EPtalk by Dr. Jayne 9/24/20
An article published last week demonstrates the ability for health systems to save money though implementation of clinical decision support (CDS) tools within their EHRs. One major outcome was the ability of CDS tools to help reduce waste by reducing unnecessary laboratory tests and antibiotic prescriptions. Researchers also noted issues with CDS systems, including maintenance costs and malfunctions that could have an adverse impact on bending the cost curve.
The authors “could not draw a sound correlation between vendor-purchased or home-grown systems’ costs to their economic benefit,” however. I would go further to state the need to look at the middle choice in that continuum as well: the heavily-customized vendor system, which sometimes is closer to homegrown than not.
Further studies are needed, and one of the elements that should be included is the impact of alerts on clinicians and the time they spend managing those alerts. They also need to assess the impact on extensive computerized physician order entry (CPOE) order sets that may add orders to a patient’s record when those orders aren’t entirely necessary. There’s always a balance between the technology, the needs of the patient, the needs of the care team, and the bottom line. A well-configured EHR can make your day go well, but a poorly-managed one will be your worst enemy.
On days that I see numbers of patients that would have been considered impossible before COVID, I’m truly grateful that my organization has stripped the EHR down to only the bare essentials that are needed to document quickly, without any extraneous content. The downside to that approach is that sometimes I find myself in a situation where I wish I had a fighter jet, but I’m piloting a Stearman. I’d love to see the vendors that are bragging about their ability to create documentation through voice recognition and artificial intelligence spend a day in my well-worn shoes. I’m sure what they see would be shocking, but we can’t solve problems that we don’t understand.

The US Food and Drug Administration is launching a Digital Health Center of Excellence within the Center for Devices and Radiological Health. Digital health technology within its purview includes mobile health services, wearables being used as medical devices, Software as a Medical Device (SaMD), and technologies used to study medical products. The FDA plans to create a network of digital health experts and to get technology to patients faster by providing technological advice, coordinating work being done across the FDA, advancing best practices, and reimagining the oversight of digital health devices.
I almost missed this one in my overflowing inbox, but apparently a new national system is being developed to track administration of the COVD-19 vaccine. Millions of people who are used to walking into a retail clinic or their local Costco and walking out with an influenza vaccine are going to be surprised by the complexity of the new coronavirus vaccine. Patients must receive two doses and the products are not interchangeable between manufacturers.
Public health officials are justifiably concerned that this new system will bypass existing state immunization registries, while watchdogs are concerned about its $16 million cost. Consulting giant Deloitte has been engaged to develop the Vaccine Administration Management System, which will use underlying Salesforce technology. It’s apparently been piloted in four states over the summer, but details are scant on what data fields are required or when states will be able to obtain access to test versions.
We’re all familiar with the COVID-related hospitalization data debacle from earlier this year, and it looks like we’re teeing up another not-so-successful deployment. Without appropriate user acceptance testing or the involvement of actual stakeholders in the field, software projects usually fail. I’ve seen this enough as a clinical informaticist and it baffles me that in such a critical moment we’re making so many systemic mistakes. Not surprisingly, patient matching is a concern in this effort. Who’s wishing we had a national patient identifier now?
I’m practicing in a community in a surge situation, where we have been featured on several “worst places for COVID” lists. It’s not an enviable position. I’m continually challenged by patients who are wearing what are essentially “non-masks” rather than accepting one of the medical masks that we offer at the front desk. Today I saw a family for COVID testing and every single one of them was wearing a bandana. When offered medical masks by my staff, the parent declined, stating that they were only wearing the bandanas to humor our request for masks, and they refuse to wear a medical mask because they cause lung disease. Unfortunately, we’re not allowed to deny service to non-maskers.
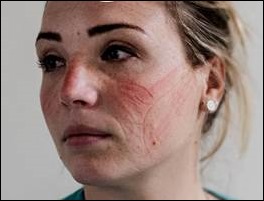
Trying to educate around those beliefs is a losing battle, and since they were there for COVID testing, I certainly didn’t want to spend a minute longer in the room than I had to. If masks are deadly, how are any operating room nurses or surgeons still standing? Why haven’t the attorneys come calling? Kudos to Dove for its “Courage is Beautiful” video that shows what we really look like under our masks. Even though many people across the US have moved back to their normal lives, our lives (and our faces) will never be the same again.
Just when you think you’ve reached the pit of despair, you’re sometimes surprised. When a pediatric patient started crying about having a COVID test, my scribe offered to show her how it was done, and literally took off his mask and swabbed himself right there. Her eyes were wide and so were mine, and the patient went along after seeing how easy it was. I’ve never seen someone perform a nasopharyngeal swab on himself, let alone do it blind, so I was impressed. We did, of course, have a conversation about how he probably shouldn’t do that again since he was unmasked and the patient / family had no way of knowing that he recently recovered from COVID and is considered noninfectious at the moment, but it was a touching gesture.
For those of you in the clinical trenches, what has been your wildest moment during COVID? Leave a comment or email me.

Email Dr. Jayne.


TBF the anti-hate non profit was funding undercover investigators trying to being down the KKK & has done successfully for…