I haven’t been to Bostain in decades so I’m having who’s-on-first problems here. Is Deaconess who they’re merging with? So…
Monday Morning Update 7/25/22
Top News

Oracle EVP Mike Sicilia tells the US Senate Committee on Veterans’ Affairs that Oracle will move the VA’s Cerner implementation to the cloud and rewrite Cerner’s pharmacy module, completing both tasks within 6-9 months. Notes:
- Sicilia told the committee to consider that Oracle’s acquisition of Cerner gives VA, DoD, and the Coast Guard “a new, vastly more resourced technology partner overnight to augment Cerner.”
- Oracle says it will shift its top talent to working on the federal government’s Cerner challenges and is running the project from a war room that is staffed by senior Oracle engineers and developers.
- Sicilia says that Cerner, like its EHR competitors, is running on dated architecture using technology that is up to two decades old, making it hard to manage, support, and scale. Oracle says it will quickly move the Cerner application to a “modern, hyperscale cloud data center,” the same infrastructure that Oracle uses for critical industries in financial services and utilities. That conversion will be performed at no cost to the federal government.
- Oracle quickly fixed a database bug that caused 13 of the most recent 15 outages once the acquisition was completed and Oracle gained access to Cerner’s source code.
- The “unknown queue” was designed to account for human error rather than to mitigate it, so it will be redesigned.
- Sicilia says Oracle will “start over” with the Cerner pharmacy module, rebuilding it as a showcase of a cloud-optimized web application.
HIStalk Announcements and Requests
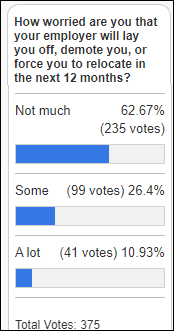
Most poll respondents aren’t too worried about negative job changes.
New poll to your right or here: Which conferences you plan to attend in person in the next 12 months? A sponsor asked if I planned to create a sponsor guide for conferences other than my usual HIMSS one, so the poll results will help me decide.
It’s an interesting phenomenon that so much of my LinkedIn feed is filled with “I’ve been laid off and need a job” posts, many of them from Olive because it laid off so many employees (450) at once. I’ve laid people off and been laid off myself and the double whammy is that not only are you out of a job, you are competing for a new position along with a bunch of your comparably skilled co-workers, most of them vastly preferring to avoid relocation. Maybe LinkedIn, combined with remote work options, will be effective in reducing the lost time between being marched out of one door (often virtually these days) and waiting for a new one to open.
Webinars
August 10 (Wednesday) 12:30 ET. “Navigating healthcare’s data quality challenge: An actionable discussion.” Sponsor: Intelligent Medical Objects. Presenters: Alastair Allen, CTO, Better; Dale Sanders, chief strategy officer, IMO. Achieving a consolidated patient record is challenging in an environment of hospital M&A, where EHR rip-and-replace projects are expensive and HIEs and FHIR connectivity haven’t significantly accelerated progress. The underlying problem is that systems don’t speak the same language due to a lack of comprehensive, persistent clinical terminology and data standards adoption. UK-based Better offers a unique, FHIR-based approach to integrating disparate EHR data. The presenters will explore how to improve clinical data quality and how interoperable information can be used to support patient safety, reimbursement, and population health management.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
Ascom acquires Appliware, a France-based developer of long-term care solutions for patient monitoring and alarming.
Elevance Health, the former Anthem, says in its earnings call that it will develop solutions that go beyond selling health insurance, touting its Carelon health services offering in which the company’s own providers will coordinate and provide patient care. Carelon offers services for behavioral health and value-based care and operates IngenioRx, an pharmacy benefits management and home delivery pharmacy company. ELV shares are up 20% in the past 12 months versus the Dow’s 8% loss, valuing the company at $110 billion.
Sales
- New York City Department of Health and Mental Hygiene will implement CareMesh’s national provider directory, which is available via FHIR APIs, file uploads, and web app.
- Hawaii’s Med-QUEST Division awards NTT Data a health analytics contract.
People

Divurgent hires Collin Jones, MBA (RedZone Technologies) as VP of finance.
Announcements and Implementations
Clearwater launches ClearConfidence, a managed services program covering cyber risk management and compliance.
An Optum consumer survey finds that providers fall short in offering online scheduling for both in-person and telehealth visits, particularly for younger adults who are not satisfied. Half of the respondents missed a scheduled healthcare appointment in the past year, one-third of those because they forgot, suggesting that appointment reminders could help reduce that number.
Three studies show that use of Bayesian Health’s AI technology for sepsis early warning reduced inpatient mortality by 18%. Founder and CEO Suchi Saria, PhD is an associate professor at Johns Hopkins University, where she also runs healthcare AI and engineering groups.
Other
WHO declares monkeypox as a global health emergency as world case counts rise to 16,000. US infections have risen from 200 to 3,000 in the past four weeks.

In the UK, IT and telephone system servers at one of NHS’s largest trusts go down as data center cooling systems fail to keep up with a record heat wave. The UK recorded its highest-ever temperature Tuesday of 104.5 degrees F. Clinicians are recording information by hand and asking patients to bring their own records to appointments. One doctor reports, “We are back to using paper and can’t see any existing electronic notes. We are needing to triage basic tests like blood tests and scans. There’s no access to results apart from over the phone, and of course the whole hospital is trying to use that line. Frankly, it’s a big patient safety issue and we haven’t been told how long it will take to fix. We are on divert for major specialist services such as cardiac, vascular, and ECMO.”
A widely cited 2006 research article on Alzheimer’s is found to contain what appears to be “shockingly blatant” examples of image tampering, leading to speculation that the authors may have altered data to support a hypothesis and thus sending researchers off on wild goose chases for years. In an interesting case of money driving the scientific process, the research was performed by scientists who were associated with the manufacturer of an Alzheimer’s drug, while the neuroscientist who reported the altered images was hired to do so by two other neuroscientists who were short sellers in shares of the same drug company. NIH spends $1.6 billion per year on research of amyloids for Alzheimer’s and scientists report that suggesting other causes of the condition to study pits them against the “amyloid mafia.” The only marketed drug in that category is Aduhelm, which earned the FDA widespread scientific scorn for approving a drug despite unimpressive research results.
Sponsor Updates

- Azara Healthcare staff train for the Pan-Mass Challenge, a bike race that will raise money for the Dana Farber Cancer Institute. Azara BKRS will ride in honor of colleague Heather Budd, who lost her battle with ovarian cancer last November.
- Northwest Clinics in the Netherlands adds Agfa HealthCare’s Rubee for AI platform to its Agfa enterprise imaging solution.
- GHX has grown its technology group by 12% in the last year, and plans to grown another 21% by the end of 2022.
- Baker Tilly releases a new Healthy Outcomes Podcast, “The rise of CCBHCs and the importance of quality of care measures in behavioral health.”
- Oracle Cerner releases a new podcast, “Improving health equality and equity through digital innovation.”
- Clinical Architecture Manager of Research & Strategy Jordan Rose becomes the co-vice chair of the HIMSS Chapter Advocacy Task Force.
- CloudWave appoints CompuGroup Medical CEO Derek Pickell to its board.
- ReMedi Health Solutions posts a white paper titled “How a Clinically-Driven Chart Preparation Process Improves the Continuum of Care.”
- RCx Rules publishes a case study titled “How US Dermatology Partners Achieved Their Highest Clean Claim Rates Despite Staffing Challenges.”
- Health Data Movers appoints former Bluetree CEO Jeremy Schwach to its Board of Directors.
- Lyniate announces a referral partnership with Solarity, which has developed an intelligent automation engine for easier use of clinical data.
- Nuance expands the availability of Dragon Medical One through the Microsoft Marketplace.
- Nordic Consulting achieves ISO 27001 certification.
- Pivot Point Consulting publishes a new case study, “A Multi-Pronged Success: AthenaOne EHR Support & Cures Act Education.”
- PeriGen earns the 2022 Frost & Sullivan Best Practices Product Leadership Award for its maternal and infant care solutions.
- PerfectServe publishes a case study, “Children’s Hospital & Medical Center Omaha: Centralizing Provider Scheduling Across an Enterprise.”
- MGMA’s podcast features Surescripts Senior Product Analyst Nicholas Chambers, “How Medical Practices Improve Medication Adherence and Patient Safety.”
- Vocera publishes a new white paper, “Smart, connected hospital framework.”
- Wolters Kluwer Health expands its Lippincott portfolio, using open science to support the higher velocity exchange of scientific findings.
Blog Posts
- Technology Best Practices for Stabilizing Healthcare Revenue and Operations (About)
- Key Steps for Successful Provider Credentialing (AdvancedMD)
- ECR2022: Thank you for joining us (Agfa HealthCare)
- Debunking 3 Myths About Offshoring Your Revenue Cycle Management (AGS Health)
- FHIR: Benefits and limitations for whole-person care (Arcadia)
- Staying the Course: 4 Ways to Reduce Patient Drop-Off in Rehab Therapy (Net Health)
- How is Your State Supporting 988 Crisis Response? (Bamboo Health)
- Getting Provider Billing Right: EHR Workflow and Optimization Tips (CereCore)
- Operational and Financial Tips for Starting a Private Practice – Part 1 (ChartLogic)
- CHIME – Always Dedicated to Serving Its Members (CHIME)
- Top 5 Spots to Check Out in Madison at the Epic UGM (Clearsense)
- 4 Steps to Increase Your Patient EHR Adoption (CTG)
- How Analytics Can Make a Difference in the Radiology Department (Dimensional Insight)
- Key Takeaway from the AHIP 2022 Conference (Divurgent)
- Cost & Utilization Explorer: Seeing, Understanding, Acting (EClinicalWorks)
- Strategies and Trends Impacting Your Urgent Care Billing (Experity)
- Telemedicine Policy Review: It’s Time for Non-Discriminatory Regulation and Reimbursement for Home Testing (EVisit)
- How FDB Leverages the CDC and FDA to Help Ensure Trusted Clinical Content (FDB)Working Toward High-Touch, Digital-First Access for All (Get Well)
- Incorporate Mentoring and See Your People Thrive (Optimum Healthcare IT)
- Advice from Supply Chain Experts: Four Best Practices for Smooth Leadership Transitions (GHX)
- 3 Ways a Neutral Zone Could Propel Personalized Medicine: Real-Time Example of Data Collaboration from Roche (Healthcare Triangle)
- HCCs under CMS and HHS: Can you spot the difference? (Intelligent Medical Objects)
- Memos from the Medhost CISO: Overcome Cyberattacks with Risk Assessments and Virtual CISO (vCISO) Services (Medhost)
- Supporting complex oncology care close to home (Meditech)
- 3 Reasons to Add Automated Prior Authorization to Your SaaS Solution (Myndshft)
- What is the Most Popular Behavioral Health Content in the NeuroFlow App? (NeuroFlow)
- Combining Cutting-Edge Technology and Deep Clinical Knowledge to Simplify Complexity in Healthcare Administration (Nym Health)
- Impact of patient activation across the ecosystem (Bravado Health)
- Unlocking Success in Palliative Care for Providers and Patients (Netsmart)
- Healthcare interoperability can put people first (Nordic)
- Expanding Access and Improving Outcomes with Measurement-Based Care (Owl)
- 3 Digital Health Trends Among Millenial and Gen Z Healthcare Consumers (PatientBond)
- Symplr Experts Guide on How to Engage Providers in Value Analysis (Symplr)
- What is Health Care Provider Credentialing? (PMD)
- How Healthcare Providers Can Tackle the Rising Costs of Services (Premier)
- How US Dermatology Partners Achieved Their Highest Clean Claim Rates Despite Staffing Challenges (RCxRules)
- In full view: Interoperability Best Practices for Specialty Labs Integrations (Redox)
- AHIP conference 2022: 3 top trends for health plans (Talkdesk)
- Transforming care delivery with modern healthcare technology (TigerConnect)
- 6 Fresh Ideas for Keeping Patients Engaged Between Appointments (WebPT)
- Homegrown, Out-of-the-Box, or Standardized Evidence-Based Clinical Decision Support: What’s Powering Your EHR? (Zynx Health)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.



Very interested to watch and see what Oracle thinks about they can do to stop the bleeding at Cerner. Hopefully, they will go back to the day of “see a snake and kill it attitude” meaning fix the problem the first time and don’t let it rear it’s ugly ahead again. Back in the day some people took ownership and worked the problem till it was resolved. Not just fixing it to work for the moment. Go back to “Show me” don’t just talk. Cmon Oracle kick butt and get Cerner moving forward like it should be. Epic is not any better it just knows how to answer the call from the client.
I am very interested in what problems you think that Epic is only temporarily papering over instead of fixing permanently.
Not sure what kind of reply you would like to have.. But here’s a shot at trying to give you something. I personally have a number of personal contacts at the user level of Epic, if you get to these nurse contacts in a hospital who have worked on both Cerner and Epic all have told me there is little to no difference in function. I worked for Cerner for 8 years back in late 1990. We knew we had the software and the technology that could make a difference and be the “superior” solution. The problem was and has now become too many managers at Cerner left “with the knowledge” and did not do a good job of mentoring their incumbent. Also, their were some very BIG egos at Cerner that forgot how to be client focused.
In my simple opinion, you have to use “Lean” type of management, that is Fix the root problem, obtain/retain people who have healthcare experience who can help lead development and function. It’s hard, but put your foot down and don’t let it up till it’s resolved and works efficiently.
I mean, I think you just responded with a lot of corporate speak without saying much at all. You said that “Not just fixing it to work for the moment” and then said “Epic is not any better”, so I asked what issues Epic is only fixing to work for the moment. If you don’t have specific examples, then I suppose that’s answer enough.
These lines caught my eye from the report and wondering if it is time to drink the kool-aid from Verona —
“Our Chairman and our CEO have made it clear that our top talent is to be shifted to working on the DoD/VA EHR system as our number one priority.”
and
“Oracle’s goals are two-fold and in this priority order:
1) To ensure patient safety above and beyond anything else; and
2) To deliver to the VA, DoD and Coast Guard the most modern, intuitive, performant and secure EHR in the world. We intend this system to be the gold standard.”
What are you doing for us Oracle/Cerner – the non-government hospitals who are using the software for last decades and expecting to be deliver the promised changes? Would we be just left to our own if all focus is on VA/DoD/CG?
I’d be honored to provide advisory services at no charge if you are interested. Cerner works just have to push them for results.
I’d be honored to provide advisory thoughts and services of so desired. (No cost). Cerner works. Why pay millions to convert.
“Cerner Works.”
…
VA has entered the chat.
Epic’s been working on migrating their code for nearly a decade. For Oracle to claim they can move all of Cerner into the cloud in 6-9 months including a full rewrite of a core application seems unlikely. If they manage to pull that off that would be an incredible pace to move an EHR product forward, especially considering what a patient safety minefield pharmacy modules are.
From a resource and strategic perspective it makes sense to me that Oracle would put their eggs in the federal contract basket, but color me surprised if they can deliver where Cerner hasn’t.
I will make an obvious statement here, but the biggest challenge isn’t moving the infrastructure and code base into the cloud (though that is a huge challenge). The biggest challenge is doing that while maintaining the integrity of the EHR as a whole and not disrupting your customer base while you are doing it. Epic has been at this for a while, but it is largely transparent to the health systems, at least to the end-users, which is a feat in itself.
What I suspect Cerner/Oracle is going to do is treat the VA as a separate system altogether. I bet they will move quickly to migrate some of the infrastructure to the cloud, but they will bifurcate their offerings and do it for the VA first and only, and then be left figuring out how to scale that to all other existing systems at a later date. Hell, they might even call this a new product, and force other health systems to pay for an upgrade to get it. Monetize their failures with the VA.
It’s not unlikely, IMHO, it’s impossible.
Here’s what I’d do to hit such an aggressive target. You migrate the entire Cerner system to the cloud, making the absolute minimum number of changes to the base code, as possible. It would be more acceptable to add something to the system than to change something.
Then, if something breaks? You have a short list of things to look at. A very short list!
Later, if you want to, you can look at redeveloping some of the core Cerner code. But first you get the system to the cloud, and hope like heck that works.
In this light, EVP Mike Sicilia’s comments about redeveloping the Pharmacy module? It really begins to stand out. Oracle may use Pharmacy as a proving ground, to see if it actually makes sense to perform complete redesigns for other modules.
The issue isn’t whether ground-up rewrites are beneficial, because they usually are. The issue is, are they worth the cost, the time and effort? And rewrites usually gain significant benefits from the experience of the first go-round. It’s not just about the headline reason why you did them.
in all this commentary, I’m not sure what “migrate to the cloud” actually means or is intended to fix. “The Cloud” just means that the servers are in someone else’s data center instead of yours. The majority of Cerner’s clients are already “in the cloud” as the servers are in Lee’s Summit, MO instead of in the basement of those health systems. If the problems facing the VA and other Cerner clients were network downtimes, latency, hitting CPU bottlenecks, running out of storage, etc…then sure, “move to a better cloud” would be a good solution for those problems.
If “The Cloud” means swapping out different underlying platform technologies, not sure that does it either — you could move the “unknown queue” from what is probably IBM’s message queue platform today to an Oracle version of that, but if you don’t change the underlying application, workflow, and business logic, you just have a faster, more stable way of dumping unhandled exceptions.
If “The Cloud” means rewriting the software to be a web application that can be updated with biweekly releases, that’s what should be done — but that’s a wholesale rewrite of the product.
Beyond impossible, but laughable. With decades of EHR implementation under my belt, I can feel the hot air from DC to my home office. I’m no techy (and have zero Cerner experience), but unless you can just “plunk” the current version and put it into a cloud, with no changes, I think 9 months is slightly doable. Will need a few months alone to test, a few months to figure out migration, and then ensure security is correct for all users, everywhere, to access new cloud… So a redesign, to actually function as users need it to, would take at least 2 years. He’s obviously never been in design/build sessions with actual doctors, nurses and pharmacists to hear the minutiae and needs that all must come together to ensure patient safety and hospital efficiency.
Yup. That 6 to 9 month timeline is definitely a significant over-commitment. If they make it, I won’t be surprised. I will be astonished.
I am just amazed at all the ways the guy slams Cerner. Bad systems architecture, bad design, bad user interface, etc. I am not surprised it’s that bad… just that someone would say it publicly.
Feel free to let me know I’m missing something but when I read the actual transcript I read it as they are just moving the environment/software to a Oracle Cloud, not a web migration type rewrite. Just moving from Cerner data center to an Oracle data center in 6-9 months.
The following section appears to address how they’ll catch up to Epic’s web migration that I think you were confusing with the above. Somewhat down the road and within the current contract envelope is the timeline. No real timeline…. 🙂 I don’t know what the contract envelope is but it is more than 6-9 months….especially at the current 2 steps forward, 1 step back approach.
“Oracle plans to
invest substantial resources to develop and deploy modern stateless web applications – with a
modern user interface – to all Cerner customers, including the VA. This is somewhat down the
road but I want to emphasize that Oracle’s acquisition of Cerner will vastly accelerate this
process and make the VA the gold standard of EHR systems globally. Again, this technology
will be provided to the DoD, Coast Guard, and VA within the current contract envelope.”
Oracle’s EVP said this: “My inclination with the pharmacy module is to start over and make pharmacy an example – a showpiece – of what is to come. We now have VA’s requirements, and we intend to use a new model of collaborative development where we will bring developers out to the users and jointly define parameters, metrics, and workflows. In fact, we plan to send a substantial number of military veterans who currently work as developers at Oracle to work with VA pharmacists, clinicians and other end-users to assist in this process. We intend to develop this as a modern, stateless web application, which simply means it is built for use in the cloud with the associated scalability and reliability you expect from popular web sites today. With this development, all the modern mobile, social, and analytical features will be built in”
Rx 9 months? Sure…and while you wait, I have a bridge you can have cheap!
Any comments on why Defense Health Agency is rolling out Cerner while VHA is stumbling so badly? Is this politics or are the implementations that different and especially that differently managed?
Bill, the DHA is stumbling just as badly (“stumbling is generous”) but there’s arguably oversight fatigue. This is the executive summary paragraph from the most recent DHMSM annual report:
Military Health System (MHS) GENESIS is operationally effective for basic operations in conventional clinics, but not for certain specialty clinics and business areas. One of the configuration management initiatives, called “Pay It Forward,” demonstrated potential for improving MHS GENESIS operational suitability. While training remains an area of major concern, with 72 percent of respondents rating it poorly, hands-on practice in a mock environment also demonstrated potential to improve MHS GENESIS operational suitability. Despite ongoing cybersecurity improvements, MHS GENESIS is not yet survivable in a cyber-contested environment.
Full report here: https://www.dote.osd.mil/Portals/97/pub/reports/FY2021/dod/2021dhmsm.pdf?ver=vUx84-fEtar0GOIyHX9YDA%3d%3d
You also have the comforting assurance of Oracle’s top government man:
“Much of the functionality is working.”
Have a little confidence, I’m sure they’re all over it!
https://www.youtube.com/watch?v=Fdjf4lMmiiI
Start reading some of the MilTwitter- new system is getting blamed for recruiting issues as integration into other instances and interfaces into other systems reveals potential recruit’s healthcare issues, some records going back to birth. Military is having issues processing the information, lot of potential recruits getting rejected, targets falling way short.