Top News

CMS publishes changes to the EHR Incentive Program that will allow returning EPs, hospitals, and CAHs to use any continuous 90-day reporting period between January 1 and December 31 for both 2016 and 2017.
CMS will also eliminate the clinical decision support and CPOE objectives and measures for hospitals and CAHs attesting under the Medicare EHR incentive program.
CMS says it is finalizing the process for a one-time EHR hardship exception for the Medicare EHR Incentive Program for certain eligible professionals for EPs who participate in the EHR incentive program in 2017 who will transition to MIPS in 2017.
Reader Comments
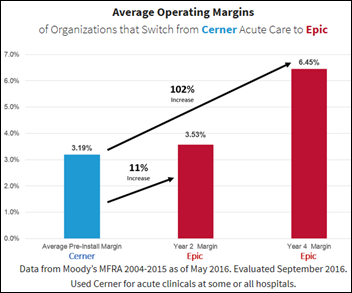
From Pilsner: “Re: Epic’s posted study showing the change in operating margins after switching from Cerner to Epic. The data are minimally cited and the methodology is not documented. It gives Moody’s as the source, but Moody’s rates only 441 hospitals and therefore the graph must not include all hospitals that implemented Cerner and Epic from 2004 through 2015.” I would be curious about how many hospitals this graphic represents. I’m also skeptical that a change in systems was the cause of the improvement as opposed to other, more impactful changes that coincided with that change (such as being acquired by a Epic-using health system that instituted its own superior revenue cycle practices). Also, the stated average margin improvement from 3.19 percent to 6.45 percent happened over years in which hospital margins improved in general and covered hospitals that could, by definition, afford Epic. There’s too little information to infer further, but Epic’s non-marketing team has done a nice job making a compelling point without providing the details in trying to discount the headlines describing hospitals whose Epic project expense got them in trouble.
From Master Blaster: “Re: [company name omitted]. Can you please remove the rumor you ran about us?” I sometimes get requests to take down a rumor, but I don’t do that, instead offering the company a chance to provide a response or to confirm/deny, which they generally decline to do. Invariably the rumor the company wants removed turns out to be accurate and they just wanted more time to spin it publicly. It’s the same when health system CIOs email me to rather sternly suggest that I contact them before mentioning items from public records indicating the cost and status of their big implementation projects – that information doesn’t seem to require IT clarification, but they’re always welcome to provide a comment. My conclusion after doing this for 13 years: everybody loves to read rumors except those that pertain to them, which instantly transform me from a must-read news-breaker to an irresponsible trouble-maker.
FHIR

Grahame Grieve provides a response to a reader’s question and my comments regarding FHIR.
World peace — we’ll do that next year. This year we sat it out because we wanted to handicap ourselves. (more seriously, Mr. H already quoted me about this).
From the original question, "After years of implementing HL7 and being able to do just about anything with an HL7 message," well, there’s all sorts of things you can’t do with HL7 v2, and ways you can’t do it, but for all the things you can do with HL7 v2, FHIR is an incremental improvement, not world shaking. But even there — testing, conformance, infrastructure — there’s still a lot in the increment.
"FHIR without discipline could turn out the same way if customers don’t demand better." Yes, but also vendors understand where the other approach ends up. We’ve lived it, and in today’s social media world, we can do better for much less. So it costs less to be disciplined, and as you said, there are other reasons to get it right this time.
"Providers understandably have no incentive to exchange data with their competitors." But banks exchange data with the customer, etc. Why? In fact, there are reasons to exchange some data, some times. It’s not a binary all-or-nothing, and some providers are keen to do it. Because of cost minimization, for example. And while data sharing might allow patients to shop between systems, it can also allow systems to shop to patients previously locked in. (more about this).
For these reasons, we — the FHIR team — believe that now is a great time to spend our effort creating a better way, and we live in hope that it will make a difference for patients across the world.
HIStalk Announcements and Requests

Ms. M reports that she’s using the iPad we provided in fulfilling her DonorsChoose grant request to assign specific reading interventions to her Texas first graders. She is also having the students record themselves as they work through the writing process, followed by taking a picture of their work and recording themselves talking the problems out.
Webinars
November 8 (Tuesday) 1:00 ET. “A CMIO’s Perspective on the Successful 25 Hospital Rollout of Electronic Physician Documentation.” Sponsored by Crossings Healthcare. Presenter: Ori Lotan, MD, CMIO, Universal Health Services. UHS rolled out Cerner Millennium’s electronic physician documentation to its 6,000 active medical staff members — 95 percent of them independent practitioners who also work in competitor facilities — across 25 acute care hospitals. UHS’s clinical informatics team used Cerner’s MPage development toolkit to improve the usability, efficiency, communications capability, and quality metric performance of Dynamic Documentation, embedding clinical decision support and also using Nuance’s cloud-based speech recognition product for the narrative bookends of physician notes. This CMIO-led webinar will describe how UHS achieved 70 percent voluntary physician adoption within one month of go-live, saved $3 million in annual transcription expense, and raised EHR satisfaction to 75 percent. It will include a short demonstration of the software that UHS developed to optimize the physician experience.
November 9 (Wednesday) 1:00 ET. “How to Create Healthcare Apps That Get Used and Maybe Even Loved.” Sponsored by MedData. Presenter: Jeff Harper, founder and CEO, Duet Health. Patients, clinicians, and hospital employees are also consumers who manage many aspects of their non-medical lives on their mobile devices. Don’t crush their high technology expectations with poorly designed, seldom used apps that tarnish your carefully protected image. Your app represents your brand and carries high expectations on both sides. This webinar will describe how to build a mobile healthcare app that puts the user first, meets their needs (which are often different from their wants), creates “stickiness,” and delivers the expected benefits to everyone involved.
Contact Lorre for webinar services. View previous webinars on our HIStalk webinars YouTube channel.
Acquisitions, Funding, Business, and Stock

Cerner reports Q3 results: revenue up 5 percent, adjusted EPS $0.59 vs. $0.54, missing analyst expectations for both. Shares dropped 2 percent at Tuesday’s close and were down another 6 percent in early after-hours trading. The company announced plans to offer a voluntary separation plan for eligible employees.
Telemedicine technology vendor Avizia closes its $17 million Series A funding round with a $6 million investment that includes the participation of New York-Presbyterian.

Meditech posts Q3 results: revenue down 7 percent, EPS $0.68 vs. $0.37. Product revenue declined 26 percent while service revenue increased 2 percent, but a 47 percent drop in sales costs boosted net income to $25.5 million.
Vital Images will acquire Karos Health, which offers “deconstructed PACS” diagnostic image viewing and sharing tools.

Private equity firm Blackstone Group will acquire hospital physician staffing outsourcer Team Health for $6.1 billion. The company was previously owned by Blackstone, which paid $1 billion for it in 2005 and then took it public in 2009. Team Health turned down a $7.6 billion acquisition offer last year after running up a pile of debt to finance the acquisition of a competitor that didn’t really work out.
Sunquest owner Roper Technologies announces Q3 results: revenue up 7 percent, adjusted EPS $1.63 vs. $1.61, falling short on revenue expectations but beating on earnings. The company said in the earnings call that Sunquest’s revenue is two-thirds recurring and therefore new orders aren’t usually that important, but the Lab 8.0 release and a new blood bank solution will cause a record number of Q3 orders.
A federal appeals court affirms dismissal of Fair Warning’s patent lawsuit against Iatric System regarding Iatric’s technology to detect fraud and misuse of PHI.
Sales
Baylor Scott & White Health will use technology from Pager to provide nurse triage services to patients seeking services.
People

Aetna promotes Patrice Wolfe to CEO of Medicity, where she will also be responsible for the company’s population health management technology products that include Healthagen Outcomes and HDMS.

Long-term care technology vendor MatrixCare hires Gary Pederson (Richland Advisors) as SVP of life plan community solutions.


Healthgrades promotes Andrea Pearson to EVP and chief marketing officer, Christian Dwyer to EVP of product management, and Chris Catallo (not pictured) to GM of hospital solutions.
Athenahealth hires Diane Holman (TE Connectivity) as chief people officer.
Announcements and Implementations
Health services price comparison vendor HealthSparq adds tools so that health insurers can offer their members financial rewards for choosing cost-conscious options, send them secure messages, and send them claims-based alerts to offer money-saving suggestions.
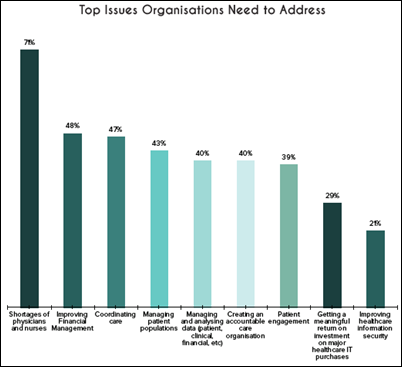
A Spok-sponsored, CHIME-administered survey of 100 CIOs finds that 81 percent name improving data security as their #1 priority over the next 18 months, while the top workflow they hope to improve with technology is care team coordination for treatment planning. Two-thirds are actively implementing secure messaging.
CareCloud will integrate population health management tools from Lightbeam Health Solutions into its EHR/PM.
Availity announces that its health information exchange technology will support the FHIR standard for eligibility, labs, diagnoses, medical attachments, and ADT and is developing a provider solution for member lookups.
Government and Politics
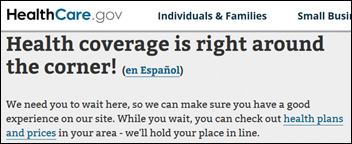
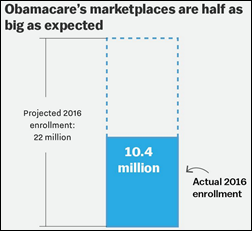
Healthcare.gov was apparently again overloaded on the first day of open enrollment, but at least the site provided a polite waiting room message instead of just timing out. I put myself in yesterday to compare to today’s new prices for 2017 and the premium for my theoretical coverage would be jumping 68 percent from 2016. I can say with confidence after looking up premiums for different parts of the country that a lot of self-employed folks who earn too much for federal taxpayer subsidies are going to be paying $1,000 per month or more for Silver-level coverage with a $3,500 deductible and $7,150 out-of-pocket maximum. Another option, I suppose, would be to purchase individual coverage directly from the insurance companies that offer it, but I don’t know if that would be a better deal than the exchange. A Wall Street Journal article says Arizona is the best example of the ACA’s problems in that most counties are down to only one insurer, premiums for some plans will more than double, and higher costs and cutbacks in the federal risk corridor program have caused nearly all of the insurers to pull out.

CMS awards its next round of Recovery Audit Contractor (RAC) contracts.
Privacy and Security
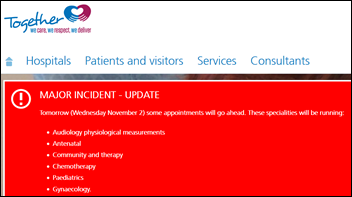
In England, the three hospitals of the North Lincolnshire and Goole NHS Foundation Trust cancel appointments and elective procedures as they go back to paper following an attack by an unspecified computer virus. The hospital hopes to restore its systems Wednesday following Sunday’s attack. They deny that ransomware is involved.
From DataBreaches.net:
- In England, a former hospital administrative employee is prosecuted for accessing the medical records of her former girlfriend and her partner.
- Three former district managers of drug company Warner Chilcott are sentenced for healthcare fraud and HIPAA violations trying to boost sales of the company’s osteoporosis drugs by using patient information to fill out prior authorization forms. The company’s drugs, Atelvia and Actonel, require doctors to justify why less-expensive generic drugs can’t be used, so the drug reps completed and submitted the forms using boilerplate text that was often unrelated to the patient’s condition. The company’s former president was arrested and charged with paying kickbacks last year (including bribing high-prescribing doctors with “honoraria” for speaking at events with no educational component) but was acquitted. Warner Chilcott paid $125 million to settle its criminal and civil liability and was acquired for $5 billion by Actavis.
Other

Among the proposed policies to be discussed at the AMA’s Interim Meeting in Orlando November 12-15 is integrating mobile health apps and devices into everyday practice. A draft resolution that calls out Epic and EClinicalWorks as “data blockers” would ask federal and state governments to prohibit withholding patient information from non-affiliated physicians and asks AMA to support legislation that would limit EHR vendor interfacing fees. Another proposed item seeks federal legislation that would eliminate medical practice costs involved with converting patient data from a replaced EHR to a new one.

Weird News Andy notes that this story is a few months old, but still amazing. A 14-year-old girl returns to competitive ballet dancing after having her leg amputated above the knee due to osteosarcoma, when was then repaired by attaching her foot backward to her upper leg in an uncommonly performed procedure called rotationplasty to give her optimal mobility.
WNA may regret going for the feel-good story above since he likes OR-related oddities such as this. A patient undergoing cervical surgery is burned when the laser ignites her passed gas.
Sponsor Updates
- HCI Group posts a podcast titled “Epic Upgrades: Key Strategies and Cost Considerations.”
- Aprima will exhibit at the American College of Phlebology event November 3-5 in Anaheim, CA.
- CenterX, CoverMyMeds, Cumberlad Consulting Group, Dimensional Insight, EClinicalWorks, and HealthCast will exhibit at the CHIME Fall Forum November 1-4 in Phoenix.
- CompuGroup Medical will exhibit at the National Association of Community Health Centers FOM/IT Conference November 2-4 in Las Vegas.
- Elsevier Clinical Solutions will present at the US News & World Report Healthcare of Tomorrow Conference November 2-4 in Washington, DC.
- Evariant will exhibit at the Healthcare Internet Conference November 7-9 in Las Vegas.
- KLAS names PerfectServe’s Synchrony as a top-performing care team communication platform.
- Extension Healthcare will exhibit at the HealthAchieve Conference November 7-9 in Toronto.
- Healthfinch will sponsor DevOp Days November 2 in Madison WI.
- Healthwise will exhibit at Wellcentive’s annual UGM November 2-4 in Atlanta.
Blog Posts
Contacts
Mr. H, Lorre, Jennifer, Dr. Jayne, Lt. Dan.
More news: HIStalk Practice, HIStalk Connect.
Get HIStalk updates. Send news or rumors.
Contact us.





























































I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…