TBF the anti-hate non profit was funding undercover investigators trying to being down the KKK & has done successfully for…
Monday Morning Update 7/18/22
Top News
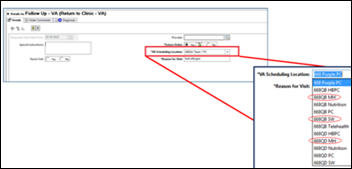
A VA OIG report concludes that the VA’s use of an “unknown queue” in its Cerner system caused multiple events of patient harm in which orders failed to reach their intended care location. Notes from the report:
- The system failed to deliver 11,000 orders in which clinicians chose a service location that didn’t match the type of service that they were ordering.
- The system did not notify the clinicians that their order had not been delivered, and in fact assured them that their order had been accepted.
- The VA learned of the unknown queue’s existence when it opened its first Cerner trouble ticket about the problem four days after go-live, after which the VA instructed staff to monitor the queue and cancel and re-enter the problem orders.
- Cerner says that a a VA leader had approved the use of the unknown queue in January 2020, but that leader and their supervisor say they weren’t aware of it.
- Cerner created a provider alert for their undelivered orders in February 2022, but the VA said that the solution wasn’t adequate.
- The OIG did not accept the response to its report from VA Deputy Secretary Donald Remy because it failed to address the report’s key finding that patients were harmed.
- Remy says that Cerner and the VA were both aware of the queue’s existence before go-live, but OIG says it was provided with no evidence to support that statement and that users weren’t informed about the queue until a year after go-live.
- OIG says it it is “troubling” that Remy absolves Cerner for failing to educate VA about the unknown queue and instead blames VA users for the negative outcomes it caused.
- OIG also notes that both the Deputy Secretary and EHRM IO executive director were aware of the patient harm that resulted, but in their testimony to Congress, they insisted that no harm had occurred.
A second new VA OIG report looks at the VA’s Cerner training:
- VA project executives sent misleading information to OIG in to a “careless disregard for the accuracy and completeness of the information.”
- VA showed OIG a training evaluation plan without disclosing that the plan had not been reviewed, approved, or implemented.
- OIG was given a slide that showed the user proficiency pass rate at 89% instead of the actual 44%, then explained the error as being due to removing a small number of outliers who had taken and failed the test up to 29 times. VA had not calculated the numbers until it received OIG’s request.
HIStalk Announcements and Requests
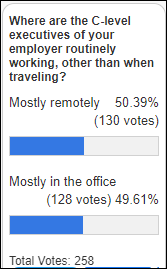
It’s pretty much an even split between C-level executives working from home or from the office. I’m surprised – I thought more of the C-suite would have returned to the office.
New poll to your right or here: How worried are you that your employer will lay you off, demote you, or force you to relocate in the next 12 months?
Thanks to new HIStalk Platinum Sponsor West Monroe, which is upgrading from Gold. The digital services firm was born in technology but built for business, partnering with companies in transformative industries to deliver quantifiable financial value. It believes that digital is a mindset—not a project, a team, or a destination—and is something that companies become, not something they do. That’s why it works as diverse, multidisciplinary teams that blend management consulting, digital design, and product engineering to move companies from traditional ways of working to digital operating models and create experiences that transcend the digital and physical worlds. Thanks to West Monroe for supporting HIStalk.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
Private equity firm Veritas Capital acquires Coronis Health, which offers physician billing and RCM. Axios speculates that Veritas will acquire one of several potentially available privately held RCM company and combine it with Coronis Health.
A fascinating Brookings report looks at Medicare Advantage insurance market, which is good timing since the eye-popping paper valuations of some tech-focused players are being shredded in a more scrutinizing stock market:
- MA represents 46% of all Medicare beneficiaries.
- Two-thirds of enrollment is concentrated among five big insurers – UnitedHealth Group, Humana, CVS/Aetna, Kaiser Permanente, and Anthem.
- These large companies have other businesses that provide services to their MA plans, such as Humana-owned Kindred’s home health and hospice services and three of the five that operate pharmacy benefit managers. Profits in those related businesses are shielded from medical loss ratio requirements, which places smaller insurance competitors at a disadvantage..
- Nearly all of the plans bid rates that are lower than Medicare fee-for-service, but plan payments are 104% of Medicare spending in generating net profit margins of 5%. However, big insurers have accounting flexibility when they operate multiple insurance product lines and related businesses that sell services to their MA plans, so their true profit and pricing competitiveness are hard to determine.
Sales
- Bedrock Management Services chooses CareCloud Remote solution for home healthcare practice groups, which it will implement at 33 locations in seven states.
- Starting Point Behavioral Healthcare will implement Owl’s measurement-based care platform, which offers evidence-based measures and predefined measure bundles to give clinicians actionable insights.
- Sutter Health signs a 10-year contract to make R1 RCM its exclusive provider of enterprise revenue cycle management services, with 1,150 Sutter employees being assigned to R1 RCM.
People

Tanner Health (GA) promotes Bonnie Boles, MD, MBA to SVP/CMIO.

Joe Bajek (Centura Health) joins Lifespan as VP/CTO.
Other
So many lessons to be learned here. A company that runs a video game operator in which players can earn cryptocurrency by battling Pokemon-like characters loses $620 million in crypto when one of its engineers falls for a fake job offer on LinkedIn. North Korea-based hackers posed as job recruiters on LinkedIn, got a bite from an engineer at game developer Sky Mavis, took the engineer through several rounds of interviews, and then sent him a generous offer letter in the form of a PDF that was loaded with spyware that gave the hackers access to the company’s blockchain network.
Sponsor Updates

- Volunteers from Arrive Health (formerly RxRevu) help Denver-based mental health provider WellPower prepare its ADA-accessible garden space at its Dahlia Campus for Health and Well-Being Market Farm.
- Quil publishes a new white paper, “Bridging the Gap Between Patient Engagement Solutions, The Provider Experience.”
- Relatient will offer TriZetto Provider Solutions customers access to its Dash patient scheduling and engagement suite of solutions.
- Talkdesk publishes a new report, “The Future of AI 2022: Progressing AI Maturity in the Contact Center.”
- Clearsense posts “Top 5 Spots to Check Out in Madison at the Epic UGM.”
- TigerConnect releases a new episode of The Connected Care Team Podcast, “A Conversation on the Next 10 Years of Healthcare Transformation.”
Blog Posts
- 4 Signs an Urgent Care Needs to Improve Their Patient Experience (PatientBond)
- 3 Questions to Ask Before Choosing a Healthcare ERP System (Pivot Point Consulting)
- Northwest Health Adopts Artificial Intelligence Technology to Enhance Maternal and Fetal Safety (PeriGen)
- Best Practices for Healthcare Software Deployment (PerfectServe)
- Celebrate the “Insiders” of Healthcare Value During Value Analysis Week (Symplr)
- Accelerating the APM Adoption with Rural Providers (Premier)
- Unpacking HIMSS Research Insights (Redox)
- Patient-Centered Marketing: 7 Strategies to Drive PT Self-Referrals (WebPT)
- Identity is More Than a Hospital Bracelet: How to Get Person Data Right Every Time (Verato)
- Not All Interventions Are Created Equally (Zynx Health)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.




“When reason sleeps – monsters are born” (Goya, 1798)
Disclaimer – I worked for Cerner and a large Midwest religious health org that was trying to implement the extremely-patient-dangerous EHR called Millenium.
1. Cerner never listened to its customers’ base – not for the requirements specs nor for testing.
2. Cerner EHR was created by a bunch of unsupervised idiots and it shows.
3. The attitude that the user is the one to blame, because the user has a license to defend – doesn’t improve the quality of a software product.
4. VA had plenty of fair warnings regarding the Cerner EHR from others’ installs – but it chose to disregard it
If harm resulted from the Cerner ‘unknown queue’ – a class action suite or similar should follow. Remember that Oracle / Cerner / VA – have the funds necessary to cover the damages caused.
Now what is needed is a sympathetic judge & jury to cause these incompetents a slight financial hiccup.