HIStalk Innovator Showcase — Trans World Health Services 9/5/11
Company name: Trans World Health Services, Inc.
Address: 10509 Professional Circle, Suite 102, Reno, NV 89521
Web address: www.transworldhealth.com
Telephone: 775.852.9440
Year founded: 2003
FTEs: 7
Elevator pitch
We provide software and consultancy to help FQHCs, Community Health Centers, and other healthcare providers deliver better, more cost-effective care.
Business and product summary
We offer three product lines – Health Center Accelerator (real-time performance improvement software), Better Care Better Value Suite (comparative benchmarking and analytics software and services), and process improvement consultancy, which all work together to give Community Health Centers and other healthcare providers the tools they need to best manage their activities. We evaluate the client’s operation; apply analytics and experience to correct process flow issues; determine which meaningful measures need to be inspected and monitored; implement the appropriate libraries of performance improvement dashboards, alerts, and interfaces to the source data systems; and train and support the users.
Users include all levels of management right through to front-line staff within the administration, finance, and clinical areas. Our cost model is based on packaged or risk-based fees for initial consulting and implementation, and a monthly license fee for use of the monitoring software and/or access to the benchmarking service. The system can either be locally hosted or delivered in a SaaS environment. By delivering real and measurable improvements in organizational performance, the return on investment for our
pilot site is greater than 500% on an annualized basis and paid for itself within the first three months of deployment.
Who is your target customer?
While our targets could legitimately be any healthcare organization from a small primary care clinic or physician practice to the largest integrated delivery network or payer organization, our current focus is on Federally Qualified Health Centers (FQHC) and Community Health Centers.
What customer problem do you solve?
We highlight and solve process and efficiency impediments that are preventing Health Centers from delivering optimal service levels so they can use their resources more effectively. This leads to cost reductions per patient encounter and increases the ability of the organization to deliver more care and treat more patients with current or slightly expanded resource levels in line with their core mission.
Who are your competitors?
Excluding competitors that are split between pure practice management consulting and pure complex dashboard, workflow, and analytics software providers (which are many and very expensive), there are few companies that offer pre-packaged, healthcare customer-specific dashboard software including pre-packaged efficiency best-practice consulting. Those that do exist, for example: onFocus Healthcare; DashboardMD; The Advisory Board; and MedeAnalytics; are mainly hospital and integrated delivery network focused. Within the Health Center marketplace, we have only found one that would appear to be even slightly similar in positioning: InterPoint Partners.
Why are you better than your competitors?
Our senior management each has over 25 years of senior expertise in healthcare performance improvement, process redesign, quality improvement, clinical utilization, and software development. That translates into knowing right where to go to uncover meaningful areas to focus and improve. Our dashboard software mashes multiple clinical, financial, and operational data sources and runs in real time, providing users with immediate access and drill-down capabilities to see why and where the problems are occurring either at the moment they can be addressed, or by identifying them through proprietary forecasting techniques to prevent problems from even arising through early warning alerts. Traditional single silo reports that are typically run days or weeks after the fact become irrelevant since they are produced too late to save the critical time-limited resources.
Pitch video created specifically for this Showcase
Customer Interview (CEO of a non-profit, community-owned health center)
Your organization was seeking financial and quality improvements. What results have you seen and how much of that was attributable to Trans World Health Services?
The actual results have been about $500,000 to $700,000 in increased revenue over the last 18 months, and about 70% is directly attributable to processes identified through the use of the accelerator and the consultative services.
Organizations always say they have plenty of data, but little information. Was that your situation before, and how has that changed?
We had an enormous number of spreadsheets and data. We also had data integrity issues. It wasn’t until TWHS did a forensic analysis and helped us to clearly define and analyze the data did we reach a point where we could actually begin making rock-solid data supported decision making. It has removed significant amount of doubt and discussion from our ability to operate.
If you were speaking to a peer from another group, how would you complete this sentence: "You should talk to Trans World Health Services under these circumstances:"
If you plan on surviving the challenges of healthcare reform. This product and the services offered by TWHS will revolutionize the way Health Centers function and operation in the future. Don’t be caught later wishing you had made the investment.
An interview with Bryan Lang, founder and CTO of Trans World Health Services
Tell me about the company.
The market that we’ve targeted and really gone after in America is the Community Health Center market, Federally Qualified Health Centers, FQHC lookalikes, and rural clinics. This market has been tremendously underserved. They’re under tremendous increase in growth and demands. They’ve never had this technology available before.
We developed this technology that was used in every single hospital in England to be able to visualize and to predict where you’re going. We wanted to make it available to this very cost-effective market segment in America. That’s our focus right now.
What do we do differently from the others? Well, it’s a very underserved market. You have occasional dashboard add-on products to the HER. For example, NextGen has an add-on dashboard product, but you get to build your own using that product.
Our approach is very different. There are five points in our framework. We want to pull information together so they can see and understand what’s going on. We have the analytics to identify variances and opportunities for improvement. We have the predictive modeling to show where they’re heading. We embed best practices into our software so that rather than building your own, you can see exactly where you are relative to others, relative to your own benchmarks, and what you need to do to make a difference. Finally, the data quality in the health center market is substandard in many cases; we really want to be able to show data quality improvement on auditing capability so they can trust their data.
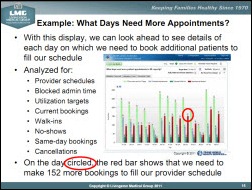
A simple example of combining the information from various systems involves patient scheduling. If a Health Center is not fully booking its appointment slots, we’re able to say, “Why is that?” and take a look at where the patterns are. Take a look from their population health management systems or their disease registries to say clinically who should be treated, and to be able to combine that, put a value associated with it.
For example, “This is the value of your diabetic population that needs to be seen.” Combine that data to put it in front of them, in front of the booking people — the people who need to be seen so they can call them up, fill those empty appointment slots, and run a full schedule. That’s a combination using the practice management system, possibly a population health management system or an electronic medical record, and financial information to say, “This is how you affect a positive change by filling your appointment schedules more.” Ultimately that leads to increased revenue with existing staff, so that that’s better for their financial performance.
I ran across a presentation from Livingston Medical Group that was pretty impressive. Can you describe some of the results that they have realized using your product?
Livingston was a very interesting client. They brought us in originally because of the concern about losing productivity due to the implementation in electronic health record. What they wanted to do was have us make them more efficient.
We originally got into a common measure of productivity, which is their providers were not achieving three patients per hour. Three patients per hour essentially is the baseline that many Health Centers run on. We then were able to take a look in that by pulling the data together showing visually that this wasn’t a function of providers slacking off — this was a function of the fact that they had not filled those appointment slots. They hadn’t even provided the providers with enough patients to be able to see to make their targets.
Right off the bat, we were able to pull this information and change some of their fundamental processes so that they could start filling those slots and achieve better provider productivity and revenue. Unfortunately, about this time, they had a tremendous financial crisis. California stopped paying, and then they had outsourced their billing services. Unfortunately, their billing backlog started climbing. They were not able to generate bills. They were not able to bring in revenue. Their financial system went into a crisis.
At that point, neither the billing company nor they were able to see where the problems were. They just didn’t have access to the information. We were re-tasked to be able to open up the information, show the visibility, provide insight into where the problems were in the process.
We found a huge number of bills that had never been transmitted. We found reasons for blockages and why they hadn’t been paid. We were able to very quickly open all this up so they could see where the problems were, see what they needed to do to solve the problem, solve the problems, and then see the revenue flowing through. It was a very, very narrowly averted crisis. As John will say, they came within a couple of weeks of not being able to stay operational. That was one of the things that we were able to provide for them.
We also showed them how we could provide a huge additional amount of retained earnings for them. Some were north of 700% was what our estimates showed if we changed a few of their fundamental processes and brought them in line with what best practices would be. You hear all this and you say, “Well, that’s something that systems aren’t going to be able replace consultants,” and, no they aren’t. We really believe that the consultancy component is a big part of what we deliver. However, by building in what a lot of consultants normally would do into the software, embedding those best practices, making it a problem-focused solution, so you can see if you have a problem in a given area.
You can say, for example, “How financially effective are our letter campaigns – our recall letter campaigns to get patients to come back in?” It’s very, very difficult to get answers to that information. That’s a question that is asked in our system, so you go right to that question and click on that and you can go right down into where you can see letter campaign by letter campaign. How effective are you every time you send out a batch of letters to get patients back in, how many are there coming in, and what value is that offering to the organization as a result of sending these recall letter campaigns out.
That’s some of the things that we did at Livingston. We’ve had a very, very good working relationship with them. We originally came in there at saying, “We’ll work with you as long as you believe us to be effective in helping you out” and added to the library item after library item to our system so that we just keep on building module after module. It’s a very interesting market and we look forward to staying in it for awhile.
Healthcare customers tend to like solutions that have quick implementation and payback. What you’re offering sounds like technology and consulting services that require a commitment to change on the customer’s operational side. How do you sell that?
We sell that in two ways. We sell it in a traditional manner where that’s bundled together, where there’s a package of consultancy based on the problems that they’ve identified and very, very similar problems exist across the spectrum. Based on the problems identified, this is what we’d do for the system to be able to plug our system into the various other systems, to be able to present the information to their executive team, and then to be able to work through the top five problems or issues that they want to focus on. We generally package that in terms of an initial three months’ worth of consultancy as well as the software. From that, they make their own determination on how much consultancy they want to have going forward.
There must be a fair amount of overhead in getting those sales by helping them identify their problems and then convincing them that your combination of services and product can help resolve them. Do you see that as a limiter of your growth potential?
Getting in the door is very interesting. We try to minimize the cost of sales, because these price points are not at all what business intelligence systems would be for hospitals. We try to go to conferences or out where groups of them come together or meet in groups. We also do a lot of WebEx demos.
But the problems are very similar across the spectrum of Community Health Centers in America. Once we have a set of solutions, we can say, “You’re probably looking at this, this, and this. Let’s show you what this would be” and you get head nods around the table very quickly.
What do you hope to gain from this exposure?
We hope to gain a lot understanding of how we can make a difference in helping Community Health Centers. Ultimately, we’d certainly like to go back to our original market, which is hospitals, and take that and step forward from the traditional models, but really build that consultancy behind it to say, “Where are my problems and what do I need to do about the problems now, today, so that they don’t become a statistic tomorrow?”






Thomas told me when he submitted his article that it was OK if I didn't run it because people generally…