News 8/23/17
Top News
CliniComp files a bid protest lawsuit against the VA, saying that it improperly issued Cerner a no-bid contract for an EHR that will replace VistA. CliniComp’s systems are used in several VA hospitals.
CliniComp prevailed in a similar 2014 lawsuit in which it protested that the VA’s selection process was flawed when it awarded a $4.5 million bid to Picis instead of low bidder CliniComp.
The White House took credit for the VA’s surprise selection of Cerner, apparently believing that interoperability with the Department of Defense will be easier if the organizations use the same vendor’s system.
Reader Comments
From Givenchy: “Re: Athenahealth. Their community hospital webpage is misleading customers by claiming financial success for a time period in which it had no hospital customers.” I’m not clear from Athenahealth’s community hospitals web page if the claimed improvement in financial and quality measures is specific to hospitals, but I’m thinking not since, as you observed, the footnote cites customer data “based on a weighted average for Athenahealth clients with valid pre-Athenahealth benchmark data that had their 15 month anniversary with Athenahealth between January 1, 2010, and October 31, 2013.” Athena didn’t acquire RazorInsights and its small-hospital system until early 2015. They also could be referring to hospital customers that use its other systems in their ambulatory operations.
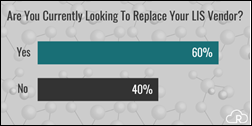
From Lab Animal: “Re: best-of-breed LIS vendors. I left one of those companies to work on Epic’s clinical solutions in a major medical center. Beaker is now competitive enough to convince enterprise customers to convert. I have seen the advantages of integrated solutions. It’s not a new trend, though – my peers and I are contacted several times each week by recruiters looking for people experienced on the LIS I previously worked on to keep the lights on while the LIS team goes to Epic training and builds Beaker. The best-of-breed writing has been on the wall for years.” Sunquest and SCC (but not so much Orchard from what I can tell) are trying to find runway in the genetics information system business to offset their significant customer losses due to LIS domination by Epic and Cerner. Sunquest has also smartly branched out into lab instrument interface software, specialty pathology applications, and clinician collaboration, although I haven’t seen numbers of how much profit those products contribute or whether revenue is growing significantly. You don’t want to be a best-of-breed vendor these days unless Cerner and Epic don’t offer your particular product (yet, anyway, since Epic’s selling the industry-leading LIS also seemed unlikely a few years ago).
From Boomer: “Re: Medhost. Heard a rumor they are being considered for acquisition by a physician systems vendor that might be interested in entering the hospital market. They are strong with chains like Community Health Systems, which is selling off a bunch of its hospitals.” Unverified.
From Leftcoaster: “Re: Portland Adventist’s partnership with OHSU and scheduled conversion to Epic. It’s at risk due to a high-profile infant death lawsuit that could place OHSU at risk if the partnership occurs.”
From Failed Merger: “Re: Presence Health merging into Ascension Amita. That should be interesting as Ascension is on Cerner, the Resurrection portion of Presence is on Epic, and the Provena part is on Meditech. At one point, Adventist Midwest was McKesson.” Thanks to Turnaround Failure, who tipped me off over the weekend of the merger rumor that I ran in the Monday Morning Update. Ascension proposes to acquire the struggling, 11-hospital Presence Health and operate it within its Amita Health joint venture that includes Adventist Midwest Health, pending regulatory approval.

Lloyd McKenzie, who is a co-chair of HL7’s FHIR Management Group, provided some background on the FHIR specifications that a reader asked about last week.
There are two mechanisms for sharing FHIR specs. The first is a computable format that uses FHIR itself. It allows sharing system capabilities and expectations; rules around data elements, such as what elements are required, optional, or conditional; what codes are allowed for use for which elements; etc. That format is intended to support automated testing, comparison of system capabilities, software configuration, etc. It can also be rendered for human review. The computable “resource” format is formally defined as part of the FHIR specification. HL7 strongly encourages implementers to expose their capabilities using this format.
The second mechanism is the human-readable rendering of FHIR implementation guides. Typically this is an HTML representation with hyperlinks back to the FHIR specification. HL7 produces tooling to support generating such human-readable rendered views, but does not mandate it. The tooling is also quite flexible, allowing content to be organized in a variety of ways, so it’s certainly possible to find interface documentation of varying quality and expressiveness that is generated using the same tooling. As well, the HL7-maintained IG publisher is not the only set of tooling available. HL7 developed and maintains it because it also needs a way to publish implementation guides and we’re happy for other organizations and implementers to make use of it. Best practices for producing human-readable FHIR interface documentation are far from settled, so expect the tooling to continue to evolve based on implementer feedback.
HIStalk Announcements and Requests

I questioned as a card-carrying cynic why so many people – many of them ignorant or even dismissive of science and math – would rearrange their lives to watch the moon block the sun for a short period, much like sticking your thumb into the air and obscuring the celestial fireball yourself for 10 seconds of child-like fun. I’ve heard that airlines weren’t able to meet the demand for flying in and out of certain (and hopefully cloud-free) parts of the country and hotels there were charging extortionate room rates for out-of-towners. I’m pretty sure that quite a few fad-following science haters who don’t vaccinate their kids, who don’t think climate change is real, or who argue passionately that the earth is actually flat still confidently uttered “totality” at every opportunity. I took a hooky break and went to the golf course — I’ve never played an actual round of golf, but I like to blast balls unskillfully on the driving range, putt on the practice green while quietly imploring others nearby to “miss it, Noonan,” and then have a burger and beer afterward, which seem to be the best parts of the game anyway – and nobody was paying the slightest attention to the sky or fishing in their golf bag for a flashlight. At least it got folks looking up from their phones long enough to share a rare in-person experience and it gave long-faded singer Bonnie Tyler a chance to sing her 34-year-old hit that has nothing at all to do with an actual eclipse (the writer, who isn’t Bonnie, says it’s about vampire love).
Webinars
September 13 (Wednesday) 1:30 ET. “How Data Democratization Drives Enterprise-wide Clinical Process Improvement.” Sponsored by: LogicStream Health. Presenter: Katy Jones, program director of clinical support, Providence Health & Services. Providence is demonstrating positive measurable results in quality, outcomes, and efficiency by implementing clinical process improvement solutions in arming operational and clinical stakeholders with unlocked EHR data. Providence’s army of process engineers use their self-service access to answer questions immediately instead of waiting for reports to be written and double checked for possibly inaccurate information. The presenter will describe practical applications that include antibiotic stewardship, hospital-acquired infections, and comprehensive knowledge management.
Previous webinars are on our YouTube channel. Contact Lorre for information on webinar services.
Acquisitions, Funding, Business, and Stock
Vestar Capital Partners acquires health plan network management software vendor Quest Analytics.
Discharge software vendor SilverVue acquires Ergo Sum Health, which offers preventive care software that supports MACRA payments to providers.

A jury orders Johnson & Johnson to pay $417 million to a woman who blames her use of the company’s baby powder for her ovarian cancer, extending a string of verdicts against the company of $110 million, $55 million, and $72 million despite a lack of evidence that the product is unsafe. That’s a lot to pay out from revenue of a product that sells for $3 at Walgreens.
Sales
University of Utah non-profit reference lab ARUP Laboratories will offer physician users Illumicare’s Smart Ribbon to display cost and risk of patient harm on EHR screens.
People

Andy Page (23andMe) joins Livongo as president and CFO.
Announcements and Implementations

Rush University Medical System (IL) sues Draeger for fraud, claiming the $18 million patient monitoring system it bought issued unreliable alarms, erased log data, and lacked the promised capability of automatically switching from wired to wireless monitoring during patient transport. Rush replaced the system for $30 million last year.
Datica posts a “Rethinking Health Technology” ebook that includes contributions from several industry luminaries, including St. Luke’s Health System VP/CIO Marc Chasin, MD and University of Wisconsin Health Center SVP/CIO Jocelyn DeWitt, PhD.
In the UAE, Al Jalila Children’s Specialty Hospital goes live on Vocera’s secure text messaging and hands-free voice communication platform.

A Department of Justice-funded project at Penn State’s nursing school will use telehealth technology to support rural sexual assault nurse examiners, offering them live physical exam mentoring, peer review, and education.
Government and Politics

The DoD proposes spending $250 million to build a five-bed hospital at Guantanamo Bay that would serve 5,500 residents and 41 prisoners. The Senate Armed Services Committee has asked for an analysis of why a tiny remote hospital would cost $50 million per bed.
Privacy and Security
Patient rights groups complain to insurer Wellmark that one of its executives described at a local Rotary Club meeting how a 17-year-old’s hemophilia cost the company $1 million per month to treat in trying to explain that health insurance doesn’t work actuarially if only people who are already sick sign up. The group claims that the remarks constitute a HIPAA violation, which might be the case since she cited the patient’s specific age even though she didn’t step over the HIPAA line in providing geographic information that is more granular than state level.
Other
A DC magazine profiles Meghan Buck, a former political consultant who formed Veda Data to apply machine learning to keeping physician directories updated.
This is either heart-wrenching, morbid, or both. A St. Louis hospital buys Cuddle Cots, a refrigerated bassinet that allows parents of stillborn or deceased babies to “put time on hold” in allowing them take photos and dress the body instead of moving it directly to the morgue. An article from earlier this year profiles families who spent up to two weeks with their deceased child’s body, taking it home and going for stroller walks as part of their grieving process.

The Miami paper runs a Q&A with CareCloud, whose CEO Ken Comee says the company will go public because, “My competitors are 20- and 30-year-old technologies and I have the best damned platform in the space.”
In India, the dean of a medical school’s hospital is placed on leave for trying to sabotage the parent company’s enterprise patient record and imaging project in favor of the hospital’s preferred vendor.
A Forbes Africa report finds that trained doctors are forced to work as restaurant servers and call center operators due to restrictive government policies and lack of coordination between the Department of Health and individual provinces, even as hospitals struggle with a shortage of practitioners.
In India, the government denies that a reported drop in oxygen levels killed three hospitalized babies. This follows an incident in which 60 babies died when another hospital’s oxygen supply ran out due to non-payment of bills. This time, a NICU doctor noticed low levels in the oxygen storage unit and called the hospital operator, who didn’t answer and was later arrested for being drunk and asleep on the job. The hospital says parallel systems kept the oxygen flowing to the wards while the problem was resolved, blaming the deaths on natural causes and therefore declining to perform autopsies, triggering the predictable complaints of a cover-up.
Weird News Andy isn’t elevated by this news. In Spain, a 25-year-old woman who had just delivered a daughter by C-section is crushed to death when a hospital elevator malfunctions on the way to the maternity ward. Her daughter was on the same gurney, but was unharmed.
Sponsor Updates

- Attendees at Aprima’s annual user conference make and donate 150 blankets to the Children’s Medical Center in Dallas.
- Datica announces self-service onboarding and free trials of its updated platform.
- Besler Consulting releases a new podcast, “Utilizing data and technology to manage your EPM programs.”
- Nine healthcare organizations select Nuance solutions to replace legacy radiology systems.
- ClinicalArchitecture and Diameter Health will exhibit at the SHIEC Conference August 27-30 in Indianapolis.

- The CoverMyMeds hockey team wins the league championship.
- CTG will exhibit at the AI Summit August 24-25 in Cincinnati.
- Cumberland Consulting Group raises over $2,000 for the Center for Family Services Project Backpack initiative.
- Ohio Business Magazine includes Direct Consulting Associates in its list of Best Places to Work in 2016.
Blog Posts
- Do Your Patient Access and Front-End Revenue Cycle Processes Need a Health Check? (Optimum Healthcare IT)
- Medicaid Incentive Program & MACRA Medicare QPP Differences (AdvancedMD)
- #RSNA17: The countdown has started (Agfa Healthcare)
- Investing in Care Management (Arcadia Healthcare Solutions)
- Spear Phishing: Hackers Aiming for Healthcare (Datica)
- Solutions for Improving Medication Nonadherence Costs (CareSync)
- Examining the Implications of the Human Cloud (CTG)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne, Lt. Dan.
Get HIStalk updates. Send news or rumors.
Contact us.





















































































































The news about AHRQ is very unfortunate. The AHRQ staff were always excellent to collaborate with. They had an impressive…