I believe it is this: https://www.investopedia.com/terms/w/warrant.asp So an option, but one provided by the original company.
News 2/28/20
Top News

HIMSS provides a coronavirus update for HIMSS20:
- The conference will proceed as scheduled March 9-13.
- CDC has deemed the coronavirus health risk for the general public as low.
- The conference will be a handshake-free meeting, with appropriate education and reminders. In a breaking news development, HIMSS recommends the “HIMSS elbow tap” instead of handshakes, apparently deciding that the Ebola fist bump was due for an upgrade.
- HIMSS is allowing registrants from Level 3 alert countries (China and South Korea) to cancel. Orlando International Airport will not allow foreign nationals who have traveled to China 14 days before their US arrival into the country, per President Trump’s February 3 proclamation.
- The cancellation rate is at 0.6%.
- CDC-established screening will be conducted on site, although details of what than entails weren’t provided. Attendees whose screening suggests risk will be immediately isolated.
- The conference will have health professionals on site and hospitals available.
- Hand sanitation stations and wipe-down disinfection wipes will be provided.
- Information booths will provide medical-grade face masks to anyone who wants them.
- Facilities will be disinfected throughout the conference.
Reader Comments

From Takeoff U. Hoser: “Re: UCSF Health. Has sent a letter to HHS supporting the proposed interoperability rule. The same organization provides de-identified patient data to Google for AI training of potentially highly profitable technologies, as was made public this week. That’s an interesting coincidence.”
From Hirepower: “Re: Allscripts. Online rumors say this is Day 2 of three days of layoffs. Any info?” I’ve seen nothing firm, although those unverified rumors say a few folks were let go from TouchWorks and Veradigm. The quarterly earnings report comes out Monday.
From Dollar Bill: “Re: COVID-19. What impact will it have on health systems?” I’m interested in hearing the financial impact that health systems expect. Most people who think they have (a) a life-threatening attack of COVID-19; and (b) insurance that covers their ED visit at minimal personal cost actually have; (c) neither. I think the biggest impact will be on people with insurance who will be left with crippling out-of-pocket costs for deductibles, co-pays, co-insurance, out-of-network costs, etc. It’s early in the insurance year to be running up a big ED tab when your deductible is thousands of dollars. The US healthcare system is rarely your friend, but is definitely your enemy when your expectations of invincibility are expensively dashed. I expect all the usual healthcare profiteers – including health systems – to make pandemic profits. China’s telemedicine companies are enjoying a stock boom from recent coronavirus-fueled usage growth, so there’s that.

From YouBoob: “Re: ZDogg MD’s Epic criticism. He talks over the CBS news profile.” ZDogg’s music parodies were pretty good back in the day when his Turntable Health clinic hadn’t yet failed and forced him to transition into an Internet celebrity selling “sponsorship, speaking, influencer, and video production packages.” He wields the scalpel of dripping sarcasm clumsily in this anti-EHR video in which he attempts impish cleverness in insulting Epic, its competitors, health systems, doctors, patients, and CBS. I couldn’t stand watching it all, but his main points seem to be:
- Judy’s $3.6 billion fortune came from patients and health systems that bought Epic at a high cost, “whereas you can pick up an IPhone and pretty much do anything you want, anywhere.” The IPhone reference is just plain stupid (and last time I checked, the folks who sell those do pretty well financially, too) but the question might be what health systems should have implemented if it wasn’t Epic, Cerner, or Meditech (he complains about all three).
- He scoffs at Judy Faulkner’s statement that Epic has to compete for technical talent against YouTube, Google, and Facebook in hiring developers for its “1990s era software” and built a great campus in the cow fields of Verona, WI to help do that. Every self-appointed expert thinks that anything written before Facebook must be useless by definition, but can never explain why the underlying technology matters one iota to anyone except a programmer who sees the actual source code.
- “They haven’t made it usable. The client is not a doctor, the client is a health system.” I’m not sure what point he was making here, unless it’s that his peers should stop accepting paychecks from health systems that insist that they use software that meets their business needs.
- “The only way you can share data from an Epic chart, your data – you’re the patient, you own this data – the only way is if you go to another health system that has Epic.” I’ve never tried this as a patient, but I would be seriously shocked if Epic data has never been shared with a hospital or practice that uses a different EHR.
- He said this: “If Athenahealth or Modernizing Medicine, both of whom I’ve worked with, or Office Practicum, who I’ve worked with, I’ve done talks for, if they were the largest electronic health vendors in this country, I’d be picking on them too.” I interpret this as meaning that ZDogg cashed promotional checks from other EHR vendors without complaint and they get a free ride because they aren’t as successful as Epic.
- He also said this: “When we were running Turntable Health, we had our own EHR that we built from scratch with our partners Iora, and patients had access to it, it was problem based, you could have a health coach and a doctor writing in it at the same time, there wasn’t a billing component to it, t was pure patient care. And it wasn’t perfect but it just worked. That’s what we need.” That would be a great supporting argument if (a) Turntable was more than a small primary care practice that didn’t accept insurance; and (b) it hadn’t gone belly up after three years. I share his admiration for Iora Health and the tools that work for them, but to compare their needs with those of health systems is unrealistic. Epic, Cerner, and Meditech have dozens to hundreds of specialty modules that support lab, anesthesia, labor and delivery, surgery, ED, oncology, etc. so any design must accommodate all of those services, not just ambulatory primary care visits.
- ZDogg is right that EHRs weren’t designed to bring joy to doctors and that the CBS profile is a silly fluff piece (although it was just filler aimed at people sitting around on Sunday mornings watching network TV, to be fair). He’s wrong in forgetting that the job is the problem, not the tools that are required to support it. Doctors sold their independence and thus their right to have software designed to meet only their needs, while health systems are like any other business in being free to buy whatever IT systems they think are best for their organizations and patients.
HIStalk Announcements and Requests
Snap poll for HIMSS20 registrants: how will coronavirus concerns change your attendance plans? I included a fake vote option so curious folks can see the poll’s results without having to make a misleading choice. Add a comment after voting if you like.

I’m always puzzled by HIMSS’s “Conference Deal” emails, which I think they rolled out years ago when Groupon was still a big thing. What’s the “deal” in being invited to see a booth demo?
Webinars
March 4 (Wednesday) 1 ET: “Tools for Success: How to Increase Clinician Satisfaction with HIT Solutions.” Sponsor: Intelligent Medical Objects. Presenter: Andrew Kanter, MD, MPH, FACMI, FAMIA, chief medical officer, IMO. Dr. Kanter will explore how striving to achieve the Quadruple Aim (by focusing on the provider experience) can improve clinician satisfaction and population health needs while also reducing per capita healthcare costs. Attendees will learn how to set providers up for success with new technology, the potential unforeseen consequences of purchasing without the clinician in mind, and the factors that are critically important to clinicians who are using new health information systems.
March 4 (Wednesday) 1 ET: “Healthcare Digital Marketing: Jump-Start Patient Discovery and Conversion.” Sponsor: Orbita. Presenters: Victoria Petrock, MBA, MLIS, principal analyst, EMarketer; Kristi Ebong, MBA, MPH, SVP of corporate strategy, Orbita. Does your digital front door capture consumers who search for health-related information one billion times each day? Do you have actionable steps to convert them into patients? Do you understand voice and chat virtual assistants? The presenters will explore the consumer challenges involved with finding, navigating, and receiving care, discuss why healthcare marketers need to embrace conversational voice and chatbot technologies, and describe how new technologies such as conversational micro-robots can improve engagement.
Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
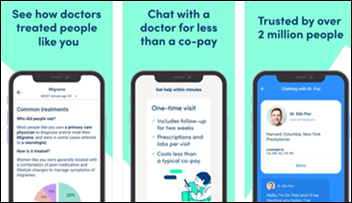
K Health, which offers consumers an AI-powered review of their symptoms and then paid telehealth visits, raises $48 million in a Series C funding round. The system, which was trained on patient data from an Israel health fund that is one of its investors, is rolling out a co-branded version for Anthem so that patients can “text with a doctor for less than a co-pay” at $19 for a single visit or $39 for unlimited chats for a year. The company says it has served 3 million users and is now available in all 50 states.

Spok reports Q4 results: revenue down 9%, EPS –$0.50 vs. $0.01.
Sales
- Northside Hospital (GA) will implement sepsis-monitoring software from Ambient Clinical Analytics.
People

Fax and documentation automation vendor Concord Technologies hires Christopher Larkin, MS (Elsevier) as CTO.
Announcements and Implementations
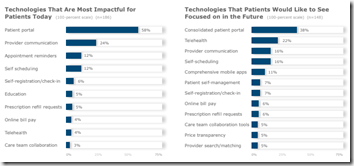
KLAS surveys 300 people about the patient engagement technologies they use and the changes they would like to see. Patients who see their provider relationship as collaborative value patient portals and technologies that allow them to stay connected without a face-to-face visit, while patients who are more transactional are happier with online bill pay, automated prescription refill requests, provider search, self-scheduling, and eventually price transparency tools. The patient portal is most impactful today because Meaningful Use money got them deployed, but patient adoption is limited and patients would prefer a consolidated version that includes all of their providers and all common functions related to lab results, billing, appointments, and secure messaging. Their second-most desired technology is telehealth. Most interesting to me is that money has driven the process – providers rolled out the minimum patient portal that earned them MU money for “having” rather than “using,” they aren’t about to share information with competitors, and they haven’t shown much interest in making themselves available outside of face-to-face visits because nobody pays them otherwise. They also don’t offer telehealth, leaving patients to use standalone services with doctors they don’t know, which is one possible reason for low usage.
The Providence healthcare system opens an innovation center in Hyderabad, India.
Government and Politics

The inspectors general at the DoD and VA announce that they will begin conducting a joint audit of efforts by the departments to roll out an interoperable EHR from Cerner. Government officials insist the audit isn’t the result of complaints, but rather an effort to ensure that the EHR modernization will enable interoperability among the departments and private sector providers.
The VA gives a new planned Cerner go-live date of July 2020, although Secretary Robert Wilkie would not commit to a specific date to a House VA committee. Programming has been completed for just 19 of the 73 required interfaces.
Other
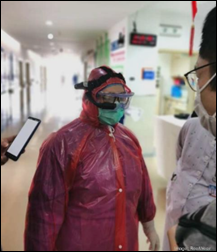
In Canada, Vancouver-based RealWear partners with Chinese technology company Tencent to adapt its headsets for medical use, giving healthcare workers on the frontlines of the COVID-19 outbreak in China access to hands-free, voice-activated software that offers remote viewing and connects to Tencent’s WeChat app.

MIT Technology Review announces its 10 breakthrough technologies for 2020.

Georgia’s lieutenant governor says it’s not improper that he talked about selling a health IT application to health and wellness platform vendor Sharecare, which is paid $14 million per year to run a digital health program for state employees. The talks didn’t pan out. Geoff Duncan is a former CEO of employee wellness technology vendor Wellview Health and remains a company director.
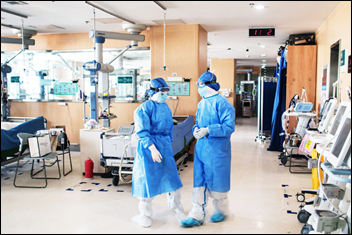
Wired looks at the ways Chinese radiologists are relying on AI from Infervision to screen for COVID-19 symptoms, especially pneumonia. Software originally developed to detect cancerous nodules in lung scans has been repurposed by hospitals that are overwhelmed with patients.
Sponsor Updates
- Elsevier will use Global Medical Device Nomenclature data to provide important clinical and vigilance information on medical devices.
- EClinicalWorks will exhibit at the AAPM Annual Meeting through March 1 in National Harbor, MD.
- Redox partners with Welldoc, giving providers the ability to view data from users of Welldoc’s BlueStar diabetes management app from within their EHR workflows.
- The Chartis Group names David Howard (Grant Thornton) director and practice leader for its ERP and Technology Innovation practices.
- Hayes Management Consulting will work with search and AI-powered analytics vendor ThoughtSpot to develop revenue cycle and compliance solutions for providers.
- Wolters Kluwer Health Language publishes a new executive brief, “Unlock Your Data: Prepare Your Organization for the New Era of Transparency.”
- Healthcare Growth Partners advises Symplr in its acquisition of The Patient Safety Company.
- Healthwise will exhibit at the HealthTrio User Group Summit March 2-4 in Tucson.
- Hyland completes its acquisition of Streamline Health’s enterprise content management business.
- Imprivata further expands identity and access management capabilities for the UK healthcare market with the launch of its new Identity Governance solution.
- VentureFizz features a “CxO Briefing” with Kyruus CEO and co-founder Graham Gardner, MD.
Blog Posts
- The Importance of Optimizing One’s Supply Chain Management (SCM) (Engage)
- The Challenges of Growth: Where to Begin? (EClinicalWorks)
- Goliath Technologies Makes Troubleshooting the End-User Experience Faster and Easier with Latest Release (Goliath Technologies)
- Nordic teammates discuss diversity, inclusion, and equity in healthcare (Nordic)
- What’s New in the Federal Health IT Strategic Plan? (Clinical Architecture)
- Benefits of Artificial Intelligence and Machine Learning in Healthcare (Optimum Healthcare IT)
- What Makes a Good Provider Champion? (Healthfinch)
- Nordic teammates discuss diversity, inclusion, and equity in healthcare (Nordic)
- Leading change to EMRAM Stage 7: Northeast Georgia Health System (Hyland)
- Natural Language Processing (NLP) Driving SDOH Adoption (Imat Solutions)
- Best Practices for EHR Implementation Training (Impact Advisors)
- Changing the Payer – Provider Relationship (InterSystems)
- Letting clinicians “speak clinician” (Intelligent Medical Objects)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates.
Send news or rumors.
Contact us.




From Takeoff U. Hoser: “Re: UCSF Health. Has sent a letter to HHS supporting the proposed interoperability rule. The same organization provides de-identified patient data to Google for AI training of potentially highly profitable technologies, as was made public this week. That’s an interesting coincidence.”
Failing to see how that’s interesting. Interop rules have very little to do with this exchange paradigm. If UCSF bought an AI tool from a startup and was using it, this wouldn’t be news. Only news is that it’s Google.
Both seem to be jerk this year.
Why doesn’t he stay in the business and create a revolution with something actually better?
He’s probably making more money from people who seek to profit from tearing down decent people at Epic who are just trying to make the world a better place.
He uses the Stockholm Syndrome first put forward by his Harvard buddies.
What a sad future with dopes like this as paid influencers and speakers at conferences.
Wonder how long till the people who pay a fortune to go to HIMSS and exhibit lay down the law when HIMSS brings jerks like him to keynote.
Coffee Talk:
ZDogg MD is neither a real dog, nor a real MD. Discuss amongst yourselves…
ZDoggie seems to think hightly of some other 80s tech though…
macOS is the second major series of Macintosh operating systems. The first is colloquially called the classic Mac OS, introduced in 1984, the final release of which was Mac OS 9 in 1999.
Ahhh…. the good old days.
“Because they are the BIGGEST”
Yeah, ZDogg, I like grinding axes as mush as the next guy, but Cerner is in the ballpark of 2x the size of Epic. Also fairly sure Athena and Epic interoperability plumbing is close to 100% via carequality. At least give those who are doing something credit for doing something.
I’m pleasantly surprised to see somebody mention Carequality, as I’m used to folks looking the other way and pretending that national interoperability doesn’t exist today. I share your understanding that the majority of Athena and Epic sites are live on it, with a sizable representation for eCW too (though I’ve heard data quality from eCW leaves much to be desired).
Wish that Carequality’s public listing of live health systems also listed vendor allegiance, but happy that the tool is on their website anyway (https://carequality.org/active-sites-search/).
HIMSS is allowing registrants from Level 3 alert countries (China and South Korea) to cancel. NICE OF THEM!
Orlando International Airport will not allow foreign nationals who have traveled to China 14 days before their US arrival into the country, per President Trump’s February 3 proclamation. HOW WILL THIS ACTUALLY BE ENFORCED?
Anyone entering and exiting China would have the appropriate stamps in their passport. The travel restrictions wouldn’t be too hard to enforce…
Re: OIG Oversight for Cerner/DoD/VA Interoperability: They’re kidding right? The DoD isn’t hooked up to CommonWell, so no, they don’t connect to community providers. And, the VA isn’t live, so no, they don’t connect to anyone. Save the trip and just send an email to verify the current state.
Please comment if I’m missing something. Are they going to roll out a cart with the Joint Legacy Viewer (JLV) to demonstrate Cerner’s patented 2-workstation interoperability workflow?