Readers Write: Social Care Help Shouldn’t Come at Social Cost: Why Dignity and Ease Should Be at the Heart of Modernizing America’s Safety Net
Social Care Help Shouldn’t Come at Social Cost: Why Dignity and Ease Should Be at the Heart of Modernizing America’s Safety Net
By Jaffer Traish
Jaffer Traish is COO of Findhelp of Austin, TX.

The Safety Net
Social safety nets are different in each country. Some focus on poverty alleviation, economic mobility, or disaster relief. The World Bank has estimated that safety net programs have helped 36% of the poorest in the world escape extreme poverty.
In the US, we have seen federal administrations strengthen and weaken safety net funding over decades. The history of social safety nets in the US has been shaped by voluntarism, the notion that the voluntary actions and agreements undertaken by private charity and industry are preferable to state-mandated social welfare programs.
Nonetheless, the US has tens of millions of vulnerable people looking for services.
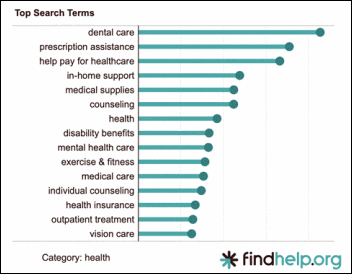
This is a breakdown of healthcare specific needs after analyzing 10% of searches from a population of 16 million Americans.
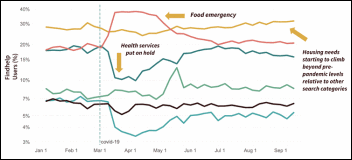
COVID-19 placed a spotlight on the vast array of needs. Our public benefit data mirrors what we heard and saw of the struggle for individuals and families.
Policy Winds
With the increasing awareness of social disparities and impact on health, we now see many major policy changes:
- ACO REACH Model. This model began on January 1 and includes focus areas on equity, access, and community health. There are reimbursement calculations and withholdings related to the area deprivation index (API) and SDoH quality measures.
- Joint Commission. New rules in effect January 1 include identifying a system leader who is accountable to address disparities in the patient population, as well as social needs screening and the sharing of community resources.
- NCQA. They released new HEDIS measures, including the SNS-E measure related to assistance for plan members needing food, housing, and transportation.
- CMS guidance letter. CMS issued a guidance letter on January 4 to state Medicaid Directors related to ILOS (In Lieu of Services) for Medicaid Managed Care, which relates to the Cal-AIM California waiver and many future waivers. The guidance strongly emphasizes the importance of measuring utilization and impact of non-traditional services such as social supports.
Private Company Technology is Accelerating Modernization
With any emerging market, we’ll see some companies taking advantage for short-term profit, multi-million dollar software costs, and a story of hype that fades post contract signature. We will see others that aim to maximize funding going to communities, to capacity building, and to community health worker staffing. Government and private sector buyers must be well educated to avoid the expensive shiny object that doesn’t deliver.
The good news is that healthcare leaders have long had a vision for what’s possible, including Judy Faulkner and Epic, where social services digitization is found in her original business plan.
SDoH is in the spotlight, with 80 bills proposed in Congress and $90 million of requested funding by states related to social care. Requests fall into several categories,including Medicaid waivers and federal match money.
We have the opportunity to build private-public partnerships that align on key principles. Education of key stakeholders is essential.
Influence
People go to helpers to get help. Those helpers might be a librarian, a pastor, or a neighbor. Those helpers may also be care coordinators, social workers, and hospital discharge planners.
State government can heavily influence the funding for services. Medicaid directors, Health and Human Services secretaries, commissioners, and deputies control how money is spent through Medicaid waivers, MCO contracting, non-profit capacity grants, and more. There are tough decisions to make, and there is incredible respect for people in these roles who are lobbied heavily by industry.
A large influence on these decisions is improving overall health and driving down the cost of healthcare. We all know over the last two decades of electronic health record implementations that technology alone is not the answer. Technology enables us to work more efficiently and more collaboratively, though it doesn’t solve governance, community engagement, or equitable service delivery.
State agencies want to understand the needs of their populations, where people are going to receive help, the services delivered, and when possible, the correlations with healthcare cost and clinical outcomes.
Some vendors promise a panacea of results via a top-down monopoly that goes something like this:
- Mandate use of a specific, single technology system.
- Force communities to use one system.
- Force non-profits into a contract.
- Force a per-user license model so the vendor makes more money with every user whether they adopt or not.
- Force a one-time consent so the vendor owns data sharing.
- Restrict federal dollars being used outside of this system.
This sounds like a good way to make a vendor rich and to skirt consumer privacy, interoperability, and non-profit autonomy.
The Choice
Procure one technology system with a hand in the face of private sector procurement or empower the community and health systems to choose the tools that make the most sense for them. Require that they report the data using standards and even certifications as the Office of National Coordinator (ONC) has supported for years.
Dignity and Ease
At the heart of this work is privacy. Imagine that you signed a single consent form for your healthcare provider to put your information into a system to facilitate a referral to a local food pantry or domestic violence shelter. But with that one action, you’ve granted more than 120 non-profit organizations the ability to access all of the personal financial, social, and medical data you reported. This is happening today because social care privacy standards haven’t kept pace with healthcare. People expect that their sensitive information will only be visible to the organizations and people they choose. Too many are blindly forced into one-time, all-in consent models in exchange for getting the help they so desperately need.
Healthcare, government, and non-profit leaders must improve safeguarding personal information by building a consumer-directed privacy approach to social care technology. Last year, the State of New Hampshire adopted a first-in-the-nation privacy protection law that established a policy framework to prioritize a person’s right to informed consent when seeking social services.
The Future of the Safety Net
- Imagine a future where applying for state benefits is a dignified, fast, digital process, not a paper process with a custom system.
- Imagine a future where a person in need can log in to a patient portal and see covered benefits, whether value-added, supplemental, community bank funded, or other non-profit led.
- Imagine a future where payers can see member needs and where their member has received help (with permission) anywhere in the country, and (with permission), intervene to prevent costly chronic or other clinical adverse events.
- Imagine a future where social workers, discharge planners, and other helpers simply use their EHR or care management system to make referrals and orders without worrying about which vendor is powering the SDoH network, a true API network model.
This is all possible. We should not be asking governments to pick winners and then learning too late about the risks to privacy and dignity taking place behind a curtain.
With network effects, community engagement, and trust building, the outcomes that we all want to see are possible. We can enact policies that do not create data silos or create monopolies with false promise. The right interoperability policies will create innovation in health and human services that are ubiquitous in every other sector.


Isn't there a Rule of Parsimony regarding words with optional, nonessential syllables? Or is this more of an AP Style…