TBF the anti-hate non profit was funding undercover investigators trying to being down the KKK & has done successfully for…
News 3/17/21
Top News
Tegria, Providence’s recently formed rollup of its nine health IT acquisitions, acquires health IT consulting firm Cumberland.
Cumberland, which was founded in 2004, will operate as an independent Tegria business unit. It will add to the company’s capabilities in claims and benefit administration systems, care management systems, managed services, and technology optimization.
Tegria’s other consulting and technology brands include Bluetree, Community Technologies, Engage, and Navin Haffty.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
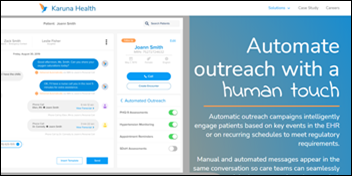
Healthcare development platform vendor Commure acquires Karuna Health, a digital patient communication startup based in San Francisco.
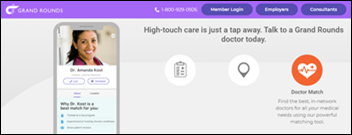
Employer-focused care navigation company Grand Rounds merges with Doctor on Demand. Grand Rounds CEO Owen Tripp will lead the new company, which will retain the Grand Rounds name. Doctor on Demand CEO Hill Ferguson will remain head of that brand.
Sales
- UC Davis Medical Center (CA) will implement adverse event tracking and disease management software from Qview Health across all of its departments and services.
- Emory Healthcare in Atlanta selects enterprise imaging technology from Sectra, which it will link with neighboring Grady Health System.
- Kidney Disease Medical Group in Los Angeles will use Emerge’s platform to enhance its Athenahealth EHR.
- The Massachusetts League of Community Health Centers will leverage PatientPing’s real-time admission, discharge, and transfer alerts to monitor patient events across its network of 52 centers.
People

Cone Health (NC) interim CTO Doug McMillian takes on the additional role of CISO.


Bright.md names Steve Giannini (Opal) as CEO. He takes over from co-founder Ray Costantini, who remains on the board.
Announcements and Implementations
Vyne Medical adds auto-indexing to its Trace integrated communication exchange engine, which allows health systems to transform documents and unstructured patient information into structured, shareable data without hand-keying information.

Spectrum Health (MI) incorporates TytoCare’s home medical exam kit into its virtual care services.
Newport Hospital and Health Services (WA) implements Epic through the software vendor’s Community Connect program.

Kingman Regional Medical Center (AZ) works with Meditech Professional Services to redesign workflows based on key performance indicators.
Digital health engagement platform vendor Quil launches Caregiving Circle, which allows a patient’s family and friends to join them for addressing health events or navigating day-to-day activities. The initial user is Penn Medicine’s orthopedic department, which will use the product for geriatric hip events.
Government and Politics
The Defense Health Agency works with Cerner to develop MassVax, a COVID-19 vaccine management system the DoD is incorporating into MHS Genesis.
The Texas Health Services Authority receives additional funding from ONC’s STAR HIE Program to expand its work with the SANER Project, a collaboration led by Audacious Inquiry that is working to develop better COVID-19-related data-sharing processes.
COVID-19
CDC reports that 28% of US adults have been given at least one COVID-19 vaccine dose. Total administered doses are at 111 million. US deaths are at 533,000.
Several EU countries suspend their use of AstraZeneca’s COVID-19 vaccine after reports of abnormal blood clotting from Norway. WHO advises that no proven link exists for the 37 cases in 17 million vaccinations and thus recommends the product’s continued use. AstraZeneca notes that the occurrence of thrombotic events among vaccinated people is actually lower than in the general public and no such events were observed in 60,000 clinical trials participants.
WHO’s chief scientist says that better COVID-19 vaccines could be released later this year or next year, possibly products that don’t require needles and that can be stored at room temperature.
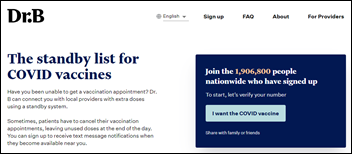
Zocdoc founder Cyrus Massoumi, MBA launches Dr. B, a website that helps eligible people locate COVID-19 vaccines in danger of going to waste. The service, largely a volunteer effort so far, is sending out availability alerts for two providers in New York and is working to onboard 200 more across the country.
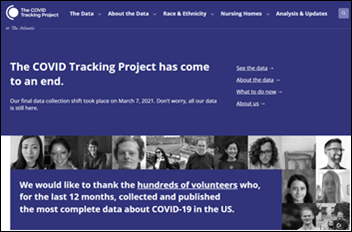
The Atlantic writers who founded the just-completed COVID Tracking Project — which for all of 2020 was the most-reliable, best-vetted source of US coronavirus testing, infection, and hospitalization, even including the CDC’s failed dashboard — say US data reporting systems failed because they were working as (poorly) designed:
- Pandemic preparation plans emphasized data-driven decision-making without considering that the required information might be unavailable or unreliable.
- States inconsistently rolled up their detailed data into simple federal feeds that appeared to be standardized, but really weren’t, leading to errors in the epidemiological models that were created from that information.
- Data “travel at different speeds,” so coronavirus testing and case data is always a snapshot in time of information that can’t just be combined, such as with fast-reported case counts and slow-reported negative test results.
- Reports of deaths are delayed from a handful of days to months, meaning that an outbreak’s death toll can’t be accurately reported until weeks after it is already over.
- The federal government says that 4 million antigen tests are being performed daily, but state records show a small percentage of that number, and nobody has been able to explain the difference or whether the unreported results are significant.
- The data the authors trust most is HHS’s hospital-reported data.
- Data-driven thinking isn’t necessarily better than other forms of reasoning, and could even be worse if the underlying data deficiencies aren’t understood. A recent example was CDC’s March 1 warning about an uptick in case and death counts caused by variants, which the authors knew wasn’t accurate since case counts had been falling sharply for the previous month. Those numbers jumped because states were processing a backlog of death certificates, especially in storm-crippled Texas.
- At least five states regularly submit incomplete data, yet that flawed information is being used by CDC to advise those states on school reopening.
Other
A study finds that quality measures that are calculated from a single provider organization’s EHR data differ from those calculated from aggregated HIE data in 19% of patients, which the authors attribute to patients who see multiple providers. Pneumonia vaccination of older adults, for example, was 7% better when looking at the data of all participants than when calculated from a single provider’s data. The authors conclude that information exchange is essential for accurately calculating quality measures that drive provider payment.
Kaiser Health News says that even though millions of Americans are wearing prescribed, expensive continuous glucose monitoring patches, little evidence exists that the extra cost over cheap daily finger sticks provide better outcomes for people with Type 2 diabetes who don’t use insulin. The manufacturers are aggressively pushing them for Type 2 use because of the large potential customer base as compared to Type 1 diabetics.
Sponsor Updates
- Ascom Americas Senior Product Mobility Manager Jack Langsam raises $5,000 for Susan G. Komen.
- CarePort CEO and founder Lissy Hu, MD will speak at the Whole Person Care Summit March 23.
- Central Logic welcomes back Jodi Hubler to its board.
- Impact Advisors is named to the Forbes list of America’s Best Management Consulting Firms for 2021.
- KLAS ranks Cumberland’s payer IT consulting services number two in the “2021 Best in KLAS: Software & Services Report.”
- EClinicalWorks publishes a guide to choosing a vaccine administration management system.
- Lyniate names Christy Evans (Surescripts) director of strategic partners, and announces new partnerships with Sensato and Secure Exchange Solutions.
Blog Posts
- 3 Actionable Tips for Reducing Claim Rejections (AdvancedMD)
- How to shape a blueprint for progress, with Business Intelligence (Agfa HealthCare)
- Ending isolation when your workforce is dispersed (Alcatel-Lucent Enterprise)
- Patient Safety Awareness Week: Annual Reminder to Advance Quality Healthcare Initiatives (Capsule)
- Why is Length of Stay Important? Five Key Reasons (Central Logic)
- What the pandemic taught me about patient safety (Meditech)
- The Benefits of Robust Immunization Information Within EHRs (ChartLogic)
- Policy Updates Can Pave the Way to Interoperable Healthcare IT in 2021 (CoverMyMeds)
- What You Need to Know About the Data on COVID-19 Vaccinations (Dimensional Insight)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.




The report that quality results are better when more data is available made me chuckle. No kidding! Those of us who implement measures know the truth: most measures required for ambulatory and pop health purposes are designed with zero consideration of the reality of clinical data and patient journeys across siloed information systems. Appropriate that the story directly follows the analysis of the failures in COVID19 data. When the measurement system is designed without consideration of the data sources, chaos ensues.
“Data-driven thinking isn’t necessarily better than other forms of reasoning, …”
That sound you hear? It’s the sound of thousands of Quants’ heads exploding!
Seriously, data-driven decision making is practically a secular religion in many quarters. I think the Atlantic article makes excellent points. But if you survey the literature, it’s always skewed towards, “make more decisions based upon the data! And if you don’t have data, then get some!”
Re: “expensive continuous glucose monitoring patches”
OK, but it’s not Unreasonable to expect better outcomes either. I’d feel free to call out blatant upsells and expense padding. This does not sound like that.
The long-term negative health implications of diabetes are believed to result from large and repeated blood sugar/insulin swings. There’s plenty of clinical research to support this.
Thus, continuous monitoring can do 2 positive things:
1). Catch short-term diabetic crises early;
2). Help manage the longer-term implications of diabetes.
IMO, the missing component is continuous insulin administration. There are several technologies available that do this, though none are in routine clinical use (AFAIK).