RE the AI GLP1 company, Washington Post has an article today by someone who used one of those compounded products,…
Monday Morning Update 11/18/19
Top News
HHS, as promised, expands its previous plan to require hospitals to publicly post all of their payer-negotiated charges by also requiring insurers to do the same.
Hospitals would also be required to post the cash payment they are willing to accept for 300 common, shoppable services.
The rule will take effect on January 1, 2021 in the imaginary world where no lawyers live (the American Hospital Association, Association of American Medical Colleges. Children’s Hospital Association, and Federation of American Hospitals immediately said they’re suing for HHS overstepping its bounds).
President Trump said in announcing his executive order:
First, we are finalizing a rule that will compel hospitals to publish prices publicly online for everyone to see and to compare. So you’re able to go online and compare all of the hospitals and the doctors and the prices, and, I assume, get résumés on doctors and see who you like. And the good doctors — like, I assume these two guys are fantastic doctors, otherwise you wouldn’t be here. (Laughter.) And the bad doctors, I guess they have to go and hide someplace. I don’t know. Maybe they don’t do so well, I don’t know. But if they’re not good, we — we are more interested in the good ones. It’s called rewarding talent.
Second, we’re putting forward a proposed rule to require health insurance providers to disclose their pricing information to consumers. We’re giving American families control of their healthcare decisions. And the freedom to choose that care is right before them on the Internet and elsewhere, but on the Internet. Very, very open. Very transparent. That’s why it’s called transparency.
Reader Comments

From Who Diss?: “Re: Who’s Who. This CIO was recognized as a ‘Top Medical Professional’ by a seedy-looking organization’s press release.” A variety of “who’s who” scammers contact people cold, preying on their vanity by advising them that they have been “chosen” by their admiring peers or the company’s editor to be included as a member in a paid online listing. After that, they are hit with the upsell to buy lifetime memberships or vanity crap like wall plaques and hardcopy books. You CIOs, pharmacists, doctors, and nurses who I see listed on this particular one’s site got taken, I’m sorry to tell you. Please don’t list this laughable accomplishment on your resume, which in some LinkedIn examples shares space with bogus educational credentials. Above is the company’s luxurious office suite in Valley Stream, NY, conveniently located above the dumpster in which visitors can pitch their “award” and possibly their careers right out the window.

From Gobsmacked Compliance Professional: “Re: SCL Health and Providence. I was having dinner adjacent to a restaurant’s ‘private’ dining room and was gobsmacked to overhear a detailed discussion about their plan to merge, including proposed timeline, financials, etc. Annual reports are due in December and will be interesting reading.” Unverified. SCL owns eight hospitals in Colorado, Kansas, and Montana that generate $2.5 billion in annual revenue. Providence operates 51 hospitals with annual revenue in the $23 billion range. Maybe this alleged privacy slip is yet another example of hospital people loudly saying things they shouldn’t within earshot of others.
From Register Ringing: “Re: HIMSS20. Look at this page of well over 1,000 things they’re trying to sell to exhibitors.” Vendors can whip out their checkbook to buy nearly every square inch of the convention center or to have HIMSS push their sales message to attendees, including:
- Sponsor pre- or post-conference supplements to “own the conversation” ($20,000).
- Pay HIMSSTV to record a panel discussion in their booth ($20,000).
- Get the impartial, hard-hitting journalists at Healthcare IT News to tweet out links to “one of your thought leadership content pieces” ($20,000, or $22,500 if you want them to just write the piece themselves).
HIStalk Announcements and Requests
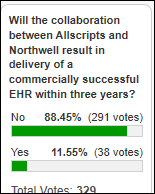
Few poll respondents think the Allscripts-Northwell collaboration will result in a commercially successful EHR any time soon.
New poll to your right or here: How would you characterize Ascension’s data analysis agreement with Google? Click the poll’s Comments link after voting to explain.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre to present your own.
Acquisitions, Funding, Business, and Stock
Brighton Park Capital acquires a majority stake in patient engagement platform vendor Relatient and appoints former Siemens USA President Eric Spiegel as the company’s board chair.
Sales
- Amedisys will deploy NVoq’s cloud-based speech recognition solutions for dictation and automation.
- Thomas Health (WV) will add Meditech’s web-based Ambulatory solution to its Expanse system, implemented by CereCore.
- San Gorgonio Memorial Hospital chooses the Azure-hosted Sunrise Community Care from Allscripts. Googling suggests that they are replacing Allscripts Paragon.
- Beebe Healthcare (DE) will improve workflow efficiency and clinician communication using TransformativeMed’s EHR-embedded work management and notification modules to eliminate printed patient lists.
People

CereCore hires Joe Wurzer (Leidos Health) as RVP of sales and business development.
Privacy and Security
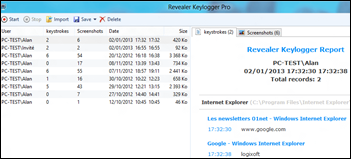
The FBI arrests a former IT employee of an unnamed New York City hospital, charging him with installing a keylogger program on dozens of employee PCs to capture their email login credentials so he could steal their photos and tax records. I was thinking that this sort of information shouldn’t have been stored on a work PC in the first place, but then realized that he probably grabbed their logins to Gmail or other web-based personal email services.
Other
The Washington Post covers “rural America’s busiest emergency room,” Avera Health’s telemedicine center in South Dakota that provides remote ED service for 15,000 emergencies each year covering 179 hospitals in 30 states “where the choice is increasingly to have a doctor on screen or no doctor at all.” Rural ED visits have increased 60% in the past 10 years, but hospitals are closing, doctors aren’t willing to move to small towns, and standalone EDs are going broke. One small hospital signed up at a cost of $70,000 per year after it received four critical automobile accident victims with just an single RN working, with no doctors available within an hour’s drive. Fun fact – the virtual service’s doctors wear scrubs and lab coats to their suburban office park location so they will look like real doctors to their TV patients. The virtual ED clinicians must work patiently with local nurses who may have no experience with intubating patients or who need help running a code blue. Avera ECare’s telemedicine network also offers services for ICU, school health, pharmacy, clinics, behavioral health, correctional health, and hospitalist coverage.

The Pittsfield, MA paper covers the $35 million implementation of Meditech Expanse by Berkshire Health Systems. The article focuses on the hospital’s problems with the Allscripts FollowMyHealth patient portal – the inability to share data, uncertainty over how the company might use its data for marketing, low usage in the 30-40% range, and patients who either can’t sign on to FollowMyHealth or who sign up directly with the service instead of through the hospital-provided link. The health system is a longstanding Meditech customer for inpatient and is apparently replacing Allscripts ambulatory with Meditech.

The Wall Street Journal profiles the technology underpinnings of the new $2.1 billion, 368-bed Stanford Hospital that opened this weekend. It was originally scheduled to be open in early 2018, but was delayed because Apple’s spaceship headquarters project sucked up all the Silicon Valley steelworkers. I was curious about Stanford’s financials, which show $4 billion in annual revenue, a profit of nearly $450 million, several executives in the $1-2 million range, and not-unreasonable IT compensation (the CMIO was paid $770K, while the CIO made $500K). Hospital features include:
- Bedside keypads that allow patients to choose entertainment and control temperature, lighting, and window blinds.
- Swisslog robotic dispensing for pharmacy and medication delivery by robots.
- A fleet of automated guided vehicles for delivering laundry and collecting trash.
- Tracking of staff an inventory in real time.
- Remote patient monitoring.
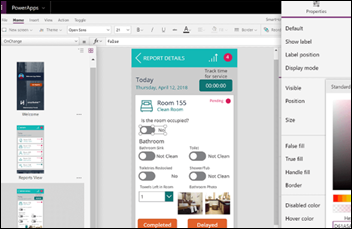
CIOs are expanding their use of “low-code” drag-and-drop automation tools such as Microsoft PowerApps to quickly create applications that automate business processes, which Gartner says will make up 65% of application development in the next five years. St. Luke’s University Health Network (PA) VP/CIO Chad Brisendine says his team has built 20 applications – none of which took more than 20 hours to create – to extract information from hospital systems. A non-programmer needed just eight hours to develop an app that extracts information from its Workday HR system to issue CME reminders to doctors. A Microsoft case study describes how Northwell Health used Dynamics 365 (and its Healthcare Accelerator) and PowerApps to develop a daily rounding app. I admit that the geek in me is aroused.
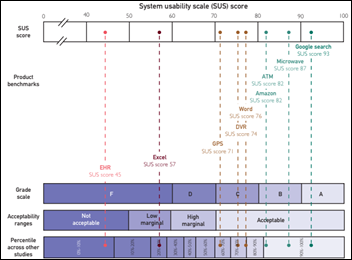
Several readers forwarded the full text of a just-published article that tried to correlate physician-perceived EHR usability with burnout, with the big conclusion being that EHRs “received a grade of F by physician users.” My critique:
- The sample size was just 870 doctors surveyed out of 31,456 invited, of which the authors used “a deliberate oversampling of non-primary care specialties.”
- Perceived EHR usability was compared to “everyday items” such as Microsoft Excel (which also earned an F), an ATM, and a microwave oven.
- I’m not clear on how the authors expected respondents to answer usability questions about “my EHR,” which would depend on their practice (one or more clinics, one or more hospitals, both, etc.)
- The authors mentioned an “incentivized secondary survey,” which suggests that they paid people to complete it.
- They note that respondents may have been conflating EHR usability with the burden of documentation it supports, with their pushback being against documentation requirements rather than the tool that captures it.
- A reader says that while one of the authors is an executive of the notoriously EHR-hating AMA, its own JAMA wouldn’t publishing the findings and it ended up in Mayo Clinic Proceedings, probably because of the low response rate.
Sponsor Updates

- OmniSys employees in Greenville, TX collect hundreds of canned goods for those in need.
- The Wharton School’s “Work of Tomorrow” podcast features MDLive CEO Rich Berner.
- The Salt Lake Tribune features Health Catalyst CEO Dan Burton.
- OpenText and Redox will exhibit at Salesforce’s Dreamforce November 19-22 in San Francisco.
- Clinical Computer Systems, developer of the Obix Perinatal Data System, will exhibit at the Perinatal-Neonatal Symposium November 18 in Williamsburg, VA.
- KLAS Research recognizes PatientPing as a high-performing, emerging healthcare IT company.
- Surescripts and TriNetX will exhibit at AMIA’s annual symposium November 17-19 in Washington, DC.
- SymphonyRM publishes a new white paper, “AI Next Best Actions vs. Traditional CRM.”
- T-System adds EvidenceCare’s clinical decision support tool to its emergency department documentation software.
Blog Posts
- OIG Series 6: Addressing Behavioral Needs and Social Determinants of Health (Lightbeam Health Solutions)
- Where’s My Pizza? A Winning New Vision for Transparency in Healthcare (Loyale Healthcare)
- How EHRs can help address patient safety concerns (Meditech)
- APIs, Alerting and Power Users Shine at MHUG 2019 (Mobile Heartbeat)
- Elevating the Role of the Nurse to Support Value-Based Care (PerfectServe)
- 3 Considerations for Choosing a Public Cloud Partner in Healthcare (NextGate)
- Why Hospice Care Matters to Me: April’s Story (Netsmart)
- Health IT leaders answer: What makes a successful Community Connect program? (Nordic)
- 4 real-world examples of how consumer data can transform the patient experience (Experian Health)
- 4 Ways to Engage Baby Boomers Using Healthcare Technology (PatientBond)
- It’s No Secret: The Healthcare Industry Can Improve Lives with Transparent Pricing (Patientco)
- CHIME 2019 Fall CIO Forum: Key Themes and Hot Topics (Pivot Point Consulting)
- 5 big questions still to be answered by the final ONC and CMS healthcare interoperability rules (Redox)
- Balancing Zero Trust with a strong identity strategy and AI (SailPoint)
- Realize Your Potential ROI with an RPA (Robotic Process Automation) Solution (Summit Healthcare)
- Welcome to VUE19 … and the Future of Care Communications! (Voalte)
- Healthcare Safety: The Big Picture (Vocera)
- 5 Strategies for Training Your Clinic Staff on Compliance (WebPT)
- The new healthcare consumer engagement landscape for whole-person health management (ZeOmega)
- How Better Patient Engagement Reduces Avoidable Readmissions (Zynx Health)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates. Send news or rumors.
Contact us.




Important to note the proposed penalty for hospitals failing to publish pricing is THREE HUNDRED DOLLARS PER DAY.
A total joke.
Seeing that the fine for not being transparent with data is $300 per day, or $109,500 per year. I suspect most organizations will just eat the cost instead of paying for the additional labor that would be required to be in compliance. Or, just look for a way to increase productivity through say, an extra 10 or so MRIs per year.
Or, just raise prices the tiny amount required to cover that $109,500 per year.
“…he probably grabbed their logins to Gmail or other…”
A good reminder for people to turn on two factor authentication for Gmail and other services. If your main email provider doesn’t supply 2FA consider switching to one that does. Also, if possible stay away from using SMS as the second factor. It’s better than nothing, but better to use an app like Google Authenticator since a malicious actor can take over your phone number and thus intercept your SMS. Not to sound like a shill for Google, but Google Voice number is also more difficult to take over. Turn on PIN authentication from your phone provider if they allow for it. I don’t know why the various phone carriers haven’t fixed the phone hijacking issue yet.