I tend to think that tests of ability (rounds, in this case), ought to stay close to real-world situations. Therefore,…
Monday Morning Update 5/27/19
Top News
The VA skips a House committee meeting that addressed oversight of its Cerner implementation, but attends a Senate meeting long enough to oppose a bill that proposes creating an independent advisory committee to oversee the $10 billion project.
Reader Comments
From Anon E. Mouse: “Re: EHR timers. Cerner was the vendor that wasn’t directly mentioned in the article, although it’s obvious since Eva Karp works for Cerner. Cerner’s Lights On Network has been freely available with such timers for years and is used by many of their clients daily. Cerner invests a ton of effort in building additional timers as they introduce new software and functionality and then works to attack the problem areas to improve performance and clinical workflow.” Cerner’s write-up of Lights On Network describes its benefits: finding users whose system actions suggest that they could use help, identifying system bottlenecks, flagging unusual system settings, and benchmarking against other Cerner clients.
HIStalk Announcements and Requests
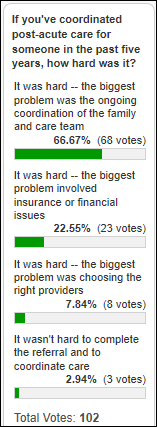
A convincing 97% of poll respondents who have coordinated post-acute care for someone said it was hard, with the biggest issue being trying to coordinate the activities of the care team and family. Some comments:
- Vicki says organizations served only their own interests in caring for her family members, such as a SNF that wasn’t interested in helping find a home health provider other than the one it owns.
- Clark’s experience with transitions from ICU to LTAC, SNF, home care, and therapy providers is that nobody every had current patient information, creating both frustration and danger.
- Brittany’s experience with hospice care is that medical equipment wasn’t delivered, transportation was delayed, and nurses misunderstood the family’s wishes and kept the family member over-sedated in denying them the chance to have meaningful final moments together.
- Another reader reports that they experienced excellent coordination at Johns Hopkins, but had a “consistently horrendous” experience at their own hospital, where they are a physician faculty member. HIM dragged their feet on providing an electronic copy of the medical records, obtaining images required two trips and upfront payment of fees, a chaotic discharge process created delays that necessitated rescheduling home health appointments, refrigeration-required antibiotics were delivered early when nobody was home, prescriptions were sent to the wrong pharmacy, hospital nurses argued with the family over the medication list in insisting that their computer must be correct, and the hospital ran out of common medical supplies.
- Caregiver Informaticist says their family member’s care was never coordinated in several trips between LTAC and the acute care hospital, with no information sharing after being falsely told that the LTAC’s doctors round at the hospital and attend joint care planning meetings.
New poll to your right or here: What is the main cause of burnout among employees of health IT vendors and hospital IT departments? My experience working for a crappy vendor makes “all of the above” attractive, but let’s focus on the most important item on the list. For me, that was incompetent, uncaring managers who interfered with our productivity in trying to add value to processes they would never understand, poring over their MBA textbooks in their spiffy offices with the doors shut before emerging into the cube farm to make a lofty pronouncement that after applying their exemplary insight to our operation, they had figured out the solution to our problems (we had tried it before and failed, but saying so elicited scorn that what we had been missing then was their keen leadership). Worst of all, they had no healthcare background and thus nothing but contempt for our users and the patients who depended on our systems – we were just a widget factory that happened to sell healthcare software. I made an impassioned, stick-figure level plea to one of the suits about a patient-endangering software defect that I had laboriously documented urging him to simply allow us to notify all customers of the problem since we hadn’t yet figured out how to fix it. His answer: “We don’t owe those clients a damned thing.”

Monday is Memorial Day, created not to serve as a nonchalant kickoff to summer, but rather to set aside time to remember those who died while serving in the armed forces. It’s perfectly fine to pass on attending a ceremony or an increasingly rare Memorial day parade, but perhaps you know someone who lost a family member (especially if it happened within the past handful of years) who was serving and could drop them a quick email or social media acknowledgement of their loss. Here’s another idea – take flowers to a cemetery that has a section set aside for soldiers and leave one on each grave that doesn’t already have some.
In Flanders Fields
By John McCrae
In Flanders Fields the poppies blow
Between the crosses row on row
That mark our place; and in the sky
The larks, still bravely singing, fly
Scarce heard amid the guns below.
We are the Dead. Short days ago
We lived, felt dawn, saw sunset glow,
Loved and were loved, and now we lie
In Flanders fields.
Take up our quarrel with the foe:
To you from failing hands we throw
The torch; be yours to hold it high.
If ye break faith with us who die
We shall not sleep, though poppies grow
In Flanders fields.
Webinars
May 30 (Thursday) 2:00 ET. “ONC Data Blocking Proposed Rule: What Health Systems Need to Know.” Sponsor: Philips PHM. Presenter: Greg Fulton, industry and public policy lead, Philips. Proposed data-blocking regulations could specify fines, disincentives, and de-certification of providers who don’t provide an API for patients to extract all of their data. This webinar will describe who is deploying APIs, the scope of data and third-party apps that can be used, the seven costs that do not count as a data-blocking exception, and the health system protections that don’t involve using a vendor. It will also provide examples of data blocking and further exceptions.
Previous webinars are on our YouTube channel. Contact Lorre for information.
People

HHS promotes Jose Arrieta to CIO.
Announcements and Implementations
Lawrence General Hospital completes its implementation of Meditech Expanse under a fixed-fee implementation agreement with Santa Rosa Consulting.
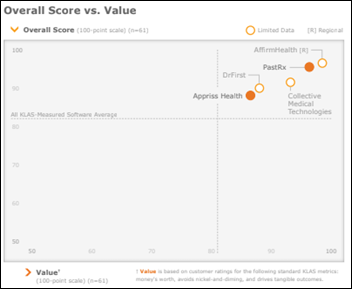
A new KLAS report covering opioid prescription intelligence finds that all vendors reviewed performed well. PastRx tops the list in pulling PDMP data into the chart for physician review, while AffirmHealth and Collective Medical were praised in their respective regional pain management clinic and ED environments. Appriss Health and DrFirst were seen as less helpful in developing an opioid stewardship strategy since they work with users only indirectly.
In England, Guy’s and St Thomas’ NHS Foundation Trust issues a 10-year, $225 million tender for a enterprise EHR that will be used by up to 35,000 employees of three London-based trusts.
Government and Politics
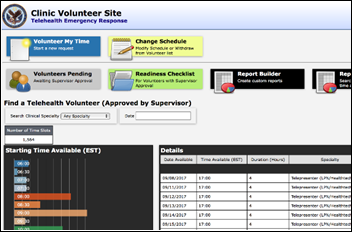
The VA’s self-developed, open source workflow tool Light Electronic Action Framework (LEAF) wins a government health IT magazine’s innovation award. The team used the tool to develop a telehealth provider volunteer site for hurricane relief efforts (pictured above) within 24 hours.
Other
A data study finds that Canadian buyers of marijuana (where it is legal) avoid paying by credit card since they know their data is likely to be stored on servers in the US (where it isn’t legal). Also in play is that some employers enforce zero-tolerance policies for non-medical use. Canada’s own Office of the Privacy Commissioner recommends that buyers pay cash since the US government can access their credit card records without a warrant and could prevent them from entering the US.
I’m fascinated by this: Elon Musk’s SpaceX uses its Falcon 9 rocket to launch the first 60 low-Earth, 500-pound satellites of its $10 billion Starlink broadband service, which will offer inexpensive broadband connectivity to the northern US after six launches, the whole country after 12, and the entire populated world after 30. The company will use the revenue from the broadband service to fund its planned colonization of Mars.

An interesting op-ed piece by the co-founder of a clinician collaboration platform says that architects ruined healthcare by emphasizing grand, soothing aesthetics for visitors while eliminating the conference rooms and lounges where clinicians can interact with each other. He also opines that the Disney-created concept of hiding the “messy parts” of running a hospital means that the healthcare professionals themselves are the messy parts. He concludes that hospital design is now obsessed with distracting people from thinking about their health rather than making them healthy.
More evidence that Americans are too science-challenged to form rational healthcare opinions: people are OK with the widespread rollout of untested medical treatments, but object to randomized trials in which two equally acceptable treatments are applied to separate groups to determine which is better. Experts can’t explain the results, but think people might worry that consent is required from those who don’t get a particular treatment or that such tests should be unnecessary because experts should already know what works.

A third-year UTHealth medical school student who has undergone six brain surgeries, survived on artificial nutrition due to gastroparesis, and had a stroke that left her temporarily paralyzed from the waist down says the experience (along with deficits in her hand function from the stroke) has motivated her to consider a career in physical medicine and rehabilitation and neurology.
Sponsor Updates
- Meditech; NextGate; Clinical Computer Systems, developer of the Obix perinatal data system; CereCore; CloudWave; Experian Health; PatientKeeper will exhibit at the 2019 MUSE Inspire Conference May 28-31 in Nashville.
- Waystar will exhibit at the EClinicalWorks Education Expo May 27-31 in Boston.
- The Chartis Group publishes a white paper titled “Bridging the Digital Divide in the Healthcare C-Suite: Positioning IT for Success in the New Health Economy.”
- OmniSys and Surescripts will exhibit at the PioneerRx Connect 2019 May 31-June 2 in Orlando.
- Relatient welcomes its 100th employee.
- Sansoro Health releases a new 4×4 Health Podcast, “Intellectual Property for Entrepreneurs and Investors.”
- The SSI Group will exhibit at the South Carolina HFMA Annual Institute May 28-31 in Myrtle Beach, SC.
- PatientKeeper will demonstrate its EHR optimization solutions this week at E-Health in Toronto and MUSE Inspire in Nashville.
- Community First Health Plans goes live with ZeOmega’s Jiva LTSS for long-term care.
Blog Posts
- The Future of Healthcare: What Can We Expect by 2025? (Dimensional Insight)
- Access and Halifax Health: Boosting Clinician and Patient Satisfaction (Access)
- 4 Types of Medical Errors (and How to Avoid Them) (Mobile Heartbeat)
- Delivering Care for Patients on Their Own Terms (Netsmart)
- 7 Keys to Better EHR Usability (EClinicalWorks)
- The 3 keys to compliance for healthcare marketing data (Experian Health)
- What Is Timeliness of Care & How Can You Make Your Practice More Efficient? (PatientBond)
- Attending HFMA Annual? Find Us at These Sessions (Patientco)
- Top Three Pain Points for Urgent Care Centers (Practice Velocity)
- Digital Health Done Right: NeuroFlow (Redox)
- One Year Down: GDPR by the Numbers (SailPoint)
- An Urgent Call for Transformation: Prescribers Need Better Information and a Streamlined Specialty Prescribing Process (Surescripts)
- Where big data and clinical communication meet. (Voalte)
- A 5-Point Communication Strategy to Help Reduce Clinicians’ Cognitive Load (Vocera)
- 5 Simple Marketing Techniques for SLPs (WebPT)
Get Involved
- Join my Rolodex to provide occasional news reaction or ideas
- Contribute regularly as a provider CIO, IT director, or informatics nurse (anonymous or not)
- Be interviewed (providers)
- Deliver an educational webinar (providers)
- Sponsor
- Report a news item or rumor (anonymous or not)
- Sign up for email updates
- Connect on LinkedIn
- Contact Mr. H





Thank you Mr. H for reminding readers of what Memorial Day is about. – A Gold Star family member.
Thanks for sharing the article on hospital architecture!
On a recent walkthrough of a brand new multimillion dollar building at our medical center, the conference rooms are gone and they’d also eliminated all of the working areas for clinicians. This means there is no place to sit at a desktop computer and actually do work or make phone calls.
The computers in the patient rooms are ergonomic disasters. Plus, it’s difficult to concentrate and write efficiently when patients or families are asking questions.
We are also a teaching hospital and the architects seem to have forgotten that it’s rather hard to teach without talking and also hard to teach clinical medicine without talking about patient related information. As it is, we often have to remind people not to discuss patient information in public or semi-public areas. This will be infinitely more challenging without any available private areas to discuss clinical issues.
They did, however, install a faux fireplace in the oncology infusion center to make it seem more welcoming and homey.
I did consulting about a decade ago for a teaching hospital that was being built to advise on how to make sure the layout promoted it being “EHR ready”. I was handed the outlines of the medical ICU floors, and they had left so little space that they were either going to have to choose call rooms or tiny conference/charting rooms on the same floor. When I pointed that out, I was told that they couldn’t change any of that, and the space was going to be offices for the ICU leadership, so no call rooms or conference rooms. Turns out a committee had put together their high-level requirements, handed it to the architects, who had returned these designs, and at that point it was too late to make any changes.
The hospital has been built for a few years now. I imagine all the residents are in great shape because they’re doing stairs all day long. The architects get another point for “healthy design.”
Thanks for reminding everyone what Memorial day is about.