I was born roughly 2 months after the US space program began (Explorer 1), and I've followed it all my…
News 11/7/18
Top News
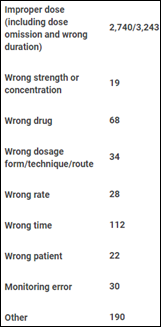
A review of 9,000 EHR-related pediatric medication events in three hospitals that use Cerner or Epic finds that EHR usability contributed to 36 percent of the reports, while 18 percent appear to have caused patient harm.
The most common problem areas were lack of system feedback and confusing visual displays.
The authors recommend that ONC add pediatric safety and usability measures to its certification requirements, that vendors and providers use realistic test-case scenarios, and that Joint Commission include EHR safety in its accreditation.
Reader Comments
From Indigenous Species: “Re: records request. I was a patient of Cleveland Clinic of Florida, which I believe is a big Epic user. They have a fancy patient portal. I used it to request a copy of an operative report and they said I had to contact the medical records department by telephone. I got through the automated attendant to the point I received a message saying I needed to either mail in a request or fax it, after which I could expect something in 10-14 days. Gazillions of dollars spent on Epic and where are we? The same place we were 20 years ago.” Cleveland Clinic Florida’s instructions (above) are embarrassing for any hospital, much less a universally-admired one – in what time warp do patients have a fax machine sitting in their homes (or for that matter, a landline to plug it into)? Why do hospital HIM departments so quickly and firmly reject the idea of printing, signing, scanning, and emailing a completed form (or even better, using DocuSign) in favor of getting their fax fix? Meanwhile, the hospital’s authorization to disclose form is, not surprisingly, a consumer-unfriendly mess for those who just want a copy of their own information. It only covers sending information to someone else, and if that’s not bad enough, the form’s footnote adds, “Cleveland Clinic Florida may, directly or indirectly, receive remuneration from a third party on connection with the use or disclose [sic] of my health information.” That’s an interesting revenue stream – taking a cut of the fees their patients are paying to obtain their own information. I hereby nominate them for my “Least Wired” consumer award, for which they may nose ahead of stiff competition via the form’s outdated reference to “venereal disease.”
From Onion Peeler: “Re: startups. Where can we send our news?” I answered, but this reminds me of a pet peeve. The misused term “startup” should carry an expiration date of maybe 3-4 years, beyond which the defining characteristics — continued outside investment, demonstrably fast growth, lots of industry buzz, and an infrastructure designed to scale — are no longer true. By that point, it’s just a less-sexy sounding small business, not that there’s anything wrong with that. Maybe “startup” should be added to the list of terms that are meaningful only when someone else uses them – innovative, world class, award-winning (preferably detailing who gave the award and for what), and disruptive. Otherwise, it’s just BSaaS.
Webinars
November 7 (Wednesday) 3:00 ET. “Opioid Crisis: What One Health Plan is Doing About It.” Presenter: Samuel DiCapua, DO, chief medical director, New Hampshire Health Families; and chief medical officer, Casenet. Sponsor: Casenet. This webinar will describe how managed care organization NH Health Families is using innovative programs to manage patients who are struggling with addiction and to help prevent opioid abuse.
Previous webinars are on our YouTube channel. Contact Lorre for information.
Acquisitions, Funding, Business, and Stock
Premier will acquire clinical decision support vendor Stanson Health for up to $66.5 million in cash. The announcement also notes that Stanson is developing a prior authorization system for medical and pharmacy benefits. Founder Scott Weingarten, MD, MPH, who is also SVP and chief clinical transformation officer of Cedars-Sinai, will remain as leader of the business. Stanson had raised just $3 million in a single Series A funding round in mid-2015.
Alphabet kicks off a two-day, employee-only conference on healthcare on its Sunnyvale, CA campus, featuring outside speakers Eric Topol, MD and former FDA commissioner Rob Califf, MD.
MJH Associates, which runs conferences and magazines such as Pharmacy Times and The American Journal of Accountable Care, acquires Medical Networking, Inc., which operates the Medstro communities and online challenges platforms as well as the Medtech Boston website.
Sales
- Health First (FL) chooses Kyruus ProviderMatch to allow consumers to find providers and book appointments via its website and call center.
- Renown Health (NV) implements PeriGen’s PeriWatch labor analysis software in its childbirth unit, including its Cues fetal surveillance solution.
- FQHC Community Healthcare Network (NY) will use Valera Health’s smartphone-based patient engagement solution for patients with behavioral and chronic health conditions.
- Massachusetts General Hospital chooses CarePassport for patient monitoring and engagement in its research studies. The company’s founder is Mohamed Shoura, PhD, who is also CEO of imaging vendor Paxera Health (formerly Paxeramed).
- LStar Imaging (TX) chooses ERad for imaging.
People

Collective Medical hires Kat McDavitt (Insena Communications) as chief marketing officer.

Cantata Health names Tad Druart (ESO Solutions) as chief marketing officer.

Health IT security and patient engagement technology vendor Intraprise Health hires industry long-timer Sean Friel (Voalte) as president.
Announcements and Implementations
Microsoft will shut down HealthVault’s Direct messaging service as of December 27, 2018, according to an email forwarded by a reader. The company did not provide a reason. The company says “other messaging services” are available, but the notice doesn’t list them and I saw no alternatives on its website except for CCD exchange. I’ve emailed Microsoft’s press contact but haven’t received a response.
In what might be the first use of teleaudiology, hearing aid manufacturer Phonak will offer access to hearing care professionals to perform online fitting and tuning via its remote support app. The company’s rechargeable hearing aids can already connect to mobile devices via Bluetooth to provide optimized sound quality for TV, music, and phone calls and its MyCall-to-Text app converts telephone conversations to text in real time. Hearing aids are inherently unexciting unless you need them (or need to pay for them, which is exciting in all the wrong ways), but this seems like pretty cool technology. Switzerland-based parent company Sonova Group is the world’s biggest hearing care solutions vendor (or close to it) with 14,000 employees and $2.7 billion in annual sales.
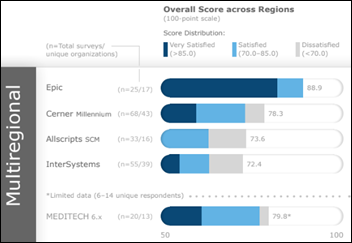
A KLAS report on how well EHR vendors serve non-US regional needs finds:
- Epic performed best with no dissatisfied customers.
- Cerner finished second despite not engaging proactively and often at extra cost.
- Meditech does well in Canada, UK, and Ireland although with concerns about slow growth and development.
- No Allscripts customers report high satisfaction and they often feel they’re on their own to implement.
- InterSystems has trending sharply down in the past two years due to staffing problems.
- Latin America is led by MV (which is increasing its lead) and Philips.
- InterSystems has slipped behind Cerner in the Middle East, while Epic has the highest score but just three live sites as prospects would like to see increased regional presence and expertise.
- Cerner and InterSystems lead in Asia/Oceania, as Allscripts customers express low confidence in the company’s R&D efforts and its acquisition strategy.
China’s Tencent announces an AI-powered smart microscope whose voice interface allows pathologists to issue commands and reports.
In England, East Kent Hospitals University goes live with the Allscripts patient administration system.
Other
Atul Gawande’s piece in The New Yorker titled “Why Doctors Hate Their Computers” makes these points:
- Computers have simplified tasks in many other industries, but have made enemies of their healthcare users.
- Partners HealthCare’s $1.6 billion Epic implementation involved less than $100 million worth of Epic software, with the remainder of the cost being lost patient revenue and the cost of implementation staff.
- Epic SVP Sumit Rana describes “The Revenge of the Ancillaries,” where ancillary departments are given a seat at the implementation table and influence decisions to make their jobs easier while forcing required fields and additional data entry on doctors.
- A busy internist colleague says Epic has reduced her efficiency, requiring her to finish documentation after going home and to struggle with a jammed Epic in basket to the point that she just deletes messages without reading them.
- The ability for everyone to modify the problem list has made it useless, requiring a review of past notes that are often excessively lengthy due to copying and pasting.
- Gawande quotes an author who in the 1970s described how users initially embrace new capabilities with joy, then come to depend on them, then find themselves faced with the choice of submitting or rebelling to the system’s control over their lives.
- An office assistant notes that much of the work she performed has been shifted to Epic-using doctors.
- Partners HealthCare’s chief clinical officer, who has been through four EHR implementations, says Epic is for the patients who look up their lab results, review their medication instructions, and read the notes their doctors have written about them. He also notes that the EHR supports population health management and research.
- Partners uses scribes, but due to concerns about turnover and errors, they chose an offshore service in which India-based doctors create visit documentation from digitally recorded encounters. A 30-minute visit requires an hour to document, with the result then reviewed by a second company doctor as well as a coding expert who looks for billing opportunities. However, as Gawande observes, “What is happening across the globe? Who is taking care of the patients all those scribing doctors aren’t seeing?”

Epic further explains how the recently mentioned New York Life integration works. People applying for life insurance ordinarily have to supply their medical history on paper after obtaining it from their hospital, a slow and expensive process. The integration uses Epic’s Chart Gateway service, which when authorized by the patient and the health system, sends information electronically to life insurance companies. It’s not blanket access to MyChart or to the data of any other patients. This is the first time I’ve heard of Chart Gateway.
The Wall Street Journal explains why smart speakers like Amazon Echo can’t make voice-requested 911 calls, at least for now: (a) lack of GPS precision; (b) inability to be called back by operators; and (c) users would need to pay 911 surcharges as they do for cell service.
Sponsor Updates
- EClinicalWorks publishes a podcast titled “How PRM Services Boosted Youth Engagement in NYC.”
- The Chicago Tribute names Intelligent Medical Objects as a “Top Workplace.”
- Former Pepsi and Apple CEO John Sculley will deliver the keynote address at MDLive’s user group meeting Wednesday at 9:30 a.m. EST, with his presentation live-streamed.
Blog Posts
- Connect 18 Recap: New Experiences, Learnings, and Friends (Spok)
- What 84 health care CIOs told us about health IT in 2019 (Advisory Board)
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates. Send news or rumors.
Contact us.








We’ll played on BSaaS
Just a small complaint…I’ve meant to send this earlier, but today, since there were two people mentioned I decided to voice (albeit a small voice) to complain…no one gives a rip about who was promoted to “Chief Marketing Officer” or of Human Resources of a vendor’s firm. Company executives, e.g. CEO, CFO, CIO, and product/development as well as implementation individuals are very important to know, particularly since they drive change (not just glossy ads, big HIMSS booths, or snazzy words). Thanks.
As a CMO, who is also a company founder and key member of our executive team determining strategy, providing input for product development, and working with customers during implementation, I politely suggest you broaden your view of what a marketing leader really does.
If you were a member of a health tech company’s leadership team you would be aware that many CMOs lead corporate and product strategy and often act as a CRO. Buying a big HIMSS booth is one of the most tactical parts of the job.
Atul seems to play a bit fast and loose with facts. Good at hyperbole though.
And, did that doc just admit to major malpractice? Deleting her inbox without looking at potential critical data? Just scanning for names she recognizes and deleting everything else without reading it?
Wonder if Partners could publish some real data about how they use Epic. Epic does provide very detailed time and motion data on each and every visit in Epic.
Also re: CCF release of records – they do have that option in Epic choose not to use it at this point. They absolutely should get on board and modernize. No reason not to (other than maybe it’s more profitable doing what they do which is sad).
I didn’t find there was anything new, just more of the same slapped with the Gawande name.
In that physician’s defense, I think what she was talking about deleting were consult finished messages or maybe hospital/ED notifications. So while it may not make her a great PCP, I don’t think it makes her a dangerous one.
I do feel for providers and their in baskets. I previously worked for a gigantic HMO with a huge amount of virtual care and no support staff and it really was a second job. I am sure it is similar for other community providers.
At my current employer we definitely struggle with revenge of the ancillaries (or perhaps just curse of complying with billing). For imaging orders providers have to enter a coded diagnosis and a separate field for reason for test. It makes me cringe every time I watch them.
“No, I ain’t got a fax machine! I also ain’t got an Apple IIc, polio, or a falcon!”
http://achewood.com/index.php?date=11222006
Since when do you have to supply health info from a hospital/provider to get life insurance?
I have had to do that for any privately acquired life insurance for the past 15 years or more. They wanted medication history, labs and information about specific types of problems or billing diagnoses. Lab work, vitals and a few social/family history questions were captured at my home by a nurse. On another occasion, I had to use their preferred lab to provide blood samples.
Just recently finished applying for life insurance and part of that was an hours long review of medical history where they wanted every place I’ve had care in the last 5 years. Had to sign ROIs and personally work with a few providers to get my medical record. Also had to have a few labs done with no existing conditions to call for it.
I am curious if part of the backlash here is due to people who didn’t have to go through a bunch of BS to get their record in paper for a life insurance company.
Glad my insurance company didn’t do that. Blood work yes, but that was it.
Not hard to de-identify the anonymous sites contributing to pediatric medication events study – Look at author’s institutions + infer correlation with # of events and size of hospital