The ruling does seem to actually touch on things like UserWeb access "...the final rule applies to terms and conditions…
Monday Morning Update 5/6/19
Top News

From the Allscripts earnings call:
- The company reported record first-quarter bookings despite revenue growth that was less than it had predicted.
- One Paragon client was committed to switch EHRs until “they experienced the sales implementation by one of our competitors” and extended their Paragon agreement for five years. The hospital was Waverly Health Center, which would suggest that the abandoned replacement vendor was EClinicalWorks, who announced them as a new inpatient customer in April 2018.
- The company says that recent development of a Paragon ambulatory platform has caused five clients to come back in the past 90 days.
- CEO Paul Black notes that the company has “the longest-tenured leadership among the top three publicly traded companies in the marketplace,” which he says allows the company to focus on long-term priorities.
- Black says Veradigm positions the company as a top provider to payer and life sciences markets, to the point that EHR competitor NextGen partnered with Allscripts instead of developing a competing product.
- Acquisitions over the past five years have added $300 million in annual recurring revenue “at a net cost approaching zero.”
- Black says Allscripts is the only one of three companies (I assume he’s referring to Epic and Cerner) that is making significant investment in core acute care solutions.
- In responding to an analyst’s observation that company debt increased due to share buy-back, the company says it is comfortable with its leverage position.
Reader Comments
From Big System CIO: “Re: HIStalk interview. My experience is that going on record encourages the vendor community to overwhelm us in claiming they can assist, regardless of whether we need help or not.” BSC politely declined my interview request for a reason I hadn’t considered – mentioning an initiative in our conversation guarantees that vendors who read it will bug them endlessly to pitch their services. I guess cold-calling it must work at least occasionally or they would stop doing it. I’m interested in both the provider and vendor side of this issue – how do you feel about reps randomly dialing someone up at the hospital hoping for a hit?
From Just Asking: “Re: IT in faith-based health systems. You’ve said you had experience there. What should I look out for if I take the IT executive job offer in front of me?” I can only relate my personal experience, which certainly varies by organization. The top problems that my IT peers had in working for an organization whose faith wasn’t ours (and that was one of the more extreme ones, I suspect) were:
- The culture was inbred, where everybody went to the same churches, graduated from the same unimpressive church-affiliated universities, and had been chosen since their diaper-wearing years for fast-tracking through various internship and training programs in traveling from one hospital to the next to the way to the top. It’s tough participating constructively in meetings where everybody except you as the IT person has longstanding, trust-based relationships that drive everything instead of knowledge or experience.
- IT was the dumping ground for underperforming but well-connected junior employees who were untouchable and knew it, so their pathetic job performance demotivated everybody else.
- IT felt like being an American contractor sent to work in a Middle Eastern hospitals – we were tolerated at best, never respected, and were forced to follow the corporation’s cultural-religious rules while having our own ignored. Be careful taking a job with any health system that declares itself to be a ministry unless you actually want to work for a ministry.
- Just about every major strategic IT decision was made in meetings to which IT was not leading or even invited because, as one top-ranking executive said in being unaware that he was on a conference line, “Can’t we get one of our own in there?”
- On the flip side, they paid me well, the benefits were unbelievable, the glass ceiling was obvious but tolerable unless you fancied yourself qualified to be on the executive fast track, and I think they were doing the best they could to integrate us interlopers into the organization in at least a clumsy, superficial way.
From Bewilderment: “Re: succession plan. People joke about that of Judy Faulkner. What’s yours?” I don’t have one. I’ll probably just keep going until I drop dead and then the HIStalk page will be forever frozen on whatever I wrote last (hopefully something decent, unlike good Hollywood actors who died after making an awful last movie as their unplanned swan song). I won’t care at that point. If I quit by choice, I’ll say goodbye.
HIStalk Announcements and Requests

Last week’s reader-requested poll was a good one. Universal interoperability won’t happen until at least 5-10 years (so say 42%) or more than 10 years if ever (46%). Some comments:
- Until you get into the details of turning a clinical note into something transmittable between two systems, you cannot understand the complexity. I remember spending an hour in a meeting discussing what values should be in the “stool appearance” drop-down. Unless every provider uses the same list, or every interface engine has a translation table, how can one system send to the other? Things like that need to be done with thousands of ideas on what exactly a stool appearance drop-down should look like. Of course you can always transmit entire documents and notes, but if you want to make data interoperable, it needs years and clinical revamping.
- Everyone everywhere? From legacy systems run by stressed organizations operating at the margin of survival? Patient-generated data, from outside of hospital/ clinic? Genomic data? Third-party analysis of same? Clinically relevant is the touchstone. Truly clinically relevant may be much smaller subset, but, still, you have to get to it. Patient-sovereign software, leveraging API-architecture through consent / authorization / access services and the patient’s right to their data, may be a route, which works because it flips the paradigm.
- I still vividly remember attending an interoperability conference in 2003, at that time experts were sure that in 5-10 years, all systems would be talking to each other. What year is it now?
- Data exchange will only move forward once EMR vendors and health systems understand they do not own the data, it belongs to the patient. And to get to that point may take payment penalties for those that do not share.
- Ask five physicians what “all clinically relevant data” is and you’ll get seven different answers. The reality is that all all of the data you mention in your example can be shared today. Why isn’t it? Because doctors aren’t demanding it and because there remain competitive business reasons to not share data with providers (aka as competitors) outside an IDN. Interoperability remains mostly a business challenge, not a technology challenge.
- There are aspects that will take longer (e.g., pathology), as today it is not widely digitized. More needs to be done to emphasize the need for the FULL relevant record – too much emphasis still today for making only PAMI (procedures, allergies, medications, and immunizations) data interoperable, as the least common denominator. Finally starting to see more recognition of interoperability needed for clinical reports, which is addressed in the next version of FHIR, but will still take a long time.
- “All” clinically relevant information is casting a wide net, including all scanned documents, waveforms, diagnostic resolution MRIs and mammos and cine loops, and it also assumes that every internal niche clinical system in a large organization can participate in HIE or at least communicate with the primary system responsible for HIE. If that’s what you mean, it won’t happen in 10 years in this country with our broken fragmented healthcare system, and maybe never.
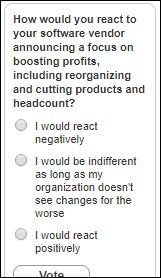
New poll to your right or here: How would you react to your software vendor announcing a focus on boosting profits, including reorganizing and cutting products and headcount? I thought of the question because of Cerner, but we’ve seen plenty of examples over the years and I’m interested in what you think. Comments are welcome, so just click the poll’s “Comments” link after voting.
Dear everyone on LinkedIn and elsewhere: please stop describing yourself as having “over XX years experience.” It’s not like a toddler’s mom or a former addict who feels the need to proudly account for fractional years, so just round up if you are that insecure. Thank you.
Live Nation is offering $20 lawn seats to some mediocre outdoor concerts (mostly 1980s has-beens and country), but I still bought tickets to three of them. It’s worth $20 to create a summer memory of sprawling on the grass while listening to the B52s supplement their Social Security checks by cautiously frugging yet again through “Rock Lobster.”
Thanks to the following companies that recently supported HIStalk. Click a logo for more information.
Webinars
May 21 (Tuesday) 2:00 ET. “Cloud-Based Data Management: Solving Healthcare’s Provider Data Challenge.” Sponsor: Information Builders. Presenters: Jeremy Kahle, manager of planning and business development, St. Luke’s University Health Network; Shawn Sutherland, patient and member outcomes, Information Builders; Bill Kotraba, VP of healthcare solutions and strategies, Information Builders. Inaccurate provider data negatively impacts revenue cycle, care coordination, customer experience, and keeping information synchronized across systems and functions. SLUHN will describe how it created a single version of provider data from 17 sources, followed by a demonstration of how that data can be used in reports and geospatial analysis. Learn how Omni-HealthData Provider Master Edition provides rapid ROI in overcoming healthcare organization provider data issues.
Acquisitions, Funding, Business, and Stock

The former “citizen-scientist in residence” of UBiome – the microbiome testing vendor that was just raided by the FBI after complaints of insurance overbilling – lists Theranos-like warning signs:
- The company didn’t hire a CFO until 2017, then fired him shortly afterward.
- A long list of scientists endorsed the company’s tests, but it’s not clear if any of them ever actually tried them. He says that “too many advisors are really just outsiders with an ego.”
- The company hasn’t released any clinical data despite listing thousands of partnerships with famous research institutes.
- VCs lose money when they back what turns out to be a fraud, but the scientific advisors just walk away from the train wreck unnoticed.
Government and Politics
FDA shuts down its “alternative summary reporting” program for breast implants and says it will eventually extend the shutdown to include all medical device problem reporting. The program allowed manufacturers to submit summary reports instead describing safety incidents individually, thus hiding them from the public eye.
Other
Doctors are using EHRs to identify patients in measles outbreak areas who have not received the measles vaccine. It mentions NYU Langone Health, which has created alerts in Epic that notified doctors and nurses that a patient lives in a ZIP code that is experiencing a measles outbreak. Epic collected customer best practices for dealing with measles and published them into a how-to guide.
A woman who counts on getting emotional support from fellow breast cancer patients from a closed Facebook group complains that people like her are “trapped” after not realizing years ago how cavalierly Facebook manages and sells the private data of its users. She says, ‘’Our group cannot simply pick up and leave … how do we keep the same cycle from repeating on a new platform?” I will, as I often do, take the counterpoint. The group absolutely can leave Facebook and move to a platform that they control. Facebook’s most insidious tactic is hooking users on its wide-ranging services to the point that like Pavlov’s dogs, they will obediently waste hours each day in return for a reward treat that was paid for by those companies willing to buy ads and user data. Use an independent technology platform that isn’t funded by invisible, unethical data practices. Consider whatever cost is involved for the platform and its support to be the price of not having your medical information sold like at a Turkish rug bazaar.

Interoperability expert Grahame Grieve is named the winner of the 2019 John P. Glaser Health Informatics Innovator Award. My most recent interview with him (from March 2019) is here. This is a nice summary by Robert Murphy, MD of UTHealth’s School of Biomedical Informatics:
As a physician and an informatician, I am singularly impressed by Grieve’s focus on pragmatic outcomes derived from a comprehensive array of tactics that are steadily moving us toward interoperability—notably, standards development, implementation, and adoption; open source and tool development and devising interoperability toolkits; enterprise architecture and governance; and clinical document and clinical interoperability solutions. He and his colleagues are extraordinary change agents within healthcare

This seems largely pointless: a new hospital in South Korea will be crammed with tech gadgets that would appear to have zero impact on outcomes or cost – hologram images of isolated patients for “visits,” augmented reality-based wayfinding systems, facial recognition biometric access, and voice assistant-powered patient room amenities. A telecom vendor is co-building the hospital, so naturally it is bragging on 5G connectivity that always seems like hype more than anything. I’m picturing patients wandering around in gowns emblazoned with Nascar-like phone company ads. I am amused that one of Yonsei University Health System’s hospitals is named Gangnam Severance Hospital, which makes me picture Psy being marched off the premises with final check in hand following a musical restructuring.
In England, former hospital CIO Richard Corbridge warns in an op-ed piece that NHS’s digital leaders are leaving for jobs in the private sector, frustrated by health secretary Matt Hancock’s unfunded push for a technology revolution such as “axe the fax.” Corbridge, who just left NHS after 23 years to join Boots as director of innovation, says hospitals can afford only 1% of their budget for IT after the cost of dealing with an aging population, historic underfunding, and staff shortages.

In England, Guinness World Records tells a nurse who ran the London Marathon in scrubs to raise money for Barts Charity that her time won’t qualify as a record for “running a marathon while dressed in a nurse costume” because it requires the uniform to include a dress, a pinafore apron, and a white nurse’s cap. They also advised her that wearing scrubs could confuse people into thinking she’s a doctor. She notes, “I’ve certainly never seen a male nurse wearing a dress to work.” I might take the side of GWR, however, since it isn’t looking for occupational accuracy in certifying records of runners dressed as lobsters or telephone booths (why those records even exist is another issue), with its guidelines cautioning costumed record seekers, “No one wants to run 26 miles dressed as a rabbit only to find out their ears weren’t long enough.”
Sponsor Updates
- Gartner cites Lightbeam Health Solutions in several industry reports.
- Mobile Heartbeat will exhibit at the Kentucky Hospital Association event May 8-10 in Lexington.
- Waystar will exhibit at the Office Practicum 2019 User Conference May 9-11 in Orlando.
- Netsmart will exhibit at LTC 100 May 5-8 in Naples, FL.
- Clinical Computer Systems, developer of the Obix Perinatal Data System, will exhibit at the HIMSS CSO Spring Conference May 10 in Dublin, OH.
- OmniSys will exhibit at the HCP Spring Hospital Pharmacy Conference May 6-8 in Miami.
- Experian Health will exhibit at the NCPDP 2019 Annual Technology & Business Conference May 6-8 in Scottsdale, AZ.
- Redox will exhibit at the Prime Health Innovation Summit May 7 in Glendale, CO.
- Relatient will exhibit at PNW MGMA May 8-10 in Tacoma, WA.
- The SSI Group will exhibit at the Louisiana HFMA Annual Institute May 5-7 in Lafayette, Louisiana.
- Surescripts will exhibit at the NCPDP Annual Conference 2019 May 6-8 in Scottsdale, AZ.
- Hungary’s University of Debrecen joins the TriNetX network to increase collaboration and growth in commercial clinical studies.
- Voalte will exhibit at the Kentucky Hospital Association Annual Convention May 8-9 in Lexington.
Blog Posts
- Harnessing Data Securely, while Managing Privacy (Liaison Technologies)
- Shaping the Future of Healthcare (Vyne Medical)
- Flipping the Script on Supply Chain Savings (Meditech)
- Avoiding Common HIPAA Violations with CC&C (Mobile Heartbeat)
- Experts Share What’s to Come in Home Care and Hospice – Part 5 (Netsmart)
- How to prevent and manage claim denials (Experian Health)
- How has the introduction of telemedicine influenced health outcomes? (PatientBond)
- Enhancing Revenue Cycle Security – Tips from an InfoSec Expert (Patientco)
- Transforming the Physician Experience through EHR Optimization (PatientKeeper)
- 5 Ways to Improve Bundled Payment Care Management (PreparedHealth)
- Digital health is ready for its second act. Will it deliver on its promise to empower patients and providers? (Redox)
- Does Changing Your Practice Management System Mean You Have to Change Patient Engagement Vendor, Too? (Relatient)
- Top Signs You Need a Denial Management Solution (The SSI Group)
- Founder Letter: 6 Ridiculously Simple Ways to Get More Direct Access Patients Today (WebPT)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates. Send news or rumors.
Contact us.











“how do you feel about reps randomly dialing someone up at the hospital hoping for a hit?”
I’ve stopped answering my phone from numbers I don’t recognize. Between the random spammers and vendor spammers, it’s become useless. Some of these vendors even sound a little upset in the VMs that I’m not answering their calls; it’s ridiculous. Don’t even get me started on the email calendar invites.
1: Don’t have voice mail; folks that I work with or, trust have my mobile number.
2: If you schedule an unrequested appointment on my calendar, I drop a note to the InfoSec team and blacklist your entire domain at the firewall.
Wow… It’s going to be a great Monday after reading the way you so deftly wove the conversation from Stool Appearance Drop Down box to frugging through another rendition of Rock Lobster…… On game!
I like to keep it eclectic and thus fun. Anybody can just reword some health IT headlines and add seemingly pithy comments, but I bet few of them would work in a B52s reference. It makes my Monday, at least.
Re: succession plan – not sure anyone could match your wit or deep industry knowledge. The bigger question is do you have an agreement with Lorre, Jenn, or Dr. Jayne to reveal your true identity upon your passing.
I do not have an agreement like that. I won’t care at that point and I doubt anyone else would, either. Mrs. H will have to get her condolences elsewhere!
Hmmm. I’ll speak for some fraction of your readership. Your HIStalk readers are a community of sorts, and we have a relationship with you: there is an easy, conversational manner about your writing that leaves us with the sense we know you, at least a little. Named or anonymous, we would miss you dearly.
RE: how do you feel about reps randomly dialing someone up at the hospital hoping for a hit?
The reality is that a majority of sales professionals aren’t very good at their jobs. If sales professionals are truly making a “cold call”, that means they’re going down a contact list name-by-name without doing research.
I have a tremendous amount of success by calling hospital executives (CEOs, COOs, CNOs), but it takes a considerable amount of planning work. If you’re shooting from the hip and hoping to get lucky — you are making the rest of us look bad.
Look at LinkedIn profiles sales professional in HIT space — typically 1.5-3 year stints. 1 or 2 of these short stints over a long career can be explained (acquisition, RIF, etc.), but if it is a pattern (which is super common to see) then it’s an obvious tell that they aren’t good at selling.
The HIT sales community is super washed up. Lots of old vets that aren’t working to hard..Also many frat bro types who show up to conferences with suit pants altered to show socks (and they expect to be taken seriously by mostly old hospital execs).
I could go on and on, but I enjoy stomping out my competition so will continue to watch them make mistakes.
All of this is 100% accurate. If you fail to plan you plan to fail. Nowhere is that more true with cold calling. The rule of thumb is it takes 10 voicemails left professionally, with info specific to the person you are calling, and spaced out over 2 years before you can break through to an executive or high level management person.
I have been at my current organization for over a year and I don’t know my voicemail password. It is all cold calls.
Also, I have B-52 tickets this summer too. I am psyched.
I’ve been on both sides of the “Cold Calling”. What I have seen and experienced is that there are, in my opinion, appear to be 2 types of businesses that cold call on Healthcare Systems/Executives: Those that have an actual product to sell (an EMR, hardware, computers, software solutions, surgical supplies, etc) and those that sell “professional services” (Consulting Firms or Staff Augmentation Firms mostly). I bring that up as I respond differently to them.
What would be great is to hear from executives on the Health System side to see why they took certain cold calls or responded to certain cold emails? Sales is the life blood of pretty much every single organization and we have all been there before. Yes, its a PITA when sales people call/email non-stop, but at the same time, lets take the opportunity to help the next generation improve. We are all busy, I get that, but you can find 5-10 minutes every single day to respond and educate.
Personally, I set aside about 30 minutes a day to respond to Sales Emails/Calls. I would say 70% of my responses are basically Thanks but No Thanks, however, every now and again, I find an interesting product or service.
Now, the issue I run into the most is responding to Consulting Firms / Staff Augmentation firms. And the end of the day, they are all the same at their core, selling the same resources that other firms sell (Hey I hear you have an upgrade coming up, I have Epic/Cerner/MEDITECH resources that can help). The truth is, these firms get the “needs” and then literally all reach out to the same candidates, it is whoever is willing to “sell them” for less that usually wins. How do many of my fellow HIT execs handle those cold emails/calls?
Mr. Kamikaze, or should I say “tough guy”, in case you haven’t noticed while you sit in your office not taking phone calls, healthcare in the U.S. is a mess and perhaps your attitude contributes to that. There’s a lot of very professional sales people out there selling products designed to help your health system solve problems, to get better, to etter care for patients, to improve processes, to drive more revenue.
Your industry is being disrupted while you sit in your office not taking phone calls from dreaded vendors trying to help and the way it is going it is going to be disrupted in such a way that places like hospitals may take on a different role and guys like you may be on the sidelines looking for a new job.
How do you ever really learn about anything new without talking to people?