EPtalk by Dr. Jayne 3/26/26
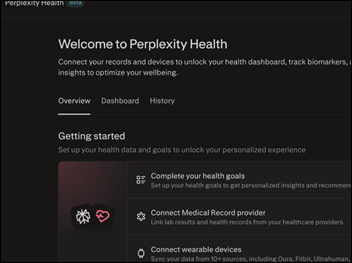
I was excited to learn about Perplexity Health. It gave me the idea of how to potentially solve the nightly “what should we have for dinner” question.
The announcement mentions that the tool can link to health records, fitness app data, blood pressure tracking, and weight data. It can couple fitness, activity, and vital sign data with lab results, which allows it to identify the time periods in which patients had a certain state of health. If people track their dietary information, they can track what they are eating each day.
Assuming that people log meals that they enjoyed, I would love to be able to tell my patients to ask, ”AI tool, look at that time in 2023 when I lost 20 pounds and my cholesterol was great. Then make me a meal plan that will replicate those conditions so that I can do it again.” Now THAT would be a good use of AI. I don’t have a paid subscription to Perplexity, but I might try this with other AI tools. More to come.
The National Resident Matching Program, also known as “The Match,” occurred last week. I was heartened to see that family medicine recruited another record-breaking class. Eight hundred family medicine residency programs offered 5,512 positions, which is the largest number ever. Of those, 4,613 positions were filled in the main match. Unmatched residents are still trying to link with open positions, so that number is likely to climb over the next week. Official numbers typically aren’t published until May.
Family medicine residency programs have offered an increasing number of positions for 17 years and the number of programs is also increasing. However, a forecast predicts that we will have a 40,000-physician deficit in primary care by 2036. As one might anticipate given recent changes in immigration policies, match rates declined for non-US citizens who attended medical school outside the US, with the lowest match rate seen in five years.
From Borderless Doctor: “Re: travel-related illness. I work at an emergency department that’s closest to a major international airport. I have seen some interesting travel-related illnesses, including plenty of patients who have infections that are not typically seen in the US and can spread quickly where hygiene might be poor. This article about Kansas health workers gearing up for the World Cup makes me wonder whether surrounding institutions will make EHR changes to encourage providers to consider different clinical possibilities.” I hadn’t seen anything about this, so I appreciate the share.
The Kansas Department of Health and Environment is preparing for the potential influx of 650,000 visitors by educating physicians and public health workers. Although most clinicians might think of respiratory and gastrointestinal illnesses first, a state epidemiologist who was quoted in the article also mentions an increase in sexually transmitted infections.
The department plans to publish weekly reports to educate health workers on the current status of outbreaks, especially given that visitors from the southern hemisphere may be bringing illnesses that aren’t typically seen at that time of year in North America.
The article mentions that Missouri is a little behind Kansas in preparing and is still planning its website, but Kansas has its site live. I’m sure that interagency coordination will occur, but this is a situation where a national focus on health and preparedness could shine.
Clinicians are encouraged to think about travel histories. As an informaticist, I can imagine some temporary popups in the EHR, especially for urgent care and other acute settings, that remind staff to ask specific questions similar to what they did when we last saw Ebola virus in the US.
If you work in a facility in the Kansas City area, I would be interested to hear about your plans. Otherwise, everyone should wash their hands, cover their coughs, and stay home if they are ill.
My healthcare tech worker friends are always having heated discussions about remote versus hybrid versus in-office work, and also the tools that organizations use to monitor employee productivity. One colleague shared this article about JP Morgan Chase’s use of technology to monitor junior members of their workforce. They compare self-reported work habits with the data that their IT systems capture.
Company spokespeople say that the effort is intended to increase awareness and to promote wellbeing among staffers who are working excessive hours. The bank limits junior staff to 80-hour workweeks.
It would be interesting to use similar tracking for medical residents to see how their actual hours worked stack up against their work hour limits. I suspect that a fair amount of work goes on behind the scenes after residents are required to leave the hospital, but I haven’t seen any articles about this kind of research.
OpenEvidence announces, in conjunction with Rare Disease Month, new features for engaging with content around rare conditions. The company has partnered with the National Organization for Rare Disorders (NORD). I was surprised to see Wilson’s disease as the example that they used to showcase the new rare disease summaries. I saw several cases of it in medical school and didn’t realize that it was truly that rare.
That’s the kind of bias that you can develop when training at a tertiary center. You are exposed to cases at different rates than they present in the actual population.
The partnership also supports the development of patient-friendly content that will be surfaced within the tool and distributed through the NORD Rare Disease Database.
In using AI tools, I’ve recently become a big fan of Claude for tone, content production, and overall usability. The company has opened access to some features that were previously available only to paid users to those with free plans, which was a nice surprise.
Anthropic says that Claude will remain ad-free, in response to OpenAI’s plan to display advertising for users who aren’t paying for a subscription. Claude’s free features include file creation, skills, and connectors, which I’m eager to try. I don’t use non-work AI tools as much as some people, so the conversation limits for free accounts haven’t been a barrier.
Even though I think it’s a great tool, it wasn’t able to help me track down the name of a book that I couldn’t remember. It had a complex plot involving a woman who committed a crime, became a detective, and later was called to investigate that same crime. I don’t remember finishing the book and searched in several ways to find it. The human brain finally remembered that it was a “plot within a plot” kind of book, where the protagonist was a crime writer and the plot I was thinking of was the one in her current novel.
I went back to Claude with the answer in hopes of better training the tool. The response was interesting. Claude said that it was essentially unsearchable because “no plot summary would mention it, because it’s a subplot within a completely different genre of book … It’s a genuinely tricky one that I don’t think I could have ever found through searching alone, and it’s a lovely example of how a book-within-a-book can stick in your memory as vividly as the main story itself!”
Are you a voracious reader? How do you track what you’ve read? Leave a comment or email me.

Email Dr. Jayne.


































I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…