I'd never heard of Healwell before and took a look over their offerings. Has anyone used the products? Beyond the…
News 3/29/13
Caradigm will integrate Orion’s HIE solution with its Caradigm Intelligence Platform (CIP, formerly Amalga) and resell the Orion product. Orion will resell and provide services for CIP and Caradigm’s identity and access management solutions in New Zealand, Australia, and certain Asian countries. Orion will also develop decision support, population health, and quality improvement for CIP and promote CIP to its HIE prospects and customers. Caradigm has also decided not to commercialize the Qualibria knowledge solution product and will instead incorporate it into CIP, which will result in elimination and reassignment of an unspecified number of employee positions in product planning and engineering operations. The Salt Lake City newspaper says 70 percent of the company’s Utah employees, about 40 to 50 people, were laid off Wednesday.
Reader Comments
From Jasmine Gee: “Re: athenahealth’s attestation numbers. To answer readers’ doubts about how many of our Medicare Part B physicians using athenaClinicals are participating in MU, the answer is about 70 percent. That’s over 5,000 total Medicare Part B physicians. The remaining 30 percent are Medicare Part B physicians who bill so few Medicare claims that their incentive check would be tiny, so they’ve declined to pursue Medicare MU. Remember: the maximum Medicare MU incentive payment is 75 percent of billed Part B charges for the program year, with a cap based on when you start.” Jasmine is the product marketing director for athenaclinicals and was responding to recent comments from readers questioning the legitimacy of athenahealth’s claim that 96 percent of its participating providers have successfully attested for MU.
From ForEclipsii: “Re: delayed go-live at the new Royal Adelaide Hospital in Australia. I believe that the application in question is actually the brand-new Sunrise Financial Manager which rolled out a few months ago. People working on it were told to drop everything and work on a version for Australia.” Unverified, but that makes sense based on the newspaper article, the mention of billing issues, and the earlier Allscripts contract.
HIStalk Announcements and Requests
![]() We opened a HIStalk Practice reader survey, which is different than the HIStalk survey we ran a couple of weeks ago. If you are a HIStalk Practice reader (and you should be!) please take 60 seconds to give us your input. Thanks.
We opened a HIStalk Practice reader survey, which is different than the HIStalk survey we ran a couple of weeks ago. If you are a HIStalk Practice reader (and you should be!) please take 60 seconds to give us your input. Thanks.
![]() Some of the HIStalk Practice goodies from the last week include: hospital-owned physician practices in Kentucky are losing as much as $100,000 per year per doctor. The Wall Street Journal examines patient-physician e-mail communications. The NCQA extends its PCMH recognition program to specialty physicians. The average turnover for physicians in 2012 was 6.8 percent, compared to 11.5 percent for PAs and NPs. Michael Brozino, CEO of simplifyMD, discusses his company, its technology, and the state of the EMR industry. DrFirst President G. Cameron Deemer shares insights on e-prescribing, EMR vendor consolidation, and the impact of government incentive programs. Take a moment and click on an ad or two – one of our sponsors may have a product or service that makes your life better. Thanks for reading.
Some of the HIStalk Practice goodies from the last week include: hospital-owned physician practices in Kentucky are losing as much as $100,000 per year per doctor. The Wall Street Journal examines patient-physician e-mail communications. The NCQA extends its PCMH recognition program to specialty physicians. The average turnover for physicians in 2012 was 6.8 percent, compared to 11.5 percent for PAs and NPs. Michael Brozino, CEO of simplifyMD, discusses his company, its technology, and the state of the EMR industry. DrFirst President G. Cameron Deemer shares insights on e-prescribing, EMR vendor consolidation, and the impact of government incentive programs. Take a moment and click on an ad or two – one of our sponsors may have a product or service that makes your life better. Thanks for reading.
On the Jobs Board: Senior Director Clinical Project Management, Product Manager, VP of Sales and Channel Development.
I’m looking for someone who can help produce Webinars and perhaps do some other paid part-time work. Industry experience would be nice but probably isn’t essential, although excellent writing, speaking, marketing, and organizational skills are. E-mail me.
Acquisitions, Funding, Business, and Stock

ReadyDock will receive $150,000 in pre-seed funding from Connecticut Innovations to continue development and marketing of its devices for disinfecting, charging,and storing computer tablets.
Bankrupt Raleigh, NC-based EMR vendor E-Cast, which had annual revenue of $4 million as late as 2006, is winding down after the business is sold to Global Record Systems LLC for $100,000.
Sales
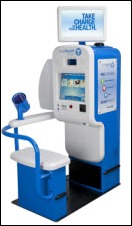
Safeway will roll out the SoloHealth Station kiosk to 700 of its stores, giving customers access to free health screenings and personalized assessments.
Kettering Health Network extends its relationship with MedAssets for its revenue cycle management and workflow services.
Philips earns a fourth-year option worth $77 million to provide patient monitoring systems and training to the Department of Defense.
Lahey Health (NH) announces officially that it has signed with Epic, which will apparently replace Allscripts in both its hospitals and practices.
People
MEDHOST hires Barbara Bryan (Bryan Advisory Group/Eclipsys) as VP of consulting.
David Joyner (Blue Shield of California) joins Hill Physicians Group (CA) as COO, replacing the recently promoted CEO Darryl Cardoza.
Mobile Heartbeat names Jamie Brasseal (Dell Healthcare and Life Sciences) as VP of its western region.
Announcements and Implementations
Drchrono will incorporate digitized patient education material developed by Mayo Clinic into its EHR.
Five healthcare organizations will participate in the pilot phase of Tennessee’s Health eShare Direct Project, spearheaded by the Tennessee REC.
Children’s Hospital at London Health Sciences Centre in Ontario implements Upopolis, a social networking tool for children receiving care in hospitals that is powered by TELUS Health.
Vibra Healthcare completes the first phase of deployment of PatientKeeper NoteWriter electronic documentation software across four of its long term acute care hospitals.
Cerner will integrate print spooling software from Plus Technologies into Millennium to streamline print operations.
ACS MediHealth will work with Troy Group to develop prescription printing solutions for Meditech.
Government and Politics
ONC announces Planning Room, a Website launched in collaboration with Cornell University to allow public input on the federal HIT strategic plan.
Two North Carolina state senators introduce a bill that would require hospitals to post on the state’s HIE their pricing for common procedures and their typical reimbursements from health plans.
Other
An NPR article covers the massive increase in the number of Americans who are receiving government disability payments for often questionable reasons such as unverifiable back pain or mental illness, with 14 million citizens now being mailed a monthly federal check without even being counted among the unemployed. The article concludes that disability “has become a de facto welfare program for people without a lot of education or job skills,” with fewer than 1 percent of recipients from early 2011 having returned to the workforce.
CNN profiles St. Louis-based Advanced ICU Care, which offers tele-ICU services.
A Reuters article finds that Wolters Kluwer is able to make good profits in healthcare because its medical references are moving from printed to electronic form, with 100 medical journals offered as iPad apps. The company says demand is increasing because apps allow teaching procedures by video, which also allows the company to sell more targeted advertising.
Studies published in JAMA find that not only has a mandatory reduction in medical resident working hours failed to improve their depression rates or sleep patterns, it has also been associated with an increase of medical errors of up to 20 percent. One possible explanation is the unintended consequence of hospitals expecting their residents get the same work done in less time.
In Canada, an Alberta ED doctor is suspended for looking up the electronic medical records of patients she wasn’t treating. She was caught when a patient asked for a copy of his access log and found that nine doctors, none of whom were treating him, had looked at his files. The hospital determined that the ED doctor was using workstations that her colleagues had left logged on.
The New York Times says radiology residents are beginning to realize that the heyday of big money for minimal work is over due to Medicare cuts, technology-driven competition, teleradiology, and demands to move public money from specialties to primary care. Financially motivated medical students pursing the high-paying, procedure-based ROAD specialties (radiology, ophthalmology, anesthesiology, and dermatology) are all seeing average incomes dropping steeply with the exception of the less Medicare-dependent dermatology.
![]() The NHS pays for a woman’s $7,260 breast implant operation after convincing doctors that her 32A chest size had put her in a state of emotional distress that could be alleviated only by an upgrade to 36DDs. The mother of two now intends to leave her children with her parents, move to London, and pursue a modeling career. She referred to TV star Katie Price in her statement: “I want the world to see the new me and want money and fame just like Katie. I can’t thank the NHS enough for giving them to me.” I can’t claim emotional distress, but perhaps I should consider moving to the UK so I could be a more successful anonymous blogger.
The NHS pays for a woman’s $7,260 breast implant operation after convincing doctors that her 32A chest size had put her in a state of emotional distress that could be alleviated only by an upgrade to 36DDs. The mother of two now intends to leave her children with her parents, move to London, and pursue a modeling career. She referred to TV star Katie Price in her statement: “I want the world to see the new me and want money and fame just like Katie. I can’t thank the NHS enough for giving them to me.” I can’t claim emotional distress, but perhaps I should consider moving to the UK so I could be a more successful anonymous blogger.
Weird News Andy says “some might call it murder.” A doctor in Brazil is charged with seven murders and is suspected of hundreds more as a hospital’s ICU team routinely freed up beds by administering muscle relaxants to patients and then turning off their oxygen supply. Prosecutors released the doctor’s wiretapped telephone conversations that included, “"I want to clear the intensive care unit. It’s making me itch. Unfortunately, our mission is to be go-betweens on the springboard to the next life.” WNA is also curious who approved a patient’s breast enlargement procedure when 1,200 people have starved to death in NHS hospitals “because nurses are to busy to feed patients.”
It’s like the postmortem version of fake Facebook friends: a UK company offers rent-a-mourners to families who want the funerals of their loved ones to be better attended or to “increase perceived popularity.” Actors, who are billed at $68 for a two-hour funeral or wake, are briefed about the deceased and trained to chat convincingly with real family and friends.
Sponsor Updates
- Minnesota Public Radio profiles Intelligent Insites and how its real-time operational intelligence software will be used in 152 VA hospitals.
- Regions Hospital (MN) reports that its use of Besler Consulting’s BVerified Transfer DRG and IME tools have resulted in significant revenue recoveries.
- The LDM Group discusses the rapid growth rate of e-prescribing across healthcare.
- API Healthcare’s President and CEO J.P. Fingado shares tips on increasing operational effectiveness with the healthcare workforce information exchange in an April 2 Webinar.
- The Albuquerque Journal spotlights Seamless Medical Systems and its SNAP iPad app for capturing patient data.
- Eric Venn-Watson MD, AirStrip’s VP of clinical transformation, discusses how private healthcare could benefit from the US military’s cutting-edge health technologies.
- Gary Palgon, VP of healthcare solutions for Liaison Healthcare Informatics, discusses how data integration can help organizations reduce readmission rates.
- eClinicalWorks opens a website for its 2013 National Users Conference in San Antonio October 11-14.
- Frost & Sullivan publishes a white paper on the impact of ClinicalKey, Elsevier’s clinical insight engine.
- Impact Advisors Principal Laura Kreofsky discusses the privacy and security risks of social medicine and Senior Advisor Ryan Ulteg offers insight into the financial implications of ICD-10 implementations for physicians.
- ADP AdvancedMD launches a website that provides a timeline for practices as they prepare for the ICD-10 transition.
- Access chooses CoSentry as its cloud and data center services provider.
EPtalk by Dr. Jayne
I didn’t have a lot of time to search for newsy tidbits this week because I was heads-down in CMS FAQs. As usual with government programs, now that money is flowing, audits have been introduced to try to recoup any inappropriate payments. My hospital is very concerned by the answers to the “Will there be audits” question, so I thought I’d share the highlights:
- Yes, there will be audits.
- You will need to have scads of documentation and it needs to be retained for six years.
- Contractors will be involved in auditing. If you already have post-traumatic stress disorder from heavy-handed RAC audits, I feel for you. They’re leaving the door wide open for abuse: “The level of the audit review may depend on a number of factors, and it is not possible to include an all-inclusive list of supporting documents.”
- Audit requests will come via e-mail from a CMS address. The e-mail used when registering for the EHR Incentive Program will be used for the initial request. If you put your physician’s e-mail address in the box, make sure she or he knows to be on the lookout for this and check your spam filters. Further communication will be through a secure communication process.
- You need to maintain documentation that supports the values you used for CQMs and payment calculations.
- Individual patient records may be requested for review.
- On-site reviews at the practice or hospital, including a demonstration of the EHR system, may be requested. For those of you gaming the system by turning on features just for your attestation period, this could come back at you unless you can re-create exactly the way you were configured at the time of attestation.
- Separate audit processes apply for Medicaid.
One of my CMIO colleagues received a hospital request in the fall. It was a spreadsheet that seemed pretty simple, but ended up requiring a ridiculous amount of data. She shared it with me confidentially. I loved the request that the reports include the EHR vendor’s logo to “prove” that it came from the EHR. If people are going to be fraudulent, I think they would be smart enough to dummy that up.
Despite clearly worded responses, the auditors didn’t understand the hospital’s answers or the math behind the calculations. They rejected spreadsheet data and insisted on screenshots from the application, or alternatively screenshots that showed a user exporting the data to spreadsheet. Again, do they not think screenshots are easy to fake? Maybe the hospital needs to film the user running the report and post it on YouTube for the auditor’s viewing pleasure.
From her recount, the auditors had all the power, and even having the vendor step in to provide supporting documentation didn’t help. MU is all or none – if there is a single discrepancy, you have to return all the money. It’s the equivalent taking a class and being expected to score 100 percent on every quiz, paper, and exam, including the final.
I hope CMS understands a simple principle about perfection that we learned in medical school — it doesn’t matter if all the lab numbers look great but the patient is dead.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis.
More news: HIStalk Practice, HIStalk Connect.













Smokin’ logo, Mr. H! Glad to see you back.
So basically Microsoft’s foray into Health IT was pretty much a complete and unmitigated disaster including their overpay for Sentillion that accomplished almost nothing and will really leave no noticeable footprint on healthcare. Just wonder if the overall tab was more than $1B or not including the price of their acquisitions.
The Caradigm consortium is heavily dependent on Orion Health’s successes in APAC as this just aint happenin in the US. Orion has too many customers and partners to protect here. I mean who’s gonna pay $5M for Amalga analytic alone? Syonara baby.
Love the smoking doc logo! – it is everything that the new sterile corporate logo is not- funny, ironic, unique, engaging and reflects what Mr. H is all about. This corporate logo is the New Coke of HIS Talk, which is just fine- making mistakes is okay and is part of tying to improve things- what is not okay is not fixing the mistake once made.
Love the old logo! Reminds me of J.R. “Bob” Dobbs.
@Dr Hertz–Healthcare IT needs more slack and fast. Far too many people not pulling the wool over their own eyes.
Dr Jayne –
So how do the auditors justify looking at individual patient records (when I think I recall CMS saying that they wouldn’t). It’s a stretch to say that this is for Treatment, Payment or Healthcare Operations
Joe Schneider