile access, to me, it’s a given. They already have a relatively decent mobile platform on the outpatient side. Most of our custom apps that we’ve built in-house, we’ve built with mobility in mind.
For instance, we have this patient hand-off tool that we built a couple of years ago. We’ve redesigned it twice ourselves. The redesign was specifically to make sure that we could scale it to an iPhone or equivalent smart phone. This replaces the traditional paper list that resident teams keep to track their patients. We saw that there was a need there. We just deployed it to the surgery department a couple of weeks ago. But medicine — my department – has been using it for two and a half years, squashing bugs and vetting it.
Mobility is going to be a big part of this. I don’t see nurses, especially, getting tied down to a computer. That’s one of the biggest complaints I have, and docs have, and nurses have, no matter what hospital I work in. I don’t just work at UT. I do teaching rounds at another hospital that uses Epic. The biggest complaint is that they feel like they’re tied to the computer typing all day. Is there a way around that?
The other thing that we implemented, right before Athena got in place, was voice-to-text. We use Nuance Dragon. How do we leverage that kind of technology to help speed up the process of inputting data in some way, shape, or form, and doing it in a way that’s hopefully structured so you can report against it?
There’s a lot of balls in the air, you’re right. How do we coalesce this down into a streamlined, functional workflow for the doc, the nurse, the physical therapist, et cetera? That’s what we’re looking to have these conversations with Athena about.
What happens if you don’t make the 2018 sunset date for the Horizon products?
We are going to be checking our progress. I think Bill McCreary, our CIO, is using Gartner as an external oversight to make sure that we are staying on task. We’re having a third party keep us honest in terms of making sure we hit these deliverables.
Worst case scenario, we would bail and go to Paragon, but I am loath to even consider doing that because the docs here have such an animus against the McKesson products. I think I’d be burned in effigy.
To answer your question, though, absent pulling a ripcord and jumping away from this — which to me, is a nonstarter — I don’t think it’s going to happen. Knowing our culture, at UT, we just get the job done. Historically, any time we ask the staff — the physician staff, the residents, the nursing staff — to step up, whether it’s Joint Commission or the ACGME coming through or Meaningful Use, they get the job done. They have this work ethic that’s phenomenal.
I get that sense from Athena as well. When I’ve gone out to visit them and seen their folks and interact with them, they are just about getting the job done and doing it really well.
That being said, there’s a couple of possibilities. One is that if we miss the deadline, it’s not like suddenly the system is just shut down at midnight. They continue working. Our IT department has a wealth of knowledge of using these systems. McKesson has made it very clear that if this goes dark, you’re on your own. We understand that.
However, that being said, in terms of the core systems that we require to function on a day-to-day basis, I think we’ve got enough buffer in the timeline. Again, we don’t have a concrete timeline yet, but when we’re talking with Athena, we’ve got enough buffer in here that I feel pretty comfortable that we’re going to have things in place.
I think the other thing I would stress is that Athena’s not starting from scratch on this. They have acquired intellectual property through RazorInsights, their acquisition there, and with their agreement or their relationship with Beth Israel. I feel pretty good about saying this — they’ve got a pretty good bench strength on the pharmacy system and inpatient core systems that we need. I think they’ve got that knowledge, intellectual property, et cetera.
On top of that, you marry that up with our guys, like on our pharmacy team. Many of our custom apps are for the pharmacy and they’ve built them themselves. We’ve got guys in my pharmacy team who are both pharmacists and IT and they build apps. We feel pretty comfortable that whatever Athena can’t deliver on, we will probably be able to, in some way, shape, or form, take care of.
That’s a risk. This is the risk of the relationship. Going down this path with someone who has something that’s on the market. They’re in some critical access hospitals, they’ve deployed in a few places, but nothing like us. Nothing with the complexity of a larger hospital and the complexity of academics.
We understood that risk going into this. We made it very clear to the board and to all the decision makers that the risk of going with another vendor is that you probably are going to have a lower-quality product for the capital expenditures and whatnot that we have available to us, versus going into a partnership with Athena. The risk is a little bit higher because there is a product that’s not basically on the market right now, but the expectation is that we’re going to have something truly awesome. We felt that that reward was worth the risk.
We didn’t feel staying with McKesson was a safe choice, either. We really didn’t. They’re a good company and the folks we work with individually are wonderful, but we felt like in terms of the product we would get, we feel with Athena it’s going to be better.
That being said, our Plan B is to go back to McKesson, if this blows up in our face, and see what they can do. We’ll see, but I don’t think that’s going to happen.
Isn’t the medical school’s academic affiliation moving to ProMedica?
That is correct. The medical school is basically a victim of its own success. It has grown tremendously and is outgrowing the footprint of the hospital here. Same with the residency. We’ve grown the residency here as well.
We are busting at the seams with learners. As many medical schools do, they look outside and they look for some affiliations. We will be transitioning learners from this campus to the ProMedica campus. Yes, that is true.
Will you still be an academic medical center and the kind of partner Athenahealth originally envisioned?
That’s a good question. I don’t think all the learners are going to go. I think there’s still going to be learners here. This transition is a five-year plan in terms of transitioning the bulk of the learners over, at least the students, and some of the residents over.
To be honest with you, we had a pretty frank conversation with Athena about this. We tried to be as transparent as possible about this process. From my point of view, if you look at what they’re trying to get out of us, which is institutional knowledge of academics, that’s not going anywhere. I’m part of this process. The staff here all know how to work with residents. When you look at the timelines involved, the bulk of the work is done well before the significant number of learners will be over at ProMedica.
I think they’re going to get what they need out of us in terms of that knowledge and ongoing expertise. We were very upfront and transparent with Athena about that. They felt pretty comfortable understanding that things are changing here, too, in terms of that affiliation, but they still felt really comfortable going forward with us.














































































































Re: Deliberately Faked Academic Papers in Nature See, this doesn't surprise me at all. Of course AI quotes these bogus…