News 10/14/16
Top News

The Department of Defense announces that the first go-live of its MHS Genesis implementation of Cerner is scheduled for February 2017 at Fairchild Air Force Base (WA), moved back from the originally planned December 2016 date that involved two test sites. Three other Washington military hospitals will follow no earlier than June 2017.
The DoD says it pushed the schedule back to give it more time to develop interfaces to legacy systems and for system testing, as well as to allow implementing speech recognition and transfusion management. The project’s budget and planned completion date of 2022 have not changed.
Reader Comments
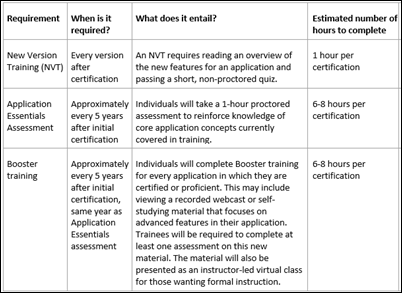
From Redacted: “Re: Epic certification. Users are now required to complete proctored exams every five years for each application they’re certified in. As a consultant, it’s not the worst thing in the world for them to remove other certified people from the pond, but I have 10 certs and their time estimate is 6-8 hours for each (doubled between the assessment and booster training). Seems like a huge pain.” Unverified, although the forwarded document above appears genuine.
From Boy Blunder: “Re: Epic‘s 2016 release. My TS contact says there was a two-month period in early 2016 where the entire development division pivoted to fixing issues with the 2015 release, delaying 2016 projects. She tells me we should not upgrade to 2016 for a while because the key features won’t be added until months after the initial release, delaying the discovery and fixing of the kinks we usually find.” Unverified.
From Booster: “Re: Epic’s Boost program. It’s an attempt by Epic to provide consulting services to customers deploying new functionality or optimizing their systems. The concept has been around for years, but was only recently formalized. Boosters tend to be less available and are rarely around for more than a short engagement, with most of them on their way out of the company and working somewhere other than Madison (less than one year). It’s good in theory, but cannot get off the ground because Epic employees have such short half-lives and aren’t compensated competitively to retain them.” Unverified.
From Little David: “Re: Hillary Clinton’s HIMSS14 speech. Did we get $225K of value?” It appears that the Secretary’s rack rate was $225K per speech, so HIMSS paid the same as everybody else. On the question of value, I’ll side with readers who observe that while we claim we want to hear selfless keynotes from patients, the size of the HIMSS crowd is always directly proportional to the fame of the presenter and Hillary (and Bill the year before) packed the house. I didn’t attend her presentation since I was tired of being at the conference before her Wednesday keynote slot, but I summarized it back then as:
I didn’t hear much about Hillary’s Wednesday keynote other than (a) it was extremely short; (b) like any skilled politician, she didn’t really say anything other than predictably lauding the work of the crowd that brought her there and kissing up to HIMSS. I would have been mad about waiting an hour or two to squeeze into the huge room for her talk given its lack of substance. Hillary’s rumored minimum speaking fee is $200K plus expenses, so she took home a big paycheck in addition to potentially impressing would-be Presidential voters who were apparently happy just to bask in her celebrity.
HIStalk Announcements and Requests
Welcome to new HIStalk Platinum Sponsor Healthlink Advisors. The St. Petersburg, FL-based consulting firm was founded by industry long-timer and former SVP/CIO Lindsey Jarrell, who hand-picks the people he (and the company’s client base) wants to work with based on their experience, passion, integrity, accountability, and commitment to social responsibility. Areas of practice include IT operations performance acceleration (leadership coaching, interim management, contract negotiation, application and technology rationalization, roadmaps); engagement (IT governance, system selection, program management, product and sales strategy development); and transformation (future state definition, consumer and digital engagement). I’m fascinated that one of the company’s core values that employees make healthy choices, which it supports by offering healthy foods at meetings, holding meetings while walking, requiring mandatory vacation time away from work, and insisting that no emails being sent after 10 p.m. or while the employee is on vacation. I also liked this insightful nugget in its “have fun” core value – “people leave managers, they don’t leave companies.” Thanks to Healthlink Advisors for supporting HIStalk.
This week on HIStalk Practice: Chinese Community Health Care Association moves forward with enterprise master patient index tech. Telemedicine companies offer free consults to victims of Hurricane Matthew. NextGen’s Cherie Holmes-Henry and Charles Kaplan offer advice on “Readying the Revenue Cycle for MACRA.” GMed develops patient check-in software for gastroenterologists. AmeriGroup partners with LiveHealth Online for telemedicine services in New Jersey. Health Fidelity co-founder Anand Shroff helps physicians understand the implications of risk adjustment. Zoom+ launches chat-based telemedicine app. Encompass Medical Partners gets into the IT maintenance and security game.
This week on HIStalk Connect: Pager raises $5.2 million. Proposal deadlines loom for the Stanford Medicine X | Withings Precision Research Challenge. Eccrine Systems closes $5.5 million in Series A financing. Bill Evans joins Rock Health. Charlie Rose focuses on artificial intelligence.
Webinars
October 25 (Tuesday) 1:30 ET. “Data Privacy/Insider Threat Mitigation: What Hospitals Can Learn From Other Industries.” Sponsored by HIStalk. Presenters: Robert Kuller, chief commercial officer, Haystack Informatics; Mitchell Parker, CISSP, executive director of information security and compliance, Indiana University Health. Cybersecurity insurers believe that hospitals are too focused on perimeter threats, ransomware, and the threat of OCR audits instead of insider threats, which are far more common but less likely to earn media attention. Attendees will learn how behavior analytics is being used to profile insiders and detect unusual behaviors proactively and to place privacy/insider risk within the risk management matrix.
November 8 (Tuesday) 1:00 ET. “A CMIO’s Perspective on the Successful 25 Hospital Rollout of Electronic Physician Documentation.” Sponsored by Crossings Healthcare. Presenter: Ori Lotan, MD, CMIO, Universal Health Services. UHS rolled out Cerner Millennium’s electronic physician documentation to its 6,000 active medical staff members — 95 percent of them independent practitioners who also work in competitor facilities — across 25 acute care hospitals. UHS’s clinical informatics team used Cerner’s MPage development toolkit to improve the usability, efficiency, communications capability, and quality metric performance of Dynamic Documentation, embedding clinical decision support and also using Nuance’s cloud-based speech recognition product for the narrative bookends of physician notes. This CMIO-led webinar will describe how UHS achieved 70 percent voluntary physician adoption within one month of go-live, saved $3 million in annual transcription expense, and raised EHR satisfaction to 75 percent. It will include a short demonstration of the software that UHS developed to optimize the physician experience.
November 9 (Wednesday) 1:00 ET. “How to Create Healthcare Apps That Get Used and Maybe Even Loved.” Sponsored by MedData. Presenter: Jeff Harper, founder and CEO, Duet Health. Patients, clinicians, and hospital employees are also consumers who manage many aspects of their non-medical lives on their mobile devices. Don’t crush their high technology expectations with poorly designed, seldom used apps that tarnish your carefully protected image. Your app represents your brand and carries high expectations on both sides. This webinar will describe how to build a mobile healthcare app that puts the user first, meets their needs (which are often different from their wants), creates “stickiness,” and delivers the expected benefits to everyone involved.
Contact Lorre for webinar services. View previous webinars on our HIStalk webinars YouTube channel.
Acquisitions, Funding, Business, and Stock
Axial Healthcare, which mines a database of 100 million patient cases to give insurers insight into risky pain care practices, raises $16.5 million in a Series B funding round, increasing its total to $26 million.
Nordic completes a minority recapitalization and announces plans to offer equity participation to all employees starting in 2017.
Sales
Providence Health & Services chooses LogicStream Health’s Clinical Process Measurement.

Meditech customer Hays Medical Center (KS) will implement the company’s Web EHR.

Cerner customer Olathe Health System (KS) will add Millennium Revenue Cycle and the RxStation automated drug dispensing system.
Insurer Highmark will implement Welltok’s CafeWell Rewards program for its Medicare Advantage policyholders.
People

Family medicine practitioner Doug Spotts, MD takes a full-time role as chief health information officer at Evangelical Community Hospital (PA).

Ascension SVP Mike Schatzlein, MD will resign effective December 31, 2016 to focus on his role as chair for the Nashville-based Center for Medical Interoperability. The non-profit was formed in 2015 with a $10 million grant from the Gary and Mary West Foundation, with membership focused on hospitals.

Population health management technology vendor Altruista Health hires Munish Khaneja, MD, MPH (EmblemHealth) as chief medical officer.

Zillion hires Cheryl Morrison Deutsch (Kronos) as chief experience officer.
Announcements and Implementations
T-System announces EVolvED, a low-cost, quickly implemented ED documentation system that combines T-Sheets paper documentation with a best-of-breed technology solution.

Adventist Health System goes live on Imprivata’s PatientSecure palm vein biometric identification system.
InstaMed achieves PCI SSC Point-to-Point Encryption Standard version 2.0 validation for protecting credit card payment data, the first company in healthcare to earn that recognition.
Portland, OR-based clinic model insurer Zoom+ launches a free medical chat service for its members that provides advice, diagnosis, treatment, prescriptions, and visit scheduling, with the chat transcript being added automatically to the EHR. I’m not sure if the apparently missing “with” in the “chat our doctors for free” page above is a mistake or intentional hipster wit.
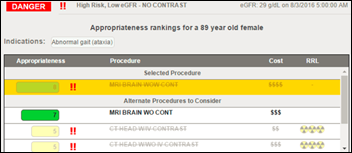
National Decision Support Company will debut its CareSelect Imaging decision support solution at RSNA, offering expanded Appropriate Use Criteria.
Government and Politics
ONC and HHS OCR update their HIPAA Security Risk Assessment tool.
CMS will review MACRA-required documentation and hold regional meetings with practices in trying to reduce the clinician administrative burdens involved.
Privacy and Security
Canada-based online medical advice startup Ask The Doctor becomes the first healthcare company to accept Bitcoin, providing users with extra privacy over charging services on their credit card. I can’t find any mention of how much the company charges to answer questions.
Innovation and Research
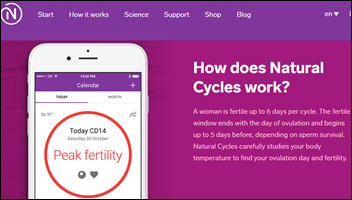
Women who avoid having sex on the days a physicist’s temperature tracking app says they are fertile avoid pregnancy 99.5 percent of the time, offering the same reliability rate as oral contraceptives and condoms and much better than the 75 percent success rate of the rhythm method alone. The company is in Sweden, which is probably a good thing since its claims might otherwise interest the FDA and the lawyers of unexpectedly pregnant women.
Other
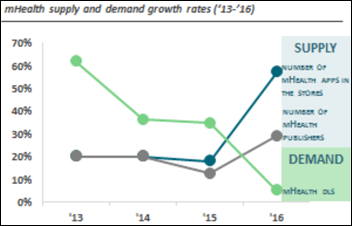
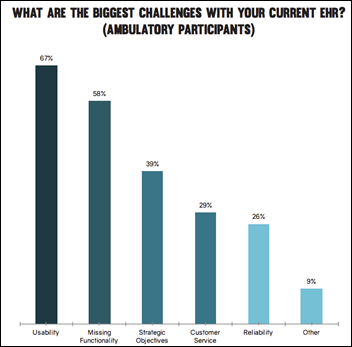
A study of mobile health apps finds a crowded market in which downloads are limited and declining, users aren’t willing to pay, newcomers have saturated the market, and 78 percent of publishers make less than $100,000 per year from their entire healthcare app business. Most app-related revenue comes from sales of sensors or other required hardware. Features seen as easiest to implement that have the highest user impact are personalized messages, dashboards, and the delivery of educational content. Publishers see their best hope of success as addressing users with chronic illnesses, but insurance companies haven’t shown much interest in getting them involved. Still, it’s a growing market even if it’s more competitive and selective.

In England, St. George’s University Hospitals NHS Foundation Trust freezes all software rollouts following a June 6 infrastructure failure in which its Cerner-provided downtime system didn’t work. The trust is out of storage capacity, can’t perform backups, runs Windows XP on 2,000 PCs, and has network stability problems.
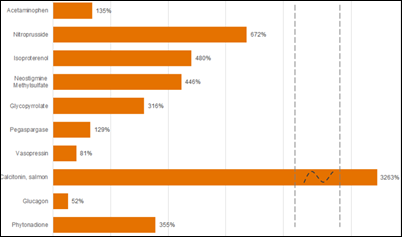
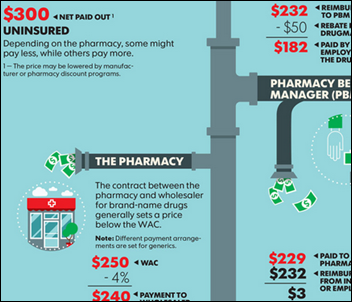
An American Hospital Association report finds that hospitals spent nearly 40 percent more on drugs for each inpatient inpatient in 2015 than they did in 2013 due to higher drug prices rather than increased volume, saying that the price jumps “appear to be random, inconsistent, and unpredictable.” Prices increased from 52 percent to 3,263 percent for the 10 drugs on which hospitals spent the most money, with even the journeyman drug acetaminophen recording a 135 percent price increase from 2013 to 2015. It’s interesting to me that a couple of decades ago, the field of pharmacoeconomics was created to make sure drugs delivered outcomes commensurate with their cost, which turned on a light bulb over the heads of drug companies that realized they could price based on those same outcomes rather than simply defend a markup based on their research and manufacturing costs. These top 10 drugs are all old, work inarguably well for mostly specific uses, and have little competition. The pharmacoeconomics model then supports high prices and thus high drug company profits.
The local paper covers the November 1 Epic go-live at Vernon Memorial Healthcare (WI), which is working with Gundersen Health System (just writing that even with a different spelling makes me think of the police chief in “Fargo” or The Swede in “Hell on Wheels,” yah).
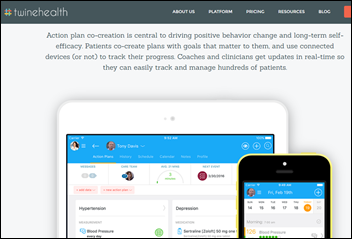
I ran across an article that mentioned Twine Health, which I’ve written about a couple of times. The company’s team-based coaching and primary care app offers shared action planning among patients, coaches, and clinicians; secure messaging; real-time population monitoring; and analytics. Practices can use its system for $1 per patient per month for up to 1,000 patients. The company has raised $6.75 million in a single December 2015 funding round. The founders are serial entrepreneur and former MIT professor Frank Moss, PhD and John Moore, MD, PhD.
A UCSF hospital medicine professor makes his case for “clinician data scientists” to analyze complex and sometimes inconsistently entered EHR patient information. He suggests training in clinical systems, data extraction, report writing, and statistical methods.
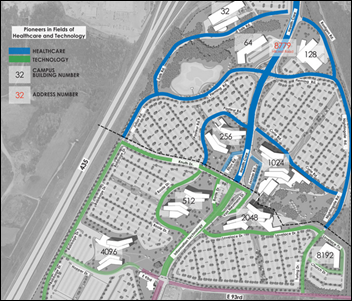
Cerner can honestly say that the company sits at the intersection of “Health Care” and “Information Technology” as it names the streets of its new campus. Other avenues are named after medical scientists and computing pioneers.
Eighty volunteers from HCA’s IT division participated in a 36-hour “Hack the Community” hackathon in Nashville this week, supporting local non-profits with limited technology resources.
Sponsor Updates
- Florida State University recognizes Vyne CEO Lindy Benton with its 2016 Distinguished Alumni Award.
- Forward Health Group COO Subbu Ravi will serve on panel discussing Wisconsin state health IT initiatives at a Wisconsin Technology Council innovation lunch in Madison on October 18.
- Iatric Systems will exhibit at the Hospital & Healthcare IT Fall Reverse Expo October 19-21 in Chicago.
- Momentum Partners includes ID Experts in its list of top 10 private cybersecurity companies to watch in Q3 2016.
- Impact Advisors will exhibit at the Scottsdale Institute CIO Summit October 13-14 in Scottsdale, AZ.
- Optimum Healthcare IT posts a white paper titled “The Problem (and Solution) With Data Governance.”
- InterSystems, Intelligent Medical Objects, NVoq, PatientKeeper, Streamline Health will exhibit at AHIMA October 15-19 in Baltimore.
- Kyruus will exhibit at the HMA Fall Forums October 19-22 in Laguna Beach, CA.
- MedData will exhibit at the ACEP Scientific Assembly 2016 October 16-19 in Las Vegas.
- Meditech Senior Manager Corinne Proctor Boudreau will speak at the Western Pennsylvania Healthcare Summit October 14 in Pittsburgh.
- Nordic will sponsor Piedmont Healthcare’s Southeast User Group Meeting October 18 in Atlanta.
- NTT Data announces its return to Chip Ganassi Racing Teams.
- Obix Perinatal Data System will exhibit at the ACOG Annual District II Meeting October 21 in New York City.
- Recondo Technology will present at the Michigan HFMA Fall Conference October 17 in Plymouth.
- Experian Health will present at NEHAM October 17-18 in Providence, RI.
- Red Hat accepts speaking proposals for Red Hat Summit 2017 through December 2.
- The SSI Group will exhibit at the AHCA/NCAL Annual Convention & Expo October 16-19 in Nashville.
- Sunquest Information Systems will exhibit at ASHG 2016 October 18-22 in Vancouver.
- Sutherland Healthcare Solutions VP and Global Health of RCMS Healthcare Tina Eller will speak at the Region 2 HFMA Fall Institute Conference October 20 in Verona, NY.
Blog Posts
- Healthcare Leaders Convene at 2016 Annual General Meeting and Fall Summit to Discuss Strategies for Expanding CommonWell (Meditech
- )Is Your Organization Trustworthy? 5 Essential Cybersecurity Promises to Keep (ID Experts)
- Digital Quality Management – Find Your Broken Link Before Your CEO Does (Influence Health)
- What Does it Mean to Offer a PCI-Validated P2PE Solution? (InstaMed)
- A Cable Care Named Interoperability: New KLAS Study Takes the Clinician View (InterSystems)
- ELearning = Painless EMR Adoption (Learn on Demand Systems)
- Radiology and MACRA: Using a Cloud-based Image Sharing Service to Address MIPS Quality Measures (LifeImage)
- Emergency Department Throughput: A Conundrum (Live Process)
- LogicStream Health Taste & Toast Recap (LogicStream Health)
- People are the Key to True Care Coordination (Netsmart)
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.



































































Sorry to be that guy, but "We remember the loss of Space Shuttle Columbia on its return" - Columbia exploded…