It's really hard to take seriously these studies targeting "misinformation." Clearly there's some bad stuff out there, like people claiming…
News 7/12/13
Top News

DoD and VA officials tell the House Armed Services and Veteran Affairs Committees that they will focus on creating a system that will display standardized information from both organizations instead of pursuing an integrated health record now estimated to cost $28 billion. DoD also announces that it will tender bids for replacement of its AHLTA, CliniComp Essentris, SAIC CHCS, and TMDS systems. Video of the hearing is here, although a lot of it involves the famous claims backlog. The DoD people are grilled at around 45:00 as to why they are ignoring the President’s mandate for an integrated record and are instead off shopping commercial software for themselves. The answer is not nearly as direct as the question, although in an interesting moment, DoD Undersecretary Frank Kendall disputes a quote about his department’s intentions and criticizes the source as “entirely incorrect,” only to be told that the quote came from the Secretary of Defense.
Reader Comments

From Lance Boyles: “Re: HCA. Just consolidated its IT staffing vendor list to just Zycron, Robert Half Technology, and Insight Global. TEKsystems, shockingly, did not make the cut even with its long-term, high-value corporate relationship.” Unverified.
From Punditry: “Re: Senate Finance Committee. Has called Farzad Mostashari, MD from ONC and Patrick Conway, MD from Center for Clinical Standards and Quality to testify at a July 17 hearing called Health Information Technology: A Building Block to Quality Care.”
From Fresh: “Re: CIOs fired during or after an Epic install. I was curious on your take.” CIOs do indeed get fired during or after their installs of Epic … and Cerner, Allscripts, Meditech, and every other system out there. My take:
- You hear about the Epic ones because, by definition, they are the highest-profile hospitals and CIOs, and the high cost of their implementation projects increases the risk of being made a sacrificial lamb when things don’t go smoothly.
- Epic takes quite a bit of time to install because it’s usually replacing most major systems, and with CIO turnover being what it is, there’s a good chance that some CIOs will leave in those years purely by chance.
- Some hospitals want an Epic-experienced CIO knowing the many millions of dollars that are at risk and — either at their own initiative or because Epic identifies potential problems — decide to make a change.
- I would hope that hospitals don’t put the CIO in charge of the project since that’s a big mistake, but I would also hope that the CIO and IT department don’t let the Epic train roll over them by being anything but ecstatic over a project that has already been embraced with possibly irrational exuberance by operational leadership.
- When you read about high-profile Epic failures, I would bet you any amount of money that the risks were spelled out well in advance in the extremely detailed (and blunt) executive status reports that Epic provides regularly, which means the facility probably either ignored its recommendations or wasn’t functional enough to fix the noted problems. If those chips fall on the CIO, hilarity will not ensue.
From Deep Thoughts: “Re: EHR usability. It’s one piece of a complex puzzle. I’ve worked with EHRs that are loved by physicians, but lack basic capabilities, like allergy checking if a medication name is spelled wrong. Per this quote about the stethoscope from 1834, there is resistance to change, and the key is channeling it into systemic improvements.” The 1834 stethoscope quote: “It will never come into general use, not withstanding its value; it is extremely doubtful because its beneficial application requires too much time and gives a good bit of trouble both to the patient and the physician because its character is foreign and opposed to all of our habits and associations.”
HIStalk Announcements and Requests
![]() Recent highlights from HIStalk Practice include: a reader wonders how EMR requirements differ between small and large practices. The American Academy of Ophthalmology will implement an eye disease patient database. A third of physician executives think healthcare costs rise when hospitals buy physician practices. CMS proposes paying providers for non-face-to-face care of patients with multiple chronic conditions if the provider uses a certified EHR. ONC’s Farzad Mostashari, MD predicts an uptick in full EHR adoption in 2014 just before providers risk penalties for not meeting MU standards. Federal financial incentive programs have spurred e-prescribing adoption. Brad Boyd of Culbert Healthcare Solutions offers recommendations to avoid impacting cash flows when prepping for ICD-10. Reading HIStalk Practice may not be a cure for the summertime blues, but it is a cool way to catch up on the latest ambulatory HIT news. Thanks for reading.
Recent highlights from HIStalk Practice include: a reader wonders how EMR requirements differ between small and large practices. The American Academy of Ophthalmology will implement an eye disease patient database. A third of physician executives think healthcare costs rise when hospitals buy physician practices. CMS proposes paying providers for non-face-to-face care of patients with multiple chronic conditions if the provider uses a certified EHR. ONC’s Farzad Mostashari, MD predicts an uptick in full EHR adoption in 2014 just before providers risk penalties for not meeting MU standards. Federal financial incentive programs have spurred e-prescribing adoption. Brad Boyd of Culbert Healthcare Solutions offers recommendations to avoid impacting cash flows when prepping for ICD-10. Reading HIStalk Practice may not be a cure for the summertime blues, but it is a cool way to catch up on the latest ambulatory HIT news. Thanks for reading.
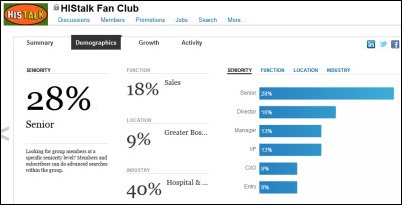
Earn HIStalk Karma Points by: (a) signing up for spam-free e-mail updates; (b) searching or navigating your way to finding the offerings of HIStalk sponsors in the Resource Center; (c) finding a consulting firm painlessly by blasting your quickly-entered RFI to the companies of your choosing – including all of them as an option – via the Consulting RFI Blaster; (d) connecting with us on Facebook, Twitter, and LinkedIn, including the HIStalk Fan Club that reader Dann set up in 2008 (happy five years, Dann!) that now has 3,200 members; and (e) sharing my amazement at the impressive roster of industry-leading companies that support HIStalk by perusing and occasionally clicking their ad to your right and telling them in person that you saw them on HIStalk. Thank you for reading, with extra gratitude to that handful of readers who were there with me when I started writing HIStalk in June 2003.
Actually, there may be more than a handful of 10-year readers out there, so if you’re one and would like to tell me how you found HIStalk in 2003 and why you’ve kept reading, that would be fun.
On the Jobs Board: Health Analytics Data Analyst, Senior Healthcare Policy Analyst, Marketing Specialist, Systems Administrator.
HIStalk Connect’s Dr. Travis and Kyle were at the Converge conference in Philadelphia this week, with Kyle on the right sporting Google Glass and Travis jealously wishing his plain old optical glasses were half as cool. A report from Travis is here.
Acquisitions, Funding, Business, and Stock
Allscripts announces that it expects Q2 bookings and contract backlog to increase 3 percent and 13 percent, respectively. That includes the just-announced $400 million services extension by North-Shore-LIJ Health System, which provided important validation that the company can meet the needs of a large health system.
In the same SEC filing, Allscripts announces that EVP of Sales Steve Shute, who joined the company in July 2011, will resign effective August 8, 2013 and will receive as severance his expected one-year compensation of $880,000.
Sales
Kindred Healthcare (KY) selects dbMotion create a single patient record.
Medical Center Hospital (TX) chooses Convergent Revenue Cycle Management.
Gundersen Health System (WI) will implement iSirona’s device connectivity solution.
The Specialty IPA of Kansas retains Wellcentive to facilitate clinical integration, manage P4P programs, and support its integrated network of primary care physicians.
People
Health Catalyst names Scott Holbrook (Medicity/KLAS) as a strategic advisor.
Bill Korn (Antenna Software) joins MTBC as CFO.
Scripps Health names Steven Steinhubl, MD director of its Digital Medicine program, tasked with leading the scientific evaluation of mobile health devices through the Scripps Translational Science Institute.
Systems Made Simple elects CFO Christopher Roberts to its board.
Acusis appoints Robert Parsons (Cerner) VP of strategic business solutions.
Announcements and Implementations
Nuance announces that 750 developers have joined its healthcare developer community.
The health IT program at the University of Texas at Austin and Jericho Systems will participate in an ONC-approved national pilot to explore advanced patient control over shared medical records and how patients can better control the release of their PHI when requested electronically from their providers.
Government and Politics
ONC issues an ONC Certified HIT mark for EHR technology that has 2014 edition certification requirements.
The HIT Policy Committee’s Information Exchange Workgroup issues preliminary recommendations on patient record queries and provider directions for Stage 3 MU.
Innovation and Research
Healthbox partners with BlueCross BlueShield of Tennessee to launch a new health IT accelerator in Nashville, joining its locations in Chicago, Boston, and London. The first class will start in September at the Nashville Entrepreneur Center.
Technology
Pixie Scientific develops a diaper that works with a smartphone app to detect possible UTIs, kidney dysfunction, and dehydration, transmitting its findings to a physician. The developers say the diaper also has potential as a consumer product and would likely cost about 30 percent more than regular diapers.
![]() In contrast to the simple genius of this diaper, I was reminded yesterday just how far behind healthcare is. My new insurance carrier offers online access to an electronic image of the insurance card. I thought it was semi-brilliant of me to take a photo of the online image with my iPhone instead of printing it. It was easy to hand the pharmacy tech my phone so she could enter the numbers into their system. The doctor’s office, however, requires the actual card so they can scan it into their system. I would have been pleased two years ago to have my card scanned for a computer system instead of photocopied for a paper chart. Today I am annoyed because the doctor’s office was unable to think outside the box and accept my electronic copy.
In contrast to the simple genius of this diaper, I was reminded yesterday just how far behind healthcare is. My new insurance carrier offers online access to an electronic image of the insurance card. I thought it was semi-brilliant of me to take a photo of the online image with my iPhone instead of printing it. It was easy to hand the pharmacy tech my phone so she could enter the numbers into their system. The doctor’s office, however, requires the actual card so they can scan it into their system. I would have been pleased two years ago to have my card scanned for a computer system instead of photocopied for a paper chart. Today I am annoyed because the doctor’s office was unable to think outside the box and accept my electronic copy.
Other
A HIMSS Analytics survey finds that network/architecture support and security are the jobs that most often require industry certification.
Indiana University School of Medicine and Regenstrief Institute endow a chair to honor informatics pioneer and LOINC inventor Clem McDonald, MD (left in the photo above). The first Clem McDonald Professor of Biomedical Informatics is Titus Schleyer, DMD, PhD, MBA, director of the Regenstrief Institute (right in the photo above).
HHS fines insurer WellPoint $1.7 million for exposing the medical information of 600,000 people in 2009-2010 due to Internet server security issues.
Texas Health Harris Methodist Hospital Fort Worth notifies several hundred thousand former patients that their medical information from the 1980s has been exposed when several microfiche pages are found in a park. The hospital says its disposal contractor, Shred-it, didn’t.

Friends of industry long-timer Milton Antonakos, who died along with his family in a plane crash in Alaska earlier this week, are welcome at a remembrance get-together at the Columbia, SC offices of Allscripts on Friday, July 12 (today) at 3 p.m. Inga will provide the RSVP information and location details if you e-mail her.
Citizens of a small town in Canada whose only doctor will be away on his honeymoon for six weeks are offered telemedicine services in the interim by the province to mixed reaction. According to one resident, “I did the doctor camera thing. Basically I diagnosed myself and he gave me a prescription. It was pretty impersonal.”
PCWorld, the only remaining print edition consumer computer magazine, publishes its last paper issue to focus on its online and digital editions.
Healthcare isn’t behind in technology, we’re just on the leading edge of security. The Kremlin, panicked by the release of electronic secrets by WikiLeaks and Edward Snowden, issues an RFP for electric typewriters of the specific German model above. Retro-secure fax machines and pagers can’t be far behind.
Sponsor Updates
- Covisint expands its partnership program to enable organizations to resell, refer, or white-label Covisint Identity Services.
- Beacon Partners will provide consulting expertise to help organizations using Information Builders’ BI and analytics solution.
- Marshfield Clinic Information Services subscribes to the Capsite Database to assist with health technology procurement and purchasing.
- CIC Advisory launches a blog entitled, “Think.Learn.Care.” or TLC, which profiles hospital leaders who are effectively using technology to improve the efficiency and effectiveness of patient care.
- Emmi Solutions selects Truven Health Analytics as its preferred partner provider of patient discharge instructions.
- Quest Diagnostics provides access to de-identified hepatitis C test results from its Health Trends national clinical laboratory database to the CDC for public health analysis.
- T-System publishes an infographic depicting the MU history of its EV product.
- University of Florida Health and Florida Hospital securely exchange PHI with the Florida HIE Patient Look-Up Service developed by Harris Corporation.
- O’Reilly Strata RX Conference posts the schedule for its September 25-27 conference.
- Surgical Information Systems discusses the role of IT in quality reporting.
- Billian’s HealthDATA Jennifer Dennard takes on Google and inaccurate hospital data.
- TeleTracking Technologies looks at patient care satisfaction and its impact on an organization.
- SpeechCheck’s Ken Schafer discusses the importance of accurately recording narrative data within the EHR.
- Advanced Medical Imaging (CO) discusses how it increased point-of-care patient collections by 315 percent within a year of implementing ZirMed’s Patient Estimation solution.
- Verisk Health announces details of its annual conference September 18-20 in Orlando.
- Optum’s CMO Miles Snowden, MD discusses how to navigate the journey from providing care to managing health.
- HMC HealthWorks will integrate the Healthwise Care Management solution into ProGuide, the HMC care management platform.
EPtalk by Dr. Jayne
Alberta Children’s Hospital has deployed a robot named MEDi to aid children receiving flu shots. Those who engaged with the robot reported less pain and distress than those who didn’t. The study involved 57 children with moderate to severe fear of needles. In addition to distracting patients, the robot also provides instructions for relaxation and deep breathing.
Nearly a third of “Pioneer” ACOs may opt out, with some joining the Medicare Shared Shavings Program instead. Some have been threatening to do so since a dispute over measures in March. Although CMS did make some changes, it may not have been enough. Pioneer ACOs have until next Monday to notify CMS of their plans to leave that model and until July 31 to apply for the Shared Savings Program.
Health Affairs looks at the reasons poor patients prefer hospitals over office-based care. Researchers from the University of Pennsylvania documented patterns where patients using less preventive care were more likely to become acutely ill and/or require hospital care, costing over $30 billion each year. Reasons cited by patients included hospitals being less costly and more convenient with better quality care. That’s a sad commentary on our clinic and safety net ambulatory systems.
Congratulations to HIStalk contributor Ed Marx, who reached the summit of Mt. Elbrus in Russia earlier this week.
Thanks to everyone who sent good wishes for my laboratory orders go-live this week. It went fairly well and the phone lines were pretty quiet. We rarely receive compliments, but sometimes not hearing complaints is enough to know we did the job right. It’s been a tiring week, nevertheless, so I’m keeping tonight’s piece short and going to bed early.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.


















RE: CIOs Fired after installing Epic
Mr. H, I think you are being very generous to Epic in giving a lot possibilities where it is the hospital fault or the CIO fault or no party fault at all but not giving any possibility where Epic or the Epic model is the cause.
Is it possible that Epic’s status reporting model and the focus on selling the Docs and the CEO or the significantly higher ongoing IT cost causes a disproportionate amount of CIOs at newly Epic hospitals to lose their jobs?
So lets do some math. Allscripts + LIJ + EVP sales leaving = CIO keeping job problem. The SEC should take a hard look at this, because most knowledgable people in the industry know that the full amount of the contract will not be realized.
There’s a joke going around – how many CIO’s does it take to install Epic? Three: 1 to buy, 1 to install, 1 to optimize. Never heard that with other EHR vendors. Hope other Epic CIO will chime in here – I agree with you 99% of the time, but not on this one. Epic is simply a different proposition (and I worked with most of them). There are many reasons – I’ll give one: Epic’s intense focus on “it’s not an IT project” often puts an operational person in charge of implementation (fair enough), but then leaves the CIO out. The CIO (because they’ve implemented lots of software) is left to tell some inconvenient truths, e.g. Epic tends to way-underestimate costs – especially post-live. There’s several recent post-lives in trouble right now… CIO’s, is that your fault? Weigh in.
Btw, if I were buying an EHR, I’d buy Epic – I think they’re the best – but would do so with eyes wide open.
Epic CIO’a – John M covered a few salient points. Of which, the “it’s not an IT project” rallying cry… let’s face it. It IS an IT project. What in the Sam Hill is the project about anyway? You can talk “transformation” all you want. You start with a massive software install. Period. Then when you put some operational schmuck in charge of the project that cannot even spell IT, what do you think is going to happen? When you tell senior leadership that even after you a live that this is nothing more than any other platform IT already supports, they look at you like you have gills and a tail. The hype around an Epic install is just ridiculous. I think it is only there to get past the large price tag, not only for the implementation, but for ongoing support. Who talks about the impact of cost and support after the go live when you are taking the rah-rah proposal to the board? Exactly. Then the CFO wants to reduce the “inflated” team by 20-30% and when you tell them you cannot support the environment with less than what you have, their head explodes. While I think Epic has good software and a solid implementation methodology, their lack of being transparent across the board in making sure the customers realize what they are getting into is reprehensible. The 3 CIO joke is not a joke at all. I can point to several places where this is a reality. There are outstanding CIO’s that have been victimized by the blindness and ignorance of organizations installing Epic. And Epic is contributing to this and they know it.
Re: Justa CIO
I don’t understand why organizations that have your mentality are buying Epic. It’s like hiring a doctor to do the work of a medical assistant – it’s a waste of time and money for all parties involved. If your organization isn’t ready to rethink how EMRs will affect your workflows, you guys aren’t ready to implement one.
looks like one hospital of HCA is trying Epic out at Utah…once they see it cost 5X other vendors and by the time its optimized it will be outdated like a flip phone.
“…their (Epic’s) lack of being transparent across the board in making sure the customers realize what they are getting into is reprehensible. ”
Tru Dat
All the people throwing around the “high costs” doubtfully worked in any place that had 24x7x365 supported CPOE, allied health, nursing and physician documentation, all key departments automated, and real data flowing to the registration, scheduling, and billing systems in both inpatient and ambulatory settings. It costs money – can we overpay someone to study that with our tax dollars and share it with the uninformed? Who knew their real total cost of technology and services before a full implementation? The costs are typically spread over many cost centers, accounts and entities within an organization. Until you compare the costs before and the costs after on the same scope of services and applications, one isn’t arguing from facts.