News 4/29/15
Top News

Vanderbilt University Medical Center (TN) will replace its McKesson Horizon system — the CPOE portion of which it developed in-house as WizOrder starting in 1995 — with either Cerner or Epic. That’s one of the last homegrown systems to bite the dust, both at Vanderbilt and everywhere else as McKesson puts its commercialized version out to pasture after a 12-year run. It’s also interesting that Vanderbilt is echoing the general market trend of considering only Cerner and Epic to be viable choices, showing no interest in looking at Allscripts, Meditech, or McKesson Paragon.
Reader Comments
From Willow: “Re: Xerox Midas+ layoffs. Four laid off so far, apparently prompted by the first poor quarterly earnings report in the company’s history, which appear to have been caused by the high consulting and infrastructure costs spent on its Juvo product.” Unverified.

From Concerned CC Client: “Re: new CEO at CareCloud. Positioned as great new, but in reality not. Since they were founded in 2009, under Santalo’s direction, they have gone through $80.5 million, are not making money, and now need $15 million to stay afloat.” EHR/PM vendor CareCloud announces Ken Comee as CEO, replacing Albert Santalo, who will remain as chairman and chief strategy officer. The company also announced $15 million in additional funding from existing investors. Technology executive Comee has been on CareCloud’s board since 2012, and according to his LinkedIn profile (which features the overly arty “more chest, less head” look above), he has no other healthcare-related experience.
HIStalk Announcements and Requests
We’ll have HIStalk Practice posts Monday through Thursday going forward (instead of just twice weekly) and Jenn will also write a Friday summary of population health management news. Sign up for short, fun, and informative updates and see what’s new in ambulatory, practice, and PHM.
Webinars
None scheduled soon. Contact Lorre for information about webinar services.
Acquisitions, Funding, Business, and Stock
Private equity firm Francisco Partners will acquire healthcare talent management solutions vendor HealthcareSource from majority owner Insight Venture Partners.

Merge Healthcare announces Q1 results: revenue up 6.9 percent, adjusted EPS $0.05 vs. $0.04, beating earnings estimates but falling short on revenue.

Validic raises $12.5 million in Series B funding from investors that include the venture arm of Validic customer Kaiser Permanente.
The Raleigh, NC business paper says Allscripts will build a new 18-story building for its 1,260 local employees, although the company hasn’t confirmed. The article mentions that Allscripts recently “rebalanced” 3 percent of its workforce.
The Chicago business paper profiles referral management software vendor Fibroblast.
Scanadu raises $35 million in a Series B round to further develop its Scout tricorder-like body scanner.
CTG announces Q1 results: revenue flat, EPS $0.08 vs. $0.19. The company blames soft healthcare IT services demand as providers delay projects or staff them internally.
Aetna announces Q1 results: revenue up 8 percent, EPS $2.20 vs. $1.82. Chairman and CEO Mark Bertolini said in the earnings call that its Medicity business is “seeing a lot of growth.”
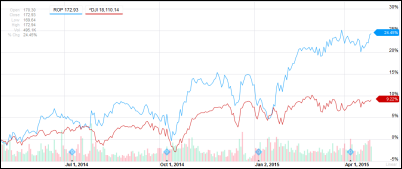
Roper Industries, which owns many companies that in healthcare IT include Sunquest and Strata Decision Technologies, reports Q1 results: revenue up 4 percent, adjusted EPS $1.55 vs. $1.46, falling short on analysts’ revenue expectations but beating on earnings. The company announced in the earnings call that it has changed its name to Roper Technologies to emphasize that it isn’t just an industrial company but rather a collection of businesses that deliver 60 percent gross margins. Above is the one-year share price chart of ROP (blue, up 24 percent) vs. the Dow (red, up 9 percent).
Sales
Consolidated Laboratory Services chooses McKesson Business Performance Services for billing.
Star Medical Center (TX) contracts with Anthelio Healthcare Solutions for revenue cycle optimization.
People



Medical kiosk vendor HealthSpot hires Gail Croall, MD (Anthem) as chief medical officer; Eric Eichensehr (Levitate Technologies) as CTO; and Bruce Roberts (RxEngage Partners) as COO.
Announcements and Implementations

In Qatar, Al Khor Hospital goes live on Cerner Clairvia for nursing staff management.
The CEO of Henry Ford Health System (MI) says that while the system took an initial financial hit in 2013 after its $353 million Epic implementation, using Epic helped it save $65 million in 2014 and HFHS will cut $300 million in cost by 2016 as its financial turnaround continues. Meanwhile, UNC Health Care (NC) also credits Epic with its stronger-than-expected operating income.
Wellcentive, SpectraMedix, and eClinicalWorks are pilot testing NCQA’s eMeasure electronic clinical quality measure program for Meaningful Use and HEDIS reporting.
T-System announces its tablet-based T Sheets Digital for Urgent care that includes 45 chief complaint-based templates.
MedAptus releases Premium Analytics for its charge capture suite.
QPID Health is named a Gartner “Cool Vendor.”
Government and Politics
The Institute of Medicine will rename itself to National Academy of Medicine effective July 1, 2015.
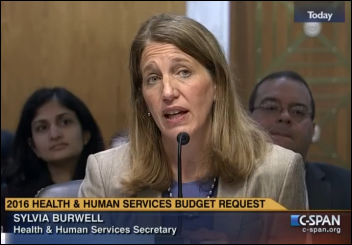
National Coordinator Karen DeSalvo, MD says in a Health Affairs blog post (which appears to have been taken verbatim from her HIMSS conference presentation) that ONC will use Medicare payments and the DoD’s EHR contract bid to push interoperability.
A security researcher finds data from Hilton Head Hospital (SC) for sale on a hacker marketplace, apparently exposed during a 2014 breach caused by PST Services, a McKesson subsidiary that provided billing services to Tenet’s hospitalist contractor and inadvertently opened up its billing records to Internet searches.
Seton Family of Hospitals becomes the latest organization to expose patient information via employee-targeted email phishing attacks. Hackers accessed the information of 39,000 Seton patients in the December 4 breach.
Other

Pella Regional Health Center (IA) opens a 24×7 nurse hotline as part of its patient-centered medical home efforts. Anyone can call the hotline to discuss concerns or make appointments with nurses who have access to the EHR.
Partners HealthCare expects to double the $80 million in annual revenue it receives from licensing and spinoffs.
Former National Coordinator David Blumenthal, MD says in a Wall Street Journal editorial that healthcare IT will fall short of its potential unless security and interoperability are improved.
A Brookings article highlights the maximum “reasonable cost” providers can charge patients for providing 75 copied pages of their records, which ranges from $19 in California to $101 in Georgia. It mentions that providers in many states can charge patients the same per-page amount for copies of their digital records even though the provider cost is essentially zero.
Sponsor Updates
- Amerinet extends through 2018 its member discounts to revenue integrity products from Craneware, also adding the company’s InSight Medical Necessity tool.
- Zynx Health and Meritage ACO will present “Using a Mobile Tool to Create a Virtual Caregiver Huddle” at the NPSF Congress April 29 – May 1 in Austin, TX.
- Cueatr posts a photo slideshow of its experience at the HIMSS conference.
- ADP AdvancedMD announces the launch of its SmartPractice e-letter for independent practices.
- AtHoc details its integration with Apple Watch.
- Besler Consulting outlines how “CMS-1498-R2 gives hospitals option to have their SSI Factor recalculated.”
- CareSync offers “Here’s How CareSync Changes Lives for the Better.”
- CareTech Solutions takes a look at how The Metro HealthSystem used the company’s solutions to realize SEO advantages and budget benefits.
- The local paper looks at how several HIStalk sponsors — CenterX, Forward Health Group, Healthfinch, and Nordic Consulting – are making an impact in their native Madison, WI.
- Team CoverMyMeds shares personal highlights of HIMSS15 in its latest blog.
- MedCPU looks back on its HIMSS15 experience.
- Health Care Improvements Institute announces its partnership with xG Health and interviews xG Health CEO Earl Steinberg, MD and President/COO Ray Herschman.
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Dr. Gregg, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates.
Contact us online.



































































I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…