Monday Morning Update 1/15/24
Top News
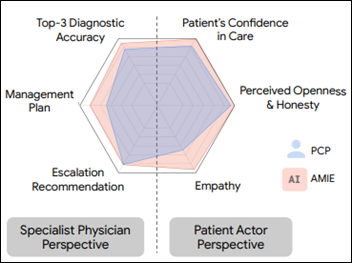
A Google-created AI system called AMIE that was optimized for diagnostic dialog outperforms primary care doctors in synchronous text chat with patient actors. The authors warn that while this isn’t representative of clinical practice and thus places clinicians at a disadvantage to AI, the accomplishment is still a milestone in developing conversational diagnostic AI.
The evaluation criteria included history-taking performance, diagnostic accuracy, management reasoning, communication skills, and empathy.
The authors observe that history-taking and diagnostic dialog is dependent on context and requires a high level of clinician skill.
The tool was trained on medical licensing exam questions, real-life medical summaries, and audio transcripts from 100,000 medical conversations. It was further trained and refined by using self-play, where AI improves its performance by playing against itself and analyzing which of its approaches were successful.
Reader Comments
From A Beautiful Mind: “Re: Amazon. Your post about Health Conditions got me thinking about previous Amazon healthcare forays such as HealthLake, One Medical, etc. Do you speculate that they are throwing a lot of darts to see which ones stick, or is there a John Nash-like team in Seattle piecing together the chaos for ultimate world domination, and oh yeah, improving care and lowering costs?” Amazon is smarter than I, but I don’t understand its healthcare plan. The company doesn’t always hit healthcare home runs (see: Amazon Care, Haven, and Halo) but it swings a mighty bat and learns from failure. It hasn’t done much with online pharmacy PillPack, and buzz about its “all the pills you take for $5 per month” RxPass died down pretty quickly after it was announced a year ago. It paid $4 billion for money-losing primary care concierge practice One Medical, with few changes except to offer Prime members a discount on joining One Medical, which still bills insurance traditionally and is now is exposed to Amazon-recruited members who are older and less affluent that One Medical’s former client base. Amazon’s recent offerings seem to focus on charging to advertise third-party healthcare businesses. Healthcare is a financially appealing vertical, but is notoriously hard for even big-name outsiders to penetrate due to billing complexity; a hellish regulatory environment; the local and trusted presence of big health systems and national drug chains where Amazon is to many just a website or app that often sells offshore-sourced junk using phony reviews, and the challenge of scaling without killing someone. I think of Amazon as a company that makes money from selling ads, fulfillment services, and AWS with zero personal touch, which doesn’t suggest a broadly disruptive role in healthcare.
From Y2K11 Maverick: “Re: HIStalk. I last said this 10 years ago, but it has remained true. Rarely does a week go by that 1) I don’t learn something new by reading HISTalk updates and/or 2) I pass along something from your posts that my colleagues hadn’t seen before. THANK YOU for all that you’ve done, do and (hopefully) continue to do for us schmoes who are just trying to keep up! Loyal listener since 2011!” Thanks.
From JD: “Re: Billy Idol at ViVE. Your mention reminded me of John Lydon, aka Johnny Rotten of the Sex Pistols, who was his wife’s caregiver.” The 67-year-old punker was a full-time caregiver of Nora Foster, his wife of 44 years, for nearly 15 years until she died of Alzheimer’s in April 2023 at 80 years old. He said in an interview just before she died, “We know that she’s going to slowly deteriorate into something catastrophic, and then death. But she will enjoy every step of it, and I’m here to make sure of that because she’d do the same for me.”
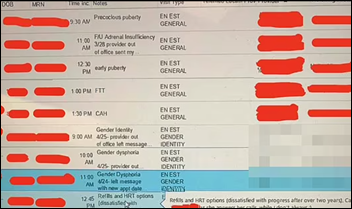
From JustScratchingMyHead: “Re: the Texas surgeon sharing gender-affirming care records. While technically he did redact the information, it still seems procedurally not correct and I would think the hospital would have some type of policy about screenshots being taken and sent externally. What happens when the next provider sends the information without proper redaction or none at all?” Ethan Haim, MD graduated from his Baylor surgical residency the day that HHS knocked on his door. He was an anonymous whistleblower until June 2023 and has moved on to Hunt Regional Healthcare as a general surgeon. The hospital’s bigger beef with him beyond screenshots would have been his efforts to get them in trouble with the state. He likens transgender interventions for children to COVID, arguing that both involve scant peer-reviewed medical evidence and the institutional censorship of those who question it.
HIStalk Announcements and Requests
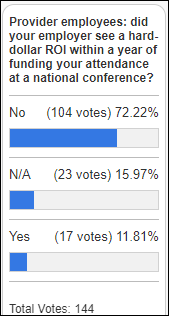
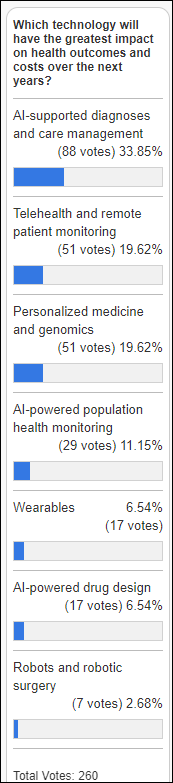
Provider poll respondents aren’t confident that their employer-paid conference attendance generates ROI. However, commenters add that attendance has value beyond immediate ROI, such as gaining knowledge, networking, and recruiting.
New poll to your right or here, for provider employees: which is your preferred medium to learn what a vendor does? This is in response to user comments. I’ll admit that while I’m critical of TL;DR types who can’t read more than two consecutive sentences without blaming the author with indignation rather than embarrassment for their phone-stunted attention span, I’m similar with videos, however – people who host them and love themselves excessively sometimes can’t shut up and let their guests speak. I f a video can’t tell me something useful in the first 30 seconds (or a text article in three sentences), the situation isn’t likely to improve and I move on.
Your to-dos for supporting what I do:
- Join my spam-free mailing list.
- Connect on LinkedIn and join Dann’s HIStalk Fan Club so that I see your posts and job changes.
- Tell my sponsors, or potential ones, that you value their support.
- Share news, rumors, and intriguing insights.
Webinars
January 19 (Friday) 1 ET. “Unlocking Reliable Clinical Data: Real-World Success Stories.” Sponsor: DrFirst. Presenters: Alistair Erskine, MD, MBA, CIO/CDO, Emory Healthcare; Jason Hill, MD, MMM, associate CMIO, Ochsner Health; Colin Banas, MD, MHA, chief medical officer, DrFirst. Health system leaders will describe how they are empowering clinicians with reliable patient data while minimizing workflow friction within Epic. They will offer real-world experience and tips on how to deliver the best possible medication history data to clinicians at the point of care, use clinical-grade AI to infer and normalize prescription instructions in Epic, and encourage patient adherence to medication therapies for optimal outcomes.
January 24 (Wednesday) noon ET. “Medication Management Redefined.” Sponsor: DrFirst. Presenters: Nick Barger, PharmD, VP of product, DrFirst; Caleb Dunn, PharmD, MS, senior product manager, DrFirst. Clinical workflow experts will paint a reimagined vision for e-prescribing that offers enhanced patient adherence, customizable clinical support, intelligent pharmacy logic, and data integrity and safety. Join this first chapter of an ongoing conversation about what medication management should be, how to deliver greater benefits today, and how to prepare for the future. Elevating your solution and customer benefits isn’t as hard, scary, or economically challenging as you may think.
Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
Sales
- Outpatient rehab provider Ability KC choses Netsmart’s TheraOffice EHR/PM.
Announcements and Implementations
Oracle moves its Health Summit to Nashville and pushes it back from February to April. Tennessee offered Oracle $175 million in incentives to build a $1.4 billion campus in Nashville that will likely have a significant Oracle Health presence. The company’s Oracle Health Conference, the former Cerner Health Conference, was held in Las Vegas in September 2023.
Government and Politics

The chairs of the Kansas senate commerce and house judiciary committees ask Governor Laura Kelly to explain why the Department for Children and Families awarded $7.7 million of a $18 million federal social services grant to software vendor Unite Us. They question why so much of the money will be sent to an out-of-state company instead of being used to support local social service programs.
A Bloomberg article on the effects of significant national relocation on elections highlights Epic, whose large headcount and 3,000 hires in 2023 are mostly young and college educated.
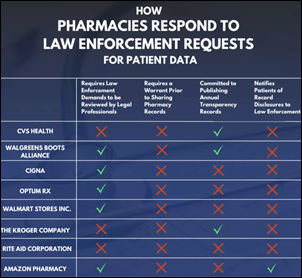
A Senate subcommittee reviews finds that national drugstore chains don’t require a warrant to provide law enforcement with the patient records they request for whatever reason, with Sen. Ron Wyden (D-OR) calling for HHS to update HIPAA to require pharmacies to insist on a warrant before disclosure in response to regulatory and law enforcement records requests.
Privacy and Security
A law firm that specializes in business security incidents is itself hit by hackers, exposing the identity, medical, and insurance information of 637,000 people that it had collected from its security incident clients.
Other
Former Olympic gymnast Mary Lou Retton was uninsured for her month-long hospital stay for pneumonia, for which she blamed pre-existing conditions and lack of affordable premiums. Either she’s not telling the whole story or she is unaware of Affordable Care Act plans that are legally required to cover pre-existing conditions and extend premium subsidies based on income. The 55-year-old Retton says she has since obtained insurance, but didn’t say if she paid for it from the $460,000 her four daughters raised for her via social media. She declines to name the hospital.
Sponsor Updates
- Meditech reports record international growth for its Expanse EHR in 2023.
- Nym will exhibit at the HFMA Western Region Symposium January 21-24 in Las Vegas.
- Optimum Healthcare IT announces that it has been named a Workday Staffing Partner.
- Verato publishes a new e-book, “How to overcome HHS identity management challenges.”
Blog Posts
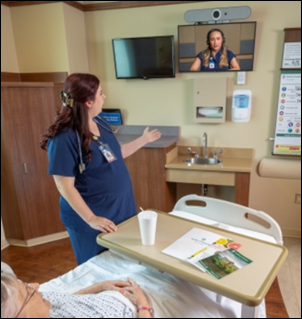
- To sit or not to sit: How a chair can affect patient satisfaction (Nordic)
- The Power of Listening: Three key components of an effective change management program – Part 1 (Qgenda)
- How to Simplify Affordability in the Specialty Medication Workflow (RxLightning)
- Not Exactly a Crystal Ball, but 8 Healthcare Trends to Watch for in 2024 (Symplr)
- Oklahoma Supports Family Caregivers with Groundbreaking “Caring for Caregivers Act” (Trualta)
- 5 most unproductive touches in the healthcare RCM process (Waystar)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.














































Yes, but why is Epic "the best in the industry for many healthcare systems"? And sure, it's a complex software…