Anything related to defense will need to go to Genesis.
Monday Morning Update 3/12/18
Top News
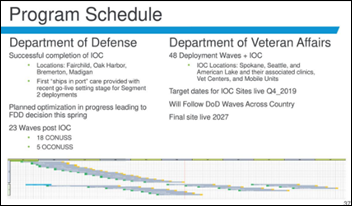
Cerner says in its HIMSS conference investor presentation that the VA will go live in 48 waves that will begin in Q4 2019 with pilot sites and then run through 2027, while DoD go-lives beyond the pilot sites will start this fall and go live in 23 waves (assuming the project reviews in both result in a go-ahead verdict). The company is also pursuing government opportunities with the Coast Guard, Indian Health Services, and CDC.
Reader Comments
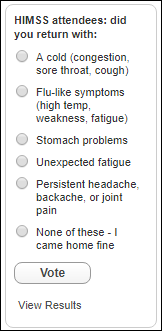
From Amy Contagious: “Re: HIMSS. I’m wondering what if any sickness people returned from the conference with? I have a light case of norovirus or similar. Wondering how many colds, flu, food issues, etc. since I don’t recall anything except exhaustion last year.” Attendees, tell us here. I’m happy to have returned just fine, other than I’m scared to get on the scales to measure the after-effect of a week’s worth of dietary destruction. Some of it was worth the calories, such as the amazing burger and fries, pizza, and wings at Home Plate Grill & Bar. I didn’t go to a single party or vendor event, spending my evenings in the rental house writing HIStalk, so low-key places nearby were just fine.
From Patiently Participating: “Re: patients at HIMSS. Did you sponsor patients to attend again this year?” I did not. I like the idea of having tech-savvy people who are actively involved in managing their chronic conditions (as well as caregivers) participate in health IT. However, I learned last time that more prep work is needed before just turning people loose in the glitzy exhibit hall to challenge random booth salespeople. Like most trade group conferences, HIMSS isn’t really designed for people who aren’t working in the field (whether that’s a feature or a bug is debatable) and just having consumers drop in isn’t necessarily productive despite noble intentions. My recommendations for offering scholarships are:
- Determine the desired outcomes of such participation.
- Develop a plan of how patients (or consumers in general) can constructively participate in the conference as a representative of others like themselves. It’s too easy to get caught up in the parties and giveaways while forgetting the real point of being there.
- Create a mandatory online training program for prospective attendees to help them understand the most effective ways to be a patient advocate and how to train others.
- Document the technology usage, frustrations, and desires of those attendees in advance so that they can be shared.
- Require as a condition of participation that attendees report to their community at large what they did there to advance their collective cause.
- Work with vendors to determine how to best engage consumer representatives during and after the conference.
- Create an online directory of companies looking for consumer guidance and for patient advocates interested in providing it.
- Set up specific meetings at the conference with the right vendor people, particularly those in product design.
- Make participation ongoing to whatever level those attendees and vendors want.
- Choose new participants regularly to bring in fresh, objective viewpoints.
From Tarheel: “Re: Novant SVP/CIO Dave Garrett. Has left the organization.” Unverified. Dave hasn’t ever been listed on the health system’s leadership page from what I can tell, but it now contains the bio of EVP/Chief Digital Officer Angela Yochem, who was hired in January. She doesn’t have any healthcare experience except for a short stint as CTO for drug maker AstraZeneca. Novant paid Dave $1 million per year, according to its latest tax forms, but he still made less than the chief consumer officer ($1.5 million) and several others just in case you were thinking that “non-profit” implies “modestly-compensated executives.”
HIStalk Announcements and Requests
With HIMSS behind us, let’s get back to the “What I Wish I’d Known Before” question about taking your first hospital IT executive job. Or more specifically, your response. Here’s mine: I wish I’d know that non-profit health systems have just as many conniving middle managers as any business, stabbing your back regularly in trying to wrest internal or external IT control. A lot of hospital people are really nice, but quite a few aren’t.
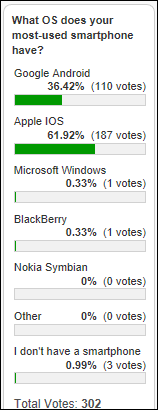
My Android phone puts me in the one-third minority among poll respondents.
New poll to your right or here: HIMSS attendees, which of the Big Five inpatient vendors made the best impression last week?
I’m interest in your thoughts about the conference. What were the best and worst parts?


Since I didn’t do a “Weekender” post last week, here’s a DonorsChoose update from Ms. M in New York City, who asked for take-home math tools for her third graders. She reports, “They couldn’t wait to see all the math games. They were even more excited when they found out they were going to be able to take the materials home with them for homework. They are so excited! These materials will help us strength our math skills and prepare us for the state exam coming up. These games will allow my students to review past math chapters in a fun and interesting way. Once again, thank you for the donation!”
My Biggest HIMSS Conference Takeaways
- The White House and HHS used the HIMSS conference to come out shockingly forcefully in vowing to attack information blocking; to give patients more control over their information; to move more quickly into value-based care; to reduce physician EHR burden; and to disrupt the system in which health systems keep charging more without delivering commensurately improved outcomes. Nobody knows how these populist talking points will get turned into policy.
- VA and DoD EHRs remain a contentious topic.
- The big keep getting bigger in healthcare, including in health IT.
- Microsoft, Amazon, and Google have their eyes on earning a chunk of our massive healthcare spending by replacing local data centers with cloud hosting and back-end services.
- AI is ready for prime time, at least in the context of powering virtual assistants that make clinician EHR interaction more tolerable.
- Health IT is spreading beyond health systems and practices to skilled nursing facilities, home health, public health, behavioral health, and pharma.
- Everybody is talking about consumerism despite little evidence that it actually exists in the classic sense due to lack of provider transparency and the involvement of intermediaries such as insurers.
- The real Meaningful Use ROI is just now becoming obvious as massive amounts of electronic data are being used for research, outcomes studies, financial analysis, and whole-patient views, all of which provide evidence to support policy and practice changes that would not have been possible otherwise.
- Interoperability is improving, but far from solved, as providers still have no financial incentive to demand it of their vendors and competitors.
- HIMSS keeps acquiring and growing its way to a bigger bottom line.
HIStalk Image Sizes
A reader complained about too-small images in news posts and I said I would put it to a vote. The choices are as follows.
Option 1 – No Change
Use small images (250 pixels wide) for low-detail items like a hospital photo, larger images (350 pixels) for web captures or anything that would be hard to read in the smaller size. Even the large size could be hard to read if the image contains a lot of text (like a dense web page). Examples are below.

A 250-pixel image.

A 350-pixel image.
Option 2 – Use Mostly Larger Images
This option involves making the standard size 350 pixels wide in all most cases, even low-detail images such as the hospital example above. The downside is that wider images are also taller, meaning it requires a bit more scrolling to read the entire post.
Option 3 – Use Thumbnails
Images would be displayed as a “thumbnail” preview that’s about the same size as the current small image. Clicking the image displays it larger, and the larger size could be much bigger than the current 350 pixels. Downsides: pretty much every image would need to be clicked to view it. You have to page back after reviewing to return to HIStalk. Accidentally hitting the image with your finger on a mobile device takes you out of the HIStalk page.
Vote for your preferred option.
Webinars
None scheduled soon. Previous webinars are on our YouTube channel. Contact Lorre for information.
Acquisitions, Funding, Business, and Stock

HIMSS extends its lease through 2021 of the top floor at Cleveland’s Global Center. They should get the American Optometric Association on board since the building’s visually jarring design has probably spurred quite a few eye exams.
Decisions
- Fairfield Medical Center (OH) will switch from McKesson to Cerner on April 1, 2018.
- Central Montana Medical Center (MT) will go live on Cerner in 2019.
- Hermann Area District (MO) will go live on Cerner in June 2018.
These provider-reported updates are supplied by Definitive Healthcare, which offers a free trial of its powerful intelligence on hospitals, physicians, and healthcare providers.
People

Contra Costa Health Services (CA) promotes CIO Dave Runt to COO.

Deloitte Consulting hires Douglas Rosendale, DO (CAIRNformatics) as federal chief medical interoperability officer.
Other

Pharma bro Martin Shkreli — who had previously boasted that prosecuting attorneys in his securities fraud case were “junior varsity” — cries like a baby before being sentenced to seven years in prison. His own attorney said in his closing statement that while he sometimes wants to comfort his client, “there’s times I want to punch him in the face.” Note that Shkreli was found guilty only of ripping off fellow rich people – ripping off not-rich patients and their insurers by jacking up the price of Daraprim by over 5,000 percent remains perfectly legal and, from a purely business standpoint, admirable.
Odd: a 52-year-old, female New York City EMT is arrested for hitting a hospital employee over the head with a computer tablet following an argument.
Contacts
Mr. H, Lorre, Jenn, Dr. Jayne.
Get HIStalk updates. Send news or rumors.
Contact us.




I say leave the images the same size out of spite towards that rude jackass commenter.
I admit that I don’t see (literally) the problem even though I read HIStalk on my small phone and IPad Mini, but apparently it’s a big deal to that commenter. It probably depends on what the image contains — I write HIStalk on my laptop and if I can’t see important detail, I go larger (which means it will be really large on my desktop monitor) or crop more to zoom in. I rarely need to go even larger, but for something important, like a detail-rich document or chart, I’ll sometimes use a thumbnail.
It really depends on what kind of device you’re reading on and how much detail you expect to see, along with other factors such as visual acuity. The current method works fine for me but it’s equally easy to change to the other options.
You might be overthinking it. I would guess that you can include a quite a high resolution image, and WordPress would manage it appropriately for different screen sizes. There’s also probably some feature to provide a modal view of the full image on a click, without leaving the page.
Are there any WordPress users who can chime in?
Nothing on telehealth from your update. It was pretty prominent this year vs others with a headline on day one etc. the interop and consumerism issue (not to mention info blocking) effect TH big time. Looked like the big DTC’s are getting bigger and the smaller ones are falling away. Thoughts?
I know many here disagree, but I don’t consider telehealth a health IT topic any longer since the technical battles have been overcome and it’s really just another healthcare services delivery venue, especially as for-profit companies expand with little technical innovation (Skype with your doctor, basically). The key issues with it involve reimbursement policy, and effectiveness rather than technology. I might get slightly interested when the topic includes home device connectivity or health system EHR integration, but otherwise I just assume video visits are as reliable and yet unexciting as calling up my doctor on the phone.
Reacting to your comment at the end of Takeaway #1 (“Nobody knows how these populist talking points will get turned into policy.”). Not sure if that is a dig because you don’t care for the current populism, or your intended humor didn’t come through, but let me try to tell how. What we DO know is that all previous stabs at doing this have failed, so perhaps a different path could be tried?
First, POTUS is a negotiator, so this is the first salvo in the negotiation. Just by firing a couple of 00-Buck shells into the room as they did, people are scrambling. This is good. I predict we will see industry action without much more input from the administration, at least for the immediate future, as they will be given an opportunity to start fixing things themselves.
Next, most everyone in healthcare who writes, including on HIStalk, decry the delays and roadblocks to patients getting their data – even WITH laws on the books, and you’ve reported on it. The “populist” angle will supply pressure to make that happen. Again – at least something is happening besides talk and the non-enforcement of existing data release laws.
I say, get your popcorn, sit back and enjoy the show. I don’t care which politician or political philosophy “wins”, I just want success when it comes to improving the healthcare industry and delivery system. Looking at the past, certain of those philosophies have failed us, so perhaps populism can get it done. Odds have improved so that we may actually get most/all of those things you listed in #1.
And I write this as a strong supporter of our healthcare system and its dedicated personnel (who masterfully handled a recent, very serious and potentially deadly illness of mine with a glowing outcome, and to whom I am eternally grateful).
Populism can’t solve anything of consequence. It only makes certain groups feel good in the short term, while destroying possible ways of achieving progress. You can look at Venezuela to see the results of populism…
Sorry Mr. Head. Venezuela’s problems are caused by Communism and Socialism, (and the word you used – “progress”), and not populism. The people didn’t cause the failure there (populists were shot), it was a corrupt, one-party rule who “stole the gold” resulting in collapse, starvation and death, which is the natural end point of a full takeover by that ilk. Populism may be the only way to save them, if it is not too late.
This is not the format to debate political viewpoints, it is a healthcare blog, and I purposely didn’t engage that way – I was answering Mr. H’s point that populism may be good at stirring things up, but not in achieving results. My response was that I think we are seeing results. As the Romans would say: “q.e.d.” Stay tuned.
Re: You keep using that word. I do not think it means what you think it means.
Just to make sure we are talking about the same things, and are not inventing different meanings to common words, here are two sources that describe populism, and I believe Mr. H was referring to exactly that kind of populism:
http://www.upenn.edu/pennpress/book/15615.html
http://www.hup.harvard.edu/catalog.php?isbn=9780674976825