Best Practices Coming Soon to a Virtual Visit Near You
Top telemedicine vendors weigh in on a recently published study calling for them to share best practices.
By @JennHIStalk
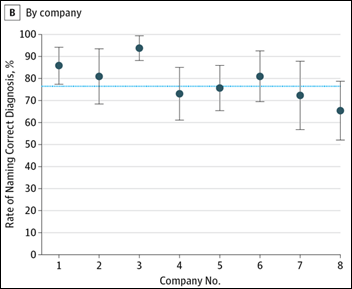
A recent JAMA-published study comparing quality of care among six telemedicine vendors highlights the growing pains that this evolving method of healthcare delivery seems to be going through. The clinical variation found in the virtual visits – ranging from asking the proper questions and performing the correct examination steps to ordering medically indicated tests – prompted researchers to recommend that telemedicine vendors share best practices.
It’s a novel idea, one that suggests telemedicine is ready to move from its awkward “tween” phase to becoming a more mature and collaborative force. Would sharing best practices reduce clinical variation? Do telemedicine vendors or other stakeholders foresee improved patient care (or the chance to market themselves better) if they were to follow standards and share best practices? Would such collaboration even be feasible?
These are the questions that will drive telemedicine stakeholders — including payers and organizations like the American Telemedicine Association (ATA) — to the next phase of market maturity.
Aren’t We There Yet?
Some may argue that telemedicine already has standards in place. They would be half right. Most if not all vendors have their own internal set of guidelines and clinical best practices, in addition to those published by the Federation of State Medical Boards and the American Medical Association (AMA).

Doctor on Demand, for example, implemented protocols from Day One that include a double-blinded peer review, daily visit feedback, and an antibiotic stewardship program.
“We employ our doctors, which I think is a big differentiator,” says Doctor on Demand Chief Medical Officer Ian Tong, MD. “For instance, we couldn’t do our peer review program with a group of independent contractors who are just getting on our platform periodically to make some extra money and moonlight. That’s much more difficult to do.”
“The way that we leverage technology allows us to monitor a number of things,” he adds, “including duration of the visit, idle time for the doctor, and patient satisfaction scores. We can aggregate that information and give our physicians feedback, letting them see patient comments at the end of every day.”
“Am I ready to say that everything I just listed is the best practice?” Tong asks. “Not yet, but I doubt anyone’s doing more. I can tell you that brick-and-mortar practices don’t do half the things I just listed. Eventually those may lead to the development of best practices, but you have to go through a certain amount of market maturity.”
Getting Past the Growing Pains

Most telemedicine vendor executives agree that market maturity is a work in progress and that shared best practices won’t become the norm until the average consumer, employer, and even payer sees the benefit in virtual care.
“We wholeheartedly believe that absolute transparency in best practices and lessons learned from mistakes are key to allowing this industry to move forward responsibly,” says American Well President and CEO Roy Schoenberg, MD, MPH. “The biggest hurdle to telemedicine is the still prevailing misconception of what it can do and the operating know-how of how to make it a safe extension of traditional care delivery.”

Scaling telemedicine’s potential in terms of user acceptance and technical capability is top of mind for the entire market right now. “The industry is in its infancy based on the market potential,” explains Teladoc Chief Medical Officer Henry DePhillips, MD, who adds that the market potential for telemedicine visits is about 550 million interactions annually. “We’re predicting that we’ll do 900,000 visits this year,” he says, “and so we’re just barely scratching the surface of the market’s potential, which has a lot to do with why, up until now, best practices have not yet been established.
“A misstep by any of the vendors in the space will potentially have a negative impact on the entire industry, not just that particular vendor,” DePhillips adds. “I think it’s incumbent on all of us to have really high standards for clinical quality of care, patient safety, reporting, record keeping, and patient experience because the industry needs to keep moving forward.”
Third Parties Attempt to Take the Lead
It’s not for lack of trying that a nationally recognized set of telemedicine best practices has not been created and adopted among stakeholders. Organizations like the ATA, Health Information Trust Alliance (HITRUST), National Committee for Quality Assurance, and URAC (formerly known as the Utilization Review Accreditation Commission) have attempted to drive the best practices conversation via certification programs.
Tong sees immense value in attaining third-party accreditations, and points out that Doctor on Demand has certifications from ATA, NCQA, and HITRUST, “which is really important, but not as sexy. That involves the security of your health records and platform. I think that’s actually a pretty high bar, to be honest. A lot of hospitals don’t have all three of those certifications.”
Teladoc has pursued similar recognition and was the first telemedicine vendor to achieve NCQA recognition. “There are a number of players in the industry that want to be seen as the stamp of approval for the telemedicine industry,” DePhillips says. “I think they’re all heading in the right direction in raising the bar on patient safety and care quality, but I don’t think any of them have really figured out how to dominate that part of the industry yet.”
He does see potential in some kind of Energy Star-like stamp of approval for telemedicine. “I think the concept of having trusted third-party validation is correct,” he explains. “End users will eventually look for that. We actually display the NCQA logo on our website. I think that it will help business. It’s just a matter of which third party you want to hang your hat on at the moment. I think the players, from the stamp-of-approval standpoint, are probably going to shift over time.”
Schoenberg is in accord with his competitors, adding that telemedicine’s eventual stamp of approval will need to have two parts – “approval for the quality and safety of the platform used and a recognition of the quality of the clinical service, which will be implied by the already familiar brands offering it, e.g. Blue Cross Blue Shield, UnitedHealth, Cleveland Clinic, etc.”
Competitive Collaboration is Key for Now
While stakeholders wait for the gold standard of telemedicine certification to emerge, vendors like those reviewed in the JAMA article have focused on collaborating with each other to ensure best practices are shared in the interests of all.
“Although we compete for customers, we collaborate in many ways,” says DePhillips, noting that Teladoc is a member of the ATA and Alliance for Connected Care, a DC-based think tank that includes other broadly defined telemedicine companies. “When it comes to regulatory, care quality, and/or patient safety issues, there’s actually a lot of collaboration among at least the top-tier telemedicine companies,” he adds. “I actually have a professional relationship with my counterpart at our primary competitors. We’ll get together occasionally and talk about how we can work together to solve regulatory issues, most of which are in the past. In some cases, some of the companies will pool funds to help with a regulatory issue. We will not pool resources, but we’ll have a pretty good, detailed conversation around the best approach to patient safety, what standards are out there from the various specialty societies, and what we should be following as an industry. Like I said, a rising tide truly raises all ships. That’s the industry we’re in, especially at this level of maturity.”
Vetting Vendors in the Meantime
For now, potential users will have to use their best judgment in selecting telemedicine services for their members, employees, or themselves. In addition to the certifications mentioned, Schoenberg, Tong, and DePhillips have their own must-haves and red flags for vetting vendors.
“Video visits are a must,” says Tong. “It’s also important to look at the quality of the physicians. What are the hiring practices and training regimens? What are the quality assurance programs that practice has in place? They may not all want to give you their secret sauce, but I think it’s very reasonable to ask, ‘How do you do that?’”
DePhillips believes that, in addition to quality and patient safety assurances, potential customers should look at three key things. “When I look at the younger, smaller players in the industry, I find that they tend to cut corners in two areas. Number one is the way in which they put their provider network together. There’s no other company besides Teladoc that has licensed providers that are physically present in all 50 states. A lot of this cross-state licensing discussion is a non-issue for us. It’s heavy lifting and it’s expensive, but we chose to do that because we think it’s the best route to take. Vendors should also have the infrastructure to support future adoption and to scale.”
Schoenberg’s advice takes a more high-level approach: “First, map out all that you want to do with telemedicine — urgent care, follow-up care, provider-to-provider consults, etc. — and ask the vendor to show you how they can support it. Then, map out all of the systems you will need those services to integrate or exchange data with, and ask the vendor to show you how they can do that. Then, think of what it will take to roll out to all involved – patients, providers, payment stakeholders, marketing, actuaries – and ask the vendor to show their depth of understanding of what needs to be done to be successful in each. Finally, look for leadership you can trust to keep you ahead of the curve as the world of delivering healthcare via technology explodes forward.”




TBF the anti-hate non profit was funding undercover investigators trying to being down the KKK & has done successfully for…