Thomas told me when he submitted his article that it was OK if I didn't run it because people generally…
EPtalk with Dr. Jayne 10/26/17
I had some additional adventures in patient-land this week when I went for a trip through the MRI scanner. Although it wasn’t a portal to adventure like some of the pediatric imaging suites I’ve seen, it did have its moments. The radiology department was running behind schedule due to short-staffing, which they promptly attributed to the hospital’s upcoming Epic go-live. Apparently, they need to get all the technicians through the training by the end of the month in order to meet the required training timelines. I was having a fairly specialized study that must not be done very often, and the only technician trained for the positioning needed was working in the emergency department, so I had to wait for her to arrive despite having been on the schedule for weeks. The study went off without a hitch, although you know you’re sleep-deprived when you sleep through your MRI despite all the banging noises. When it was time to assist me off the table, the tech let slip that she was glad the images turned out well because it’s the first time she’s performed this particular study. Not a confidence builder but I’m glad my results were unremarkable. I get to do it again in a year, so hopefully they’ll be through their Epic issues and have a little more experience with specialized MRIs under their belts.
![]()
The ONC Annual Meeting is coming up, from November 30 to December 1 in Washington, DC. This year’s theme is “Tackling Barriers to Interoperability and Usability.” After a keynote from the National Coordinator, attendees can choose from a variety of breakouts on topics such as the Trusted Exchange Framework, standards, data infrastructure for patient-centered outcomes research, and reducing provider burden. There will also be a panel discussion on improving health IT usability. The hotel block expires Sunday, so make your reservations now.
I had to take some annual training this week for one of my clients, including HIPAA, fraud and abuse, harassment, and a charming refresher on how to use fire extinguishers. There were a few other courses required of all hospital employees and contractors. Fortunately, I could do them online while watching my favorite new show on Netflix, The Doctor Blake Mysteries. The HIPAA course reminded me of a recent article about a Capitol Hill pharmacist who commented publicly about some of his prominent patients, although he later retracted this to say he was talking speculatively. In addition to serving Congressional staffers and lobbyists in the community, his pharmacy delivers medications to the Capitol’s Office of the Attending Physician. Even if he was joking as he says he was, it’s a bad idea for a healthcare professional to put himself in this type of position.
I had never heard of the Office of the Attending Physician before the article, which apparently serves as a mini-concierge practice staffed by Navy physicians, nurses, and ancillary personnel. Lawmakers pay around $600 annually for the physician services, although the prescriptions are billed to insurance like they would be for any other patient. The Office has an annual budget of $3.7 million, which is certainly more than many of the primary care physicians I know who are carrying thousands of patients in their panels. The article mentions that the Office doesn’t yet use e-prescribing, which most of the rest of us have been forced to adopt, but rather that the physicians call prescriptions to the pharmacy by phone, which slows his business.
The justification for the Office is to allow lawmakers to receive care without interrupting their busy schedules, but I think that maybe if our legislators had to juggle physician visits like the rest of us do, they might be more sympathetic to the plight of the average patient. If they had to wait for physicians who were running late due to multiple competing priorities, overloaded panels, and clunky EHRs, they might have a different feeling about mandating how physicians practice. And if they had to sit on hold while making an appointment, then wait a few weeks for the visit, put in a time-off request, take off work, hand-off their responsibilities to a co-worker, clock out, sit in traffic, and barely make it to the office on time for their appointments, they might have a better understanding of the healthcare system they’re trying to fix legislatively.
Speaking of who should tell physicians and other healthcare professionals how to practice, I enjoyed this piece by New York Times op-ed writer Sandeep Jauhar. I had previously enjoyed his book “Doctored” about physician disillusionment, and so was interested to hear his thoughts on whether physicians or business leaders should make decisions about care in our hospitals. He notes that 90 percent of the nation’s hospitals are run by leaders without medical training, along with the increasing focus on profitable service lines regardless of the general medical needs of a community’s patient population. I’ve seen that in my own city where hospitals compete brazenly for orthopedic and cardiac procedures while running other service lines with a skeleton crew.
Jauhar notes that physicians are partly to blame for their loss of authority at hospitals: “If we had taken better care of our institutions, perhaps there would not have been a need for others to manage them for us.” It’s something to think about as we consider the many forces impacting patient care, not only for physicians but for other clinicians – we have lawmakers, payers, regulators, attorneys, accountants, and technology vendors driving our interactions with patients and with our peers. It’s certainly not going to get any better unless we do a better job advocating for our patients, our colleagues, and ourselves.
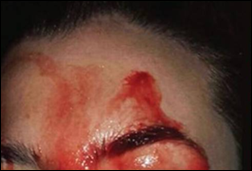
Weird news of the week, just in time for Halloween: A patient is diagnosed with hematohidrosis, a condition in which she literally sweats blood. The write-up appeared in this week’s Canadian Medical Association Journal. With only 18 documented cases in the last five years, it’s not surprising that we haven’t heard more about it, but it’s a condition you certainly wouldn’t miss if you ever came across it.

Email Dr. Jayne.


Your observation about legislators’ disconnect from the real world of getting medical care is on the mark. I frequently remark to patients after their visit with me that now they need a travel agent, not a doctor, and that scheduling everything and gathering all the papers will take longer than our time in the exam room. Further, this is not how doctor shows on TV show things. . .of course, we all know there were no nurses in House’s mythical Princeton hospital, either.
Wow, that observation on the lack of nurses is…amazing. I watched the show for a while but got pretty weary of the ‘brilliant jerk’ trope, but that never really sunk in. Contrast that with ER, which had its own set of flaws and absurdities, but where the nurses were ever-present.