TBF the anti-hate non profit was funding undercover investigators trying to being down the KKK & has done successfully for…
Monday Morning Update 4/11/22
Top News

All federal Cerner systems – DoD, VA, and Coast Guard – went down for two hours Wednesday due to a server problem.
The irony is that the server in question was running database software from Oracle, soon to be Cerner’s owner in giving CIOs their “one throat to choke.”
VA Deputy Secretary Donald Remy says that the VA and Cerner will conduct a root cause analysis of the downtime.
Meanwhile, the VA’s Walla Walla facilities went live as planned on March 26. Columbus is up next on April 30.
HIStalk Announcements and Requests
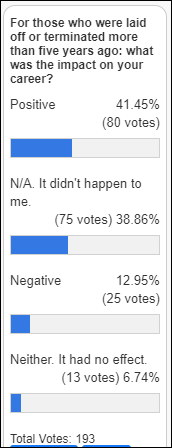
Two-thirds of poll respondents were laid off or fired more than five years ago, and two-thirds of those said it turned out to be a good thing career-wise.
New poll to your right or here: What is the most significant result of hospital mergers?
Listening: Pink Floyd’s first new recording since 1994 in “Hey, Hey, Rise Up!,” a fundraiser that protests Russia’s invasion of Ukraine. The song features Boombox singer Andriy Khlyvnyuk, who cancelled the band’s US tour and returned to Ukraine to take up arms to defend his country.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Announcements and Implementations
- Inova Health System signs an eight-year, $24 million contract with Visage Imaging to replace two legacy PACS with Visage 7, implemented in the public cloud.
Other

A reader sent me a copy of the paywalled Axios piece whose author claims that $4 billion startup Olive “overpromises and underdelivers.” It’s not exactly a smoking gun or a showcase of investigative journalism technique, obsessing instead with the company’s being “buzzy,” richly valued by investors, and driving purple buses around conferences. The article’s click-baity headline seems equally prone to underdelivering:
- Axios interviewed 16 “former and current employees, health tech executives, and others,” but apparently no actual current or former Olive customers, which seems to be a glaring omission for an investigative piece that focuses on customers. It does not list any cancelled contracts, aborted sales, or litigation that would suggest that Olive’s users are unhappy with the value they are receiving.
- The company claims that it uses AI/ML to automate administrative tasks, but often actually uses old-fashioned screen scraping. It is hardly unique to Olive that a lot of mundane technology has been optimistically relabeled as AI/ML because that imprecise term arouses prospects and especially investors. If Olive delivers the results it promises, I’m not sure the customer cares how they do it anyway.
- Former employees say the company uses questionable calculations to estimate potential cost savings, with one claiming that customers who expect $10 million in value “ultimately got less than a fifth of that.” A specific example would have been nice, hopefully including the reaction of the actual customer rather than that of a single ex-employee whose previous role wasn’t stated.
- The company doesn’t track outcomes and cost savings, and in some cases, has no way to do so. I would think that the customer is in the best position to audit Olive’s performance, so I’m not sure I find this relevant.
- Epic asked Olive to remove its name from company materials, saying Olive was misrepresenting the relationship internally and externally. I seem to recall writing about this as a reader rumor.
- Several sources say Olive salespeople installed capabilities that customers didn’t necessarily request because they know that the solutions would be difficult to remove afterward.
- Olive said in its response to Axios that it serves 200 enterprise customers, but Axios says internal documents say the real number is 80.
- My conclusion is that the article is thin on sourcing, not especially authoritative or insightful, and chose an easy target in a company whose market valuation is high but whose level of innovation is murky.
- The article doesn’t really change the basic of being a smart customer of Olive or any other vendor – perform due diligence of reference sites, get promises and expectations in writing, and share risk with the vendor instead of just writing them checks.

Amazon lists another interesting healthcare job. The senior clinical informaticist will join a team that is building “a completely new healthcare experience” (quibblers such as myself might point out that the “completely” is redundant and “new” might be as well). The job involves Amazon Care’s clinical systems, specifically its EHR.
It’s a slow news weekend, so I caught up on tweets from iconoclast Jay Parkinson, MD, MPH, who is about to launch a new venture, but meanwhile has some fresh thoughts that interest me (paraphrasing):
- The gold standard in healthcare is the status quo. If that is a procedure, we’re probably the best in the world. If it’s a service, near the worst, yet the worst is fiercely defended.
- Patient histories at Jay’s former company Sherpaa ended with the same last question – what do you think you have? Patients were right 95% of the time. That would be an interesting way to design a telehealth service.
- It’s interesting that one-condition companies pivot to add more to grow their bottom line, like Noom doing weight loss for 15 years and now they are adding stress and anxiety.
- Journalists covering digital health funding, rather than reporting milestones that justify company valuations, is like baseball news reporting only that a new batter is up.
- Medical is pills, procedures, and feeling fleeced. Health is fun, it feels good, and people are happy to pay for that. The most successful DTC brands in “digital health” are consistently “health” rather than medical.
- The evidence for a drug is at the population level, not at the individual level. Since most people aren’t doctors acting on populations, they only think at the “me” level. They don’t really realize that most drugs are a crapshoot at the “me” level.
- Teladoc transitioning from being known for 20 years as one of the many places to turn to for a quick prescription for a UTI or pink eye to now wanting to manage all things serious and branding it as the “whole health” of a population … well, that must be a real bear.
- The amount of money and time people will spend to see the same guys on different stages answering the same questions is astounding. It proves that there is insatiable demand for health conferences, and if you really want to make a buck, start a
platform for health conferences powered by AI and schedule one every week with the same lineup. To scale up, develop Glen Tullman and Jonathan Bush robots who can appear on stage, and they themselves can invest in it so they can focus on being CEOs.
Sponsor Updates
- Applied Clinical Trials magazine features OptimizeRx VP of Data Product Mike Rousselle in a new episode, “A Passion for Predictions.”
- Olive will open a new office in Columbus, Ohio, adding 400 jobs.
- Symplr CEO BJ Schaknowski joins Susan G. Komen’s Board of Directors.
- Premier releases a new podcast, “How AI Can Drive Value in Healthcare.”
- The Highway to Health Podcast features Relatient VP of Marketing Josh Byrd in a new episode, “How Josh Byrd Uses Songwriting Experience to Tell the Patient Story.”
- TriNetX enabled researchers at Hospital Universitario 12 de Octubre to leverage European real-world data for a study that found that multiple myeloma patients were more likely to contract COVID-19 and suffer a higher risk of mortality than non-MM patients.
- Optum publishes a white paper titled “5 priorities to improve financial performance.”
- Wolters Kluwer Health publishes a new report, “Nursing’s Wake-up Call: Change is Now Non-Negotiable.”
- VisiQuate announces major enhancements to its Flo and Late Charges predictive analytics solutions that help healthcare organizations achieve peak business health.
Blog Posts
- Patient Engagement Strategies that Improve Health Outcomes (PatientBond)
- 4 Healthcare Trends from HIMSS22 (Pivot Point Consulting)
- PerfectServe’s Clinical Collaboration Solution Reduces Care Team Toil (PerfectServe)
- The Quest for Evidence in Value-Based Care (Symplr)
- Geisinger Implements EHR Alerts, Reduces Costly Lab Orders (Premier)
- Why you shouldn’t underestimate the importance and value of contact center technology (Spok)
- 3 Benefits of Advanced Clinical Workflows in Alarm Management (TigerConnect)
- The year ahead in cancer statistics: Why personalized risk assessment remains so important in cancer care (Volpara Health)
- Better Together: What Joining Forces with Clinicient and Keet Means for the Industry (WebPT)
- How Patient-Provider Communication Can Support Community Mental Health (Well Health)
- If you built it, people will come – when you build what matters (West Monroe)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.



On single condition vendors, there’s some amount of bulk pricing to acquiring consumers, a small addressable market, and a low cost to scaling the service. For example, maybe google sells you the second million ad clicks cheaper than the first million. You do simple pink eye cases, but you can’t run the same pink eye ad for those second million clicks because you’ve already found everyone who wants to get their pink eye treated remotely. Having your medical staff start treating UTIs in addition to pink eye doesn’t cost much from a service perspective. Now you can leverage your existing scale in marketing to make a better margin on your new UTI service line. I think a lot of these opportunities are going to get burned through in the next five years and these companies will end up in the business of acquiring consumers to refer into big health systems, just like your town doctor’s office got assimilated into being a channel by which the mega health system catches all the referrals for high margin medical services in your town. You can already see these “partnerships” starting to develop between cash rich health systems and single condition vendors.
Don’t know if it’s a bear but it definitely makes things a little hairy.
It seems obvious but the platform features that you need for robust telehealth delivery are not the same as for a brief pinkeye or UTI visit. And Teladoc just isn’t up to speed yet in that regard. People have gotten used to Zoom and expect that level of features for telehealth (except perhaps being able to turn yourself into a talking cat). Without technical basics, it’s hard to understand how broader “whole health” initiatives would be successful.
The obsession with funding and valuations for health IT companies gives me the WeWork creeps. Where’s the tangible evidence that the technology matches the hype? Too many are making money off of healthcare’s inefficiencies by adding more complexity to the mix. What ever happened to the importance of people and process, which actually determine how a technology is used and the benefits it may or may provide?