I think you are missing the point. When you are dealing with a new type of disease/tumor, most average doctors…
News 1/29/20
Top News

Allscripts-owned Practice Fusion accepted a $1 million kickback from (presumably) OxyContin manufacturer Purdue Pharma in return for allowing the drug maker’s marketing department to design EHR decision support rules that encouraged overprescribing of its opioid product, according to Department of Justice details about Practice Fusion’s previously announced $145 million settlement.
Practice Fusion also made similar arrangements with drug companies involving 13 other CDS rules.
DOJ also accused the company of allowing its users to inappropriately collect Meaningful Use payments by using its EHR, ONC certification of which was fraudulently obtained.
Reader Comments

From Timeliner: “Re: Practice Fusion. Previously fired CEO Ryan Howard says via Twitter that selling opioid-friendly decision support rules didn’t happen under his watch from 2005-2015.” The Department of Justice and the company’s own settlement indicate otherwise. I’ll take a refreshing counterpoint to the argument that Practice Fusion was unethical in working with Purdue Pharma to push OxyContin prescribing via EHR nudges, maintaining that it shouldn’t be much of a surprise when a struggling company with outsized IPO ambitions slides its hand shamelessly into the deepest of pockets:
- Purdue executives were scumbags who were happy to turn much of the population into opioid addicts for profit.
- Many of us had low opinions of Practice Fusion’s management, business practices, and Silicon Valley mindset in which patients were incidental to profits. Although, healthcare-specific ethical considerations aside, you could argue that businesses are supposed to do exactly that and are rewarded for doing so. We just unreasonably expect healthcare to be voluntarily different.
- Practice Fusion was clear in stating from the beginning that the point of its free EHR was a drug company advertising platform, i.e. it was paid to get prescribers to use a company’s drugs in situations where their own conclusions suggested they shouldn’t. As the old saying goes, if you aren’t paying for it, then you are the product.
- Purdue had money to burn and thus the $1 million payment to Practice Fusion was a rounding error and was probably not studied carefully for potential return on investment. There’s a high net present value in creating a loyal customer, whether the product is opioids or something else.
- DOJ termed the arrangement as “illegal kickbacks,” but I might make the same accusation against medical journals that accept drug company advertising. “Kickback” usually means sharing in the proceeds of illicit activity, and I’m not sure that selling fixed-cost advertising in any form fits that definition.
- If you believe Ryan Howard’s claim of innocence, then the blame must rest on his CEO successor Tom Langan, a former drug company sales rep, medical magazine ad salesperson, and president of a drug marketing company. With the Allscripts acquisition of Practice Fusion, he’s now CEO of the Allscripts Veradigm payor and life sciences analytics business, which among other activities helps drug companies “reach specific HCPs [providers] of interest within their point-of-care workflow through dynamic media solutions,” which I assume means pushing drug company ads at prescribers. Veradigm also sells Allscripts-held de-identified patient data to drug companies via Komodo Health.
- Or perhaps you believe that Allscripts knew that DOJ was coming for Practice Fusion no matter what and signed off on the settlement knowing that its allegations were untrue or misstated just to avoid future problems. The current administration seems intent on punishing EHR vendors for the $38 billion spent to get their products used and maybe Allscripts saw the writing on the wall along with the opportunity to throw previous management under the bus.
- The reported reduction in the Allscripts offer price for Practice Fusion nearly exactly matches the settlement amount, which Allscripts obviously knew about from doing its due diligence. Allscripts says it expects to recover some of the money from unidentified third parties, although the possibility of lawsuits can’t be ruled out.
- Practice Fusion’s EHR certification was awarded by ONC-Authorized Certification Body Drummond Group, which also awarded certification to EClinicalWorks and Greenway Health under similarly phony circumstances, resulting in DOJ settlements of $155 million and $57 million, respectively.
- The real question is how many doctors accepted the nudge of prescribing opioids inappropriately since the DOJ settlement only said that “numerous prescriptions” were issued after the doctor received the loaded CDS guidance. We don’t know how many of those prescriptions were inappropriate or whether those prescribers were already prescribing outside of medical guidelines even in the absence of EHR influence, especially since Practice Fusion’s target market was small practices looking for a Meaningful Use payday with minimal commitment.
- Allscripts has claimed that other companies have behaved similarly and the DOJ settlement requires the company to report the competitors that are doing so. I wouldn’t be surprised if other EHR vendors aren’t called out soon given the trend of clawing back a small percentage of Meaningful Use money by going after vendors rather than providers.
From Goody Three Shoes: “Re: Epic’s problems with the interoperability rule. You didn’t give an opinion.” My thoughts:
- Epic is correct that allowing patients – who are just as clueless as any other consumer in regularly exposing their own information in return for immediate electronic gratification – will create a Facebook-like situation in which companies that have otherwise been blocked from sketchy activities that require patient data are cheering at the opening of an unregulated back door.
- As a counterpoint, patient advocates maintain correctly that it should be the patient’s choice, although the skeptic in me keeps remembering that nobody ever went broke underestimating the intelligence of the American people.
- Bottom line: we as a nation have fallen behind our European counterparts that have adopted wide-ranging consumer data protection, so we’re expecting HIPAA – which was passed in the pre-Internet year of 1996 – to protect health data even though its loopholes don’t even ensure that providers, much less anyone else, will find it burdensome in their pursuit of profitable activities.
- I say pass HHS’s rules instead of awaiting perfection, then see what happens and act accordingly when a few big scandals come to light that might belatedly send us to a much-needed, GDPR-like law.
- Epic placed itself in an awkward position when it registered its concerns late in the legislative process, failed to anticipate public skepticism of its motivations as a huge technology company, and was hurt by its PR-averse practices that left it red-faced when mass media uncovered its letter to customer CEOs that urged them to oppose regulations that would benefit their own organizations as well (health systems, as the chief information blockers, have every reason to love the status quo). Epic’s objections are pretty much the same as AMA’s except Epic isn’t complaining about excessive EHR vendor connectivity fees, but only Epic is taking the black eye.
From Justin Time: “Re: health IT article. Does this look like a paid placement to you?” I’ll only say broadly that I dismiss any article or review about a company, product, or person that doesn’t include at least one negative statement. That covers an additional situation beyond paid collusion, that being journalistic incompetence.
Webinars
January 29 (Wednesday) 2:00 ET. “State of the Health IT Industry 2020.” Sponsor: Medicomp Systems. Presenters from Medicomp Systems: Dave Lareau, CEO; Jay Anders, MD, MS, chief medical officer; Dan Gainer, CTO; Toni Laracuente, CNO. Despite widespread adoption of EHRs, healthcare professionals struggle with several unresolved systemic challenges, including the lack of EHR usability, limited interoperability between disparate systems, new quality reporting initiatives that create administrative burdens, and escalating levels of physician burnout. Join the webinar to learn how enterprises can address current industry roadblocks with existing market solutions and fix health IT’s biggest challenges.
Previous webinars are on our YouTube channel. Contact Lorre to present your own
Acquisitions, Funding, Business, and Stock

The private equity owner of wearables-powered employee wellness vendor VirginPulse reportedly is preparing to sell the company for up to $2 billion. The company was founded in 2004 by Sir Richard Branson’s Virgin Group and has since acquired RedBrick, Blue Mesa Health, SimplyWell, and Preventure.

The private equity owner of imaging and radiology workflow systems vendor Intelerad sells a majority stake in the company to investment fund manager Hg Capital, which acquired the Rhapsody integration business from Orion Health Group in October 2018. Intelerad had been looking for a buyer since mid-November.
Sales
- CommonSpirit Health chooses Premier for clinically integrated supply chain management.
People

Access promotes Cody Strate to VP of marketing.

Brian Taylor (MCG Health) joins First Databank as VP of sales.

PatientPing hires Jitin Asnaani (CommonWell Health Alliance) as VP of strategic partnerships.

Industry long-timer Joe Carey, who held executive roles at Allscripts and Livongo, has died at 62.
Announcements and Implementations
Surescripts releases a Specialty Patient Enrollment service that automates the specialty drug prescribing process. Several EHR vendors, including Cerner, will implement it.
Northwell Health develops a premature infant growth chart application, with SMART on FHIR and InterSystems HealthShare making up the underpinnings. The health system says it took just six weeks to develop the app.
Government and Politics
A Health Affairs blog post notes the problems of the Indian Health Service in its continuing use of its obsolete RPMS EHR and enterprise system, which relies on the VA’s VistA platform that is being replaced with Cerner:
- IHS has received its first-ever IHS health IT budget item ($25 million in FY2020) to determine how it will proceed with the VA rug pulled from under it.
- IHS facilities experience perpetual staff shortages, including IT, and often don’t even have Internet or Wi-Fi access.
- IHS has followed the VA’s model of customizing each instance of RPMS, making it hard to support and train users.
- Facility customization prevents IHS facilities from exchanging patient information with each other.
- Patients lack the ability to view or download their own data.
- IHS IT is underfunded and received no additional budget to comply with federal initiatives such as Meaningful Use and ICD-10.
- The VA and DoD were given many billions to move to Cerner, but IHS has received nothing versus its estimate of $3 billion needed over 10 years to modernize its health IT platforms.
- A November 2019 report from IHS IT recommended that the federal government honor the federal-Tribal relationship, establish governance, create a patient portal, study end user needs, provide interoperability among IHS facilities, improve analytics, modernize infrastructure, and strength security.
Privacy and Security
TechCrunch notifies LabCorp that a since-fixed website vulnerability left its patient CRM system and at least 10,000 documents containing patient information exposed to Internet searches.
Other
Epic explains its opposition to HHS’s proposed interoperability rules, saying that EHR vendors would be forced to send data to any app of a patient’s choosing and many of them have been found to sell or misuse patient data. The company is also concerned that some parts of the medical record, such as the family history, contain the information of people other than the patient themselves who did not necessarily give their permission.
Cerner expresses its support for HHS’s proposed interoperability rules.
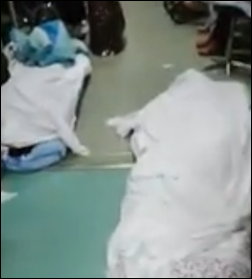
A New York Times article questions how China will deal with a potentially huge number of coronavirus patients when its hospital-centric healthcare system is already too overwhelmed to meet even basic healthcare needs. Experts question whether patients are even being tested for the virus before being sent home to spread it to others. Videos show chaotic hospital hallways crammed full of patients, both living and dead. The government says it will complete construction of a new 1,000-bed coronavirus hospital within 10 days and another 1,300-bed hospital in two weeks, using rapid response plans developed during the SARS epidemic of 2003.
A Lancet editorial warns that despite headlines proclaiming AI’s value in analyzing mammogram and other diagnostic images, AI doesn’t work well in diagnosing cancer in real world settings, with just 14 of 20,000 studies justifying possible clinical use. The authors call for clinical trials and making sure that the systems are trained on diverse patient populations for broad applicability. They also question whether proprietary algorithms, such as those developed by Google Health, can be trusted without external validation.
Good timing related to the Practice Fusion settlement news: a JAMA Network-published study finds that ED doctors prescribed fewer doses of opioids for discharged patients when the default prescription quantities were reduced. Patients were ordered 0.19 tablets more for each one-tablet increase in the default prescription quantity.
Weird News Andy says the BioFabrication Facility will indeed be the BFF for organ recipients. A commercial microgravity company 3D prints human heart cells on the International Space Station that were then returned to Earth in a SpaceX capsule, with executives concluding that “our BFF has the potential to transform human healthcare in ways not previously possible” in creating an entirely space-based industry.
Sponsor Updates
- Imat Solutions announces that its Clinical Reports module has achieved NCQA ECQM certification.
- AdvancedMD publishes a new e-guide, “7 Key selection criteria for outsourcing RCM for VBC.”
- Artifact Health will exhibit at the Florida ACDIS Quarterly Meeting February 1 in Jacksonville, FL.
- Elsevier creates a free information center to bring together the latest clinical research on the Novel Coronavirus 2019-nCoV.
- CI Security’s Drex DeFord will present at the AHA Rural Health Care Leadership Conference February 2 in Phoenix.
- The local paper covers the development of the new, 15-acre CoverMyMeds campus in Columbus, Ohio.
Blog Posts
- OR Delays Cost Hospitals Time and Money (Access)
- 2019 Product & Technology Wrap-up Positive Changes (AdvancedMD)
- Susy Liem: My First 30 Days at Avaya (Avaya)
- Health IT Predictions for 2020 (Datica)
- Easing Physician Burnout: Helping Physicians be Physicians Again (ChartLogic)
- Alarm Fatigue in Nursing (Spok)
- Webinar recap: How to reduce the burden of quality reporting (Nordic)
- Third Party Risk Management for Healthcare Cybersecurity (CI Security)
- How ACOs are Taking Advantage of Home Health (Collective Medical)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.





Re: AI – Maybe AI is not be sufficiently advanced (yet) to detect cancer, but it was good enough to detect the coronavirus outbreak before the official announcements from the CDC and the WHO, and despite the initial official information blackout:
https://www.wired.com/story/ai-epidemiologist-wuhan-public-health-warnings/
Great , rational analysis of the PracticeFusion settlement and Epic’s position on interoperability. Too bad “evidence-based policy” is an oxymoron in today’s political climate.
“…nobody ever went broke underestimating the intelligence of the American people.”
Quote of the day! Love it.
It’s from the cynical H.L. Mencken (1880-1956), who coined these gems as well:
“Democracy is a pathetic belief in the collective wisdom of individual ignorance.”
“Under democracy, one party always devotes its chief energies to trying to prove that the other party is unfit to rule. Both commonly succeed, and are right.”
“For every complex problem there is an answer that is clear, simple, and wrong”.
“It is hard to believe that a man is telling the truth when you know that you would lie if you were in his place.”
“Before a man speaks it is always safe to assume that he is a fool. After he speaks, it is seldom necessary to assume it.”
Wow; I have a new favourite cynic 🙂
Do you think they fire stopped every wire penetration in the new Chinese hospital?