I doubt much has changed with the former Cerner except that Safra stopped ripping the business after Oracle ended breaking…
Monday Morning Update 3/27/23
Top News
ProPublica says that Cigna’s reviewing doctors use “auto-denial” software that allows them to declare a patient’s test as medically unnecessary in an average of 1.2 seconds, without ever looking at the patient’s medical records.
A former Cigna executive says that it’s easier for the company to just deny everything knowing that policyholders will appeal its decision only 5% of the time, not to mention that is saves hundreds of dollars of research time per test by simply rejecting claims using a procedure-to-diagnosis table.
Featured prominently in the article is health IT long-timer Nick van Terheyden, MBBS, who dug into Cigna’s process when they refused to pay for his own test that he knew as a doctor was medically necessary.
Reader Comments
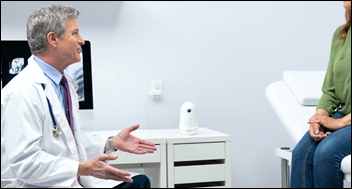
From Ricochet Rabbit: “Re: ambient notes. My doctor asked if I was OK with her using an ambient automated note taker to help her with the progress note. She said it wasn’t as good as Robin, which she has used elsewhere. I can imagine systems identifying key clinical concepts from the discussion and then use ChatGPT to create a progress note.” Accurately summarizing transcribed encounter conversations seems well within even today’s AI capabilities. It would also encourage doctors to communicate their thoughts to the patient, maybe as an intentionally spoken end-of-visit summary. The result could be like a research article’s abstract that tells most readers all they need to know about the article that follows. Robin is a smart assistant for creating clinical documentation for orthopedics, capturing both audio and video from the exam room that are then used by virtual scribes to deliver SOAP notes. The information is collected by a dedicated hardware device and then can be changed or enhanced afterward via the Robin app. I first mentioned Robin when it was released in May 2018.
HIStalk Announcements and Requests
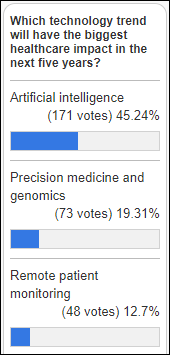
Results from last week’s poll aren’t surprising, neither for the top vote-getters (above) and the bottom-finisher ones (Internet of Things, blockchain, and virtual reality).
New poll to your right or here: From your most recent patient experience with a health system, how would you grade their use of digital tools? I personally don’t mind manual and/or outdated consumer-facing technology as long as the people themselves are empathetic and friendly. My problem is that the people who shove poorly-designed paperwork at you via a clipboard are often arrogantly uninterested in what you think as a customer. Sometimes I wonder if their candidate pool is made up of people whose customer service skills were insufficient to keep their jobs at DMV.
Welcome to new HIStalk Platinum Sponsor JTG Consulting Group. The Miami Shores, FL-based boutique consulting company – which was founded in 2018 by President and CEO Jamel Giuma — specializes in laboratory IT, supporting EHR and laboratory strategies in health systems of all sizes. With 400 years of combined experience, the talented JTG advisory staff has established many longstanding relationships with health systems, providers, and vendors across the industry. It provides vendor-agnostic, patient-centric, and tailored IT services and solutions that help clients maximize interoperability, operational efficiencies, and revenue opportunities. JTG also offers advisory services to help organizations find the optimal path for achieving their strategic vision , helping affect sustainable success through short-term critical turnarounds and instituting long-run foundational changes. The rapidly growing company prides itself on on-time completions, cost effectiveness, and quality of product outcome. It scored 96.1 in an October 2022 report by KLAS Research, with 100% of clients saying they would buy again, and was #7 in Best in KLAS in the HIT Staffing category. Thanks to JTG Consulting Group for supporting HIStalk.
ReMedi Health Solutions will attend ViVE23, so I’ve added them to my sponsor guide for the conference. Ditto Nuance, which should be a fun booth visit given recent DAX and Microsoft ChatGPT-4 announcements.

Speaking of conference guides, sponsors can send me their HIMSS23 participation details for that upcoming guide. It’s easy, it’s free, and you will likely get some booth visitors you would have missed otherwise (especially if your booth features interesting presentations or perhaps site-baked scones).
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present or promote your own.
People

TriHealth promotes Donna Peters, MBA to SVP/CIO.
Announcements and Implementations

A new KLAS report finds that EHR personalization is the biggest driver of provider satisfaction, although those providers often feel they don’t get much support and that area and resort instead to personal initiative. Nurse aren’t given many options for EHR personalization, so the top success factor for them is being proactive about learning the EHR.
Government and Politics
The federal government will solicit bids to provide services that have been offered by non-profit United Network for Organ Sharing, which has run the country’s transplant program for 40 years. The government’s top priority is replacing the organ-matching computer system in hopes of shortening transplant wait lists and addressing racial inequity.
The National Labor Relations Board clarifies that a February ruling prohibits employers from including non-disparagement or confidentiality clauses in their severance agreement, also noting that the ruling is retroactive and such clauses that are contained in already-signed agreements are nullified by the ruling. The original case involved a Michigan hospital whose severance contracts contained clauses that violated the labor rights of employees.
Sponsor Updates
- Potomac Urology achieves growth with EClinicalWorks EHR and Healow patient engagement solutions.
- Optimum Healthcare IT names Natalie Tollefson HR service delivery director.
- Pivot Point Consulting will sponsor the OCHIN Learning Forum April 2-5 in Las Vegas.
- Volpara Health will exhibit at the National Consortium of Breast Centers conference in Las Vegas through March 27.
- West Monroe Managing Partner Tom Hulsebosch retires to launch the Hulsebosch Hope Foundation, a family foundation that funds public charities that seek to serve the needs of under-resourced communities in Chicago.
Blog Posts
- National Guidelines for Child and Youth Behavioral Health Crisis Care: SAMHSA’s Response (Netsmart)
- Leverage Generative AI to Liberate Information Critical to Patients, Providers (Orbita)
- Medical Answering Services: Urgent Versus Non-Urgent Calls (PerfectServe)
- Accounts Payable Automation in Healthcare: It’s Not Just for Hospitals (Premier)
- How to Track and Measure Provider Support Activities in Real Time (RCxRules)
- Place your bets on data (Redox)
- 3 hospital contact center metrics that indicate the health of your operations (Spok)
- Post-Public Health Emergency Changes to Patient Care (Surescripts)
- Speeding AI implementation in the contact center (Talkdesk)
- Simple Strategies to Boost Online Visibility: A Guide for Rehab Therapists (WebPT)
- From Theory to Reality: Realizing the Elusive Promise of Value-Based Care (Zynx Health)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.




The Cigna operational model closely resembles the fictional insurance company that is at the center of John Grisham’s novel The Rainmaker, which was made into a movie in 1997 starring Matt Damon and Claire Daines. In the story, a young man is denied coverage for cancer, and he succumbs from his illness. In the ensuing jury trial, a former employee of the insurer testifies that she was instructed to deny all claims and not allow any medical review, since very few of the company’s subscribers would request an appeal.
re: Cigna payment model/denials – this is not surprising at all. I had a client sue another large national payer many years ago. As part of the settlement agreement, the affected facility was granted access to the payer’s claims facility to witness the reprocessing of claims. One of the things they noticed on day 1 is people in the call center with no computers, telling callers they don’t have the claim on file, to resubmit it. It’s harder for them to pull that off now as claims go electronically and you can prove the accepted the claim.
I encourage everyone to engage with your local insurance commissioner and understand the medical billing laws in your state. Then be armed with that info when you appeal claims. I have many independent clinic clients in Oregon and Washington State, they have very strong MGMA local chapters who work in concert with the local medical societies and their legal teams to hold payers accountable. I encourage all clinic managers and administrators to engage with your local MGMA chapter and become a force for good.
I remember years ago hearing someone talk about a (certain unnamed payer)’s adjudication process when they asked for supporting medical records. They required that the supporting documentation to be stapled to the paper claim. When they documentation was received, the person opening the envelope would pull apart the claim and the medical record. They’d put the claim in one pile, the medical record in the other, and both would be sent off for review, after which the claim would be denied for missing supporting documentation.