Download and print a PDF version of this guide.
Access

Booth 4761
Contact: Lindsey Keith, sales and marketing operations manager
lindsey.keith@accessefm.com
913.752.9938
One place. One view. ALL of your forms. Access develops electronic forms management solutions that clear your paper path—eliminating the expense, risk, and inefficiency of paper forms. Our software, including Web-based Access Passport and Formatta, enables organizations to capture, manage, sign, and share e-forms data with other systems without paper, printers or scanners. Staff can interact with paperless e-forms anywhere, anytime using any device. By integrating e-forms, e-signatures, and clinical data into EHRs and other healthcare or business applications, you can improve care, remove the impact of paper, and enhance patient safety, compliance, and downtime planning initiatives. Everything related to forms is in one place with Access — so reduced costs, paper-free routines, and complete EHRs can be real-world destinations. And, if you’re feeling worn out from all those educational sessions, stop by our booth (4761) for a free latte, Americano or whatever you need to keep you going for the rest of the show.
AdvancedMD

To schedule a meeting:
Contact: Aaron Glauser, director, product marketing
aglauser@advancedmd.com
801.984.9500
Since 1999, AdvancedMD has helped private practices improve clinical outcomes, patient experience, staff productivity, and financial performance. Our cloud EHR and PM suite is exclusively designed for independent physicians and includes financial analytics, peer-to-peer benchmarking, patient engagement, and telemedicine. Control your destiny. advancedmd.com
The Advisory Board Co.

To schedule a meeting:
Contact: Jordan English, senior director, strategic marketing
EnglishJ@advisory.com
202.266.6237
Please come to our HIMSS16 presentations: Closing Keynote for the Nursing Informatics Symposium: Shifting from Implementation to Optimization: “Looking Towards the Future; Imagine the Possibilities” with Edward Marx (Monday at 3:15 pm in Marcello 4404) – Innovation Symposium opening presentation: “The Rise of Intelligent Machines in Health Care” with Ken Kleinberg (Monday at 8:15 am in Galileo 901) – “PQRS and Alignment Opportunity – Concept to Operationalization” with Tony Panjamapirom (Tuesday at 2:30 pm in Palazzo D) – “The Rise of Intelligent Machines in Health Care” with Ken Kleinberg (Wednesday at 4:00 pm in Galileo 1004) – “Planting Seeds: Developing a Mature Health IT Team” with Ernie Hood (Friday at 10:30 am in Marcello 4401). The Advisory Board Company is the leading provider of insight-driven analytics, research, and services for healthcare organizations. Through its innovative membership model, the Company collaborates with more than 230,000 leaders at 5,200 member organizations to elevate performance and solve their most pressing problems. The Company provides strategic guidance, actionable insights, cloud-based software solutions, and comprehensive implementation and management services. For more information, visit www.advisory.com.
AirStrip

Booth 6642
Contact: Chris Lato, director, marketing communications
chrislato@airstrip.com
210.805.0444
Experience how the AirStrip ONE mobile interoperability platform transforms care coordination and drives health system innovation. AirStrip ONE lets you achieve true interoperability. Mobilize your existing technologies to give caregivers the insights they need to provide patient-centered care — anytime, anywhere. Enter our daily social media drawing to win: Bose SoundLink On-Ear Headphones and a GoPro Hero4 Session Camera Apple TV 4 (32 GB).
Aprima Medical Software

Booth 7314
Contact: Judy Friedman, marketing and events
jfriedman@aprima.com
844.4APRIMA
A single application, built on a single database, the Aprima EHR and PM systems are fully integrated. That’s why our software continues to be one of the fastest products for doing complete visit documentation in real time. Stop by booth 7314 at HIMSS to take our Stopwatch Challenge and compare Aprima to ANY EHR! When you take the Stopwatch Challenge, we’ll give you a stopwatch so you can do your own comparison. Thousands of providers have left their old EHR and made the move to Aprima. When you work in the ever-changing world of healthcare, your medical practice needs systems that are agile and responsive. That’s why over the last 10 years more than 95 percent of our customers have stayed with us, and why thousands of providers have recently made the switch to Aprima. Aprima is one of the few companies with a 18-year track record of success. To learn more about Aprima, visit us at HIMSS in booth 7314 or visit www.aprima.com.
Arcadia Healthcare Solutions

Booth 4612
Contact: Greg Chittim, vice president, strategic marketing
greg.chittim@arcadiasolutions.com
603.496.1242
Think aggregating high-quality data from many different EHRs is impossible? Come see how we’ve been doing it for a decade. Come to booth #4612 (near the main entrance behind McKesson) to receive: HIStalk’s "best giveaway of HIMSS15" – a conference survival kit and a bottle of water; a look at our "Data Gallery" – an art gallery of visualizations from our provider benchmark database; a demo of our platform recently rated by Chilmark as the best "User-centered Design" among Analytics platforms for Population Health Management; and a raffle for fantastic prizes. Arcadia Healthcare Solutions (http://www.arcadiasolutions.com) is an EHR data aggregation and analytics technology company delivering managed care to ambulatory networks taking on value-based risk. Arcadia specializes in the integration of data from 30+ EHR platforms, enriching them with claims and operational data, and using that data to drive improvements in patient care quality, practice efficiency, and financial performance. Trusted by independent provider groups, health plans, and integrated delivery networks nationwide, with expertise in both fee-for-service optimization and value-based performance environments, Arcadia supports providers with the benchmark data, insights, and outsourced services to excel in the evolving landscape of American healthcare. Founded in 2002, Arcadia is headquartered outside Boston in Burlington, MA, with offices in Seattle and outside Chicago in Rockford, IL.
Aventura

Booth 1324
Contact: Jennifer Haas, vice president, marketing
jennifer.haas@aventurahq.com
978.697.3921
With Aventura, security and clinical efficiency doesn’t have to be black or white. Aventura’s Sympatica platform leverages situational awareness to deliver a highly secure, personalized clinical desktop. With security, personalized desktop and interoperability functionality, Sympatica is a flexible, modular offering that fits every operational need and budget. Choose from three levels of functionality to solve a specific issue or leverage all three for a complete, integrated clinical desktop solution. Stop by booth 1324 for a demo and pick up a copy of our Iris & Friends coloring book.
Besler Consulting

To schedule a meeting:
Contact: Jim Hoffman, COO
jhoffman@besler.com
732.233.5008
Billian’s HealthData

Booth 1459
Contact: Ben Mauldin, national sales manager
bmauldin@billian.com
678.282.1029
Billian’s HealthData offers unparalleled business intelligence on 875,000 US healthcare providing organizations, including 2M+ healthcare executive contacts. Insight into breaking hospital news, RFPs, emails, financials, HIT utilization, CRM integration, and more offer you an unprecedented amount of data you can use to reduce prospect and market research burdens, identify best-fit partners, and initiate relevant correspondence. Search profiles at https://billianshealthdata.com or visit booth 1459 for a data demo.
Boston Software Systems

To schedule a meeting:
Contact: Nick Topping, marketing program manager
nick.topping@bossoft.com
913.839.9527
Boston Software Systems revolutionizes how healthcare works by providing error-free automation for any application, enabling successful EHR migration, streamlined business processes, and improved productivity. Our Active Data Quality (ADQ) platforms are the most sophisticated automation platforms available, giving customers’ peace of mind that critical data is 100-percent error free. We have the best reputation for ease of use and customer support, helping organizations bridge the gap between technologies to help provide optimal patient care. Hospitals and healthcare vendors worldwide respond to regulatory and business initiatives by using technologies from Boston Software Systems to automate and improve processes throughout a variety healthcare organizations and departments. For more information, please visit the company’s website at www.bostonsoftwaresystems.com or call 866.653.5105.
Bottomline Technologies

Booth 5046
Contact: Heather Barr, marketing manager
hbarr@bottomline.com
603.501.6654
Bottomline Technologies powers mission-critical business transactions. Our privacy and data security solution for healthcare protects healthcare information, prevents fraud, and helps customers with their compliance of the HIPAA and HITECH mandates. Our healthcare solutions improve patient and clinician satisfaction while reducing costs with digital forms management, discrete data capture, and eSignature across platforms and devices. Based on our deep market knowledge combined with development and business expertise, we constantly set, anticipate, and respond to changing industry and organizational demands. http://www.bottomline.com/us/healthcare
Caradigm

Booth 5427
Caradigm is an award-winning population health company dedicated to improving patient care, advancing the health of populations, and reducing healthcare costs. Its enterprise software portfolio encompasses all capabilities critical to delivering effective population health management, including data control, healthcare analytics, care coordination and management, and wellness and patient engagement. See a live demo by visiting us in booth 5427 at HIMSS16 or learn more at www.Caradigm.com.
CareSync

Booth 147
Contact: Courtney Larned, vice president of marketing and corporate communications
courtney@caresync.com
727.366.5389
CareSync is the leading patient-centered engagement solution that combines technology with 24/7 nursing services to facilitate care coordination among patients, family and caregivers, and all providers. CareSync provides turnkey chronic care management services and a software-only option, allowing practices of any size to easily meet the billing requirements for CPT code 99490. CareSync patients are at the center of their healthcare, with access to health information, actionable goals, and comprehensive care plan tasks, and as a result, are experiencing more productive medical appointments and better health outcomes.
Catalyze

To schedule a meeting:
Contact: Kevin Lindbergh, vice president, sales
kevin@catalyze.io
612.202.7087
CenterX

Booth 3073
Contact: Christopher Marshall, president
christopher@centerx.com
855.CenterX
CenterX is a is a comprehensive e-prescribing network that helps your physicians spend more time with their patients and less time completing prior authorizations. The CenterX ePA solution will execute all PA types electronically – pharmacy, medical, and specialty – decreasing PA turn-around time by 90 percent. Save time by identifying, capturing, and automating the PA process in your EHR – before the patient leaves the office. Giveaway: Stop by booth 3073 to learn how CenterX can help you save time and grab a free swag bag, pen and notepad.
The Chartis Group

To schedule a meeting:
Contact: Daniel Herman, director and informatics and technology practice leader
dherman@chartis.com
412.370.4900
The Chartis Group is a national advisory services firm dedicated to the healthcare industry. We provide strategic and economic planning, accountable care, clinical transformation, and informatics and technology consulting services to the country’s leading healthcare providers. Our firm is comprised of experienced healthcare professionals who apply a distinctive knowledge of healthcare economics, markets, clinical models, and information technology to help clients achieve demonstrative outcomes. Chartis has been privileged to work with leading healthcare organizations across the world. Our collective experience across many organizations provides us a deep knowledge base, client network, and perspective on what it takes to make meaningful and sustainable change. Over the past decade, we have worked with leading healthcare organizations across the country and throughout the world including over two-thirds of the academic medical centers on the US News & World Report “Honor Roll of Best Hospitals,” seven of the 10 largest integrated healthcare systems, four of the five largest not-for-profit health systems, nine of the top 10 children’s hospitals, emerging and leading ACOs, hundreds of community-based health systems, and leading organizations in healthcare services.
Clinical Architecture

Booth 721
Contact: Mark DuBois, executive vice president of sales
marck_dubois@clinicalarchitecture.com
317.853.1080
We develop software focused on the quality and usability of clinical information. Our solutions address industry gaps in content acquisition, terminology management, interoperability, decision support, and analytics. Each day we will donate $500 to the charity of the winner’s choice. Stop by our booth (#721) to enter.
CoverMyMeds

Booth 754
Contact: Alison Bechtel, marketing manager, EHR solutions
abechtel@covermymeds.com
614.581.1803
More than 500,000 providers choose CoverMyMeds, the nation’s largest electronic prior authorization platform. CoverMyMeds is integrated with over 360 EHR systems including Epic, Cerner, and Allscripts. Providers submit requests for medications in workflow at the point of prescribing for the fastest, most efficient way to complete prior authorizations. Check your integration status at http://www.covermymeds.com/epa/healthsystems CoverMyMeds is located in booth 754 in the main exhibit hall. Stop by and mention "HISTalk" to be entered to win a $100 VISA gift card.
Craneware

To schedule a meeting:
Contact: Rick Weissinger, vice president, marketing communications
r.weissinger@craneware.com
404.617.6794
Craneware executives will be at HIMSS to speak about the value cycle, an exciting new strategy for achieving quality patient outcomes and optimal financial performance and how Craneware is building their solutions for a value cycle future. Attendees can expect to learn more about the switch from revenue cycle to value cycle, and how this will impact the healthcare IT community.
CTG

Booth 5255
Contact: Amanda LeBlanc, vice president and CMO
amanda.leblanc@ctg.com
800.992.5350
We’re Computer Task Group (CTG), the most reliable IT services provider – built on 50 years of meeting our commitments to make technology work for you and deliver real business value. Our customers come to us from industries worldwide including healthcare and life sciences, energy, financial services, government, technology, and telecommunications. Visit us at booth #5255 to join the celebration! CHEERS T0 50 YEARS. Toast innovations in healthcare and CTG’s success over the past half century with our CEO and team members.
Cumberland Consulting Group

To schedule a meeting:
Contact: Dave Vreeland, managing partner
david.vreeland@cumberlandcg.com
615.335.5272
Founded in 2004, Cumberland Consulting Group is a leading full-service strategic advisory, performance improvement, information technology implementation, and support services firm. Cumberland provides technology implementation and project management support to help its clients advance the quality of services they deliver and to improve their overall business performance. Our experienced consultants deliver results for clients through technology optimization and process improvement. Need help with IT planning? Integration? Upgrades? Optimization? RCM? If so, we can help. For more information on Cumberland, please visit www.cumberlandcg.com.
DataMotion

Booth 12144
Contact: Bud Walder, vice president, marketing
Budw@datamotion.com
973.455.1245 x512
DataMotionHealth at HiMSS16: Sharing information is at the heart of healthcare reforms and initiatives! At HIMSS16, DataMotion Health will showcase the latest in secure health information delivery services and solutions. Learn about empowering your team to share information for care coordination, patient engagement, population health, and more. Stop by Booth #12144! Or if you prefer, contact us at www.datamotionhealth.com to schedule some time for a meeting at our booth or hospitality suite at the Venetian.
Direct Consulting Associates

To schedule a meeting:
Contact: Frank Myeroff, president
fmyeroff@dc-associates.com
440.996.0051
Direct Consulting Associates provides a broad range of healthcare IT consulting and staffing solutions including staff augmentation, temp-to-perm, and direct hire. Healthcare organizations trust us to acquire the best IT talent in the industry in order to meet their IT initiatives.
Divurgent

Booth 11612
Contact: Keri DeSalvo, marketing director
keri.desalvo@divurgent.com
757.213.6875
Back by popular demand … Divurgent will host a fast-paced, fun-filled interactive High Roller Charity Drive to raise $5,000 for the Children’s Hospital of Nevada at UMC. HIMSS attendees are encouraged to stop by booth #11612 and toss the bright red, oversized inflatable dice high into the air – whatever number the dice lands on, will determine the donation value that Divurgent will contribute on the attendee’s behalf!
Divurgent will also be announcing some very exciting, industry-breaking news during the HIMSS conference centered around our cybersecurity, MACRA/MU, and revenue cycle optimization strategies … stay tuned!
Divurgent is a nationally recognized healthcare IT consulting firm, specializing in cybersecurity and privacy solutions, population health management, clinical documentation improvement, and activation management and implementation. Visit booth #11612 to learn how Divurgent can help improve your operational effectiveness, financial performance, and quality of patient care. To view all of Divurgent’s exciting events and happenings during HIMSS, click here.
DrFirst

Booth 943
Contact: Ellie Whims, director, marketing communications
ewhims@drfirst.com
301.231.9510 x2808
DrFirst (www.drfirst.com) pioneers healthcare technology solutions that inform the doctor-patient point of encounter, optimize provider access to patient information, enhance the doctor’s clinical view of the patient, and improve care delivery and clinical outcomes. Our growth is driven by a commitment to innovation, security, and reliability across a wide array of e-medication management and secure communication and collaboration services. We are proud of our track record of service to over 335 EMR/EHR/HIS partners and an extensive network of hospitals, post-acute care facilities, ambulatory practices, and pharmacies nationwide. Come by the DrFirst booth on Tuesday, March 1st at 5 PM for a special reception, and world premiere of a new ZDogg Video!
ECG Management Consultants

To schedule a meeting:
Contact: Michelle Holmes, principal
mholmes@ecgmc.com
206.689.2231
ECG is a strategic consulting firm that is leading healthcare forward, using the knowledge and expertise built over the course of more than four decades to help clients see clearly where healthcare is going and to navigate toward success. We work as trusted, professional partners with medical groups, hospitals, health systems, and academic medical centers across the country. With deep expertise in technology, strategy, finance, and operations, ECG builds multidisciplinary teams to meet the unique needs of every client. We’re proud to partner with providers across the country to better leverage technology and achieve their goals. For more information, visit www.ecgmc.com.
Elsevier

Booth 3039
Contact: Yazmin Zayas, senior manager, events/exhibits
y.zayas@elsevier.com
215.239.3490
Encourage Quality. Enhance Efficiency. Improve Outcomes. Consistent, high-quality patient care requires evidence-based content incorporated into the care process. Elsevier provides more than 25 percent of the world’s clinical content and serves more than 20 million healthcare professionals. Integrated into clinical workflows and EHRs, this content empowers healthcare professionals and their patients to make better decisions at every stage of the patient journey. Reference and Decision Support • Order Sets and Care Plans • Learning and Competency Management • Patient Engagement • Professional Practice Services • Academic Education and Certification. When you visit our exhibit, be sure to step inside our Rewarding Knowledge prize booth for a daily chance to win a FitBit, Beats by Dr. Dre, or a $100 VISA gift card. It’s the one place in Vegas where the odds are in your favor. Empowering Knowledge. Enabling Action.
E-MDs

Booth 5222
Contact: Allison Jones, director, marketing
ajones@e-mds.com
512.257.5200
E-MDs is a leading provider of integrated EHRs, PM software, revenue cycle services, and credentialing solutions for physician practices and enterprises. Founded by physicians, the company is an industry leader for usable, connected software that enables physician productivity and a superior clinical experience. E-MDs software has received top rankings in physician and industry surveys including those conducted by the AAFP’s Family Practice Management, AmericanEHR Partners, MedScape, and Black Book. E-MDs has a proven track record of positioning clients for success as demonstrated by Meaningful Use attainment in 2011, 2012, 2013, and 2014. According to data provided by CMS, E-MDs clients are attesting in the top proportion of all major vendors. For more information, please visit http://www.e-mds.com.
Etransmedia Technology

Booth 1469
Contact: Connie Smith
connie.smith@etransmedia.com
518.283.5418
Etransmedia helps improve revenues and clinical outcomes, enabling physicians to focus on patient care. Etransmedia is a leading healthcare information technology company delivering integrated software, service, and connectivity solutions to simplify critical functions for healthcare providers. Our clients include some of the country’s leading healthcare systems and hospitals, as well as affiliated physician practices. Eight consecutive years, Inc 5000 and four consecutive years, Deloitte Technology Fast 500.
Extension Healthcare

Booth 1261 and Intelligent Hospital Pavilion Booth 11655-17
Contact: Jenny Kakasuleff, social media PR manager
jkakasuleff@extensionhealthcare.com
317.345.4176
Learn what Extension Healthcare has done for Kaiser Permanente, St. Joe’s, University of Maryland Medical Center, Parkland, and 200 more customers at HIMSS16 booth 1261. Our team at HIMSS will be demonstrating our award-winning, event-driven care team communication workflows, including our real-time waveform integration, and can answer any questions about new features, functionality, and enhancements to Extension Engage Mobile. On Wednesday, March 2, at 11:30 am, NYU Langone Medical Center, an Extension Engage customer, will present the details of their deployment in the Intelligent Hospital Pavilion. Visitors to either Extension booth will be entered into a drawing for an Apple Watch upon completing a survey.
FormFast

Booth 4849
Contact: Aaron Vaught, director, marketing
avaught@formfast.com
314.603.9674
FormFast’s enterprise software platform automates documents and workflow, capturing data and streamlining processes. With more than 20 years exclusively focused on healthcare needs and over 1,000 healthcare clients, FormFast is considered the #1 in eForms for hospitals, according to HIMSS Analytics. At booth #4849, FormFast will give HIMSS16 attendees a test-drive of their automation offerings, which include solutions for registration, mobile bedside consents, electronic signature capture, human resources, clinical documentation, and more. Learn more at: www.formfast.com and follow us on Twitter @FormFast. Booth Promotions: Register to win the Ultimate Supercar Driving Experience! Visit FormFast at booth #4849 to register! Includes: -Exotic Supercar Test Drive on Course – Round Trip Airfare for 2 -3 Day/2 Night Deluxe Hotel Stay -$250 Gift Card. FormFast will also have a premiere, luxury car on display at booth #4849 for attendees to check out and to capture an amazing photo opportunity!
Forward Health Group

Booth 2477
Contact: Barry Wightman, director of marketing
bmw@forwardhealthgroup.com
608.729.7522
Forward Health Group to unBooth at HIMSS16! A visual extravaganza is rolling into booth #2477. FHG, a leader in value-based population health management solutions, zigs when everyone else zags. The fast-growing company will feature prodigious, on-the-fly artistic talents, generating marvelously whimsical graphic population health management collaborations with HIMSS visitors. Producing giant, eight-foot hand-drawn murals each day, recording booth visitors’ visions of their value-based population health futures. FHG will also provide demonstrations of five new PopulationManager products – including innovative pre-packaged FastStart PopulationManager solutions for chronic care, acute episodes, behavioral health, bundled payments, and national standards reporting. Fresh oranges, too. A splendid time is guaranteed for all! Don’t miss the unBooth #2477.
Galen Healthcare Solutions

Booth 3273
Contact: Justin Campbell, vice president
justin.campbell@galenhealthcare.com
617.379.0841
Galen Healthcare Solutions is an award-winning, #1 in KLAS, healthcare IT technical and professional services and solutions company providing high-skilled, cross-platform expertise. Galen Healthcare Solutions was one of the few vendors to receive multiple 2015/2016 Best in KLAS awards, winning #1 in Technical Services and #1 in HIT Implementation Support & Staffing. For over a decade, Galen has partnered with more than 300 specialty practices, hospitals, HIEs, health systems, and integrated delivery networks to provide high-quality, expert-level IT consulting services including strategy, optimization, data conversion, archival, project management, and interoperability. Galen also delivers a suite of fully integrated products that enhance, automate, and simplify the access and use of clinical patient data within those systems to improve cost-efficiency and quality outcomes. We will be giving away three Apple Watches. HIMSS attendees can enter the contest by scheduling a time to meet during HIMSS: www.galenhealthcare.com/HIMSS16/
GE Healthcare

Booth 3055
Contact: Chris Bowler, general manager, Americas region marketing
christopher.bowler@ge.com
860.747.7123
Visit GE Healthcare at booth 3055 to learn how actionable insights can help you improve clinical, financial, and operational outcomes. With over 20 demo stations showcasing solutions for financial management, workforce management, enterprise imaging, and care delivery management, you’ll see first-hand how our software, services, and partners can help spark your success. And don’t miss the chance to talk to our experts and see live presentations featuring our newest solutions: GE Health Cloud – a scalable, secure, connected cloud ecosystem that will enable you to manage data as you need it; and Analytic Applications – an advanced analytics platform and consulting service that helps healthcare organizations quickly generate actionable insights that drive better outcomes.
The HCI Group

Booth 6832
Contact: Chris Parry, marketing director
chris.parry@thehcigroup.com
904.239.4670
The HCI Group is recognized as a world leader in healthcare IT consulting. Our services include implementation and training of all EHR vendors as well as service lines in optimization, clinical adoption, integration and testing, go-live, and advisory services, among others. From Johns Hopkins and Tenet Health to, Canada, Europe, Asia and beyond, we’ve developed a track record of proven excellence in developing smarter approaches to solving healthcare IT challenges.
Healthcare Growth Partners

Booth 10650
Contact: Christopher McCord, managing director
chris@hgp.com
312.445.8750
Healthcare Growth Partners is an investment and merchant bank focused exclusively on health IT, digital health, and health information services. Since its founding in 2005, HGP has closed over $2 billion across over 80 health informatics and digital health transactions. Services include M&A advisory, capital raising, and strategy, as well as principal investments through HGP Capital. Through our advisory relationships and investments, HGP aims to unlock health IT’s great potential in solving fundamental challenges in the management and sustainability of health.
Health Catalyst

Booth 3069
Contact: Patty Burke, program manager
Come by booth #3069 and read any one of our 50 client success stories on display in and around our booth.
Health Data Specialists

Booth 8402
Contact: Steve Grenier, vice president
sgreiner@hds-llc.com
805.233.0616
Health Data Specialists (HDS) is a privately held, healthcare information services company that has been providing quality consulting services to healthcare organizations nationwide since 2003. Our mission is to provide exceptional consulting services, valued specialists, and trusted advisers to facilitate the IT business strategies of our clients. We focus on assisting healthcare organizations in meeting their IT goals in a cost-effective, efficient manner. HDS is committed to bringing value and proven solutions to our clients’ information technology initiatives. HDS has assisted facilities of all sizes – from large teaching facilities to multi-entity IDNs to regional healthcare centers. We offer a full range of staff augmentation, optimization, and consultative services with expertise in software solutions for Epic, Cerner/Siemens, and Meditech. We provide expertise in Meaningful Use, mock audit services, revenue cycle and ICD-10 support. We value our intangibles, such as our ability to relate to clients regarding their needs, management style, corporate culture, commitment, and confidentiality. These elements differentiate us from other consulting firms and give us a sustainable competitive advantage while strengthening our long-term relationships with our clients.
Healthfinch

Booth 10828
Contact: Karen Hitchcock, vice president, marketing
karen@healthfinch.com
608.513.6566
Healthfinch’s practice automation platform, Charlie, leverages EHR data to automate, delegate, and simplify routine, repeatable tasks, like prescription refill requests, visit planning and diagnostics results management. Our flagship application, Swoop for prescription refill requests, is used by major health systems to improve workflows and get providers working top-of-license by reducing their inbox volume. Healthcare leaders who want to improve efficiencies, workflows, and maximize their investment in their EHR should stop by booth 10828 to learn how "Charlie" can help.
Healthwise

Booth 3617
Contact: Dave Mink, market solutions director
mink@healthwise.org
208.921.4918
Stop by Healthwise booth 3617 and check out our demo stations to discover how to effectively engage your health populations. Healthwise solutions for episodic care, care coordination, automated programs, and patient portals will deepen the impact of your patient touchpoints. Visit our kiosk in the Population Health Knowledge Center and learn how the right population health strategy can broaden the reach of your care team without adding resources.
Iatric Systems

Booth 7730
Contact: John Danahey, executive vice president
John.Danahey@iatric.com
978.805.4153
We invite you come by the Iatric Systems booth #7730 in the Venetian Ballroom to see how we can help you enhance your existing healthcare technology investments. Your challenges around analytics, EHR optimization, interoperability, and patient privacy are serious. We look forward to a great conversation around how our diverse healthcare experience, extensive partner network and advisory/consulting services are the foundation for solutions that enhance your healthcare technology investments. It’s serious business, but you won’t want to miss The Magic Castle performer and professional magician Chef Anton’s entertaining and amazing magic tricks – and be entered to win not just one, but TWO Apple Watches. www.iatric.com/HIMSS16
IMO

Booth 4221
Contact: Dennis Carson, director, marketing and tradeshows
dcarson@e-imo.com
847.728.4997
IMO provides the most widely-used and physician preferred medical terminology solutions for EHRs. Visit us at booth 4221 to see the latest innovations around IMO Problem IT Terminology and IMO Procedure IT Terminology. New at HIMSS16: IMO Anywhere – the mobile-enabled solution that lets users access IMO Terminology anytime, anywhere, on any device. IMO 2.0 Enhanced Terminology Platform (ETP) – a new, feature-packed platform that keeps dictionaries updated long into the future. IMO Problem IT Plus – now with our unique intelligent Problem List to give users a clear, concise, and organized view of their patient Problem Lists. IMO SurgIT – the new service that provides highly accurate IMO codes for surgical procedures. Come learn about “The IMO Way” to capture and preserve true clinical intent because The Patient Story is too important to lose. At the vendor solutions sessions, don’t miss “How Capturing True Clinical Intent Improves Patient Care” Tuesday, March 1 at 2.30 pm in Galileo 1001 at the Sands Expo Convention Center. Cool giveaways include T-shirts, flashlights, and more!
Influence Health

Booth 6232
Contact: Anna Powell, vice president, marketing
anna.powell@influencehealth.com
205.982.5805
Momentum demands movement, movement demands Influence Health. Run, walk, skip or hop toward booth 6232, where a specialized team can help you explore solutions to support your population health and patient engagement efforts. Learn how we can help your organization gain the momentum you need to provide successful, value-based care and improved outcomes. Influence Health’s digital solutions are helping hospitals and health systems nationwide close the gaps in care by providing aggregated patient data and reporting quality measures and outcomes. Stop by the Influence Health booth 6232 Tuesday-Thursday at 11 am and 2 pm for a product demo and a chance to win NIKEiD custom shoes!* * Winners will be randomly selected at the end of EACH demo. Must be present to win.
InMediata

To schedule a meeting:
Contact: Nick Challen, vice president, strategic partnerships
nchallen@inmediata.com
704.998.9129
InMediata drives innovation in healthcare payments by focusing on solving complex reimbursement issues for large provider groups, hospitals, and billing services. We believe in challenging the status quo, utilizing our experience and knowledge to provide tailored solutions that address specific client and industry needs. For example, our InBanking product suite bridges the gap between banking and healthcare claim payments. By automating the payment reconciliation process, healthcare entities are able to gain greater insight into their finances and cash flow while reducing the administrative inefficiencies involved with processing payer and patient revenues. At inMediata, we’re different for a reason. Please contact us to discuss strategic partnership opportunities, and to register for our $500 drawing, which will take place on Wednesday at 5:00 pm.
InterSystems

Booth 4443
Contact: Ross Whittaker, market development manager
ross.whittaker@intersystems.com
617.621.0600
InterSystems provides the information engines that power some of the world’s most important applications. In healthcare, finance, government, and other sectors where lives and livelihoods are at stake, InterSystems has been a strategic technology provider since 1978. InterSystems is a privately held company headquartered in Cambridge, MA (USA), with offices worldwide, and its software products are used daily by millions of people in more than 100 countries. HIMSS2016 – THEME Right Connections, Right Conclusions, Right Actions – FEATURED HX360, Transforming End-of-Life Care, HIE Community Networking Breakfast The Path to Deriving Clinical Value from FHIR, The Internet of Healthy Things presentation and book signing by Joseph Kvedar, MD. SAMPLE PRESENTATION TOPICS HIE cost and care improvements – HIE support for population health – Hospital in “The Cloud” – Genomic data – Remote patient monitoring. GIVEAWAY – Conference Survival Kit. More info about InterSystems at HIMSS16 http://www.intersystems.com/himss16.
Legacy Data Access

Booth 949
Contact: John Hanggi, director, business development
jhanggi@legacydataaccess.com
678.701.5589
Running old applications just to get to the data? STOP! We need to talk … With a singular focus on the healthcare industry, Legacy Data Access provides the industry’s most comprehensive set of software tools and solutions for working with data from retired systems. Legacy Data Access stores data from systems that are being retired and provides secure, Web-based, interactive access to the information. Please visit us to discuss how we have successfully retired 192 different healthcare applications – a total of 463 applications. We will be providing “Coffee, Tea, and Legacy” Tuesday morning in our booth. Giveaways include ear buds, tote bags, and the best dark chocolate in the Exhibit Hall. Sign up for a chance to win an Apple Watch or one of two Apple TVs.
Leidos Health

Booth 3432, 9908, and 13329
Contact: Matt Maloney, director, marketing
matt.maloney@leidoshealth.com
317.908.8345
For more than 25 years, Leidos Health has been helping our clients improve care and reduce costs by leveraging information technology and best practices. As one of the largest and most experienced health IT consulting firms, and a provider of health IT services to nearly every federal agency focused on healthcare, we bring diverse perspectives and proven solutions to help you succeed. Our experts will be available to discuss the latest happenings and challenges in healthcare, and share how we’re helping organizations with solutions for implementation, optimization, interoperability, cybersecurity, federal health IT, and more. Come by our booth to register for a chance to win an Apple Watch ($350 value). We’ll be giving one away each day.
Lexmark Healthcare

Booth 6225
Contact: Katie Booth, manager, global healthcare marketing
katie.booth@lexmark.com
913.307.4549
Patients are anxious. Clinicians are frustrated, and IT staffs are overwhelmed. All because the EHR is missing vital patient information. Lexmark Healthcare can help. Our solutions uniquely deliver comprehensive information — medical images, documents, and clinical photos — in one view within the EHR. Ready to transform your tomorrow? Visit HIMSS booth 6225.
Liaison Technologies

Booth 11610
Contact: Amanda Thomas, director of marketing
athomas@liaison.com
408.309.0867
Liaison Technologies will be giving away a Drone a Day! You can also enter to win a Hoverboard. Stop by the booth to find out how!
LifeImage

Booth 968
Contact: Jackie Leckas, vice president, marketing
jackie@lifeimage.com
617.244.8411 x203
LifeImage is a network for connecting users and systems to patient imaging histories online. Our platform has been adopted by more than 120 multi-site health systems across the country, which use it to extend their enterprise imaging infrastructure to exchange data with outside facilities, physicians, and patients. This improves care coordination, increases referral business, and eliminates redundant imaging. Visit us at booth #968 during HIMSS16 to learn: •Best practices for integrating external imaging data into your EHR. •Common workflows for exchanging images with patients. •How to ensure your image sharing platform is interoperable with needed applications. We’ll also be giving away an Apple Watch Sport each day of the conference. For more information, visit us at www.lifeimage.com.
LogicStream Health

Booth 4977
Contact: Nicole Nash, marketing coordinator
nicole@logic-stream.net
651.269.2454
Stop by LogicStream’s booth to enter a drawing to win a hover board. Schedule your show floor demo and get a Starbucks gift card at the booth (email nicole@logic-stream.net).
MEA|NEA|TWSG

To schedule a meeting:
Contact: Jerry Thomas, chief sales officer
jerry.thomas@twsg.com
407.375.7272
Contact MEA|NEA|TWSG at marketing@mea-fast.com and find out how our solutions for hospitals, including those for esMD (Electronic Submission of Medical Documentation) – a topic that will be discussed in the HIMSS16 Session: Improving Workflow and Increasing Efficiencies with the CMS esMD Electronic Solution on March 3 – along with a suite of highly-integrated software solutions facilitate the secure exchange of health information and the efficient management of healthcare communication via voice, fax, image, data, and electronic documents. Our solutions allow clients to effectively manage critical information that typically resides outside the EHR, closing the continuum on a fully accessible patient record. www.mea-fast.com / www.tracecommunication.com
MedAptus

Booth 418
Contact: Malachi Charbonneau
mcharbonneau@medaptus.com
617.896.4000
MedAptus solutions streamline the process of delivering patient care. From simplifying pre-care clinical workforce needs to automating administrative tasks at the point-of-care, our offerings provide customers with a foundation for improved operational efficiency, personal productivity, and ultimately, optimized financial performance. Adoption of the MedAptus suite enables providers to spend their time where it matters most – with patients.
MedCPU

Booth 435
Contact: Gabriela Benincasa
GBenincasa@medCPU
Visit medCPU’s booth (#435) at HIMSS 2016 and experience a quantum leap in healthcare IT. MedCPU proudly hosts Key Opinion Leaders in Decision Support at HIMSS 2016. MedCPU joins Froedtert/Medical College of Wisconsin and UPMC at HIMSS 2016 for a timely presentation on decision-support challenges and solutions. http://www.medcpu.com/himss
MedData

Booth 5065
Contact: Chris Farrell, vice president, marketing
chris.farrell@meddata.com
440.627.2642
MedData is among the nation’s leading providers of RCM services including coding, billing, patient reimbursement, eligibility and enrollment, third-party liability, and patient satisfaction services – all with a proven compliance record. For more than 35 years, we’ve been committed to delivering industry-leading and patient-focused RCM solutions to our growing network of more than 1,000 hospital sites nationwide. Giveaways and promotions: Retro candy throughout the day and craft beer in the afternoons/evenings * ICD-10 or Not Game – Test your knowledge of the new codeset for a chance to win gift cards and other prizes.
Medecision

Booth: 3438 Population Health Knowledge Center: 14115 Career Center: 13329-8
Contact: Sherri Stuart, senior vice president, marketing services
Sherri.Stuart@medecision.com
610.540.0202
Make Accountable Predictable at HIMSS. Be sure to drop by to experience Aerial for Population Health Management. You could be the winner of Nest, a programmable WiFi learning thermostat.
Medhost

Booth 3821
Contact: Tom Mitchell, vice president, marketing
Tom.Mitchell@medhost.com
615.761.2011
Medhost HIMSS16 – Solutions to Manage your Facility, Provide Care, and Build a Brand. Visit us at booth #3821 to discover tools to transform healthcare in your community. We offer integrated EHR solutions and an engagement platform that not only empowers providers but also promotes healthy consumers while helping you build a brand and consumer loyalty. Medhost has the solutions you need to optimize patient care while running your healthcare organization with a strong bottom-line.
Medicity

Booth 4049
Contact: Lauren Tilelli, director of marketing
ltilelli@medicity.com
770.633.9013
Medicity, a Healthagen business, has been creating clinically connected communities for more than 15 years. Today, the company provides population health solutions for more than 90 million people. Medicity makes data smarter, removing the noise and turning it into a strategic asset that enables better sharing of information across the health system. This creates a new dimension in population health, one that leads to more robust analytic insights, more effective care management, and more proactive physician engagement. Medicity’s solutions further enable clinician engagement, improved transitions of care, reduced duplicative services and the opportunity for patients to take an active role in their personal health. Medicity’s breadth of industry reach includes: · 1,000 hospitals · 27 million lives in its analytics solution · 3.6 billion annual transactions · 265 unique EHRs integrated · 250,000 end-users. For HIMSS16, Medicity will be showcasing its entire suite of population health solutions, with a spotlight on Manage, its most recent care management offering. The company also will be launching its new network analytics solution, Explore SmartNetworks, which provides a more complete picture of network leakage and opportunities for network development.
Medicomp Systems

Booth 1354
Contact: Dave Lareau, CEO
info@medicomp.com
703.803.8080
Lights, camera, action! Let’s play Quipstar. Back by popular demand, Medicomp Systems invites you to play Quipstar, the World’s Favorite HIT Quiz Show. This interactive health information technology quiz show will show the live, studio audience why doctors love Quippe, and how easy it is to learn and use. New this year, teams of contestants will compete for cash and prizes using Medicomp’s newest member of the Quippe family of products, Quippe Clinical Lens. Working with existing EHR systems, Quippe Clinical Lens provides problem-oriented views of relevant clinical information at the point of care. After a brief training, Quippe contestants will utilize Quippe Clinical Lens to answer questions in a game show format. Register to reserve a seat at www.medicomp.com/himss16. Show times are Tuesday and Wednesday at 11 am and 4 pm, and Thursday at 11 am and 2 pm. Giveaways: At each show, participants will have an opportunity to win one of 5 iPad Pro tablets and cash prizes. That is a total of 30 iPad Pros over the course of HIMSS16. Register now!
Merge Healthcare

Booth 2116
Contact: Kayley Weinbaum, marketing communications lead
kayley.weinbaum@merge.com
312.946.2517
At HIMSS 2016, we will be showing multiple demonstrations of work in progress that unites IBM Research, Watson Health Imaging, and Merge technologies to help transform HIT in addition to our full solutions suite, including our Best in KLAS solution, IConnect Enterprise Archive (our VNA). IConnect Enterprise Archive helps organizations easily collect, manage, archive, and present growing volumes and variances of patient images – DICOM or non-DICOM – both from inside and beyond the walls of your healthcare enterprise.
MModal

Booth 5029
Contact: Lisa Martin, manager of marketing
lisa.martin@mmodal.com
267.535.7222
MModal’s Fluency is the only closed-loop clinical documentation platform on the market today. What does this mean to you? It means that from technology to tools to services, MModal’s Fluency platform delivers everything a healthcare provider needs to create, complete, and use clinical information in one connected platform. Learn more about our: •Front-end speech recognition •Intelligence-driven CDI •Enhanced coding workflow •Flexible transcription platform •Radiology reporting solution •Technology-enabled transcription, CDI, and coding services. MModal’s closed-loop clinical documentation solutions support the revenue cycle, facilitate compliance and quality, and most importantly, deliver information where and when it is needed most – to the physician at point-of-care. Come see us at HIMSS, booth #5029, to learn more.
National Decision Support Co.

Booth 11010
Contact: Bob Cooke, vice president, marketing strategy
rcooke@nationaldecisionsupport.com
855.475.2500
NDSC is a globally recognized provider of innovative clinical decision support (CDS) solutions widely adopted by healthcare providers and integrated with leading EHR vendors. We offer a scalable, cloud-based architecture for delivering actionable CDS based on nationally recognized guidelines into provider workflows. Through production and delivery of its flagship solution, ACRselect, NDSC has developed a proven process for digitizing consensus medical guidelines and delivering them at the point-of-care. Healthcare is evolving and so is National Decision Support Company. As part of our commitment to making medicine safer, more effective, and accessible, we have launched CareSelectDS to better reflect our company’s scope, competency, and mission. With CareSelectDS, we have broadened the current solutions portfolio in diagnostic imaging and extended its reach into lab and care pathways with the CareSelectDS content community. Whether you’re looking for more information about National Decision Support solutions and services, have specific questions about workflows and integrations, or just have some thoughts to share — we’re always interested in hearing from you.
NEC

Being the first enterprise communications technology provider in healthcare, NEC is proud to be part of HISTalk and the dedicated professionals who have grown with us and made this the most exciting, challenging, and rewarding vertical industry. Leveraging 65,000 patents and over 100 years, NEC continues to develop healthcare industry-focused applications in communications infrastructure, IT/networking solutions, and award-winning biometrics. Want to learn more about NEC’s mission to orchestrate a brighter world through optimized solutions for healthcare? Follow us @NECHealthcare or #NECHIMSS16 and join our traveling “meet-and-greet”! We will post our positions to host you for coffee or a libation several times a day throughout HIMSS.
Netsmart

Booth 5057
Contact: info@ntst.com
800.472.5509
Netsmart is committed to helping health and human services providers deliver effective, outcomes-based care to more than 25 million consumers. Netsmart serves more than 20,000 clients organizations across all 50 states, resulting in approximately 450,000 users of its software and technology solutions. Netsmart clients include mental health and addiction services agencies, health homes, psychiatric hospitals, private and group mental health practices, public health departments, social services and child and family services agencies, managed care organizations, and vital records offices. Netsmart’s CareFabric, a framework of innovative clinical and business solutions and services, supports integrated, coordinated delivery of health services across the spectrum of care. Netsmart’s HIT Value Model, a vendor-agnostic planning and measurement system, provides a path for health and human services organizations to evaluate where on the healthcare IT spectrum they should focus their efforts, the value associated with that strategic decision and a comparison with peer organizations nationwide. Netsmart is pleased to support the EveryDayMatters Foundation, which was established for behavioral and public health organizations to learn from each other and share their causes and stories. For more information, visit www.everydaymatters.com. Learn more about how Netsmart is changing the face of health care today. Visit www.ntst.com or call 1-800-472-5509.
NextGen Healthcare

Booth 4421
Contact: Lynn Belanger, marketing director
lbelanger@nextgen.com
215.657.7010
NextGen Healthcare is a leader in value-based care, population health, interoperability, and revenue cycle services. See demos and speak with our experts on how we help practices foster healthy communities, engage patients, manage care, and deliver healthy bottom lines – all key elements for a successful transition to value-based care. We will be showcasing solutions designed to help you transform your practice to a value-based revenue entity. To totally understand the costs associated with your provider model, you’ll need to meet at least three goals: Achieve interoperability – data exchange and aggregation across hospitals, physicians, and other systems for a clear, longitudinal view of the patient and your population; enhance the patient experience ― patient access, patient engagement, and communication; and improve financial performance ― revenue cycle management and operational efficiencies. While you’re at our booth, pop across the aisle and visit booth #4429 to see how NextGen interoperability, powered by Mirth technology, is changing the game for interoperability and patient data management, and helping to facilitate care for over 150 Million patients. Happy Hour each day! Of course, we’re not all work and no play! We invite you to stop by the booth after a long day pounding the convention floor for a pick-me-up. Happy hours run the last hour of the show each day at our booth. Get your headshots at the NextGen Healthcare booth: Drop by and “Say Cheese!” If the last headshot you got was in high school or college, then you NEED to stop by NextGen Healthcare booth #4421. We know you look good and we want to give you proof. We’ll be taking professional headshots for attendees, so stop by and let us get your best side! Headshots will be available about a week after HIMSS16.
Nordic

Booth 8233
Contact: Drew Madden, president
drew.madden@nordicwi.com
608.616.2000
Visit Nordic, Help a Charity – Stop by booth #8233 and vote on one of three charities to which Nordic will donate money at the end of HIMSS. The charity with the most votes will get the largest donation. As a bonus, while you’re at the booth, you can chat with any of our health IT experts about improving health outcomes and the health of your business with our #1 in KLAS EHR consulting services. Visit booth #8233. Vote on a charity. Have a great HIMSS16.
NTT Data

Booth 3854
Contact: Larry Kaiser, senior marketing manager
lawrence.kaiser@nttdata.com
310.301.1284
NTT DATA offers IT solutions that increase efficiency, reduce medical errors, and enhance the revenue cycle. Our ONC-ATCB certified solution, Optimum, features an industry-leading RCM solution, EHR, ERP, portal, and post-acute solutions. Reasons attendees should visit the NTT DATA booth: 1. Discuss current industry trends and see how NTT DATA is addressing them. 2. Learn about what NTT DATA offers. 3. Have your mind read by our mentalist. NTT DATA will be giving away a drone to attendees who watch our show and get a raffle ticket.
NVoq

Interoperability Showcase Booth 11954-38
Contact: Debbi Gillotti, CMO and VP/GM Healthcare
deborah.gillotti@nvoq.com
206.465.1765
NVoq is a cloud-based provider of speech recognition services for the healthcare industry headquartered in Boulder, CO. We offer a real-time client application and RESTful API services for developers to voice-enable their applications, and optional point-of-care coding support for ICD-10 and other standards. No voice training is required to use SayIt, so providers can be productive immediately. Our proven cloud solution works anywhere there’s an Internet connection and there’s no network software or equipment to purchase. In the 2016 Interoperability Showcase, we’ll be demonstrating how simple SayIt voice commands can convert audio to text, create structured data using NLP, and interface structured data directly to major EHRs. We’ll be presenting a variety of specialty use cases illustrating the range of workflow automation powered by SayIt. Didn’t think you had options for speech recognition? You do now. Come see us in booth 11954-38.
Obix by Clinical Computer Systems

Intelligent Health Pavilion Booth 11655 and Booth 6052
Contact: Heather Ruchalski, director, marketing
marketing@obix.com
888.871.0963
Obix by Clinical Computer Systems, a medical software company, will be participating in the Intelligent Health Pavilion at HIMSS. We are sponsoring the LDR Suite in the pavilion, which will highlight ours and other technologies associated with labor, delivery, and recovery of mother and baby. Within the pavilion, we will be in Kiosk 6, where you can learn more about our strategic perinatal software solutions. The Obix Perinatal Data System is a comprehensive, computerized system for central, bedside, and remote electronic fetal monitoring. It includes archiving, point-of-care charting, single-click management reports, and Internet-based physician access. We will also feature the TrueLabor Maternal Fetal Monitor, which offers a unique digital signal processing technology that enhances fetal monitoring in evaluating uterine contractions and FHR information. We would like to spotlight two speakers that will be presenting in the Leadership Theater within the pavilion on Tuesday, March 1. 1 pm – 1:30 pm Sean Blackwell, MD will speak to: Resign of Patient Care Work Flow for the Diabetic Gravida: What Should We Be Doing in the Digital Age? 3:15 pm – 3:45 pm Dick Taylor, MD will speak to: A Clinician in the Intelligent Hospital: Free to be Me. You will have the opportunity to ask questions following their presentations.
Oneview Healthcare

Booth 8215
Contact: Jeff Fallon, president, North America
jfallon@oneviewhealthcare.com
724.272.1240
Oneview Healthcare, founded in Dublin, Ireland in 2007, is a patient engagement technology company. Come to our booth (8215) for a pint of Guinness, Irish music, and Irish dancers from 4:30 to 6:00 pm on Tuesday, March 1 and Wednesday, March 2! Or stop by any time for a demo and to meet the team. Oneview Healthcare’s patient engagement solution integrates seamlessly with a hospital’s existing EHRs to connect patients with their care teams across the care continuum. While patients enjoy movies on demand, games, meal ordering, hospital concierge services, educational content, and more at their fingertips on a bedside device, the solution works behind the scenes, gathering valuable data for hospitals. Tasks and requests are routed seamlessly to the right resources at the right time, streamlining hospital workflows and creating a relaxed environment for patients. Perhaps most importantly, hospitals can keep a real-time pulse on patient satisfaction through customized surveys they can distribute at any time. Oneview’s ambulatory solution, Oneview Connect, brings patient engagement full circle on patient mobile devices. Patients receive pre-admission scheduling, notifications, and education to prepare them for their hospital visits. They can view maps and check in once they arrive. The high-touch interaction continues post-discharge as patients receive follow-up care notifications, appointment scheduling and continued education, all with care team messaging capabilities to ensure all questions are answered and patients are fully equipped to take care of themselves at home.
Optimum Healthcare IT

To schedule a meeting:
Contact: Jenny Paal, marketing manager
jenny@optimumhit.com
904.373.0831
Optimum Healthcare IT is committed to building a true business partnership with our clients. We are not just another staff augmentation vendor or consulting firm. Our motivation and passion is about supporting your success and healthy outcomes for your patients. We understand patient care does not stop so your health system can implement new IT processes. That is why our clients rely on our expert IT consultants and FTEs to manage the IT side of the implementations so our clients can focus on their patients. Our commitment to providing excellence in service is driven by a Leadership team with more than 50 years of experience in providing expert healthcare staffing and consulting solutions to all types of organizations. We are passionate about what we do and work hard to deliver premium services to our clients. This philosophy starts at the top of our organization and is the core set of values we impart in all of our employees and consultants. Optimum Healthcare IT is different from the rest because we have built our business on personal experience, based on years in the healthcare industry. We have been on both sides of the transaction and know what is most important to our clients and our consultants. We have based our business model on attracting the best and brightest consultants the industry has to offer, who are experienced clinicians and hospitalists and are considered to be experts in Healthcare Information Technology and business. Working with these stellar consultants make our presentations to healthcare systems that much more impressive. Our ability to view the client from this holistic perspective gives us the advantage of providing superb services, which span a large spectrum of Service Lines. When our clients have a need, we can fulfill it.
Orchestrate Healthcare

Booth 7520
Contact: Charlie Cook, president
charlie@orchestratehealthcare.com
877.303.3377
What Happens In Vegas … Helps You Positively Impact Your Organization! Stop by booth #7520 to hear how our consulting philosophy is Best In KLAS, share with us your upcoming projects and learn how we come in on-budget and without scope creep, and discuss how our information security practice can proactively help your organization. See how 30 impactful minutes with us will change your IT consulting direction!
Patientco

Booth 14034
Contact: Annie Czarnecki, sales representative
annie.czarnecki@patientco.com
888.747.2455 x401
Patientco empowers healthcare providers to optimize and increase patient revenue cycle efficiency with cloud-based patient payment technology. Patientco goes beyond basic payment processing to connect every patient payment event throughout multi-facility healthcare networks—delivering unrivaled visibility into and control over the patient revenue cycle. The result is improved cash flow, reduced A/R days, cost-saving efficiencies, and increased patient and provider satisfaction. Any provider who schedules and attends a Patientco demo will receive a $25 Amazon Gift Card.
PatientKeeper

Booth 5249
Contact: Cristina Christy, senior events manager
cchristy@patientkeeper.com
(781) 373-6378
PatientKeeper believes in the promise of IT to enable better healthcare, just as numerous medical technology innovations over the years have dramatically improved our quality of life. Visit our exhibit at HIMSS16 to discover the many ways PatientKeeper is making physician lives better through intuitive applications that streamline order entry, medication reconciliation, documentation, charge entry, and other common workflows. While you’re visiting, have your picture taken in our Pioneers of Modern Medicine photo booth.
PatientMatters

To schedule a meeting:
Contact: Sheila Schweitzer, CEO
info@patientmatters.com
407.872.7969
PatientSafe Solutions

Booth 4257
Contact: Alex Condurso, senior manager, marketing
acondurso@patientsafesolutions.com
760.525.1081
Schedule your show floor demo and get a Starbucks gift card at the booth! http://www.patientsafesolutions.com/himss-2016
PDR

Booth 1068
Contact: Todd Helmink, national senior vice president, business development
todd.helmink@pdr.net
201.358.7140
Trusted by generations of healthcare providers, PDR delivers innovative health knowledge products and services that support prescribing decisions and patient adherence to improve health. As a leading provider of behavior-based prescription management programs, PDR provides event-driven and clinically relevant healthcare messaging through its patented process that improves patient compliance and outcomes, while preserving privacy. This network is made up of e-prescribing, EMR, and EHR applications, chain and independent pharmacies, and sponsors of healthcare-related education such as pharmaceutical manufacturers, health plans, payers, and pharmacy benefit managers. Learn more at www.pdrnetwork.com.
PeriGen

To schedule a meeting:
Contact: Chip Long, senior vice president, growth and development
chip.long@perigen.com
727.460.8167
PeriGen offers the only fetal surveillance software solution that is single-vendor, comprehensive, and fully-integrated. While at HIMSS, preview our new "on-demand" perinatal integration feature.
PerfectServe

Booth 225
Contact: Leigh Ann Myers, chief clinical officer
lmyers@perfectserve.net
865.212.6140
PerfectServe delivers healthcare’s only secure care team collaboration platform, making it easy to quickly connect with the right care team member in any situation. Using a cloud-based system, PerfectServe Synchrony features Dynamic Intelligent Routing, high reliability notifications, cross-organizational connectivity, and proven interoperability. Nearly 58,000 physicians use the platform for improved care team productivity, better patient experience and HIPAA-compliant messaging. At PerfectServe booth #225, you’re going to feel like a kid in a candy store. Not only will you be surrounded by sweet treats, you’ll get to play with devices and experience first-hand how PerfectServe Synchrony can enable more efficient and productive care teams.
Phynd Technologies

Booth 10728
Contact: Tom White, CEO
twhite@phynd.com
855.749.6363 x710
The Phynd Unified Provider Management (UPM) Platform allows healthcare organizations to unify, manage, and share a single, verified, custom profile on each of their providers, regardless of where that data exists in their multiple legacy IT systems. With the UPM Platform, hospitals and health systems have the ability to manage their provider (referring and credentialed physicians, nurses, and mid-levels) profiles across all of their core IT clinical, financial, and operational systems. This single, accurate source for provider information streamlines workflow, improves productivity, speeds up billing, optimizes the revenue cycle, and enhances care coordination enterprise-wide.
Point-of-Care Partners

To schedule a meeting:
Contact: Tony Schueth, CEO and founder
tonys@pocp.com
877.312.7627
Point-of-Care Partners is a leading management consulting firm assisting healthcare organizations in the evaluation, development, and implementation of winning health information management strategies in a rapidly evolving electronic world. Our accomplished healthcare consultants, core services, and methodologies are focused on positioning your organization for success in the integrated, data-driven world of value-based care. Areas we can help you achieve success include: •ePrior Authorization (drug, device, procedure) •ePrescribing/EPCS/Specialty •Clinical Decision Support •Biosimilars (tracking, tracing, naming) •Health Information Exchange •Long-term, Post-Acute Care •Patient Engagement •Population Health/Analytics •Specialty Pharmacy Automation •Telehealth •Medication Therapy Management. In addition, we provide resources to help you stay up-to-date with frequent changes in US healthcare regulatory requirements for both ePrescribing and electronic prior authorization. Visit www.pocp.com to learn more.
Porter Research

To schedule a meeting:
Contact: Cynthia Porter, president
cynthia@porterresearch.com
678.427.6241
Porter Research has been in the healthcare IT industry as a proven go-to-market research firm for HIT vendors, healthcare payers, providers, biomedical companies, and consumers for 25+ years. Porter Research offer seven proven services: •Go to Market Strategy Research •Win-Loss Analysis •Brand /Competitive Analysis •Content Development •Customer Experience •Prospect Profiling/Lead Generation •Mergers and Acquisition Research Services. “So many companies in healthcare attempt to package and launch new solutions without fully understanding their target market, articulating their value proposition, and correctly positioning their solution,” says Cynthia Porter, president, Porter Research. We solve these foundational business problems through data-driven research and decades of healthcare experience. “By truly listening to the market and building strong value propositions that resonate with targets, our clients achieve faster brand awareness, market penetration, and business growth.” Porter has worked with over 300 HIT vendors, payers, providers, and biomedical companies since its inception in 1989.
Qpid Health

Booth 11421
Contact: Amy Krane, senior director, marketing
Amy.Krane@QpidHealth.com
617.982.5400
Is your CFO asking if your value-based reimbursement is what it should be? Do your clinical leaders doubt you are getting credit for the care you deliver? Is manual data abstraction to fill the gaps your current – and costly – solution? If so, it’s time to take a fresh look at how you are reporting on quality measures. Please visit us in Booth #11421 to learn how QPID Health’s clinical reasoning technology locates and synthesizes information from anywhere in patient records to streamline quality reporting, clinical data registry submissions, and medical necessity reviews. Sorry no raffles or giveaways. But … we guarantee that you will be a Super Hero to your team back home when you tell them there’s a new way to optimize the data in your EHR.
Recondo Technology

To schedule a meeting:
Contact: Jay Deady, CEO
jay.deady@recondotech.com
Now THIS is a game-changer…. If you are interested in learning about the FIRST true, self-service price transparency solution in healthcare, reach out to Recondo’s CEO, Jay Deady, to schedule some time to connect at HIMSS2016. jay.deady@recondotech.com. View a demo of the first self-service price transparency solution in healthcare and receive a FREE Amazon gift card.
Sagacious Consultants

Booth 4770
Contact: Stephanie Speth, manager, marketing
stephaniespeth@sagaciousconsultants.com
314.487.0819
Sagacious Consultants leverages its extensive Epic and healthcare industry experience to drive financial performance and improve patient care in organizations worldwide. Using proven methodologies for revenue and clinical transformation, Sagacious Consultants improves KPIs and enhances provider efficiency. Sagacious Consultants is now part of Accenture, expanding its breadth of services and geographies served. Visit Sagacious Consultants at HIMSS booth #4770 to chat with our EHR experts and pick up some great swag! Hear our revenue cycle presentations: 1) “Rady Children’s Hospital Recharges its Revenue Cycle” on Tuesday, March 1 at 11:00 am in the Accenture Booth #7710; and 2) “IT Transformation: Rev Cycle Insights from the CIO” on Wednesday, March 2 at 2:30 pm in the Rock of Ages Theater, Session ID: 155.
Santa Rosa Consulting

Booth 2157
Contact: Ashley Burkhead, sales operations and marketing manager
ashleyburkhead@santarosaconsulting.com
972.804.4216 (texts welcome)
Booth Giveaway: This year, we will have another tiered giveaway program. We will be giving away 2 items: a $100 Amazon gift card and a tablet (winner’s choice – value up to $400).
Sensato

Booth 11612 (Divurgent’s booth)
Contact: John Gomez, CEO
john.gomez@sensato.co
844.736.7286
Cybersecurity – one of the hottest and most challenging topics facing HIT leaders this year. Unfortunately, the topic is surrounded by hype, conjecture, and a healthy dose of myth. Practical strategies, approaches, and real-world solutions are fast becoming unicorns. Sensato is a small, boutique healthcare cybersecurity firm – we are 100-percent focused on HIT and our DNA is HIT. We don’t use hype, fear, or uncertainty to establish long-term partnerships. Rather, we focus on earning the trust and support of our clients by providing real-world, practical cybersecurity solutions that are respectful of an organization’s challenges and economics. Medical Device Security – Managed Security Services – Compliance – Security Operations Center – Education – Incident Response – Incident Simulation – Strategic Planning – Virtual CISO – Friends – Partners – Coaches … yes … stop by … introduce yourself … changing the world starts by just saying hello! 😉
Spok

Booth 4829
Contact: TJ Fisher, business solutions advisor
thomas.fisher@spok.com
952.230.5366
Spok is proud to be a leader in critical communications for healthcare, government, public safety, and other industries. We deliver smart, reliable solutions to help protect the health, well-being, and safety of people around the globe. Organizations worldwide rely on Spok for workflow improvement, secure texting, paging services, contact center optimization, and public safety response. When communications matter, Spok delivers. JOIN SPOK AT HIMSS IN BOOTH 4829 TO SEE HOW YOU CAN: • Manage patient alarms to reduce alarm fatigue and improve the patient experience • Encrypt smartphone communications for HIPAA compliance • Deliver patient test results quickly to speed discharge times • Reach the right on-call clinician quickly for well-coordinated care. Spok will do one drawing at the end of each exhibit day for a chance to win an Amazon Echo.
Stanson Health

Booth 162
Contact: Kimberly Denney, vice president, commercial operations
kimberly.denney@stansonhealth.com
747.220.4190
Stanson Health recently launched version 2.0 of its closed-loop analytics platform. This powerful platform pulls in all alert data of every type from best practice notifications to drug-drug, barcode, health maintenance, allergy, duplicate checking, etc. to provide more meaningful provider insights across your EHR’s entire alerting environment. During our in-booth demonstrations, we can show you how Stanson Health’s closed loop analytics and active CDS have helped our clients save on average $3k per provider.
Stella Technology

Interoperability Showcase Booth 11954 |Exhibit Hall G Use Case #11
Contact: Salim Kizaraly, senior vice president, business development and founder
salim@stellatechnology.com
650.793.4131
Visit the Stella Technology kiosk located in the HIMSS16 Interoperability Showcase booth 11954 in Exhibit Hall G. Stella Technology will be conducting the following product demonstrations and theater presentations:
- Interoperability Showcase Use Case #11 – Stella Technology will participate in this use case by ensuring that the clinical documentation (CCDA) sent by the PCP to the specialist as part of the referral is of high and meaningful clinical quality, as measured by its IQHD (Inspector of Quality Healthcare Data) tool.
- Demonstration of the Interoperability Test Tool (ITT) used by the ConCert by HIMSS
- lnteroperability Showcase Theater Sessions:
Tuesday, March 1st at 1:00 pm PT. Come listen to our interoperability expert and CTO, Lin Wan, who will be presenting on the topic of “Content Interoperability” and how to overcome any challenges your organization is having around the quality of your clinical data.
Wednesday, March 2nd at 12:00 pm PT. “ConCert by HIMSS: The Trusted Solution for Interoperability.” Learn how the ConCert by HIMSS certification program is defining interoperability.
- HIMSS Blog: "Content Interoperability: Achieving Clinical Data Quality Success" by Lin Wan, CTO, Stella Technology – http://www.himssconference.org/updates/content-interoperability-achieving-clinical-data-quality-success We look forward to seeing you at the Interoperability Showcase!
Strata Decision Technology

Booth 119
Contact: Rachael Britnell, senior marketing specialist
rbritnell@stratadecision.com
312.827.7711
Strata Decision Technology provides an innovative, cloud-based financial analytics and performance platform that is used by healthcare providers for financial planning, decision support, and continuous improvement. Founded in 1996, the company’s customer base includes 1,000 hospitals and many of the largest and most influential healthcare delivery systems in the US including CentraCare Health System, Fairview Health Services, Mission Health, and Yale New Haven Health System. The Company’s StrataJazz application is a single integrated software platform that includes modules for capital planning, contract modeling, cost accounting, cost management, decision support, financial forecasting, management reporting, operational budgeting, and performance improvement and strategic planning. StrataJazz earned top honors for the second consecutive year as the KLAS 2015/2016 Category Leader for Decision Support – Business in the 2015/2016 Best in KLAS: Software and Services report. The company has also been recognized with the Chicago Innovation Award, as one of Becker’s Healthcare 150 Great Places to Work in Healthcare, #1 in Black Book Ranking, and inclusion on the Inc. 5000 Fastest Growing Companies list, among many other industry accolades.
Summit Healthcare

Booth 3700
Contact: Sara Wildes
swildes@summit-healthcare.com
781.519.4840
Summit Healthcare offers an array of integration/automation solutions. Our Summit Downtime Reporting System delivers access to critical data during downtime, while the Summit Scripting Toolkit and Summit InSync cover your automation needs. The Summit Interoperability Platform features the Summit Express Connect interface engine; Summit Care Exchange, which supports CCD data exchange with an integrated HISP; and Summit Provider Exchange, which simplifies bi-directional physician office integration. Visit us at booth #3700.
Sunquest Information Systems

Booth 1925
Contact: Corrine Tso, vice president, marketing
corinne.tso@sunquestinfo.com
520.570.2240
At HIMSS16, Sunquest is demonstrating its solutions to enable fully-connected diagnostic communities across the care continuum. Attendees can receive in-booth demonstrations of Sunquest’s clinical and anatomic pathology solutions, as well as learn more about how GeneInsight, Atlas Medical, and Data Innovations can enhance the Sunquest solution. In addition to solution demos, Sunquest and Jitin Asnaani, the executive director of the CommonWell Health Alliance, will co-present on the future of interoperability and Sunquest’s strategy. Join Sunquest at HIMSS16, booth #1925.
SyTrue

To schedule a meeting:
Contact: Kyle Silvestro, CEO
kyle@sytrue.com
530.321.7484
Talksoft

Booth 2272
Contact: Josh Mogilefsky, finance manager
jmogilefsky@talksoftonline.com
866.966.4700 x6023
The Coolest thing in Healthcare! Giveaways include coolers and beverage coozies.
Fujifilm Medical Systems – TeraMedica Division

Booth 1024
Contact: Beth Roncke, manager, marketing communications
beth.roncke@fujifilm.com
414.908.7744
Synapse VNA integrates more specialties, more devices, and more data than any other VNA. Period. With 16 years of industry leading experience, our TeraMedica Division remains independently focused on advancing VNA technology and healthcare interoperability, while now leveraging Fujifilm’s clinical capabilities. As the centerpiece of Fujifilm’s comprehensive medical informatics portfolio, Synapse VNA provides the industry’s leading image management solution. Schedule your private HIMSS16 appointment at himss.fujimed.com and visit us in booth 1024.
TransUnion Healthcare

Booth 11318
Contact: Pat Gilmore, vice president, sales
pgilmor@transunion.com
303.256.7187
TransUnion’s ClearIQ patient access platform and coverage discovery solutions (eScan) more accurately identifies and helps providers understand, predict, and integrate the financial behavior of patients so they can efficiently maximize reimbursement for the care provided, which ultimately help providers reduce uncompensated care and deliver a more transparent and improved patient experience.
T-System

To schedule a meeting:
Contact: Ann Baty, senior marketing communications manager
abaty@tsystem.com
469.791.2445
Robert Hitchcock, M.D., FACEP, T-System Chief Strategy Officer will be leading an educational session alongside Joseph Pocreva, M.D., Col., USAF, MC, Medical Director, Keesler Medical Center at HIMSS16. Learn how to leverage the power of EHR data to facilitate process change and improve key performance indicators. Using the U.S. Air Force’s Keesler Medical Center as an example, this session discusses utilizing EHR data to actively manage and make decisions related to clinical flow, throughput, staffing resources, bottlenecks and more.
HIMSS Presenter Session ID 57: http://www.himssconference.org/session/using-ehr-data-process-change-throughput-and-satisfaction
Valence Health

Booth 1368
Contact: Kevin Weinstein, chief growth officer
k_weinstein@valencehealth.com
888.847.0250
If you’re not familiar with Valence Health, we’ve been helping provider organizations accept financial responsibility and rewards for the care they provide since 1996. With our integrated set of population health technology, advisory services, and managed services, our goal is to help you make the essential volume-to-value transition as seamless as possible. Visit us at booth #1368, where we’ll be showcasing our population health technology solutions, which help you: •Aggregate multiple data sources to create a comprehensive patient view •Identify and close care gaps to manage populations •Measure performance to align clinical and financial goals and •Track patient adherence to care plans.
Validic

To schedule a meeting:
Contact: Chris Edwards, chief marketing officer
chris.edwards@validic.com
919.260.2231
Validic is the healthcare industry’s leading cloud-based, digital health platform. Validic provides convenient and quick access to patient data from in-home clinical devices, wearables and patient healthcare applications. By connecting its growing base of customers – that includes providers, pharmaceutical companies, payers, wellness companies and health IT vendors – to the continuously expanding list of digital health technologies, Validic enables healthcare companies to better coordinate care across their communities, improve their patient engagement strategies and more efficiently manage their patient populations. Validic’s innovative, scalable and FDA Class I MDDS technology delivers actionable, standardized, and HIPAA-compliant consumer health data from the best in-class mobile health devices and applications. Validic was recognized for healthcare innovation by Gartner and received Frost & Sullivan’s Best Practices and Best Value in Healthcare Information Interoperability award, as well as Top Ten Healthcare Disruptor award. Validic’s leading global digital health ecosystem reaches over 160 million lives in 47 countries and continues to grow daily. To learn more about Validic, follow Validic on Twitter at @validic or visit www.validic.com.
Versus Technology

Booth 5246
Contact: Jeanne Ehinger, marketing communications manager
jeannee@versustech.com
231.946.5868
Are you looking for locating technology but can’t decide on a direction? With our multi-platform, scalable approach, you’re always on the right path with Versus. Whether you want to leverage WiFi infrastructure for enterprise visibility or delve into advanced locating to optimize clinical workflow, your first step begins at HIMSS16. The only live RTLS demonstration on the exhibit floor, our Experience Center features a fully operational Versus Sensory Network, demonstrating real-time cues for clinical workflow. Learn how we use location data combined with powerful workflow intelligence to not only drive efficiency at the point of care, but also automatically document key measures – helping you measure and manage your operations. We also offer ample opportunity to speak peer-to-peer with RTLS users. Visit the Versus booth to meet a client with 10 years of experience using RTLS automation across eight different solutions. Or, visit us during our exhibit hall cocktail reception, where you’re sure to meet more Versus clients – Wednesday from 4-6pm.
Vital Images

Booth 732
Contact: Nichole Gerszewski, corporate brand and PR manager
ngerszewski@vitalimages.com
952.487.9500
Visit Vital’s booth (#732) to get your All Access Pass to our VIP Suite featuring game-changing technology. Learn more about VNA on demand, zero-cost data migration, personalized viewing, enterprise interoperability, ACO image governance, and more.
VitalWare

Booth 6251
Contact: Leslee Paganelli, ambassador, company culture and communication
lesleepaganelli@vitalware.com
VitalWare makes the business of healthcare easier through intuitive cloud-based technologies and advanced knowledge sharing. Our team shapes businesses in the marketplace by delivering best-in-class products and service for a powerful user experience. We identify and simplify challenges in an ever changing and regulated industry, making your job easier. Visit us in booth #6251 to speak with our experts and enter for a chance to win a GoPro HERO.
Wellsoft

Booth 3128
Contact: Denise Helfand, vice president, sales and marketing
dhelfand@wellsoft.com
800.597.9909 or 732.507.7200
Wellsoft Corp., developer and provider of the industry-leading EDIS since 1988, offers complete solutions for freestanding emergency centers, hospitals EDs and urgent care centers. Visit Wellsoft at HIMSS16 – Booth 3218 and learn more about 1) How to realize more revenue each year with Wellsoft 2) Why Wellsoft is ranked #1 3) Why clinicians and IT love Wellsoft. Wellsoft EDIS is Best in KLAS – Wellsoft ranked #1 in the 2015/2016, 2014, 2013, 2012, 2010, 2009, 2008, 2007, 2006, 2003, and 2002 Best in KLAS Awards: Software & Services Emergency Department Market Segment.
West

Booth 6221 & 4200
Contact: Tanya Flores-Olney, campaign marketing manager
ttflores-olney@west.com
800.841.9000
The West Engagement Center combines technology enabled communications with clinically managed services to activate and engage patients beyond the clinical setting. Our solutions for patient access, routine care, transition care, chronic care, and RCM help organizations maximize revenue, quality, and the patient experience. Stop by daily for a hot cup of gourmet coffee and a chance to win an Apple Watch.
Wolters Kluwer – Clinical Drug Information

Booth 5537
Contact: Matthew Bennardo, market manager
matthew.bennardo@wolterskluwer.com
330.650.6506
Wolters Kluwer Clinical Drug Information joined forces with some of our Medi-Span drug data clients, collaborating on two presentations for HIMSS16 — both related to how healthcare organizations used Medi-Span filter settings and standard EHR tools to better manage alerts, helping reduce noise and the fatigue that comes with unwanted alerts, while simultaneously enhancing medication safety and clinical decision support.
ALERT FATIGUE: IMPROVING ALERT IMPACT BY REDUCING NOISE
WHEN: Wednesday, March 2, 4-5 pm PT
WHO: Michael Ochowski and Phillip Boll, Group Health Cooperative South Central Wisconsin
OPTIMIZING DRUG DOSE CHECKING TO MINIMIZE ALERT FATIGUE
WHEN: Friday, March 4, noon-1 pm PT
WHO: David Kaelbar, MD, The MetroHealth System, Cleveland, Ohio
Come visit us at HIMSS booth 5537 and tell us about your alert wish list. We can share more about how we help healthcare organizations reduce alert fatigue and better manage and optimize medication-related alerts.
Xerox

Booth 8005
Contact: Kirsten LeMaster, vice president, marketing and communications, Healthcare Provider Solutions, Xerox
Kirsten.lemaster@xerox.com
214.693.5040
Xerox Healthcare helps healthcare organizations focus on improving lives through better, more affordable, and more accessible care by designing processes that work for the people delivering, enabling, and receiving care. We provide a range of technology, analytics, and business process solutions to over 2,200 hospitals, 32 states, and major health plans. Come visit us at booth #8005 and learn why so many health professionals choose us. We can help you implement EHR and ERP, optimize business processes, increase technology adoption, deliver quality and care data, support claims accuracy, communicate member benefits, drive medication adherence, provide risk assessments, and enable access for patients. Stop by our booth to speak to Regina Holliday, artist, influential patient advocate, and founder of The Walking Gallery. She will be speaking with guests and painting their stories in the Xerox booth.
ZeOmega

Booth 262
Contact: Gus Orr, marketing manager
gorr@zeomega.com
214.619.3961
Stop by ZeOmega’s booth (#262) at HIMSS to learn how we can supercharge your EHR and deliver the unique tools you need for a successful transformation to value-based care. While you’re there, you can recharge your mobile device at our convenient charging station while you complete a Jiva demo!
ZirMed

Booth 6647
Contact: Stacy State, director of enterprise marketing
Stacy.State@zirmed.com
888.803.8732
1. Stop by booth #6647 at HIMSS16 to learn how leading US hospitals and health systems uncover 1-3 percent in new net patient revenue.
2. Visit ZirMed at booth #6647 to find out how one health system cut AR days by more than 20 percent — while implementing a new EHR and growing their physician business by more than 20 percent!
3. Come see ZirMed at booth #6647—meet the team that just won Best in KLAS for the third year in a row, and learn about ZirMed’s solutions for population health, remit and deposit management, and AR management!
Comments Off on HIStalk’s Guide to HIMSS16



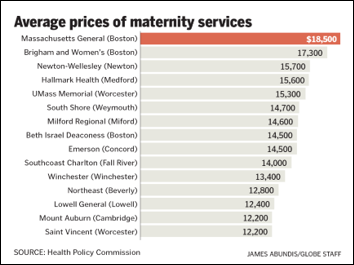


















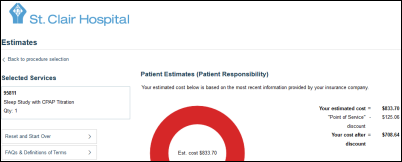













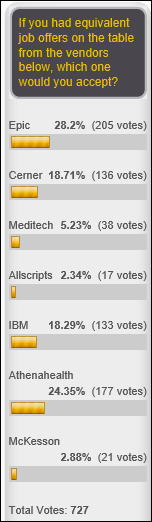



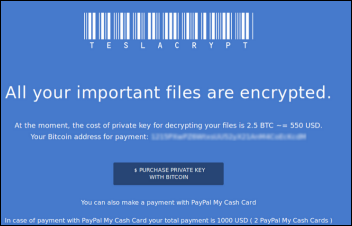




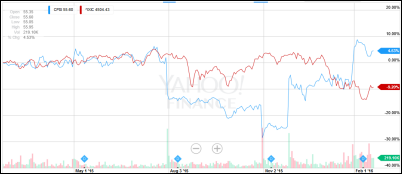


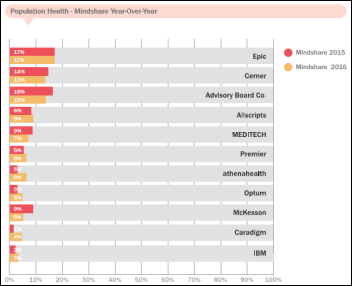











































































































Aaand, 4th to last graf, 1st sentence, not a distance, so you would go further, not farther.