LOL @ Ascension. Who knew that outsourcing your entire IT department wouldn't be the best idea? I can't speak to…
Monday Morning Update 4/6/20
Top News
The FCC publishes details of the $200 million COVID-19 Telehealth Program, for which it will start accepting applications immediately.
The program will fully fund provider purchases of telecommunications, information services, and connected medical devices to provide remote services, with an emphasis on those that help low-income Americans and veterans.
Reader Comments
From Recovering CIO: “Re: provider layoffs. As they start to hit, I wonder how the organizations of readers are looking at funding in the CARE Act as well as the FCC’s $200 million telehealth funding.” I’ve created a submission form for provider readers to tell us.
From Imburse Me First: “Re: hospitals. Do they have incentive to game insurers, Medicare, or the bailout program by claiming patients died of COVID-19 when they don’t know for sure?” I’m guessing hospitals have the theoretical incentive to overstate COVID-19 deaths (I was reading a wacky conspiracy theory about that on Twitter), but I’ll ask experts to weigh in. My question is how deaths are categorized as being caused by COVID-19 – have all those patients tested positively, and was COVID-19 the cause or was it an incidental condition? Shelter-in-place should have reduced deaths from car accidents and injuries, so shifts in the numbers for deaths from heart disease, cancer, stroke, respiratory disease, and diabetes might indicate creative coding, although most of those are also predictors of COVID-19 outcomes. Obviously this is not a good time to suffer from a serious non-COVID condition that requires medical or surgical intervention, and we may see problems down the road as a result.

From Panama Jacques: “Re: your logo. Doctors should not be smoking – what a poor example for a healthcare site.” I’m happy for the recent uptick in readership, but it has sparked yet another round of smug observations from newbies who feel uncommonly blessed with perceptive powers. Your logo doctor smokes a pipe? The Monday Morning Update comes out Sunday? You’re biased for or against (insert any health IT vendor or political party here)? You write about music? Why are the news posts so long when I’m too busy to read it all? I started writing HIStalk four years before the first IPhone came out and haven’t changed it much since 2003. People have either kept reading it or they’ve moved on. Annual reader survey numbers for “reading HIStalk helps me do my job better” are always high (92% this year), so those folks apparently aren’t sweating the doc’s pipe or my periodically professed love for oddball music.
From Was A Community CIO: “Re: HIMSS20. Looks like a cash grab for OnPeak or HIMSS. Hyatt waived penalties for room cancellations due to COVID, but the charge remains on my card and Hyatt says they returned the money to HIMSS. Someone has my company’s money and I don’t think it’s Hyatt.” HIMSS says in the email thread that was attached that Hyatt didn’t send it money. I checked other conferences and it seems that OnPeak uses the credit card to hold the reservation, but it’s the hotel itself that actually charges your card for the initial deposit. In that case, I don’t know why Hyatt would have sent your refund elsewhere, which leads me to suspect they are the problem rather than HIMSS or OnPeak. I would probably dispute the charge with your credit card company since it shows Hyatt as the recipient. That will put the ball in Hyatt’s court.
HIStalk Announcements and Requests
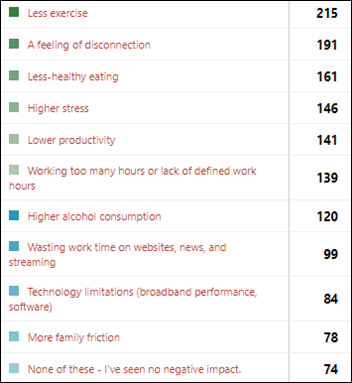
Most poll respondents report experiencing some negative effects in working from home, most commonly related to exercising less, feeling disconnected, or eating unhealthily.
New poll to your right or here: what is your personal experience with COVID-19? Vote and then click the poll’s “Comments” link to tell us more.
Thanks to the following companies that recently supported HIStalk. Click a logo for more information.
Webinars
April 15 (Wednesday) 1 ET: “Scaling front-line COVID-19 response: virtual education, screening, triage, and patient navigation.” Sponsor: Orbita. Presenters: Lawrence “Rusty” Hofman, MD, medical director of digital health, Stanford Health Care; Kristi Ebong, MPH, MBA, SVP of corporate strategy, Orbita. The presenters will describe how chatbots can be quickly deployed to streamline individual navigation to the appropriate resources, administer automated virtual health checks for monitoring and managing specific populations, increase access to screening and triage for high-risk populations across multiple channels (web, voice, SMS, and analog phone), and reach individuals in multiple languages.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Announcements and Implementations
PatientBond offers hospitals its digital engagement services at no cost through June 2020, providing a weekly patient education email campaign related to COVID-19 prevention, detection, and treatment.
COVID-19
The Trump administration is considering paying hospitals at Medicare rates for treating uninsured COVID-19 patients, taking the money out of the $100 billion that was designated for hospital relief. The government proposed such payments as an alternative for opening up the ACA insurance marketplace for the many millions of Americans who have lost their jobs in the past few weeks, but experts question how payment would be assigned when patients may receive treatments for conditions other than COVID-19 in a single hospitalization.
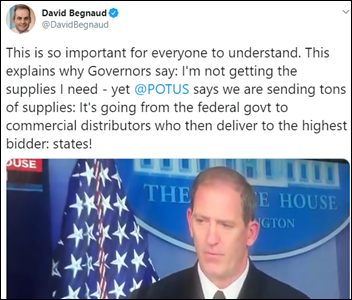
The White House explains that the COVID-19 supplies it is bringing in from China and sending to states are actually going to commercial distributors for resale to the highest bidder, as the federal government does not want to disrupt the supply chain.
New York State virtually merges all of the state’s 200 hospitals into a single state system that will share staff, patients, and supplies under the direction of the state’s department of health. Challenges include how billing will work when a patient is moved to an out-of-network hospital, how staff can be moved to a distant facility without disrupting their families, and determining how hospitals pay each other for the resources they share.


CNBC profiles the New York City “disease hunters,” who after 9/11 set up a syndromic surveillance system using data from hospital EDs. One of those involved was NYC Department of Health Assistant Commissioner Farzad Mostashari, MD (later National Coordinator, now CEO of Aledade), who looked at his old system on March 4 (the day before HIMSS20 was cancelled) and started tweeting about a high volume of patients with flu-like symptoms, when the city had only 100 confirmed COVID-19 cases. As with many public health projects, this one suffered from federal-state clashes, a heavy-handed yet underfunded CDC, and overall public health funding cuts in 2019.

The first and best public health school in the world, Johns Hopkins Bloomberg School of Public Health, lists the “5 Ways the US Botched the Response to COVID-19.”
The Gates Foundation is testing seven coronavirus vaccines and is building manufacturing capacity for each of them to speed up any eventual production, even with the knowledge that one or two of them at most – and possibly none of them – will be found to be effective. He says the parallel process will waste a few billion dollars, but it’s worth it given the trillions of dollars that are being lost economically.
CDC rolls out COVIDView, an outbreak monitoring tool that displays key indicators that will be updated weekly. Sounds like a good idea, other than it’s late in the game and the infrequent updates limit usefulness. I truly don’t understand why the federal government isn’t tapping into the Cerner, Epic, and Meditech EHR databases that cover the vast majority of hospitals and a significant portion of their ambulatory operations, and instead is asking for daily worksheets to be emailed. Maybe epidemiologists just aren’t aware of the trove of real-time electronic data that hospitals are sitting on, or don’t have the right people demanding access to it.
Hospital staffing firms that are owned by private equity firms are cutting the hours and pay of their doctors as COVID-19 has reduced the demand for other services, especially elective procedures. Among them: TeamHealth, SCP Health, US Acute Care Solutions, Envision Healthcare, and Alteon Health. The latter laid off clinicians for 1-6 months and won’t guarantee hours for part-time employees, explaining in an internal email, “Anyone not willing or unable to share the burden will need to be terminated to preserve employment for those who really feel part of our team and care about their co-workers.” An anonymous ED physician who works for Alteon said. “Healthcare workers are being applauded in the streets and we are being stepped on by them.” Meanwhile, the wave of hospital layoffs and furloughs has turned into a tsunami as our screwy healthcare non-system finds itself under attack financially as well as microbiologically.
Other
Maryland-based contractor Cesar Capule, who was working on the Epic go-live at St. Agnes Hospital (WI), fell ill with COVID-19 symptoms during the project, was asked to self-quarantine at a local hotel, and eventually was admitted to the hospital’s ICU, where he was ventilated and died 17 days later on March 29. He was 49. I could find no further information about him.
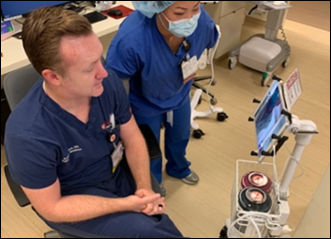
A Palo Alto news site describes how Stanford Health Care is using telemedicine to screen patients who are worried they have COVID-19, saving the health system PPE and potential provider exposure in having ED doctors do video screening of people in the drive-through testing location. Stanford is now doing 40% of visits virtually, 50 times its pre-pandemic volume.

New Jersey’s governor calls for volunteer COBOL programmers (which he calls “cobalt”) to maintain the 40-year-old state systems that issues unemployment checks.
The New York Times profiles people who have moved to the US from other countries, but are going back because of our lack of universal healthcare, ineffective COVID-19 response, and overwhelmed hospitals in which even insured patients may not be adequately treated. Some had bought travel insurance as their primary healthcare coverage because US insurance is so bad.
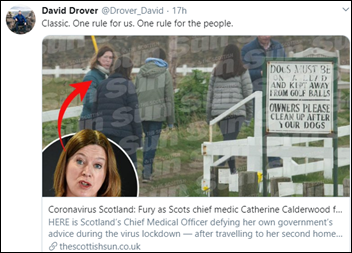
The chief medical officer of Scotland, who appears in TV public service announcements in which she urges people to stay home, is formally warned by police after being captured in a photo walking her dog outside her second home that is 45 miles from Edinburgh. Residents of that town are annoyed at visitors who are traveling to their second homes and walking outside, some of them relocating from cities to self-isolate in their vacation homes where goods and medical services are scarce. Others note that while she is being vilified, Prince Charles – who has tested positive for coronavirus – moved freely from London to Balmoral. It is indeed good to be (future) king.
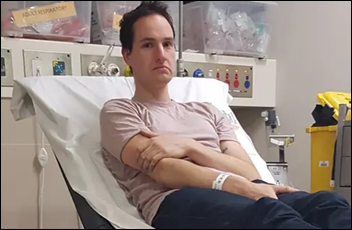
@drnic1 found this fun story. A bored, working-from-home astrophysicist in Australia is inspired by coronavirus to invent a necklace that sets off an alarm when the wearer touches their face. Not only did he inadvertently invent the opposite (the necklace alarms constantly until it detects a hand approaching the face), he also had to visit the ED to have the sensing magnets removed from his nose. His partner took him to the hospital where she works because “she wanted all of her colleagues to laugh at me.”
Sponsor Updates
- Spok offers a video tribute to healthcare workers who are on the front lines of COVID-19, including a wall of thanks from employees.
- Meditech extends its virtual visits offer to all customers for a six-month period.
- Wolters Kluwer Health releases a new educational video, “Understanding COVID-19 and How to Stay Safe.”
- The Chartis Group publishes an IS checklist for COVID-19.
- Wolters Kluwer Health adds COVID-19 tools to Sentri7 (infection prevention rules and population of Notifiable Conditions for COVID-related lab tests and results) and Health Language Clinical Interface Technology (access to COVID-updated SNOMED CT and ICD-10 codes).
- PerfectServe offers free software and services for Patient & Family Communication and free services to implement best practices for COVID-19 purposes.
- Relatient offers a free download, “Using Patient Engagement Solutions to Communicate with Patients during the COVID-19 Pandemic.”
Blog Posts
- Navigating Uncertainty: CMS Signals that Value-Based Care is Here to Stay (Lightbeam Health Solutions)
- The COVID-19 Financial Crisis: 6 Steps Hospitals Can Take Now to Help Their Patients and Themselves (Loyale Healthcare)
- Health IT crisis and disaster planning recommendations for COVID-19 (Meditech)
- COVID-19 Healthcare Cybersecurity: Best Practices for a Remote Workforce (Health Catalyst)
- As of 3/30/20, Medicare Has Still NOT Added PT, OT, or SLP as Telehealth Providers (MWTherapy)
- Long-Term Advocacy Effort Pays Off with Patient-Centered Changes to 42 CFR Part 2 Privacy Regulations (Netsmart)
- How Can OmniSys Help Your Pharmacy Support COVID-19? (OmniSys)
- COVID-19: The Implications for Industries (OpenText)
- Could the coronavirus make patient portals access point No. 1? (Experian Health)
- What Consumer Search Behavior is Telling Us About Coronavirus & Implications for Access to Care (Kyruus)
- 5 Benefits Provider Organizations, Health Plans, and ACOs are Seeing with PatientPing’s COVID-19 Flag (PatientPing)
- A Tool for Our Times (PatientKeeper)
- Pivot Point Perspective: New COVID-19 codes to improve data capture for tracking and payment (Pivot Point Consulting)
- 5 Ways to Boost Urgent Care Clinic Morale During Uncertain Times (Experity)
- Fool’s Gold and the Future of AI (Waystar)
- Videos from our Healthcare IT Interoperability Virtual Conference (Redox)
- Our Customers Have Our Hearts (SailPoint)
- Addressing COVID-19: Santa Rosa Offers Support (Santa Rosa Consulting)
- Prevent social distancing from becoming social isolation (StayWell)
- Managing change on a burning platform (Nordic)
- How to Convert Non-HL7 Files to HL7 Messages (Summit Healthcare)
- COVID-19 Influx: Using SymphonyRM’s HealthOS to Manage Through a Pandemic (SymphonyRM)
- Keep in Touch: 3 Technologies That Connect Rehab Therapists and Patients from a Distance (WebPT)
- Learning from COVID-19: Urgent Call for Innovation (Capsule)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.
























It’s amazing that such a wonderful idea and collaboration (New York hospitals pooling together and sharing resources to fight a once in a lifetime emergency) could all be undone by the terrible “in network vs. out of network” debacle that we’ve allowed the for profit healthcare machine in America to create. Why not pass a law mandating that all out of network care is simply paid at medicare like rates? Are there any downsides that I’m not thinking about here?
From Imburse Me First: “Re: hospitals. Do they have incentive to game insurers, Medicare, or the bailout program by claiming patients died of COVID-19 when they don’t know for sure?”
In our county, a single for profit health system owns the hospital and all urgent cares in the county. Last week, my wife had all of the symptoms of Covid, and she began to decline. I took her to the ED, and the note said that she was suspected of having Covid19. The interesting part is they didn’t test her for Covid. Their protocol was not to test anybody for Covid unless a positive test would change the treatment course.
So instead of a single test, the did a CXR, metabolic panel and a chem 7. So the medicare reimbursement rate for a CDC covid test is around $35.91, while my wife’s visit rang up $4000.00.
From a revenue perspective, it seems far more lucrative to not test for Covid 19.
In general isn’t it good medicine to skip tests that won’t change the treatment course? Wouldn’t they likely have run all of those other tests anyway if your wife was getting worse and was going to need treatment?
I have no doubt that there are people out there trying to game the system to maximize reimbursement, but without any other details, this sort of seems like good practice – don’t run the test is the results aren’t going to mean anything.
Sorry to hear about Cesar Capule in WI. I’ve worked with many of these traveling Epic “ATE” support folks during implementations and upgrades. They are a silent army that allows the hospital to keep running during an intense time with new system. They work the shifts that FT staff don’t want, offer expertise to hospital staff new to the systems, are friendly and patient with frustrated clinicians. I can’t imagine being ill and dying so far from home and family, and hope for peace for his loved ones.
I think you are correct that Hyatt is the problem, not OnPeak or HIMSS. We booked rooms at 2 hotels for HIMSS. I noticed this week that the Rosen Shingle Creek refunded our credit card for the room charges. Hyatt has not. I guess I will be calling the credit card company to dispute the Hyatt room charges…