News 3/21/14
Transcription and software vendor MModal files for Chapter 11 bankruptcy protection less than two years after being acquired by One Equity Partners for $1.1 billion. The company, which lists its assets and its liabilities between $500 million and $1 billion, says it is in “constructive discussions” with its lenders and bondholders regarding the terms of a consensual financial restructuring plan and expects to continue normal business operations throughout the restructuring process.
Reader Comments
From Experienced CIO: “Re: reader survey. I had to write to admire how many ways you politely declined to go down rabbit holes and chase information that is not within your (broad) span of knowledge. You are great at delivering what you know and show a comprehensive understanding of the business. Thus, I welcome your personal opinions and commentary. I also recommend that you discontinue HIStalkapalooza, which is a wonderful gesture when you were smaller, but has become unmanageable. Just invite everyone to get together at a cash bar and it will take care of itself in a year or two. Good job, well written, and you stick to your knitting. That is why your publication is so popular.” I appreciate the comments. I like the idea of a simpler, cheaper HIStalkapalooza, having initially envisioned a big parking lot or park with kegs of beer, grill-your-own hot dogs, and a band. Dr. Travis from HIStalk Connect wanted me to put something like that together for startups at HIMSS, but the idea didn’t come up until too late. I’m considering options for next year. Party planning isn’t my core competency.

From Arcanity: “Re: your poll about professional certifications on your business card. I think this guy takes the cake.” Looks like either a big ego or a small … well, you know. Diplomate-ically speaking, his business card must be the size of a poster board.
HIStalk Announcements and Requests
![]() A few of the stories you may have missed this week on HIStalk Practice: CMS offers a free online tool to help small practices transition to ICD-10. Over 60 percent of practices don’t plan to participate in an ACO. A reader suggests that Practice Fusion, CareCloud, and ZyDoc might follow Castlight’s IPO lead within the year. The potential costs associated with information loss during the ICD-10 transition could be substantial. Four major insurance carriers tell the AAFP they’ll be ready for ICD-10 by October 1. NCQA intends to raise its PCMH recognition standards in 2014. Thanks for reading.
A few of the stories you may have missed this week on HIStalk Practice: CMS offers a free online tool to help small practices transition to ICD-10. Over 60 percent of practices don’t plan to participate in an ACO. A reader suggests that Practice Fusion, CareCloud, and ZyDoc might follow Castlight’s IPO lead within the year. The potential costs associated with information loss during the ICD-10 transition could be substantial. Four major insurance carriers tell the AAFP they’ll be ready for ICD-10 by October 1. NCQA intends to raise its PCMH recognition standards in 2014. Thanks for reading.
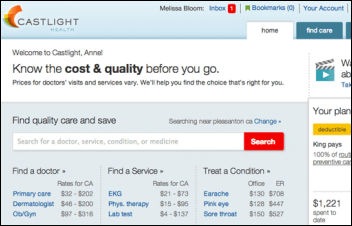
This week on HIStalk Connect: Castlight Health shares soar 149 percent on the day of its IPO. Physician-only social networking site Doximity reaches 40 percent market penetration with US physicians. SharePractice launches a mobile app designed to let doctors use crowdsourcing to collaborate on and rank the best approaches to treating specific conditions. Dr. Travis dissects the recent failings of Google Flu Tracker and its implications on big data at large.
Welcome to new HIStalk Platinum Sponsor NYeC (New York eHealth Collaborative). NYeC is New York State’s not-for-profit public resource for healthcare IT, facilitating the EHR transition for providers and improving healthcare for all New Yorkers. Its activities include the SHIN-NY HIE; NYeC Regional Extension Center serving the upstate region and Long Island; the multi-state EHR-HIE Interoperability Workgroup; and the Patient Portal for New Yorkers that will go online this year. It runs the New York Digital Health Accelerator along with the Partnership Fund of New York City, supporting early- and late-stage digital health companies working on care coordination, patient engagement, predictive analytics, and workflow management. Chosen companies, which are required to have a New York presence, receive $100,000 in upfront funding and participate in a leadership program of healthcare leaders, entrepreneurs, and investors for the five-month term. Applications for the 2014 class are due April 11. The class of 2013 included ActualMeds, Aidin, Avado, CipherHealth, Cureatr, MedCPU, Remedy Systems, and SpectraMedix. Thanks to NYeC for supporting HIStalk.
Here’s my free “how not to look stupid” tip of the week: don’t reply to business emails on your phone. I see this constantly: the sender doesn’t notice incorrect spellcheck changes, they write barely intelligible terse text that makes little sense, and the tiny keyboard makes it too much trouble to make desirable changes to the subject or to the “Sent from my iPhone” email signature that indicates they are dashing off a reply on the fly while doing something else. You would be better composing a more thoughtful reply on a real computer later unless it’s an emergency.
Upcoming Webinars
April 2 (Wednesday) 1:00 ET. A Landmark 12-Point Review of Population Health Management Companies. Sponsored by Health Catalyst. Presenter: Dale Sanders, SVP, Health Catalyst. Learn the 12 criteria that a health system should use to evaluate population health vendors and to plot its internal strategy, then see the results of grading seven top PHM vendors against these criteria. No single vendor can meet all PHM needs. The most important of the 12 criteria over the next three years will be precise patient registries, patient-provider attribution, and precise numerators in patient registries.
Acquisitions, Funding, Business, and Stock
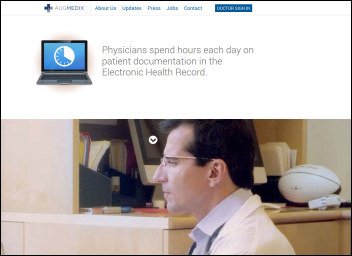
Augmedix, a startup building clinical applications for Google Glass, secures $3.2 million in venture funding.

CitiusTech announces an investment partnership with General Atlantic. The company, which works with 50 healthcare organizations worldwide, reported 2013 revenue growth of 51 percent.
HIMSS acquires Harrogate, England-based conference promoter Citadel Events, renaming it HIMSS UK.
Social health management vendor Welltok acquires wellness game developer Mindbloom.
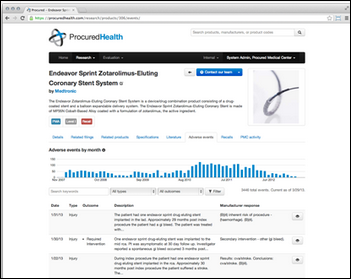
Procured Health, which offers software that manages hospital purchases of medical devices, raises $4 million in a Series A round.
Sales
The New England Healthcare Exchange Network will implement the Ability Secure Exchange Platform across its member hospitals and provider sites.
Mercy Orthopedic Hospital Springfield (MO) selects Emmi Solutions for patient engagement.
Adventist Health Hospitals (CA) will deploy Aperek Ellipse for real-time anytime spend visibility and analytics.
BJC Healthcare (MO) selects Health Language to assist with its transition to ICD-10.
People

Clinovations promotes Kevin Coloton from COO to president.
Announcements and Implementations
Methodist Healthcare (TN) deploys MedAptus Professional Charge Capture for inpatient coding and billing.
La Clinica del Pueblo (DC) goes live on Forward Health Group’s PopulationManager and The Guideline Advantage.
The Nashville paper profiles RoundingWell, the patient engagement software company launched by the founder of bulk email software provider Emma. It uses EHR-generated information to send patients questions, education, and guidance from a proprietary content library developed with Vanderbilt University School of Nursing and The Center for Case Management. A tiny study found that patient engagement rates were at 60-70 percent over 90 days, with the average patient having eight risks identified that it says wouldn’t have been addressed otherwise.
Aprima offers Etransmedia customers running Allscripts MyWay a conversion to Aprima Patient Relationship Manager, hosted by either Aprima or Etransmedia.
HealthEast Care System (MN) goes live with an early intervention program for heart failure patients that uses patient engagement technology from Pharos Innovations.
Catholic Health System (NY) deploys Juniper Networks Meta Fabric, an open standards-based architecture for data centers.

Sanford Health (ND) completes the installation of RTLS technology from Sonitor Technologies and Intelligent InSites at Sanford’s soon-to-be-opened Moorhead clinic.
Government and Politics
OIG testing of the 28-hospital Indian Health Services computer network reveals inadequate security and significant network vulnerabilities. OIG hackers were able to gain unauthorized access to the IHS web server and an IHS computer, as well as obtain user account and password data and records in the IHS file system.
The HHS Office of the Assistant Secretary for Preparedness and Responses and ONC launch an initiative to promote the use of HIT in emergency medical services.
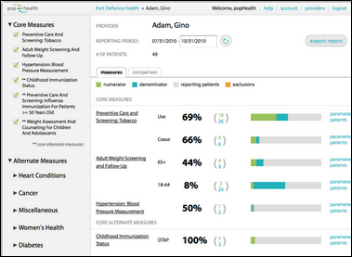
ONC announces that its open source popHealth tool to process electronic clinical quality measures has been certified as a 2014 edition EHR module.
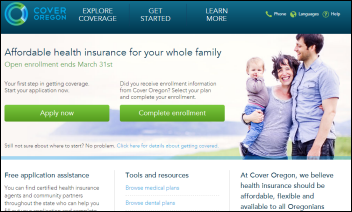
Oregon Governor John Kitzhaber fires the head of the state’s health authority and asks Cover Oregon to replace its senior management team, including the CIO and COO, following an independent investigation. Cover Oregon remains the only state whose exchange, which cost $200 million, hasn’t enrolled a single person after its planned October 1 rollout failed. The report concluded that the state’s managers had too much confidence that Oracle, which has been paid $160 million so far, could deliver what it promised.
Innovation and Research

Harvard University Medical School researchers find that use of the EarlySense monitoring system on a medical-surgical unit was associated with a significant decrease in length of stay, code blue events, and ICU stay times. EarlySense uses a sensor that is placed under a patient’s mattress to detect potential adverse events, as well as monitor heart and respiratory rates and movement.
A study finds that facial recognition software beats humans at detecting patients who are faking pain, with accuracy of 85 percent vs. 55 percent.
Other
An ONC-commissioned review of nine RECs finds that their most difficult challenges are poor EHR product usability and the “unsavory” business practices of some vendors. Other struggles include physician resistance to EHRs and the MU program, sustainability of RECs once federal funds are depleted, and difficulties communicating often confusing details of the MU program. The authors also note three best practices that emerged for helping providers achieve MU:
- Maintain strong partnerships with the community
- Hire technical employees who that have a mix of IT skills, clinical understanding, and general business understanding
- Work with a physician champion.
The Business Journals names its “10 Markets with the Strongest Brainpower”: Washington DC, Madison, Bridgeport-Stamford, Boston, San Jose, Durham, San Francisco-Oakland, Raleigh, Minneapolis-St. Paul, and Colorado Springs.

Supply chain software vendor Global Healthcare Exchange, acquired by private equity firm Thoma Bravo a week ago, reportedly lays off 130 of its 500 employees.
Google CEO Larry Page, speaking at a TED conference in Vancouver, touts the sharing of medical records, saying, “Wouldn’t it be amazing if everyone’s medical records were available anonymously to research doctors? We’d save 100,000 lives this year. We’re not really thinking about the tremendous good which can come from people sharing information with the right people in the right ways.” He described losing his voice because of an undocumented condition and finding thousands of people with the same problem after posting a description online.
St. Luke’s Health System (ID), which lost an antitrust lawsuit filed when it attempted to buy a physician group and used its Epic system as one of the benefits, receives a $10 million legal bill from the the hospital, surgery, center, and attorney general that successfully sued it.
Cerner is among 23 Kansas City-area employers recognized for their commitment to lesbian, gay, bisexual, and transgender equality.
Doctors in England using Skype to check on a home dialysis patient notice her husband collapsing in the background and send an ambulance to help the 70-year-old man, who was later found to have bowel cancer.
Sponsor Updates
- ScImage will deliver its PICOM365 PACS with Cedaron’s CardiacCare.
- Direct Consulting Associates joins the HIMSS Innovation Center in Cleveland as a Supporting Collaborator.
- CommVault will add 250 jobs in the next three years at its 275,000 square foot headquarters under construction in Eatontown, NJ.
- Pandodaily.com spotlights Validic and its data pipeline solution for healthcare.
- GetWellNetwork sponsors the 28th annual National Disabled Veterans Winter Sports Clinic March 30-April 4 in Snowmass, CO.
- Emdeon CEO Neil de Crescenzo tells the Nashville Business Journal that his company has hired 100 people in the last six months.
- AdvanceNet Health Solutions will add the CoverMyMeds ePostRx automated prior authorization solution to its enterprise pharmacy management platform.
- Summit Healthcare partners with Indigo HIT to offer complimentary services to enable clients with streamlined and scalable CCD integration.
- Kareo adds Rignadoc to the Kareo Marketplace to help physicians with phone triage.
- ICSA Labs certifies First Databank’s MedsTracker as a 2014 Edition Ambulatory and Inpatient Modular EHR.
- The Ethisphere Institute names Premier a 2014 “World’s Most Ethical Company” for the seventh consecutive year.
- Angela Hunsberger, senior consultant for Hayes Management Consulting, discusses the need to balance security and usability in patient portals.
- Healthcare services firm Accreon partners with identity management solution provider NextGate to deliver services and technology for enterprise data awareness and exchange.
- RelayHealth Financial releases RelayClearance Plus 5.0, a pre-service financial clearance solution that includes an eligibility benefits detail viewer.
- Clinithink launches its suite of CLiX Online Solutions to translate unstructured clinical narrative for real-time use.
- TeleTracking Technologies names Hill-Rom a licensed reseller of TeleTracking’s asset and temperature tracking software, while Hill-Rom extends re-sale rights to TeleTracking for its hand hygiene compliance solution.
EPtalk by Dr. Jayne
I spent all day Tuesday at yet another continuing education class to recertify a life support certification. This is the last one until summer, so I’m glad to have a break.
I understand why they require us to stay certified, but the odds of my actually having to participate in a code situation in the hospital are pretty slim based on my clinical practice patterns. I’m more likely to have to use basic CPR at the supermarket than any of the other skills, which I guess is a good thing. This year I took the “independent study” course, which included an online pre-course as well as the in-person practice and skills testing sessions using a computerized mannequin.
In some ways, the certification seems like a racket. This week confirmed my thoughts. The health system I work for has a master license to be able to train staff on adult cardiac life support because they require most of the clinical staff to maintain certification. I have no idea how much that master license costs, but I know that the individual certification fee is $220 because I had to pay it out of pocket.
In a quirk of rule-making, since I’m not employed by the hospital in a clinical service line (my Emergency Department work is through a third-party contracting firm), there isn’t a department to cost it back to. Apparently neither the administration or IT cost centers are valid for the education department to use, which makes me nervous that someone thinks administration and technology don’t need continuing ed.
At other hospitals (such as the one where I take my pediatric course) the fee for the all-day course includes the textbooks and lunch, but ours doesn’t. I’m a girl who knows how to brown bag and I don’t mind not being allowed to keep the books because I’m never going to look at them again. Neither of those are that big of a deal, but the twist at the end of this course was unbelievable. When we turned in our evaluations at the end of the day expecting to pick up our certification cards, we were asked to pay an additional $2.25 (in cash) for the actual card. Talk about unbundling!
Hospitals are infamous for nickel and diming patients. I suppose I shouldn’t be surprised that they’re now doing it to the medical staff and the independent contractors who fill the positions they can’t staff on their own. When I registered for the course, I had to wait until my check had cleared to actually schedule it and borrow the text books. I thought that was a little weird, especially since I’ve been on staff for more than a decade and they know where to find me if the check bounced, but I understand not everyone is that reliable. Incidentally, the pediatric hospital takes online payments for their courses, so they don’t have the check cashing issue.
My suggestion to the education department was to just raise the course cost to $222.50 (or even $225) so that they’d have the full payment up front and not ask for cash at the end of the course. I was told that the clinical departments only allowed $220 for the course and the reason they charge for the card was because the “regular employees” don’t actually need the card, they just need a statement from the education department that they had passed the course. Only “external” attendees need the card, hence the extra charge.
I guess external is a nicer way to say that I’m an irregular employee, or to possibly admit that our hospital is so cheap they won’t pay $2.25 for the 20 or so “external” attendees who take the course each year. Or that they’re ignoring the cost savings of recycling textbooks that they’re charging individuals for.
I’m afraid that as healthcare reform evolves, this is only going to get worse. Our hospital has hired a fleet of financial staffers to micromanage every facet of patient care (without admitting they’re telling physicians how to practice medicine) at the same time they’re cutting positions for nurses and patient care technicians. They were already in the business office, where I did battle over the fact that I can only order one printer cartridge at a time (despite the fact that they’re cheaper in a two-pack) due to new purchasing rules. They were already on the hospital floors, where we have to bar code scan every gauze pad and bandage we touch. Now they’re even in CPR class.
We are the embodiment of penny-wise and pound-foolish. I’m curious about the trends our readers are seeing in the hospital or clinic. Has everyone gone as mad as my employer seems to have gone? Are we headed towards the level of care seen in other parts of the world, where patients are expected to provide their own bandages and meals? Email me.
Contacts
Mr. H, Inga, Dr. Jayne, Dr. Gregg, Lt. Dan, Dr. Travis, Lorre.
More news: HIStalk Practice, HIStalk Connect.

.






































































































































Re: Deliberately Faked Academic Papers in Nature See, this doesn't surprise me at all. Of course AI quotes these bogus…