I've figured it out. At first I was confused but now all is clear. You see, we ARE running the…
Monday Morning Update 4/20/20
Top News
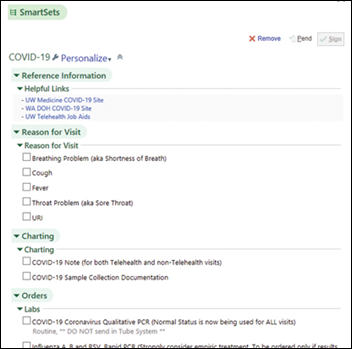
UW Medicine (WA) publishes its IT experience with COVID-19 in the journal Applied Clinical Informatics. The organization:
- Participated in the hospital incident command system.
- Moved to iterative implementations in some areas, such as escalating COVID-19 related EHR change requests.
- Developed a real-time dashboard of critical metrics.
- Worked with HR and local sites to develop internal email lists for specific areas and topic types, including a master list of EHR users for change notification.
- Worked with groups that oversee community communication (websites, automated emails, appointment reminders, on-hold contact center telephone messages) to align messaging.
- Created intranet and extranet pages to house COVID-19 resources, with the former including screening and testing algorithms, policies and procedures, and printable posters for clinics.
- Developed workflows for specimen collection for the organization’s self-developed COVID-19 lab test to cover new areas (such as employee health) and to print labels for community organizations that still use paper and faxed orders.
- Developed COVID-19 lab ordering under easily found synonyms and configured those orders and related interfaces to bypass the co-signature requirement.
- Created a master order set that includes hyperlinks, lab orders, ICD-10 codes, billing codes, and discharge instructions.
- Created a documentation template that includes a checklist of symptoms and risk factors, testing recommendations, and support for virtual visits.
- Implemented a centralized lab results notification process since the lab is serving non-UW Medicine patients, using remote professionals to monitor an EHR inbox and communicate positive and inconclusive results and posting negative results within one hour on the patient portal for established UW Medicine patients.
- Trained 500 primary care physicians in telemedicine, then extended the service to areas that serve vulnerable patients. This involved acquiring equipment, managing software licenses, supporting remote access, and integrating teleconferencing into Epic.
- Masked the personal telephone numbers of providers who are conducting virtual visits remotely by using Doximity Dialer or the phone system’s call forwarding feature.
- Set up ICU telemedicine carts with cameras to allow practitioners to conduct visits remotely and thus save PPE.
- Supported surge planning by providing emergency-level system access, EHR changes, EHR expansion to new areas, and support for a drive-through testing site with cellular hotspots that were later replaced with microwave line-of-sight connectivity.
- Supported teleworking by extending teleconferencing, VPN, and file-sharing tools and helped employees check out their desktop equipment for home use.
- Fended off an increase in phishing attempts and malware.
- Learned these three lessons: (1) integrating videoconferencing into the ambulatory EHR should have been given higher priority; (2) expanding the telemedicine solution would have helped, including ramping up training and installing more cameras; and (3) a larger supply of equipment to support teleworking and telemedicine would have been beneficial.
Reader Comments

From Show Me The Shortage: “Re: LexisNexis COVID-19 drill-down of provider and hospital bed shortages. Seems like the socio info could be used for flattening the curve, or at least being proactive for prep for health crises.” I wondered how LexisNexis was getting the data to display at-risk populations, community shortages of critical care resources, and COVID-19 deaths (that’s the death map above). They aren’t, exactly – the age, comorbidity, and socioeconomic data is based on historical national percentile rankings, while the critical care resource shortage display is derived from comparing the high-risk population percentage with the known number of specialists, hospital beds, and ICU beds (it’s not a real-time snapshot). They don’t say where they’re getting COVID-19 death counts, but I assume it’s Johns Hopkins since they credit them as a dataset resource. It’s an interesting exercise in data presentation, but I would say it is questionably actionable in a pandemic crisis where none of the factors that are modeled can be changed in the short term. I also question the usefulness of dividing the data by county since we are hardly constrained by those virus-indifferent borders in seeking the closest medical care. All of this is the kind of information needed to plan a war, not fight one, and we are still massively failing in even basic public health execution, such as getting people tested and protecting providers with basic gear.
From Another Doctor Who: “Re: whole-body doctors. Here in the Midwest, doctors who can treat an entire human are not rare. I realize you are inured by loud reports of professionals behaving badly, but the good clinicians are not making noise. They are just practicing their trade and attempting to be human themselves. Here’s how I know I am surrounded by holistic physician colleagues: When I have a family or friend that needs a referral, I have multiple choices, even to the point of not referring too many to one person, matching up personality, and even type of humor (that’s a tricky one). Cynicism is usually an accurate worldview, but watch the availability bias. Ditto for our nurses; it is a team sport.” Some specialists are no doubt comfortable and skilled in handling general medical issues, but it probably relates to how long they’ve been out of residency and how far their specialty is from whole-body medicine (internal medicine is right on it, electrophysiology or diagnostic radiology, maybe not). My point is that doctors are not interchangeable, and our system of training and payment – not to mention the incessant onslaught of new medical knowledge and application — creates specialists whose bedside contributions in a pandemic may be limited. Regardless, you would rather have them than not, and it’s selfless of them to volunteer for dangerous duty that falls outside their chosen practice area.
HIStalk Announcements and Requests
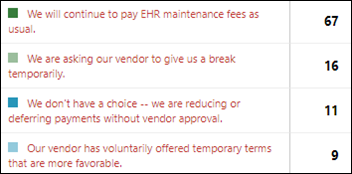
Two-thirds of hospital poll respondents are paying their EHR maintenance fees as usual, although another 25% are either asking their vendor for a break or are reducing or deferring payments by necessity.
New poll to your right or here: which terms would you apply to HIMSS? I can’t include all the possible options, so click the poll’s Comments link after voting and describe which I missed. I’m not looking for shade-throwing here – I’m genuinely interested in how industry people, especially HIMSS members and exhibitors, view their relationship with the organization. I’m happy to share my own views as a member, but perhaps I should save that until after the poll closes.
Webinars
April 28 (Tuesday) 1 ET: “COVID-19: Managing an evolving patient population with health information systems.”Sponsor: Intelligent Medical Objects. Presenters: Julie Glasgow, MD, clinical terminologist, IMO; Reeti Chauhan, senior product manager, IMO. IMO recently released new novel coronavirus descriptors to help clinicians accurately record diagnoses and also created free IMO Precision COVID-19 Sets to help identify and analyze patients with potential or documented infection. The presenters will discuss these new tools and describe how to use them optimally.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
A private equity firm sues Intel for failing to consummate a deal in which the firm intended to buy Intel’s Care Innovations remote patient monitoring subsidiary in early 2017. The complaint says that Intel signed an exclusive agreement to sell the business, but then used the private equity firm’s offer to negotiate a higher price from the eventual buyer, venture fund ISeed Ventures. The Intel-GE Care Innovations joint venture was formed in August 2010.
People

University of Maryland Medical System promotes Joel Klein, MA, MD to SVP/CIO. He had served in the interim role since July 2019.
Announcements and Implementations
Netsmart launches a telehealth solution for behavioral health, home health, hospice, senior living, and social services providers.
A peer-reviewed observational study of data from Glytec’s insulin management software finds that the mortality rate of hospitalized COVID-19 patients was much higher for patients who had a history of diabetes and uncontrolled hyperglycemia, confirming WHO’s determination of diabetes as a comorbidity that affects survival. More surprisingly, the study also found that 42% of patients who had no history of diabetes and who experienced inpatient hyperglycemia died in the hospital, which is seven times the death rate of patients who had neither diabetes nor hyperglycemia. The results are interesting, although not definitive due to the absence of proving causation versus correlation, the inability of the authors to review the longitudinal records of patients, the likely contribution of other comorbidities (how many of the patients who died also had heart disease?), and the limitations of looking only at particular hospitals whose policies, resource availability, and socioeconomic case mix might have skewed the results.
KLAS looks at three vendors of technologies related to social determinants of health in surveying a small number of customers (four to 12 organizations):
- Healthify, which screens patients and creates a referral summary. Clients are seeing benefits, including better communications and identifying patient needs, but EHR integration is a challenge and ROI is hard to determine.
- Aunt Bertha, which allows searching for community resources and tracking referrals. Clients report ROI and are enjoying the community organization relationships the system allows them to build. They would like to see better EHR integration. Clients report the highest satisfaction among the three products and 100% would buy it again.
- NowPow, which supports referrals to community resources. Customers find value in it and 100% would buy it again.
COVID-19
The World Health Organization warns that while COVID-19 serological tests can detect antibody evidence of previous infection, they cannot predict whether a given person is immune to re-infection. WHO says several countries believe they can incorporate presumed immunity from tests into their reopening plans, but nobody knows what the results mean and the rate of false negative results is concerning.

FDA waives limitations on using digital health for treating psychiatric disorders such as obsessive compulsive disorder, anxiety, insomnia, depression, substance use, PTSD, autism, and ADHD, whether new conditions or created by the public health emergency. Developers must have tested their app, apply cybersecurity protection, and require the user to verify that they should contact a doctor before using. The exception, which will remain in place until the public health emergency ends, does not include apps that are intended to treat a specific psychiatric condition, that address conditions that may require urgent intervention, or that replace in-person or telehealth visits.
Kaiser Health News says that hospitals aren’t able to quickly repair broken ventilators or bring mothballed ones back into service because ventilator manufacturers don’t allow hospital biomedical engineers or third party service companies to repair them. Manufacturers make money from controlling who can service their machines, using software locks and internal-only manuals to prevent unauthorized repairs. These limitations have elicited a “right to repair” movement like the ones organized for cars, farm equipment, and cell phones that allow owners to fix their own devices or hire whoever they want to do so. One manufacturer has only two technicians available to service an entire state, which is a bottleneck in the pandemic.
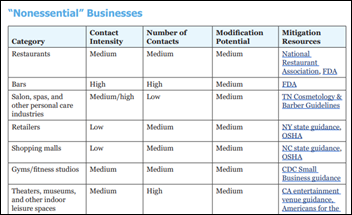
A report from the Johns Hopkins Bloomberg School of Public Health, with former FDA Commissioner Scott Gottlieb, MD as a co-author, lists public health principles for use by governors as they reopen their states. Excerpts:
- The only epidemic control measure that is available in the absence of a vaccine continues to be social distancing combined with case-based interventions. Large-scale distancing measures will need to be reinstated if the epidemic’s growth returns.
- A loosening of distancing measures requires meeting four criteria: (a) a 14-day day decline in new cases; (b) having enough diagnostic tests available to test, at minimum, every person who tests positive and their close contacts; (c) having adequate hospital capacity and personal protective equipment for healthcare workers; and (d) having enough people assigned to perform contract tracing for new cases.
- State leaders must communicate clearly what is being done so that it is not taken as approval for an immediate return to normal activities.
- Prolonged, close contact among people creates the highest risk and must be considered in deciding what to reopen – risky situations include people who travel or share meals together, religious services, family gatherings, cruises, prisons, and long-term care facilities.
- Businesses still need to have people work from home or outside of large groups whenever possible. They should require employees to wear non-medical cloth masks, employ physical barriers where possible, keep people at least six feet apart, and continue paying employees who have been exposed or who are sick at home.
- The risk of reopening schools is uncertain, and tele-education may need to be provided in any case to accommodate high-risk students and those whose parents want to keep them safe at home.
- Risk of transmission in outdoor facilities such as parks, pools, beaches, and playgrounds is lower than indoor settings, especially if people maintain distancing.
- Church services introduce high risk.
- Mass transportation is high risk, but limiting it disproportionately affects under-resourced populations.
- Mass gatherings, such as sporting events and conferences, should follow WHO guidance.
- Re-opening should be separated into phases of 2-3 weeks to allow review of case counts, hospitalizations, and deaths.

Farzad Mostashari, MD gives the epidemiologist’s view of where we are with coronavirus:
- The number of new cases isn’t reliable because nobody is collecting when the patient’s symptoms began versus when the test results became available.
- The high (and increasing) rate of positive tests (at nearly 20% nationally) probably means that only high-risk people are being tested, so we don’t know the extent of the pandemic.
- New York City’s ED trend should be watched closely.
- New York City recorded 9,447 non-COVID deaths in just over one month versus the normal of 5,400.
- Cases are being undercounted based on the ratio of cases to deaths, and deaths are being undercounted as well because it can take up to a month for a patient to die from coronavirus. He thinks new US cases are more likely running 400,000 per day versus the 30,000 that are being reported.

A new NBC News / Wall Street Journal voter poll finds that:
- 60% are worried that the government will lift stay-at-home measures too quickly and cause more deaths.
- 32% worry that the restrictions will remain in place for too long, harming the economy.
- 44% approve of the White House’s handling of the pandemic, while one-third of respondents are satisfied with the federal government’s efforts to provide COVID-19 tests and medical supplies.
- CDC continues to earn a high level of public trust even though its public visibility has been nearly eliminated.
The CDC’s failure to get a COVID-19 test rolled out quickly was caused by poor manufacturing processes that contaminated one of the test’s three components, according to an HHS review. FDA has concluded that CDC violated its own lab standards in failing to isolate the kit-making process. The kits were usable, but CDC took more than a month to remove the spoiled component. The CDC also made mistakes in choosing to include the problematic component at all (since it added little value but delayed rollout) and decided to make the kits themselves in Atlanta instead of using an outside contractor.
Federal authorities arrest California internist Jennings Staley, MD for selling an undercover FBI agent a $4,000 “COVID-19 family treatment pack” that included hydroxychloroquine, azithromycin, anti-anxiety medications, IV drips, and use of a hyperbaric oxygen chamber. The doctor guaranteed the FBI agent that the kit would prevent or cure coronavirus, bragged about smuggling the hydroxychloroquine into the US from China, and sold the agent package upgrades that included Viagra and Xanax. He’s charged with mail fraud. The doctor also operates Skinny Beach Med Spa, which offers medical weight loss, testosterone and growth hormone treatments, laser hair removal, tattoo removal, face rejuvenation, vein removal, Botox, vampire facials, platelet rich plasma therapy injections, hangover IVs, and body sculpting (that’s a lot of external medicine for an internal medicine doctor).

Best tweet of the weekend.
Other

Weird News Andy observes that a leopard was “spotted” (WNA is showing off that he knows that leopards don’t have stripes) in a hospital bathroom in India. It was captured safely and relocated.
Sponsor Updates
- Cerner is collaborating with Fortified Health Security to offer managed security services to healthcare organizations, regardless of their EHR vendor.
- Elsevier launches the COVID-19 Healthcare Hub for free access to toolkits, expert insights, research resources, and COVID-19 guidelines.
- Wolters Kluwer will give AHIMA members access to a custom solution within the MediRegs Compliance Suite that includes content on federal regulatory changes to HIM professionals.
- Meditech releases updated decision support and guidance for coronavirus.
- Clinical Computer Systems, developer of the Obix Perinatal Data System, releases a the latest episode of its Critical Care Obstetrics Podcast, “Maternal Levels of Care.”
- Pivot Point Consulting VP of Advisory Services Laura Kreofsky receives Consulting Magazine’s 2020 Women Leaders in Technology Award.
- Redox releases a new podcast, “Digital Health Startup Advice with Dr. Roxie Mooney.”
- The National Council for Prescription Drug Programs re-elects Surescripts CIO Mark Gingrich to its trustee board, and elects Director of Standards Tim McNeil and Manager of Clinical Informatics Larry King to two NCPDP workgroups.
Blog Posts
- Using Facesheets to Act on Powerful Information (Lightbeam Health Solutions)
- Innovation: The Lasting Legacy of the COVID-19 Crisis (Loyale Healthcare)
- Rural Health Models in the Age of COVID-19 (Meditech)
- Using Improvement Science in Healthcare to Create True Change (Health Catalyst)
- Physical Therapy Work from Home Telehealth – HIPAA Compliance Basics (MWTherapy)
- 4 Ways Location Data Can Help Public Health Experts Fight COVID-19 (NextGate)
- Three Big Trends that Will Impact Pharmacy Communication (Omnisys)
- How health plans can prepare now to close gaps in care when COVID-19 subsides (Experian Health)
- How to Improve Telehealth for COVID-19 (PatientBond)
- Real-time Solutions for Provider Organizations to Increase In-person and Telehealth Appointments Amidst COVID-19 (PatientPing)
- Three Communications Challenges Impacting Collaboration in Healthcare (PatientKeeper)
- New CMS Tools and Guidelines for COVID-19 Now in Effect (QliqSoft)
- What Our Four Core Values Really Mean (SailPoint)
- Stay professionally connected while socially distant (StayWell)
- COVID-19 Pandemic: Prevent the Oncoming Medical Information Crisis (SyTrue)
- COVID-19 clinical pathways available at no charge for 12 months. (Voalte)
- Communication Workflows in Pop-Up Bed Locations: We Can Help (Vocera)
- 4 steps to getting the most out of your analytics (Waystar)
- New Telehealth and COVID-19 Updates for Google My Business (WebPT)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.




RE: SDH referral platforms. The SIREN network (out of UCSF) published its evaluation last year (full disclosure I was a consultant on it):
https://sirenetwork.ucsf.edu/sites/sirenetwork.ucsf.edu/files/wysiwyg/Community-Resource-Referral-Platforms-Guide.pdf (chrome gives a security certificate warning but it is the legitimate pdf)
What’s missing from all these platforms and reports on them is their actual impact on health outcomes.
Dr. Gottlieb, can we simply say that if businesses can maintain social distancing they can reopen tomorrow? That would be huge.
In regards to Consulting Magazine’s 2020 Women’s Leaders Technology Award presented to Laura Kreofsky – Excellent Choice, I worked with Laura way back when at First Consulting Group, and have followed her outstanding rise to Leadership over the years since then. those who lead IT Organizations back then knew she was a rising star. Congrats Laura !
Jim Lachner
Cerner & Epic Analytics Executive