TBF the anti-hate non profit was funding undercover investigators trying to being down the KKK & has done successfully for…
Monday Morning Update 3/19/12
From Eric Rose MD: “Re: proposed MU rules. Like a lot of people, I get annoyed at how difficult it is to get to the actual regulatory text because the headings are embedded. I’ve extracted the actual text and marked them up with section headings. Turn on the Navigation Pane in Word and you can easily find the sections, particularly those with certification criteria or MU objectives. I created these for my own convenience, but others might find them useful. Feel free to share with the HIStalk community.” I’ve set up the certification criteria and MU objectives for downloading. Thanks to Eric, who is a clinical terminologist with Intelligent Medical Objects.
I’ve been having problems with the e-mail blast application that nobody can figure out, so I’m changing it to a hosted solution since I have no time for further investigation. The differences you’ll notice are: (a) the update notices will be HTML messages, which are a little bit nicer looking and easier to use than plain text; (b) the e-mails will look better than before when reading on mobile devices; and (c) hopefully the e-mails will go out faster and get delivered more often. I’ve learned way more than I ever wanted to know about the technical side of Exim, SMTP hosting, and server message queues and it’s not nearly as simple as just sending someone an e-mail. I’ve still got some fine tuning to do and I may need to change again if this doesn’t work as well as I’m hoping, so be patient and we’ll get through it.
Listening: Penelope Houston, one of the better female folk-rockers you’ve never heard of. She used to be singer of punk band The Avengers, but now does moody Euro-sounding 60s pop with mandolin, autoharp, some vintage Hammond B3 organ in the mix.
My Time Capsule editorial this time: US Healthcare Value is Low – Follow the Fancy Buildings, summarized by this snippet: “I’m not smart enough to figure out who the good guys and bad guys are in healthcare, so I look at just one thing: buildings. When I see stunning hospitals, vendor headquarters, insurance offices, and doctors’ houses, I figure they’re doing a little better than I’d like.”
A couple of readers chimed in on my comment about Epic implementations slipping from their aggressive, MU-driven timelines, saying they’ve heard of places having that problem. I think you’ll hear more about this. Big money at risk or not, system implementations are always harder and more complicated than they seem, and hospitals are notoriously bad at change management (although Epic leads them through it by the hand.)
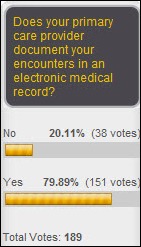
This is encouraging in an “eat your own dog food” kind of way: 80% of respondents have primary care providers who use electronic medical records. My university-associated doc does and it’s made a huge difference in how my encounters work: I get accurate medication reconciliation performed at every visit with the system (even though all I take is a diuretic), he has all my history right in front of him (it’s fun to see how my weight has changed over the years, mostly because it’s gone down quite a bit), and we have avoided duplicated lab tests. The doc looks smarter, I feel like my entire health situation has been considered, and we use the on-screen information together as a teaching and planning tool. I’ll say something I would not have said a couple of years ago: I really think I’d sadly have to find another doctor if mine was stuck in the paper chart world. New poll to your right, in honor of the Mostashari vs. academic researchers flame wars: will wider EMR usage reduce the number unnecessary imaging exams? Maybe someone should just ask doctors themselves instead of trying to make inferences from sketchy data.
On the Jobs Board: Client Care Engineer, Mobility Software Engineer, Epic Inpatient Module Go-Live Support, Vice President Healthcare, Meditech CPOE Activation Support, Consultant. On Healthcare IT Jobs: NextGen Analysts and Consultants, Horizon Meds Manager Consultant, Assistant Health Services IT Director. I don’t know about your phone, but mine is ringing constantly from recruiter calls, although I do have specific expertise that’s hard to find. A lot of the calls are from folks looking for consultants.
Thanks the the following new and renewing sponsors that supported HIStalk, HIStalk Practice, and HIStalk Mobile in February (click on a logo for more information):
An article in the newsletter of the USAF’s Hurlburt Field describes the Air Force’s MiCare Portal, a RelayHealth-powered site that allows patients to send secure messages to clinicians and request refills, while the providers can send patients appointment reminders, results, referral information, and changes in clinic hours. The group practice manager says the goal is to make MiCare the preferred method of communication after in-person appointments, avoiding phone tag and missed handoffs. Other bases using MiCare: Hanscom, Langley, Nellis, Offutt, Scott, Seymour-Johnson, and Travis.
Weird News Andy offers his own flavor of March madness with this story, in which an enterprising urology group is offering a free pizza with each vasectomy performed in March. The practice says March is their busiest time as men figure they might as well recover on the couch while watching basketball games on TV. WNA finds the last line of the story, which describes the free pizza, disturbing: “It does actually come with one topping. Maybe you can put some meatballs on it.” He also adds his own joke: what did the urologist’s wife sing to her husband when he finished his residency? “Urine the money, urine the money, we’ll have a lot of what it takes to get along.” </rimshot>
Here’s Vince’s HIS-tory of CliniCom (Part 3.) Check out the resemblance of the 1980s-era CliniCare handheld nurse terminal to the iPad.
I remembered Friday at work to print off the Archives of Internal Medicine article that has generated all the simplistic rag headlines that meet their goal of being stupid-simple and sexy at the expense of accuracy in summarizing the original study (example: iPads: Increasing Doctor Efficiency, Decreasing Patient Wait Time). The actual University of Chicago study wasn’t nearly that conclusive. The university gave iPads to 115 internal medicine residents and taught them to use Epic on it, along with online publications and the internal paging system. Four months later, the residents were surveyed. Results: 90% were using the iPads for work (it’s interesting that 10% weren’t) and 75% of those were using them daily (meaning 38% of those given an iPad weren’t.) Three-quarters of those said they thought they were more efficient and 68% of them said they thought patient care delays had been avoided because of the iPad. Residents entered a few more (5%) orders before 7 a.m. rounds and within the first two hours of admission. Study weaknesses:
- A sample size of 115 residents in one academic hospital isn’t all that predictive and doesn’t cover other specialties.
- Residents work a lot differently than attending physicians and community-based docs.
- Asking residents if they thought their free iPads were useful may have encouraged them to inflate the results to avoid having to return the iPads.
- The difference in order timing was tiny and compared 2010 patterns with those of 2011, a time during which other factors surely changed.
- The team had no way to determine which orders were entered from the iPad vs. from a desktop or laptop, so there’s no proof that the “earlier” orders came from iPads at all. It was also not stated whether Epic was available on wireless devices in 2010.
- It was not stated which devices were in use in 2010 – wireless laptops or hard-wired desktops. If residents didn’t have their own individual wireless laptops in 2010, you would expect orders to be entered more quickly (no waiting for a device) and closer to post-call rounds (the device would be at hand in the conference room).
- Placing orders early doesn’t necessarily translate to better outcomes or increased patient satisfaction, although it’s still a good thing overall.
- Epic has a native iPad client that most systems don’t offer, so experience with a less-functional clinical systems client would likely be less positive.
- Still, all that aside, if you can make residents think they’re more effective (not to mention cooler) for just $500 and you even potentially avoid the cost of buying them their own laptops, why wouldn’t you?
Mission Health (NC) names Sulaiman H. Sulaiman, formerly CIO of Cleveland Clinic’s hospital in Abu Dhabi, as SVP/CIO, replacing the retiring Arlo Jennings.
Athenahealth will hire 80 people to work at its Belfast, ME office, raising its headcount by 20%.
An article in The Atlantic says innovators develop products for people who are like themselves, which is why mHealth apps influence only the already-good health of what it calls “The Social Network” (well-educated, technically savvy, and affluent whites and Asians living on both coasts) while having minimal influence on the behaviors of the more diverse and more healthcare-expensive population as a whole. As Dr. Travis has said on HIStalk Mobile, running apps are a lot more popular with runners than couch potatoes. Or as Bill Gates says, we already have healthcare technology that tells people that they need to change their habits, but unhealthy people just ignore what it’s telling them (bathroom scales.)





























Last I checked anyone who is providing that much capability on the ipad for epic is doing it through citrix. Which would be the same integration as any other vendor. Please let me know which client they are using if that’s not the case.
[From Mr H] They used Citrix in the article. Epic has the native iPad app Canto, but I don’t know if it does CPOE (I’m thinking not). But the functions it does have could possibly still improve utilization and efficiency if were used and as Epic enhances it now that the iPad has proven itself to have staying power.
Can I just make this unscientific observation and comment about the “Mostashari vs. academic researchers flame wars: will wider EMR usage reduce the number unnecessary imaging exams?” I don’t think we’re giving doctors enought credit if we think that a new tool will influence them to order more of any kind of tests. Docs, if we let them do their job, typically try to order the most appropriate tests, procedures, meds, therapy, etc. that benefits the patient’s condition, regardless of what payers or technology might want to influence them to do. How do we know that they weren’t “under-ordering” before because they didn’t have all the pertinent data in front of them at the point of care to suggest a test should be ordered?
To add on to RustBeltFan… I’d suggest that question asked (“will EMRs reduce unncessary tests”) is only part of the equation. So yes, EMRs should ideally reduce unncessary tests in two ways: (1) Letting docs see past tests more easily, and (2) CDS Rules which tell a doctor if a test is unncessary.
However, this is different than asking “will EMRs reduce all testing”, or “will EMRs reduce the costs associated with testing”. In those cases, we are starting to see that EMRs may actually INCREASE the amount of tests being ordered in two ways: (1) CDS Reminders (eg HbA1C, Mammograms) and (2) Simply making it easier to order (“1 click to order 100 tests”). However, these are more likely the appropriate test – which is better quality…but likely will increase costs (at least initially). Some might argue this will save costs down the road via better control and earlier detection.. but others would argue that we never save costs with preventive care, we simply delay costs at best.
In other words, both sides have a point – and it is possible to argue that you both DECREASE some tests (which are not needed) while INCREASING other tests (which are needed). But neither can easily claim that there is an absolute answer on saving costs – and it will be hard to test because EMRs are still too different, and even the “rules” organizations might use for decision support are not always consistent.
Interesting article about Mission Hospitals in Asheville, NC. Losing Dr. Arlo Jennings is a huge loss for Mission and aligning with the “mission” of this website…a huge loss for Cerner. I wonder if Suliaman and his Cleveland Clinic ties might try to bring EPIC in. I am sure Judy wouldn’t mind visiting the Grove Park Inn after a long week…
Epic’s Canto does not offer Order Entry at this time. It is primarily a results viewer with e-prescribing.
[From Mr H] Which does bring up a good point … having information available at the right time and place on the iPad could still increase early entry of orders even if those orders aren’t actually entered on the iPad, or if they are entered sub-optimally on a Citrix presentation of a screen not designed for mobile use. Seeing new lab results, being alerted of new admissions, and looking at overall patient status while rounding could speed up decision-making, even if the resident decided to walk over to a desktop PC to actually enter the resulting orders.
Many thanks to Dr. Rose for reformatting the proposed MU regs into a more usable format, especially breaking out the certification regs separately.
Thanks Mr. H. the page loads much faster. The change was noticed immediately!
Loved the new email format this morning – nice surprise. The HTML looks good.
Well, you know then but, the good Dr. Lyle produces good points. But then, my golly gosh, it is much easiers to order new tests than to scroll through the screens searching for results of past tests. This may take many minutes of time of professionals, wasting them to save dollars for others.
Well then but, why waste my times searching when the vendors have no any search systems? If you wonderful bloggers here know of any searching programs of the history by any vendors, by all means, tell us them.
My golly gosh, with all of these innovative EHRs, sad there is not any searcher mechanism but scrolling.
Well then but, I know no any of you but of me, quicker to click new orders than to scrolls.
Prabda – try the results section area of your EHR and pick the tab that at least phonetically seems close to you. Rodeology, Labyrinths, eatcelera
Every once in a while those crafty developers will even allow you to click on the top of the column and sort by name, or type, or even date. (I know, what will they think of next).
Have fun! Please continue to present your challenges so we can feel good helping you! Maybe we can get together for a reality TV show or something. That’d be cool.
Best wishes to Arlo Jennings for a wonderful retirement. He represents a class of CIO rarely encountered. I truly enjoyed working with the Mission group. Cloning might be a good idea!
Prabda
I know that both Meditech 6.0 and Cerner have imbedded EMR search tools that will execute a search for your term/phrase across visits, across care settings – similar to a google search- and present you with the results. Sounds like this would work for your needs. I would be shocked if other vendors did not offer something similar.
What’s with all the golly gosh’s?