Monday Morning Update 8/4/25
Top News
Digital physical therapy vendor Sword Health launches an AI division.
Sword Intelligence will have its own dedicated team and go-to-market strategy in operating outside of the company’s care delivery business. It will sell solutions to health systems, governments, and payers.
Sword Health’s June 2025 funding event valued the company at $4 billion.
Reader Comments

From Doc Martin: “Re: Sol Health rebrand. I thought this email notice was a joke at first. At least they named themselves after the most frequent response to mental healthcare needs nowadays.” The company renamed itself Sol Mental Health in 2023 as a reference to the sun. A hyped up rebrand evangelist decided it would be much cooler to shout it out in ALL CAPS, which turned the solar-themed company name into a version that starts with a vulgarity and ends with “out of luck.” HIStalk don’t play that — I capitalize the first letter even if the company doesn’t (Athenahealth), excise gimmicky symbols (M*Modal), and lowercase everything but the first letter unless it’s a clear initialism (KONZA Network is fine, SOL Health is not). Pedantic grammar note: an initialism is an abbreviation where each letter is pronounced (EHR), while an acronym is pronounced as a word (FHIR). Long-timers will recall the annual conference when HIMSS told its staff to turn the name into an initialism, forcing them to perform lingual gymnastics to sound it out as H-I-M-S-S to justifiably puzzled looks.
From Yardbird: “Re: LLMs. They might encourage generalists to manage specific conditions instead of sending the patient to a specialist if judgment rather than a procedure is involved.” That could happen and fits the cognitive displacement theory in which LLMs will replace people whose jobs involve recalling obscure facts, following a checklist, or reformatting information into a desired format such as a legal brief or a prescription. You could argue that non-procedural specialists often rely on pattern recognition to make a blink diagnosis that an LLM could replicate, with a generalist present to meet legal requirements or apply minimal judgment. Medicine changes so fast that the most valuable thing a specialist might offer is the focused-factory advantage of volume-bred expertise.
HIStalk Announcements and Requests
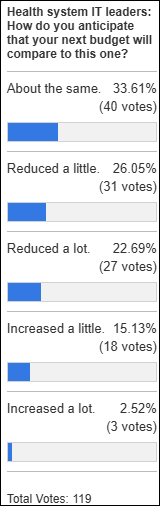
About half of health system IT leaders expect their next budget to be less than the current one.
New poll to your right or here: How much will HHS’s “Make Health Tech Great Again” voluntary campaign improve healthcare?

I got some $10 AirPod knockoffs from Temu that are surprisingly good. Similar-looking versions go for as little as $5. I rarely use earbuds, so I was startled by the clarity and volume when I queued up some R.E.M. I’m sure the Apple product is fine, but not worth $200 to me.
I’m using Substack to create a solo hobby-style newsletter-website. It’s free unless you charge subscribers (that’s why I’m using it instead of the not-free Beehiiv) and definitely worth $100 or so to hire a Fiverr freelancer to tweak the CSS for formatting changes that the Substack UI doesn’t allow.
Sponsored Events and Resources
None scheduled soon. Contact Lorre to have your resource listed.
Acquisitions, Funding, Business, and Stock

Waystar reports Q2 results: revenue up 15%, EPS $0.36 versus $0.26, beating analyst expectations for both. WAY shares are up 72% since their June 2024 IPO, valuing the company at $6.2 billion.
Visage Imaging’s parent company Pro Medicus invests $10 million in lung function technology vendor 4DMedical.
Government and Politics

I was surprised to see NantHealth as a participant in HHS’s “Make Health Tech Great Again” event. I’m actually even more surprised that the company remains in business — shares are down 99.99% to just over a penny since the company’s much-touted IPO in June 2016, its market cap has been flat for years at less than $500,000, and the company’s top institutional shareholder owns less than $1 worth. It’s one of 11 Nant-named companies that were spawned off by billionaire Patrick Soon-Shiong, MD under the NantWorks label.
Other
A study finds that most ED patients who had a high mortality risk did not have their advance directive and treatment goals recorded in their EHR. The authors checked for healthcare proxy, power of attorney, living will, advance care plans, and physician orders for life-sustaining treatment.
Epic consulting firm Anura Connect posts on LinkedIn that some third-party EHR consultants are quietly double-dipping by working two full-time jobs at once and being paid by multiple health systems. The company says it’s easier to pull off now with loosely supervised remote work and a lack of vetting when hiring. It warns consulting firms that their reputation and long-term relationships could suffer when a client finds out, while the consultant themself could be blacklisted, at least until the next desperate recruiter calls.
Sponsor Updates

- SmarterDx donates $10,000 to Children’s Hospital Colorado.
- Black Book Research highlights Waystar in its latest report on the prior authorization technology landscape.
- Linus Health partners with consumer experience software vendor League to make online cognitive screening and care available to consumers through private health plans.
- Arcadia will provide its customers with a streamlined pathway into the CMS Aligned Network Strategy.
- Inovalon’s Converged Quality solution achieves NCQA HEDIS Measure Certification for HEDIS Measurement Year 2025.
- Ellkay, Surescripts, and TruBridge announce their support for the CMS Digital Health Ecosystem and Interoperability Framework.
- Nym names Sasha Ben David software engineer, Noa Landau coding specialist, Victoria Fitzgibbon and Kim Langner medical coding and compliance auditors, and Maya Enoch product manager.
- Symplr will present at AHRMM 2025 August 5 in Denver.
- Waystar will exhibit at the Mid America Summer Institute August 4-8 in Omaha, NE.
- CereCore releases a new podcast episode titled “The Value of Leadership and Optimization: A CNO to CEO Story.”
Blog Posts
- Iredell Health Sees Major Benefits from an Outsourced SOC (Fortified Health Security)
- Thriving through digital change: the critical role of nurse leaders (Meditech)
- 5 key takeaways on the EHR experience in 2025 (Nordic)
- Navigating the Shift to Modern Infrastructure (Optimum Healthcare IT)
- Getting to ‘Yes’ with Hospital IT in a No-Spend Environment (Redox)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Follow on X, Bluesky, and LinkedIn.
Sponsorship information.
Contact us.














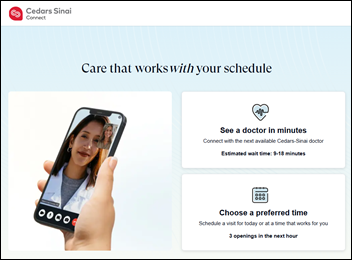




























One solution would be federal (or state) requirements; but more ideally health systems would view their digital patient tools as…